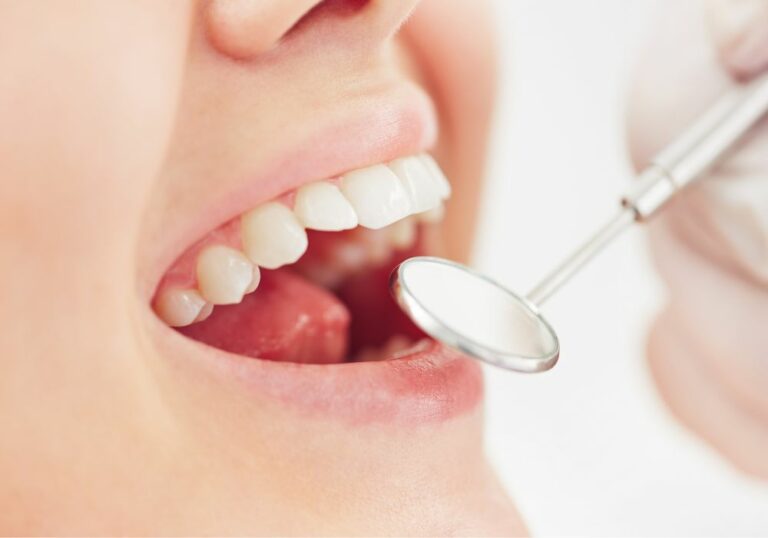
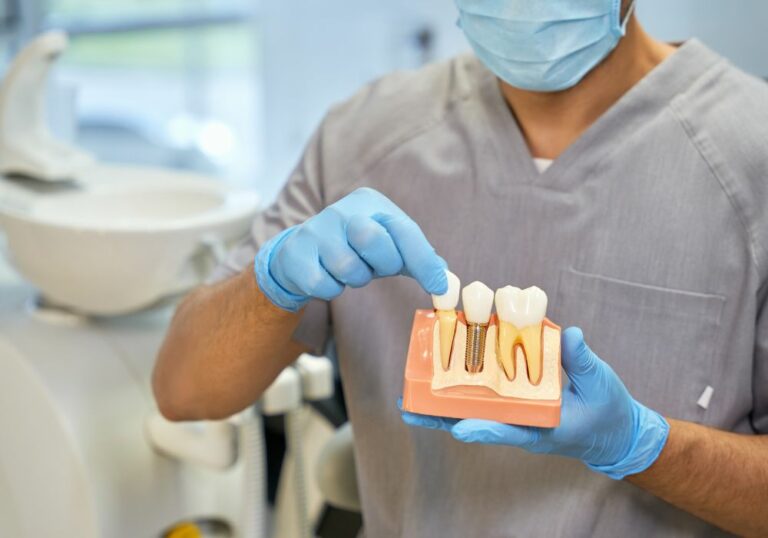
What are dental cavities and tooth decay?
Dental cavities, also known as caries or tooth decay, are holes in teeth caused by deterioration of the tooth enamel (outer layer). Enamel erosion occurs when acids produced by plaque bacteria dissolve the minerals in the teeth. This leads to softer, weakened areas that develop into cavities or tiny holes in the teeth.
Cavities can range in severity from mild (surface level) to deep (affecting inner layers or pulp). Mild cavities are small, beginning lesions that only involve the enamel. Once they reach the second layer, dentin, they become moderate cavities. Severe cavities have penetrated through the dentin to reach the inner pulp layer.
Without treatment, cavities become larger infections that can damage teeth and supporting bone structures. As they grow, cavities compromise more and more of the tooth surface and underlying layers. This can lead to pain, tooth fracturing, and eventually loss of the tooth entirely.
What causes cavities to form?
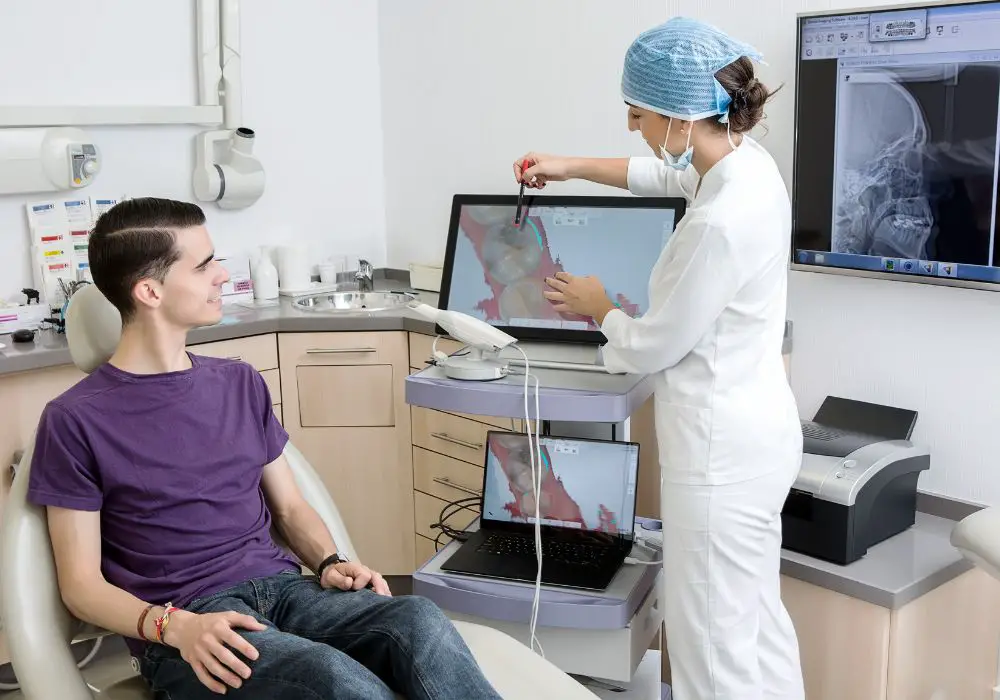
Several factors influence cavity development:
Bacteria
Plaque, a sticky film containing millions of bacteria, constantly forms on teeth. Certain bacteria like Streptococcus mutans and Lactobacillus are most associated with cavities. They produce acids that dissolve enamel. The more frequent and prolonged the acid attacks, the more likely cavities will occur.
