What causes tooth root sensitivity?
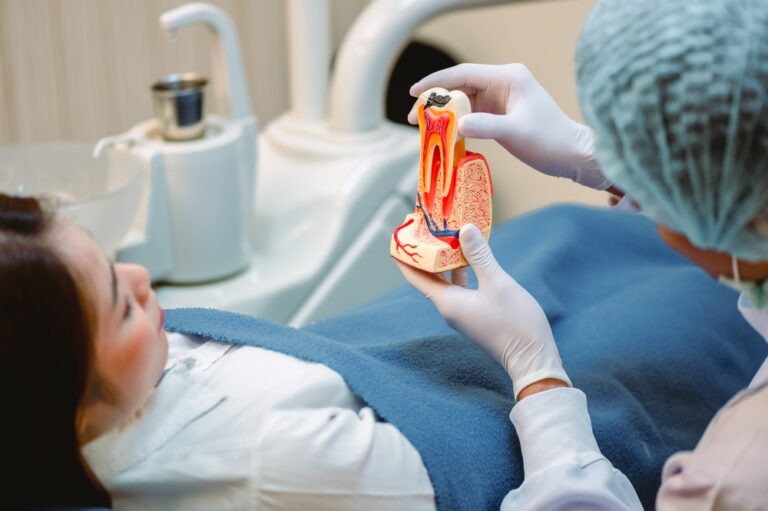
Tooth root sensitivity, also known as dentin hypersensitivity, is a common dental problem that occurs when the root surface underneath the gum line gets exposed, leading to pain and discomfort. The root surface contains thousands of tiny tubules that run from the pulp chamber down to the root canal opening. These tubules contain fluid and nerve fibers that are extremely sensitive to stimuli.
When the root loses gum coverage due to receding gums, the tubules become exposed to the oral environment. Things like hot, cold, acidic or sticky foods and drinks can then penetrate the tubules and trigger sharp pain by stimulating the nerve. This is why anything that causes gum recession and root exposure can lead to root sensitivity.
Some of the most common causes of gum recession and exposed roots include:
- Gum disease – Also called periodontal disease or gingivitis, gum disease is caused by a buildup of plaque on teeth. Plaque contains bacteria that trigger inflammation and infection that damages the gum tissue over time. As gums recede due to periodontal disease, more of the tooth root underneath gets uncovered.
- Aggressive brushing – Habitually brushing too hard with a stiff bristle toothbrush or abrasive toothpaste can damage gums and cause them to wear away from the teeth. Over time, this gradually exposes more of the root surface.
- Tooth grinding – People with bruxism or teeth grinding problems can put excessive force on the teeth when clenching or grinding at night. This can lead to accelerated gum recession around the teeth as well as exposing dentin.
- Age – As we get older, our gums naturally recede to some degree just from normal aging effects. This causes long-time adult teeth to become more prone to root sensitivity.
- Poor fitting dental work – Defective fillings, loose crowns, and ill-fitting dentures can lead to chronic inflammation and localized gum recession around affected teeth.
- Mouth injuries – Any kind of trauma to the gums and bone supporting the teeth, such as sports injuries, aggressive orthodontic treatment, or tooth extractions can damage the gum and bone tissue and expose more of the tooth root.
- Genetics – Some people are just prone to thinner gum tissue, lower bone density, and a higher risk of gum recession and root exposure through no fault of their own. It may run in their family.
- Medical conditions – Diseases like diabetes that impair healing can increase gum problems and recession. Osteoporosis and other causes of bone loss also increase root exposure risk.
Why does exposed root cause pain?

When the root surface loses its protective gum covering, thousands of tiny tubules that run from the pulp to the root canal opening get exposed to the environment. These tubules transmit temperature, pressure and pain signals from the outside world directly to the tooth nerve.
The crown of the tooth is covered by super strong enamel, while the root has cementum over it which is softer and more porous. So the exposed root tubules are very vulnerable to irritation and stimulation from hot, cold, acidic, sticky foods, brushing, dental work, etc.
When these stimuli reach the inner tooth nerve via the tubules, the nerve registers them as pain or discomfort. The pain is often sharp and intense when hot or cold foods hit the exposed root surface because of how quickly these temperatures conduct through the tubules to the nerve fibers.
In addition to hot and cold pain triggers, existing tooth decay, development of cavities at the root, and recent dental treatments like fillings and root planing can all contribute to root sensitivity. The closer the irritation occurs to the nerve center, the more likely it is to provoke pain.
When does exposed root pain occur?
