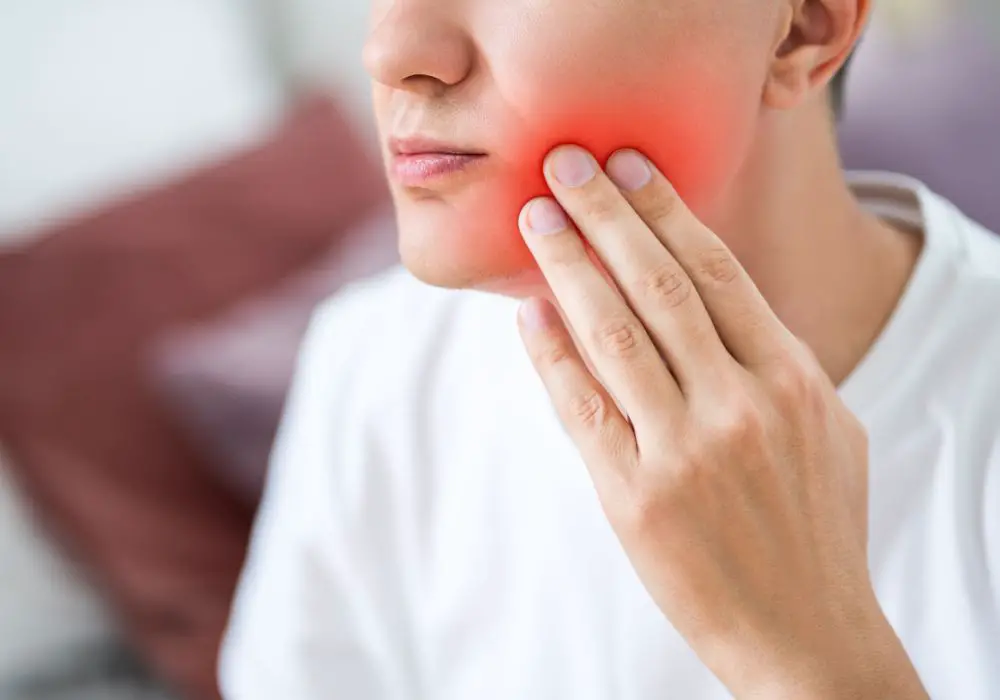
Pain or discomfort near your wisdom teeth can have a variety of causes. Your wisdom teeth, or third molars, are the last teeth to erupt in your mouth, usually between the ages of 17 and 25. They are located at the very back of your mouth in the upper and lower jaws. As wisdom teeth begin pushing through the gums and erupting, they may cause pain as they put pressure on surrounding teeth, nerves, and tissue. Even after wisdom teeth are fully erupted, pain may occur due to problems like infection, decay, or damage to nearby structures. Understanding the common causes of wisdom tooth pain and discomfort can help you determine when and how to seek treatment for relief.
