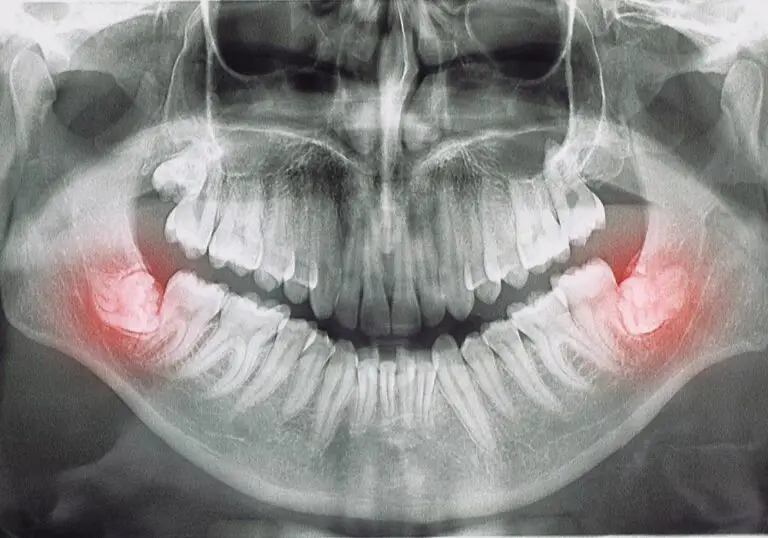
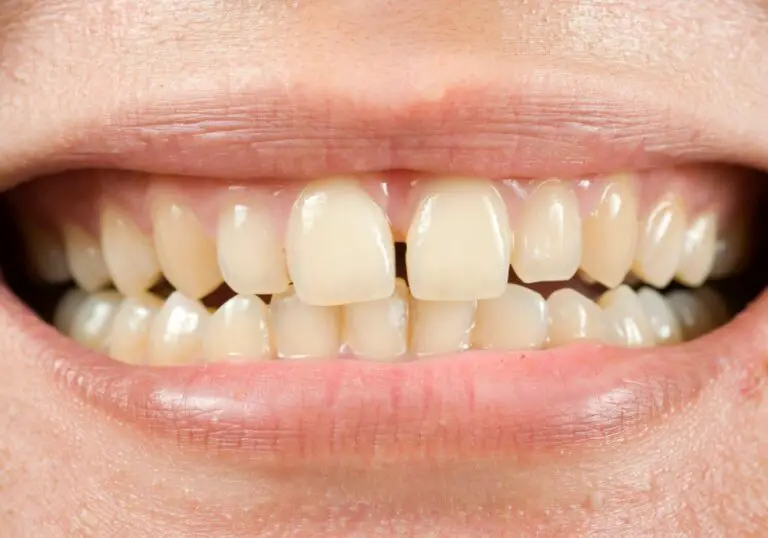
Cavities, also known as dental caries or tooth decay, refer to holes or structural damage that forms in the hard outer enamel layer of the teeth. Cavities begin when acids produced by oral bacteria begin dissolving minerals from the teeth’s enamel coating. If left untreated, cavities can progressively eat away at the enamel and penetrate deeper layers of the tooth, eventually causing severe infection and tooth loss.
What Causes Cavities?