Root sensitivity pain can come on suddenly, get worse over time, or only happen occasionally depending on the individual case. Here are some of the times those with sensitive tooth roots may experience pain:
- During eating/drinking – Hot, cold, sugary, acidic or sticky foods and drinks are common triggers that provoke sharp pain when making contact with exposed roots. Pain when sipping hot coffee or cold water is very characteristic.
- During brushing – Exposed roots may throb or cause discomfort when brushing vigorously with a hard bristled brush. It can also occur using abrasive toothpaste.
- After dental procedures – It’s very common to have increased root sensitivity for days or weeks after fillings, root scalings, extractions, crowns, or implants that can irritate the inner root surface.
- At night – Some people report increased root pain when resting or laying down, as pressure from the pillow may further aggravate the exposed root area.
- Seasonal changes – Many people find their root sensitivity worsens during the colder winter months or when frequently exposed to air conditioning which can cause pain.
- For no apparent reason – Low-grade constant sensitivity may persist even without any clear triggers, as exposed root surfaces tend to get inflamed easily on their own.
If the tooth root pain comes and goes but lasts more than 3-4 weeks, seems to worsen over time, or disrupts eating and sleeping, it’s best to get evaluated promptly by your dentist.
When to see a dentist
You should have an exam with your general dentist if you experience:
- Ongoing root sensitivity that lasts more than 3-4 weeks
- Root pain that is severe and interferes with eating, drinking or sleeping
- Increasing sensitivity that seems to be getting worse over time
- Gum recession, swelling, redness, sores or bleeding in the affected area
- Bad breath, bad taste in the mouth or other signs of oral infection
- Difficulty chewing or apparent decay in the sensitive tooth
- Medical conditions like diabetes, osteoporosis, cancer treatments that impair healing
Seeing your dentist as soon as possible for evaluation and treatment helps resolve sensitivity before it gets more severe.
How do dentists diagnose the cause of root sensitivity?
Accurately diagnosing the underlying reason for root sensitivity is key to targeted treatment. At your dental visit, expect your dentist to:
- Ask questions about your oral symptoms – when does the pain occur, what provokes it, does it keep you up at night, etc.
- Do a clinical exam looking for signs of decay, cracked teeth, gum recession, swelling, and inflammation.
- Check for loose teeth, defective fillings, or ill-fitting dental work that could be contributing to the problem.
- Examine your bite alignment for signs of teeth grinding which accelerates wear.
- Evaluate gum recession visually and by probing gently around the teeth with a periodontal tool.
- Take X-rays to look for hidden structural problems, cavities at or below the gumline, and bone loss.
- Assess your risk factors like diabetes, osteoporosis, smoking, and medications.
- Do individual tooth testing by exposing teeth to hot and cold stimuli, tapping them, or using an air jet to pinpoint sensitivity.
With the information gathered from the exam, your dentist can piece together why the root got exposed and what factors are provoking the pain response. This drives the right treatment plan.
What treatments are available for sensitive tooth roots?
There are a variety of ways dentists can treat root sensitivity, both at home and professionally in the dental office. Common treatments include:
1. Treat gum disease
Since gum disease is a major player in gum recession and root exposure, treating any active or chronic periodontal infections is crucial to halt the tissue damage. Typical treatments include professional cleanings, antimicrobial mouth rinses, antibiotics and oral hygiene instruction.
2. Improve your oral hygiene routine
Your dentist may recommend switching to a soft bristle toothbrush, using less abrasive toothpaste, and brushing with a gentle touch to avoid gum abrasion and recession. Daily flossing and mouthwash use helps keep gums healthy.
3. Use desensitizing toothpaste
There are many over-the-counter toothpastes containing novamin, stannous fluoride, arginine or strontium chloride that can relieve sensitivity. Brushing twice daily with a desensitizing paste gives the best effects.
4. Have fluoride treatments
In-office fluoride applications done professionally or prescription strength fluoride gels/rinses at home help strengthen enamel and protect exposed roots.
5. Get a gum graft
Periodontists can graft gum tissue from the roof of the mouth to cover exposed roots, protecting them from stimuli. This is done for moderate-severe gum recession cases.
6. Apply desensitizing dental products
Dentists can coat the root surface with bonding agents, glass ionomer cements or composite resins that seal the tubules and block sensitivity.
7. Use prescription strength rinses
Special prescription rinses with potassium nitrate or stannous fluoride help control root sensitivity when used twice daily.
8. Take supplements
For those with osteoporosis contributing to gum recession, calcium and vitamin D supplements may help strengthen bone and reduce sensitivity.
9. Use oral analgesics
For short-term pain relief, over-the-counter analgesics like ibuprofen can temporarily reduce sensitivity discomfort until a dental treatment can be done.
