Doing a root canal is one of the most common dental procedures. During this treatment, the pulp tissue inside the tooth is removed and the canal system cleaned, shaped, and sealed. But not all teeth present the same level of difficulty when it comes to root canal therapy. The type of tooth and its individual anatomy can greatly impact the complexity of performing a root canal. Let’s take a detailed look at which teeth tend to be the easiest and most challenging for root canal treatment.
Anatomy Factors Influencing Root Canal Difficulty
There are several anatomical factors that determine how straightforward or difficult it will be to perform a root canal on a particular tooth:
Number of Roots
Teeth with fewer roots have simpler canal systems requiring less treatment. Anterior teeth generally have one root while premolars may have one or two roots. Molars have the most complex anatomy with three or four roots in lower and upper first molars, and two to three roots in second and third molars. The greater the number of roots, the more difficult the procedure.
Number of Canals
Each root contains at least one canal, but may contain multiple canals. Additional canals are more likely in teeth with multiple roots. Higher numbers of narrow, curved canals to locate, access, shape, and fill adds more challenge to the root canal therapy.
Curvature and Dilaceration
Straight roots with minimal curvature are ideal for root canal treatment. Severely curved, hooked, or dilacerated roots make accessing the apex more difficult. Curved canals must be shaped with specialized flexible files and techniques.
Canal Diameter
Teeth with wide canal diameters are easier to instrument and fill compared to narrow canals. Anterior teeth have wider canals than premolars and molars. Very fine, ribbon-shaped canals provide less room to maneuver instruments.
Calcifications
Extensive calcifications and canal blockages due to past trauma or caries complicate canal location and negotiation. Teeth requiring access through calcified tissue are more difficult.
Accessibility
The location and position of the tooth in the mouth impacts accessibility. Anterior teeth in the front of the mouth provide straight-line access. Posterior teeth, like molars, are hard to view and access due to their recessed location.
Periodontal Condition
Teeth with excessive bone loss from periodontal disease provide less ideal isolation and access to canal orifices. Additional procedures may be required to stabilize periodontally involved teeth during endodontic therapy.
Prior Treatment
Teeth receiving prior unsuccessful root canal treatment or exhibiting significant defects from restorative procedures present added challenges. The original canal anatomy may be obscured, making retreatment more difficult.
Tooth Difficulty Ranking for Root Canals
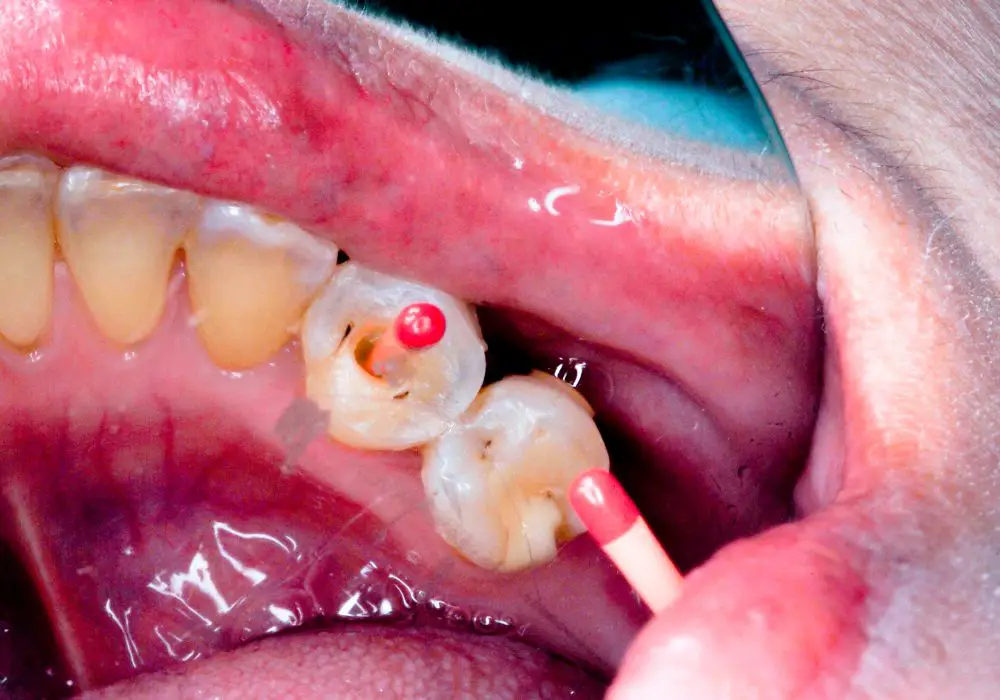
Based on these anatomical factors, we can categorize different tooth types from easiest to most difficult for root canal therapy.