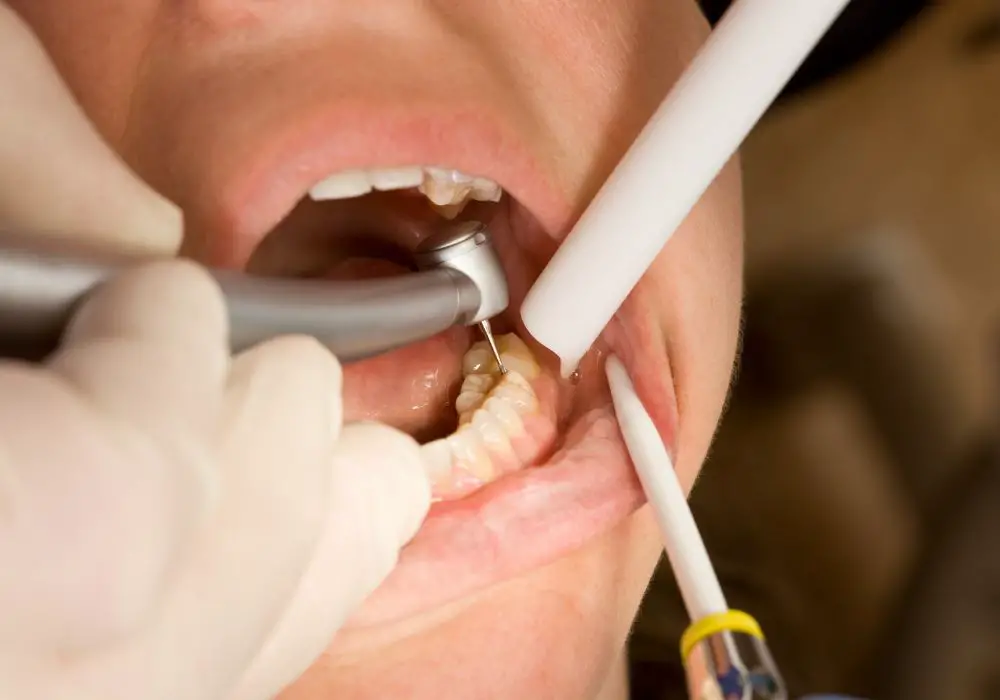
The cavity formation process
The formation of cavities involves the complex interplay between specific bacteria, dietary carbohydrates, saliva composition, and tooth anatomy. Here is an overview of the cavity formation process:
- Bacteria accumulation: After eating sugary or starchy foods, remnants get left behind on the teeth’s surfaces. This allows bacterial biofilms called plaque to build up. The most cariogenic (cavity-causing) bacteria include Streptococcus mutans and Lactobacillus acidophilus.
- Acid production: The bacteria within plaque metabolize carbohydrates and produce acids like lactic acid as a byproduct. The most troublesome sugars are sucrose, fructose, and glucose.
- Demineralization: These plaque acids diffuse into the tooth’s enamel layer and dissolve the hydroxyapatite mineral crystals. This causes subsurface lesions and tiny pores to form – the first stage of cavity development.
- Remineralization: Saliva contains minerals like calcium and phosphate that can diffuse back into the porous regions and rebuild the enamel before a cavity forms. The balance between acid attacks and remineralization determines cavity progression.
- Cavitation: As acid attacks become more frequent, remineralization cannot keep up. The pores grow larger and eventually form a hole penetrating through the enamel – a cavity is now established. The decay front continues advancing into inner dentin.
- Bacterial ingress: Once a cavity breaks through the enamel barrier, bacteria start invading deeper tooth layers. Their acids and toxic byproducts irritate and inflame the inner pulp tissue.
- Abscess and necrosis: Finally, the pulp infection can spread through the root canal system and form abscesses. The pulp tissue dies, leaving the tooth nonviable.
Key risk factors for cavities
Several risk factors can tip the balance in favor of demineralization and increase someone’s susceptibility to cavities:
- Poor oral hygiene – Inadequate brushing and flossing allows plaque to accumulate and thrive.
- Frequent snacking – Constant snacking and sipping of sugary foods or drinks frequently drops pH and decalcifies enamel.
- Reduced saliva flow – Saliva helps neutralize acids and provide mineral ions. Insufficient saliva removes this protective effect.
- Enamel defects – Thin spots, pits, or grooves in enamel allow bacteria to penetrate more easily. Genetics can make enamel formation imperfect.
- Bad biting alignment – Crooked teeth or misaligned jaws create traps for plaque and food to collect.
- Dry mouth-causing medications – Hundreds of medications like antihistamines, antidepressants, and pain pills reduce saliva output.
