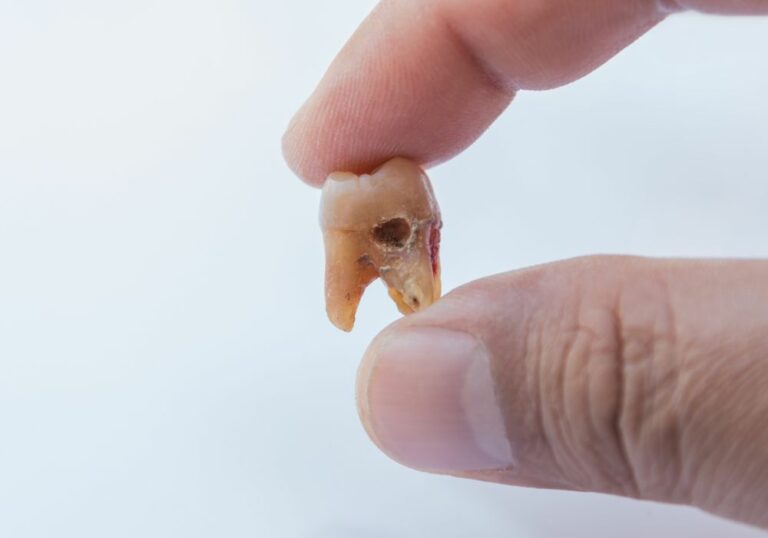
What is tooth decay?
Tooth decay, also known as dental caries, is a breakdown of the tooth structure caused by bacterial acids. It starts when plaque, a sticky film containing bacteria, builds up on the teeth. The bacteria in plaque metabolize sugar and release acids that dissolve the enamel on the tooth surface. This results in cavities or holes in the teeth.
As decay progresses further into the tooth, it can infect the inner pulp tissue (dental pulpitis) and root canals. If left untreated, tooth decay can lead to severe infection, tooth loss, and systemic health issues.
Causes and risk factors for tooth decay
Some of the common causes and risk factors for tooth decay include:
- Poor oral hygiene – Inadequate brushing and flossing allows plaque to accumulate on teeth.
- Frequent sugar consumption – Bacteria feeds on sugar to produce acids that demineralize tooth enamel.
- Dry mouth – Lack of saliva fails to neutralize acids and wash away food debris. Certain medications, health conditions, and aging can cause dry mouth.
- Acidic foods and drinks – Frequent exposure to acidic foods like citrus fruits, tomatoes, and sodas erodes enamel.
- Orthodontic appliances – Braces and other appliances trap food and make plaque removal difficult.
- Deep pits and fissures in teeth – The grooves are hard to clean and are prone to decay.
- Exposed root surfaces – Gum recession exposes the cementum layer which is more susceptible to decay.
- Reduced fluoride exposure – Fluoride remineralizes enamel and makes it more decay resistant.
- Genetic predisposition – Some people may have naturally thinner enamel or enamel prone to demineralization.
Signs and symptoms of tooth decay
Some common signs and symptoms of tooth decay include:
- Visible holes or pits in the teeth
- Brown, black or white stain on the teeth
- Pain or sensitivity to hot, cold, or sweet foods
- Dull, constant toothache
- Bad breath
- Crooked or cracked teeth
- Breakdown of tooth structure
Why placing a crown on decay can be problematic
Compromised tooth structure
As mentioned earlier, tooth decay compromises the integrity of enamel and dentin which provide the solid foundation required for placement of a crown.
Enamel is an extremely hard mineralized substance covering the visible section of the tooth. It functions as a protective layer shielding the softer dentin beneath.
Dentin is a calcified tissue that forms the bulk of each tooth. It contains thousands of microtubules extending from the pulp chamber to the dentinoenamel junction. These tubules transmit sensations of hot, cold, salty, etc to the innervated pulp.
When decay attacks enamel and eats through to the dentin, it progressively dissolves these load-bearing mineralized tissues. Over time, this destruction undermines the structural strength of the tooth.
Placing a crown requires removing even more tooth structure to accommodate its thickness. If such aggressive removal is done on a decayed tooth, it could critically weaken its support system. This increases the chance of fracture under bite force pressure.
Risk of infection
Bacterial acids are not the only deleterious product released when plaque bacteria metabolize fermentable carbohydrates. They also generate toxic enzymes and waste products that stimulate inflammation and interfere with wound healing.
If decay is sealed under a crown, these noxious irritants remain trapped inside the tooth. They can trigger pulpal inflammation and compromise the tooth’s natural defenses.
This provides an ideal anaerobic environment for cariogenic bacteria to thrive and rapidly propagate. Their uncontrolled growth causes rampant recurrence of decay and infection within the sealed tooth.
Progression of decay
Decay usually does not progress uniformly. Some areas of decayed enamel and dentin may look reasonably solid during crown preparation.