Overview of Wisdom Teeth Pain
Causes
- Pericoronitis (infection in gum tissue around partially erupted tooth)
- Tooth eruption through gum
- Impacted or partially erupted wisdom teeth putting pressure on nearby teeth/structures
- Cavities or tooth decay
- Cysts or tumors around wisdom teeth
- Damage to nerves
- Food impaction between teeth or under gum flaps
- Bruxism or teeth grinding
Symptoms
- Swelling, redness, bleeding in gum near wisdom tooth
- Pain or throbbing around wisdom tooth area, often worse with chewing
- Sensitivity to hot/cold in nearby teeth
- Bad breath or unpleasant taste in mouth
- Headache, earache, sinus pressure from referred pain
- Jaw pain or stiffness, difficulty opening mouth fully
- Numbness, tingling, or shooting pains in face, lips, tongue
Risk Factors
- Poor dental hygiene and plaque buildup
- Smoking or tobacco use
- History of chronic infections or gum disease
- Orthodontic work like braces or crowding
- Older age (wisdom teeth often erupt late teens/early 20s)
- Genetics or small jaw structure
Diagnosis
- Dental exam, x-rays to visualize wisdom teeth
- Assessment of gum swelling or infection
- Biting and occlusion evaluation
- Allergy testing if pericoronitis recurs
Treatment
- Wisdom tooth extraction
- Drainage and antibiotics for infections
- Pain medication, anti-inflammatories
- Salt water rinses, mouthwash
- Dental work if cavities or decay present
- Surgery for cysts, tumors, impaction issues
Prevention Tips
- Proper oral hygiene with brushing, flossing, and mouthwash
- Regular dental cleanings and checkups
- Stop smoking and tobacco use
- Soft diet after wisdom tooth eruption
- Stress management techniques
Common Causes of Wisdom Tooth Pain
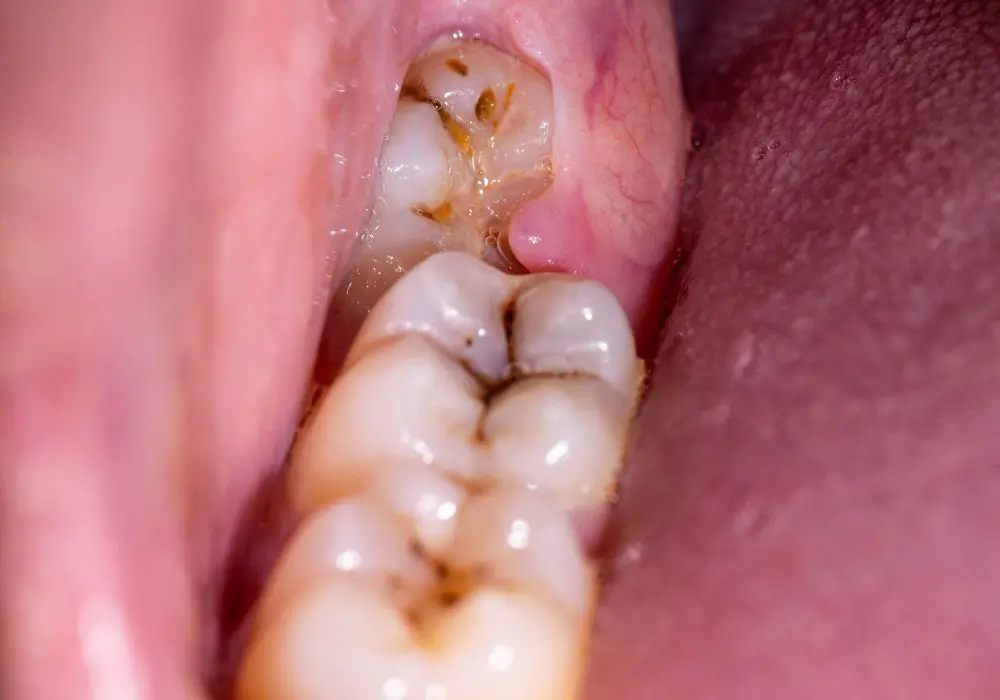
Pericoronitis
Pericoronitis refers to inflammation and infection of the gum tissue surrounding a partially erupted wisdom tooth. Food, bacteria, and dead cells can become trapped under the flap of gum tissue overlying an erupting wisdom tooth. This causes swelling of the gum flap, infection, and intense pain when chewing or biting down.
Symptoms of pericoronitis include:
- Bright red, swollen gums around the tooth
- Severe throbbing pain, especially when chewing
- Pain that radiates to ear, jaw, and side of face
- Bad breath or putrid taste from the infection
- Lymph node swelling and fever if infection spreads
Treating pericoronitis involves:
- Salt water rinses after meals to keep area clean
- Antibacterial mouthwash to reduce bacteria under gum flap
- Antibiotics to clear up bacterial infection
- Removal of any food debris trapped under gum flap
- Extraction if the problematic wisdom tooth cannot erupt fully
Pericoronitis commonly recurs until the wisdom tooth is extracted or fully erupts. Regular dental x-rays can help monitor for partial eruption issues.