- High numbers of cariogenic bacteria – Some people have higher baseline levels of cavity-causing bacteria that are more acidic.
Do Cavities Heal Naturally Without Treatment?
Unfortunately, cavities will not heal or remineralize on their own once a definitive hole has formed through the enamel layer. The reason cavities do not repair themselves comes down to the composition of enamel:
- Enamel is an acellular tissue, meaning it lacks any living cells. Other tissues like skin and bone contain cells that can regenerate and heal damage.
- Enamel lacks blood vessels. Therefore, it cannot recruit cells or factors from the bloodstream to drive regeneration.
- Enamel contains hydroxyapatite crystals that give teeth their hardness and help prevent decay. However, once acid corrosion has dissolved away hydroxyapatite, spontaneous remineralization cannot replenish it.
In the early stages before a cavity forms, limited remineralization and arresting of lesions may occur. But once cavitation happens, the decay process becomes virtually irreversible. Studies show that 97% of cavities will continue to expand without professional intervention.
While some early-stage lesions may harden and turn brown or black, this arrested decay does not indicate true healing. These darkened lesions are stuck in an inactive phase but can easily reactivate in the future if the oral environment becomes more favorable to acid attacks.
Overall, cavities require direct professional treatment like fillings, crowns, or root canals to stop lesion progression. The idea of “healing cavities naturally” using diet or alternative therapies is currently unsupported by scientific evidence.
Conventional Treatments Used by Dentists for Cavities
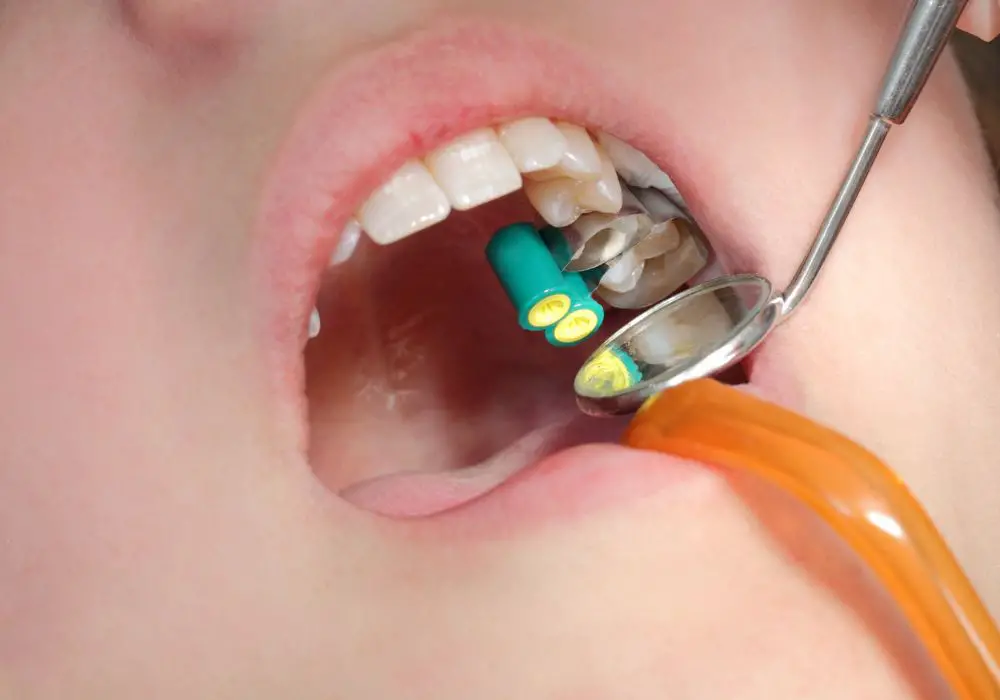
Modern dentistry offers several effective approaches to treat existing cavities and replace lost tooth structure:
Dental Fillings
Dental fillings involve cleaning out the decayed material from within a cavity using a dental drill. The space is then filled with a synthetic biocompatible material to seal up the lesion. Fillings act as substitutes for the missing enamel and dentin. The two main types are:
- Amalgam fillings – An alloy containing about 50% elemental mercury combined with silver, copper, tin, and zinc. Amalgams hold up well to chewing stresses but are less aesthetically appealing.