However, demineralization from bacterial acids often proceeds in an irregular course through the microscopic pores and channels within the tooth structure.
So even if the visibly decayed areas are excavated, hidden infection may still remain deeper within the tooth. These infected tunnels of decay cannot be detected clinically but will continue to spread beneath the crown.
This insidious process will gradually undermine the foundation of the tooth. Over time, the tooth becomes more likely to fracture under occlusal forces.
The crown preparation process
Tooth preparation
Before taking impressions, the tooth is prepared by removing 1-2 mm of its outer surface to make space for the bulk of the crown. This is done using a high speed dental handpiece and abrasive burs.
The preparation aims to achieve 6 degrees of convergence from all sides towards the occlusal surface. This taper provides mechanical retention by allowing the wider crown material to grip the narrower walls of the preparation.
The margins of the preparation should end on sound tooth structure, not decay. Extension of decay beyond the planned margin may require additional tooth removal.
Impression taking
An accurate impression is crucial for proper crown fabrication and fit. Common impression materials include polyvinyl siloxane, polyether rubber, or hydrocolloid.
Light-cured acrylic resin provisionals can be made chairside from the initial preparation impression. But this direct method is less precise than lab-fabricated temporaries from a separate impression.
The master impression material must flow accurately into the preparation to capture its finest details. Any distortions will produce crown misfit with poor margins permitting bacterial ingress.
Bite registration
Bite registration captures the occlusal relationship between the prepared tooth and opposing dentition. Accurate mounting of working casts on the articulator recreates this bite for ideal crown contouring.
Bite distortion from decay may require altering the registration through selective grinding. This helps avoid crown interference and improper occlusal contacts.
Crown placement on a decayed tooth
Crown selection
The crown material must be strong enough to withstand bite forces without fracture. Metallic alloys are the strongest options for posterior decayed teeth at high risk of breaking.
Gold crowns are very durable but limit aesthetics. Porcelain fused to metal provides more natural appearance while retaining strength.
All-ceramic crowns like zirconia may not be suitable for badly decayed teeth unless the walls are built up with composite first.
Crown preparation
Preparation for decayed tooth crowning is more conservative than for a non-decayed tooth. The clinician must balance aggressively removing decay with preserving tooth structure.
Rotary instrument speeds, force applied, and extent of taper may be reduced. A butt joint margin may be used instead of a heavy chamfer.
Crown cementation
Retention of the definitive crown is critical. Weak, decayed walls may not withstand the pressure required for cementation. Precementation of a thin resin coating can enhance the internal surface grip.
Dual-cured resin cements are commonly employed for their high bond strength, insolubility, and low solubility. Pre-treatment of the internal surface with adhesive further increases retention.
Often a glass ionomer or temporary cement is placed initially in case the crown needs to be easily removed later. The final resin cement is applied at a subsequent visit after confirming the patient’s satisfaction.
Potential problems with crowning a decayed tooth
Despite best preventive efforts, crowning a decayed tooth does incur additional risks:
- Fracture of unsupported enamel rods and weakened cusps
- Splitting of the marginal ridge from excessive taper
- Microleakage around defective margins leading to recurrent decay
- Pulpitis, infection, abscess due to residual decay reaching the pulp
- Hypersensitivity from compressed dentinal tubules transmitting fluid movements
- Crown loosening requiring recementation or replacement
- Need for root canal treatment due to pulpal complications
- Eventual extraction of the tooth if decay causes excessive damage
Close monitoring and patient compliance are mandatory following crowning of a decayed tooth to avoid adverse sequelae and achieve satisfactory long-term outcomes.
Ideal candidates for crowning decayed teeth
Although crowning extensively decayed teeth is ill-advised, carefully selected cases with minor decay in a limited area may still yield acceptable results.
Some examples of suitable candidates include:
- Decay confined to a small pit or fissure with good peripheral enamel
- Localized decay near the gingiva amenable to crown lengthening
- Lingual surface decay easily accessed for complete caries removal
- Teeth with sufficient intact coronal tooth structure to retain a crown
- Compliant patients with good plaque control and regular dental follow-up
- strategic abutment teeth for fixed bridges may be crowned despite mild decay
Proper diagnosis, caries risk assessment, effective communication, and vigilant monitoring are key to determining if a decayed tooth can be successfully crowned.
Conclusion
In the presence of extensive decay, crowns are typically contraindicated. However, when localized decay is detected early and has not penetrated too deeply, crowning may be possible after caries excavation and restoration with a filling material.
Careful case selection based on factors like the extent, depth, and location of decay is imperative. Skill, experience, and prudence on the clinician’s part are also critical for achieving acceptable outcomes.
With thoughtful planning, strict caries control measures, patient compliance, and persistent vigilance, crowning a judiciously chosen decayed tooth can result in good long-term prognosis. However, these cases demand more cautious monitoring than crowning an intact non-decayed tooth.