Easiest
Maxillary (Upper) Central and Lateral Incisors
These anterior teeth have:
- A single straight root
- A wide canal diameter
- Minimal curvature
- Large, easily accessed pulp chamber
- Straightforward access due to anterior location
Maxillary (Upper) and Mandibular (Lower) Canines
Canines have:
- A single straight root in most cases
- May have a slight distal curve
- Wider canal diameter than premolars/molars
- Accessible anterior location
Moderately Difficult
Maxillary (Upper) First and Second Premolars
Premolars have:
- Typically one or two roots
- Moderate curvature possible
- Narrower canals than anterior teeth
- Posterior location provides less visibility
Mandibular (Lower) First and Second Premolars
These have:
- High frequency of two roots
- Distolingual root curvature common
- Narrow mesial-distal canal diameter
Most Difficult
Maxillary (Upper) First, Second, and Third Molars
Molars have:
- Three or four roots depending on the molar type
- Multiple fine curved canals
- Calcifications common
- Limited access and visibility due to posterior location
- Complex internal anatomy
Mandibular (Lower) First, Second, and Third Molars
These present:
- Two to four roots
- Severe curvature of distal and distolingual roots
- Multiple narrow canals
- High incidence of anatomical complexities
- Extremely limited accessibility to posterior area
While this ranking provides a general guide, difficulty can vary on a case-by-case basis depending on the particular tooth anatomy and pulp morphology. Other factors like trauma, age, restorations, and periodontal status can increase the level of root canal difficulty.
Factors That May Complicate Root Canal Treatment
Beyond just the anatomy of the tooth itself, there are additional procedural factors that can complicate root canal therapy:
- Retreatment cases – Teeth requiring root canal retreatment due to failed previous treatment often present greater challenges due to changes in the internal anatomy. Accessing and fully cleaning all aspects of the canal system is more difficult.
- Multiple appointment procedures – Root canals requiring multiple visits over several weeks increases the difficulty and chance of complications like reinfection or leakage. This allows more time for changes to occur internally before the tooth is permanently sealed.
- Limited opening – Patients with restricted oral opening prevent ideal straight-line access for visibility and instrumentation of the canals.
- Extensive dental work – Existing large restorations, crowns, or bridges may impede direct access to canal orifices during treatment.
- Isolation challenges – Situations where optimal rubber dam isolation is difficult due to large edentulous spans or severe periodontal disease complicate treatment.
- Immature apices – Teeth with open, incompletely formed apices provide less canal wall support during cleaning and filling procedures.
- Canal obstructions – Blockages like ledges, perforations, broken instruments, and calcifications within the canal space severely hinder proper instrumentation.
- Root resorption – Loss of root structure due to inflammation or pressure complicates sealing of the canal terminus.
Importance of Technology and Specialist Skills
Today’s advanced technologies like dental operating microscopes, ultrasonics, and nickel-titanium rotary instruments allow intricate root canal procedures to be performed even on very challenging teeth. Specialist endodontists undergo 2-3 extra years of advanced training to gain the skills necessary to tackle difficult root canal anatomy. Referral to an endodontist may provide the best chance of success when confronted with complications or complex morphology.
Conclusion
In summary, anterior teeth, particularly the upper central incisors, provide the path of least resistance when performing root canals. Premolars are moderately difficult, while molars present the greatest obstacles. However, today’s specialized techniques and equipment allow successful root canal therapy even on very challenging tooth anatomy. Proper training, clinical experience, technological aids, and specialist referral enable optimal outcomes.
Frequently Asked Questions
Q: Which anterior teeth are the absolute easiest to do a root canal on?
A: The maxillary (upper) central incisors are generally considered the easiest teeth to perform root canals on. They have a single large straight root and canal with a pulp chamber that is easily accessed. Their location in the front of the mouth also provides good visibility and straight-line access.
Q: Do third molars (wisdom teeth) have the most difficult root canal anatomy?
A: Third molars often rank among the most difficult teeth for root canals due to their posterior location providing very limited accessibility. They also tend to have aberrant anatomy with extra roots, severe curves, and calcifications. However, in some cases third molars may be easier than lower first or second molars if the root anatomy is relatively straightforward.
Q: Does the lower jaw tend to have more difficult root canal anatomy compared to the upper jaw?
A: Generally yes, the mandibular (lower) teeth tend to have slightly more complex canal anatomy compared to the maxillary (upper). The roots tend to be more curved and smaller in diameter. However, difficulty can vary on a case-by-case basis depending on the particular tooth and root/canal configuration.
Q: How does previous trauma to a tooth impact the difficulty of doing a root canal on it?
A: Trauma, especially when it results in pulp necrosis, often precipitates calcification of the canals. It can also lead to abnormalities in the internal anatomy. This will significantly complicate canal location and instrumentation. Traumatized teeth often require the use of operating microscopes and advanced techniques to locate and manage the canals.
Q: Is a root canal harder if a patient has extensive gum disease or bone loss around the tooth?
A: Yes, poor periodontal support around a tooth makes isolation more challenging and access to the canals more difficult. It also increases the permeability to bacteria and likelihood of post-treatment infection. Additional procedures to stabilize the bone may be required to support long-term root canal success.