- Composite resin fillings – Made of glass or quartz particles embedded within an acrylic polymer matrix. Composites can be color-matched but aren’t as durable.
After numbness sets in, the decay is excavated and the tooth conditioned. The liquid amalgam or composite resin is applied to the cavity and shaped. As it hardens, the material bonds firmly to the tooth walls and closes off the lesion.
Dental Crowns
When cavities are extremely severe and encompass multiple tooth surfaces, a filling may not be strong enough. Dental crowns offer full-coverage protection.
The dentist reshapes the damaged tooth to a peg so a cap can fit over it. An impression is taken and sent to a lab for crown fabrication. The custom-designed crown is cemented onto the prepared tooth during a follow-up visit.
Crowns are made of porcelain, ceramic, metal alloys, or a combination. They fully surround the visible portion of the tooth down to the gum line, guarding against fracture.
Root Canal Treatment
If tooth decay compromises the blood supply in the pulp tissue inside, root canal therapy is required. This involves:
- Accessing the pulp chamber
- Removing infected/inflamed pulp
- Disinfecting the root canals with instruments
- Filling and sealing the root canal system
Finally, a crown is placed for reinforcement. Together, the root canal procedure and crown save the tooth and prevent extraction.
Outcomes For Saving Teeth With Existing Cavity Damage
The prognosis for maintaining a tooth with cavities is very positive if appropriate professional treatment is carried out in a timely manner. With today’s dental techniques, the vast majority of cavitated teeth can be restored and protected against further decay.
However, the more severe the decay, the poorer the long-term survival. Extensively damaged teeth may become non-restorable and require extraction if:
- Caries has extended near the tooth’s nerve or pulp chamber
- Periodontal disease has weakened surrounding bone support
- The remaining tooth structure is inadequate to hold a filling or crown
Regular dental exams and prompt treatment ensure cavities are caught early when conservative therapies like simple fillings have the highest chance of success. Allowing rampant, neglected decay to spread puts teeth at serious risk.
With diligent oral hygiene and consistent dental care, patients can conserve their natural dentition for life despite previous cavity development. The adage that cavities inevitably lead to tooth loss is outdated – the vast majority can be arrested and maintained.
Common Questions Patients Have About Cavities:
Q: What are the most common signs and symptoms of a cavity?
A: Early cavities may produce no obvious symptoms. As they enlarge, common signs include toothache, sensitivity to hot/cold, visible pits or holes in enamel, discoloration, spontaneous pain indicating pulp inflammation, and food packing between teeth.
Q: How fast do cavities progress if left untreated?
A: The rate of cavity progression varies based on multiple factors like diet, bacteria levels, saliva pH, and enamel thickness. However, on average, an untreated cavity may take 1 to 2 years to reach the inner pulp chamber, turning into a dental emergency.
Q: Can cavities be prevented through dietary changes?
A: Reducing sugar intake, minimizing acidic beverages, and limiting frequent snacking can help reduce cavity risk. However, cavities cannot be entirely prevented through diet alone. Excellent oral hygiene and professional care are also required.
Q: Can cavities go away if I brush and floss better?
A: Unfortunately, existing cavities cannot be brushed or flossed away once enamel has actually broken down. However, improving oral hygiene can prevent new cavities from forming and slow the progression of existing ones.
Q: Do all cavities require traditional fillings?
A: No, early-stage cavitated lesions and non-cavitated lesions may be arrested with techniques like intensive fluoride therapy. However, once they advance beyond the enamel, fillings become necessary to stop decay.
Q: Can cracked teeth always be saved?
A: Minor chips and cracks can often be restored with dental bonding, veneers, or crowns. But severely fractured teeth with pulp exposure ultimately require extraction if the remaining tooth structure cannot support a proper restoration.