Tooth Eruption Through Gum Tissue
As wisdom teeth begin pushing through the gums, the razor-sharp edges of the emerging tooth slice through gum tissue. This can cause inflammation, swelling, and throbbing pain as the tooth erupts.
Symptoms from erupting wisdom teeth may include:
- Sharp pain when biting down
- Sore, tender gums around the tooth
- Metallic taste from blood mixing with saliva
- Headache or jaw soreness from referred pain
Discomfort usually peaks in the first 24-48 hours as the tooth emerges. Pain management strategies include:
- Salt water rinses to keep area clean
- Over-the-counter pain medicine like ibuprofen
- Apply cold compresses to outside of cheek
- Soft diet until tooth fully erupts through gum
See your dentist if pain lasts more than a few days or worsens. This may indicate an infection or problem with wisdom tooth impaction.
Impacted or Partially Erupted Wisdom Teeth
Impacted wisdom teeth are unable to fully break through the gums due to obstruction from other teeth or lack of sufficient jaw space. Partially erupted wisdom teeth get “stuck” partway through the gums. Pressure from impacted or partially erupted wisdom teeth can damage nearby teeth, bone, and nerves. This can lead to symptoms like:
- Red, swollen gums around the impacted tooth
- Jaw pain or stiffness that worsens with chewing
- Headaches and tooth sensitivity as teeth get pushed together
- Changes in bite alignment as teeth shift position
- Numbness or tingling of the tongue, lips, and chin
Bacteria and food debris easily become trapped around impacted wisdom teeth, increasing infection risk. Extraction is often necessary for impacted wisdom teeth to prevent decay, cysts, and other complications.
Cavities and Tooth Decay
Like any tooth, wisdom teeth are at risk for tooth decay and cavities due to buildup of plaque and tartar around the tooth surface. Lack of good oral hygiene makes wisdom teeth especially prone to decay. Signs of wisdom tooth decay include:
- Pain when eating or drinking hot, cold, or sweet foods
- Sensitivity to air hitting the tooth
- Constant, throbbing pain not relieved by removing stimulus
- Bad breath and white spots on tooth enamel
- Gum inflammation around the tooth
Early wisdom tooth decay can often be treated with fillings if accessible. Heavily decayed wisdom teeth likely require extraction.
Cysts and Tumors of Jaw/Gums
Cysts or tumors can rarely develop around wisdom teeth and press on surrounding nerves, tissues, and bone. Dentigerous cysts form around the crown of an impacted wisdom tooth, enclosing it in a fluid-filled sac. Odontogenic tumors start in the tooth-producing cells of the gums and jaw. Symptoms may include:
- Jaw pain or swelling that worsens gradually
- Pus discharge and foul odor from the gums
- Teeth feeling loose or separated
- Difficulty opening mouth fully
- Numbness or tingling in the face, lips, tongue
- Headache and sinus pressure from a growing mass
Dentists can perform biopsy tests to determine if a growth is a benign cyst or concerning tumor. Treatment requires surgical removal of any wisdom teeth involved along with the cyst or tumor.
Nerve Damage
The inferior alveolar nerve runs in close proximity to the roots of lower wisdom teeth. Impaction problems during tooth eruption can sometimes damage this nerve. Symptoms of nerve injury include:
- Numbness or loss of sensation in lower lip, chin, and/or tongue on the affected side
- Tingling, burning, or “pins and needles” sensations
- Increased sensitivity and pain (hyperesthesia) over time
Nerve damage may occur suddenly during wisdom tooth removal or extraction. It can also develop gradually later on, even years after wisdom teeth are erupted. Extraction often becomes necessary to relieve nerve impingement causing numbness or pain. Nerve symptoms may be temporary or permanent.
Who is at Risk for Wisdom Tooth Pain and Complications?
Certain factors may increase your risk of problematic wisdom teeth and related pain:
- Poor dental hygiene – Inadequate brushing and flossing raises your risk of tooth decay and gum disease with wisdom teeth or pericoronitis.