10. Root canal treatment
If sensitivity is severe and persistent, removing the inner nerve and pulp tissue of the tooth with a root canal can fully eliminate the pain. A specialist performs this endodontic treatment.
How can I prevent recurrent root sensitivity?

Once the active root sensitivity gets treated, regular dental visits plus diligent at-home care can help keep it from returning. Prevention tips include:
- Maintain impeccable oral hygiene with daily brushing, flossing and antimicrobial mouthwash. This prevents gum disease from worsening.
- Use extra soft bristles, limited pressure and fluoride toothpaste when brushing to protect your gums.
- Avoid very hot, cold, sugary, acidic or sticky foods/drinks that can penetrate the root tubules.
- Drink water after consuming acidic foods or drinks to neutralize erosive acids.
- Don’t over-brush! Let proper dental cleanings remove stains rather than aggressive brushing.
- Have any defective restorations like crowns or fillings replaced before decay forms.
- Use prescription strength fluoride toothpaste or rinses daily to strengthen enamel.
- Ask your dentist about application of fluoride varnish every 3-6 months to protect your roots.
- Wear a custom night guard if you grind your teeth to prevent accelerated wear.
- See your dentist every 6 months for professional cleanings and close monitoring.
- Monitor your health conditions and medications that can impact oral health.
When should I follow up with my dentist about root sensitivity?
It’s recommended to follow up with your general dentist around 4-6 weeks after initial treatment for root sensitivity. This allows them to evaluate your healing and function. If the sensitivity was due to gum recession, your dentist will want to monitor areas at high risk for more recession frequently, usually every 3-6 months.
Maintaining regular 6 month dental cleanings and check-ups lets your dentist detect any recurrent or new areas of sensitivity early before they become problematic again. Sudden reappearance of throbbing, severe root pain should prompt an immediate dental visit for reevaluation. Stay vigilant with at-home preventive care and professional monitoring to successfully manage root sensitivity long-term.
Conclusion:
Tooth root sensitivity is a very common problem that occurs when the roots below the gumline lose their protective covering, exposing microscopic tubules that transmit pain from stimuli to the tooth nerve. Root exposure is often caused by gum recession from gum disease, brushing too hard, dental trauma, grinding, and aging. The result is sharp pain triggered by hot, cold, sweet, acidic foods and touch.
If left untreated, root sensitivity usually increases over time as the area of exposed tubules grows. The good news is dentists have many effective options to treat the sensitivity, numb the symptoms, and prevent recurrence. Excellent oral hygiene plus seeing your dentist promptly at the first twinges of root pain allows early intervention before severe discomfort occurs. With vigilant home care and follow-up, root sensitivity can be successfully managed by you and your dental professional.
Frequently Asked Questions
Why does root sensitivity hurt more at night?
Root sensitivity typically worsens at night for several reasons:
- Lying down increases pressure on the exposed root area from your pillow or mattress. Extra pressure on the thousands of open tubules can increase nerve irritation.
- Saliva flow decreases substantially when you sleep, so there is less protective saliva coating the root surface.
- If you grind or clench your teeth at night, this can accelerate wear and further expose sensitive root surfaces.
If I ignore the pain, could my root sensitivity get worse?
Yes, it’s important not to ignore persistent root sensitivity as it can definitely worsen over time without treatment. As more of the root surface loses gum coverage, more microscopic tubules become exposed. More exposure means more pain signals can reach the nerve and provoke increased inflammation and discomfort. Severe cases can eventually lead to tooth loss.
Why do sweets aggravate my root pain?
Sugary foods and acidic drinks allow acids and sugars to penetrate deep into the tiny tubules on the root surfaces, reaching the tooth nerve and causing irritation. Sticky candies also tend to adhere to exposed root surfaces, prolonging the irritation. After consuming sweets, drink plenty of water to rinse sugars away and neutralize acids.
Is sensitive tooth root linked to osteoporosis?
Some research indicates people with osteoporosis and diminishing bone density seem prone to more severe gum recession and increased root exposure compared to others in their age group. Getting sufficient calcium and vitamin D helps strengthen bones and reduces sensitivity in those with low bone density. Let your dentist know if you have osteoporosis.
Will I need a root canal for my sensitive tooth?
In most mild-moderate cases of root sensitivity, topical treatments like fluoride and desensitizing toothpastes work well to reduce pain. However, if you have intractable, constant severe sensitivity that fails to respond to more conservative treatments, a root canal may be required. It involves removing the inflamed nerve and pulp tissue to stop the pain signals. An endodontist performs this procedure.