- Tobacco use – Smoking impairs healing after extractions, increasing the risk of painful dry socket. It also worsens gum disease.
- Existing dental issues – Having crowded, crooked, or missing teeth makes wisdom tooth impaction and maleruption more likely.
- Jaw size/structure – Insufficient space in the jawbones increases impaction risk. Small jaw shape is often genetic.
- Older age – Wisdom teeth left unerupted into the 20s and beyond are more likely to become impacted or decayed.
- Chronic illnesses – Conditions like diabetes or immune disorders increase susceptibility to infections like pericoronitis.
- Medications – Certain drugs like steroids or bisphosphonates can lead to jaw bone problems and poor healing.
Consult your dentist promptly if you notice any symptoms of wisdom tooth pain or infection. Extraction is often advised for high-risk patients to prevent complications.
How are Wisdom Tooth Problems Diagnosed and Treated?
If you are experiencing pain near your wisdom teeth, see your dentist for proper diagnosis and treatment. Be prepared to describe your symptoms, timeline, and pain triggers. Diagnostic measures may include:
Clinical examination – Your dentist will check for redness, swelling, decay, or gum disease around wisdom teeth. They may press on your jaw to test for tenderness.
Imaging – X-rays, CT scans, or MRIs are done to evaluate wisdom tooth position, impaction, root development, and signs of cysts or tumors.
Bite evaluation – Your dentist may have you bite down on a stick-like tool to check your occlusion with wisdom teeth present or absent.
Allergy testing – For recurrent pericoronitis, you may be tested for allergies to certain proteins in plaque that may contribute to gum inflammation.
Biopsy – A small sample of tissue from a cyst or growth may be sent for laboratory analysis to rule out cancer.
Based on the exam findings, your dentist will recommend appropriate treatment, which may include:
- Salt water rinses and mouthwash to keep area clean
- Antibiotics to treat infections or steroids to reduce swelling
- Pain or anti-inflammatory medications
- Dental work like fillings if cavities are present
- Wisdom tooth extraction or surgical removal
- Referral to an oral surgeon for complex impactions
Be diligent with post-procedure instructions to support healing. Call your dentist if you have signs of complications like excessive bleeding, swelling, fever, or uncontrolled pain. Proper diagnosis and treatment can effectively resolve most wisdom tooth problems.
Frequently Asked Questions
What home remedies provide relief for wisdom tooth pain?
Saline rinses, cold compresses, cloves or clove oil, and over-the-counter pain relievers can temporarily alleviate wisdom tooth pain and inflammation. But see a dentist to address the underlying problem.
Should you have wisdom teeth removed if they are fully erupted and painless?
Though wisdom teeth may seem problem-free initially, partially erupted or impacted wisdom teeth often worsen with time. Most dentists recommend extraction in the teen years before impaction complications occur.
How long does wisdom tooth extraction pain last?
It is normal to have some discomfort for 3 to 5 days after extraction. Pain or swelling lasting over 1 week may indicate complications like infection or dry socket and warrants a dental follow up.
When should you go to the emergency room for wisdom tooth pain?
Seek emergency care for uncontrolled bleeding from the surgery site, difficulty swallowing or breathing, severe swelling in the face or neck, fever over 101 F, or uncontrolled pain. These may indicate a serious problem.
Can wisdom teeth re-erupt after being extracted?
Wisdom teeth do not normally re-grow if the extraction removes all tooth fragments and the dental follicle surrounding the crown. Residual tissue left behind can sometimes allow re-eruption, requiring further surgery.
Conclusion
Wisdom tooth pain most commonly results from pericoronitis, eruption through gum tissue, or impaction. Cavities, cysts, nerve damage, and other problems can also occur. Seeking prompt dental assessment and appropriate treatment like antibiotics, extraction, or dental work can help resolve wisdom tooth pain and prevent serious complications like infections or tumors. Maintaining excellent oral hygiene and regular dental checkups is crucial for minimizing issues with wisdom teeth, even after full eruption. Addressing problems early is key to avoiding more complex tooth extractions later on.