S. mutans adhere strongly to teeth and metabolize sucrose (table sugar) into lactic acid. Lactobacillus also generate significant acid. These bacteria thrive and multiply when fed by sugary and starchy foods in the diet. It only takes 24 hours for populations to expand in the presence of fermentable carbohydrates.
Sugary Foods
Sugary foods like candy, cookies, soda, and even fruits provide fuel for acid-producing plaque bacteria. Sucrose, glucose, and fructose are metabolized by bacteria through glycolysis and other pathways, producing lactic acid as a byproduct. The greater the sugar quantity and frequency of intake, the higher the decay risk.
Sticky candies and dried fruits are especially harmful, as they cling to teeth longer and provide prolonged acid exposure. Hard candies also dissolve slowly, bathing teeth in sugar that gets metabolized to acid. Frequent sugar intake keeps acid levels high and promotes demineralization.
Dry Mouth
Saliva washes away food particles and neutralizes plaque acids. Normal resting saliva pH is around 6.5-7, which buffers acids. When saliva flow is reduced or altered, acid can linger near enamel longer and cause more extensive erosion. Dry mouth promotes an environment conducive to caries formation.
Certain medications, radiation therapy, medical conditions, aging, anxiety, and lifestyle factors can cause chronic dry mouth or xerostomia. The lack of lubricating saliva accelerates decay, as acidic biofilm remains on enamel longer. Proper hydration and saliva substitutes can help combat a harmful dry mouth.
Poor Oral Hygiene
Toothbrush bristles cannot reach into deep grooves, crevices between teeth, or along the gumline. Plaque buildup in these areas leads to cavities. Insufficient brushing and flossing allows bacteria colonies to thrive and produce enamel-damaging acids.
If plaque remains for over 48 hours, the bacteria begin to generate extracellular polymers that form a biofilm matrix. These stickier biofilms tightly adhere to teeth and protect acidogenic bacteria. Regular brushing and flossing removes plaque before it becomes highly acidic and cavities develop.
Enamel Defects
Thin, weak spots in enamel make teeth more prone to acid dissolution. Enamel damage can occur from birth defects, malnutrition, trauma, gastroesophageal reflux disease, or other conditions. Teeth with enamel defects have increased cavity susceptibility in affected areas.
The enamel surface normally protects dentin from rapid decay. But thinner or eroded sections permit acid penetration to the more porous dentin, enabling lesions to expand quickly into the tooth interior. This leads to larger cavities requiring more extensive restoration.
Deep Fissures and Pits
The chewing surfaces of back molar and premolar teeth contain deep fissures or pits that can trap food debris and plaque. These recessed grooves provide the perfect habitat for cariogenic bacteria to multiply unseen and cause decay. Their shape makes them difficult to clean thoroughly each day.
The crevice anatomy shelters S. mutans and lactobacilli that ferment carbohydrates sitting in the pits. Chewing forces food particles deeper into fissures. Without diligent oral hygiene, bacteria thrive and produce sustained acid that erodes vulnerable enamel within these protected sites.
Orthodontic Appliances
Braces, clear aligners, retainers, and other orthodontic appliances create areas near brackets or bands that are hard to clean. Extra plaque buildup around these appliances raises the likelihood of white spot lesions and decay during and after treatment.
The added surface area and intricate edges of brackets/wires provide more area for plaque to adhere. Food particles get caught readily. Patients must take extra care to brush thoroughly around orthodontics and avoid excess sweets to control acid attack.
Medications
Hundreds of common prescriptions like antihistamines, decongestants, pain pills, diuretics, antidepressants, sedatives, Parkinson’s medications, and others reduce saliva flow. Without sufficient saliva washing and lubricating the teeth, plaque acid can erode enamel longer. This medication-related dry mouth leads to more cavities.
Some medications also contain sugars that get metabolized to acid. Liquid medicines and chewable pills with sucrose promote higher streptococcal counts. Consult a dentist and doctor to find alternative meds without these side effects if possible.
Medical Conditions
Diseases and disorders that cause chronic dry mouth make patients very susceptible to rapid decay. Sjogren’s syndrome, diabetes, Parkinson’s disease, eating disorders, cystic fibrosis, yeast infections, and autoimmune disorders all influence oral environment.
Cavities develop readily without adequate saliva to wash away acid and food debris. Often these patients take multiple medications that compound the problem. Working closely with medical providers to improve hydration, saliva production, and oral pH helps control this increased risk.
Substance Abuse
Drug and alcohol abuse are linked to poor oral hygiene,nutrition, and dental care. Methamphetamine is notoriously devastating, as “meth mouth” rots teeth from a combination of decay and grinding. The drug is acidic itself, while also causing dry mouth and sugar cravings. Opioids reduce saliva and make patients less aware of oral health.
Additionally, chronic use of alcohol, marijuana, and tobacco all slow saliva flow. Smoking allows more plaque to collect and converts saliva pH to the acidic range. Those dealing with addiction issues often neglect hygiene and experience rampant cavities, gum disease, and tooth loss.
Why are some people more prone to cavities than others?
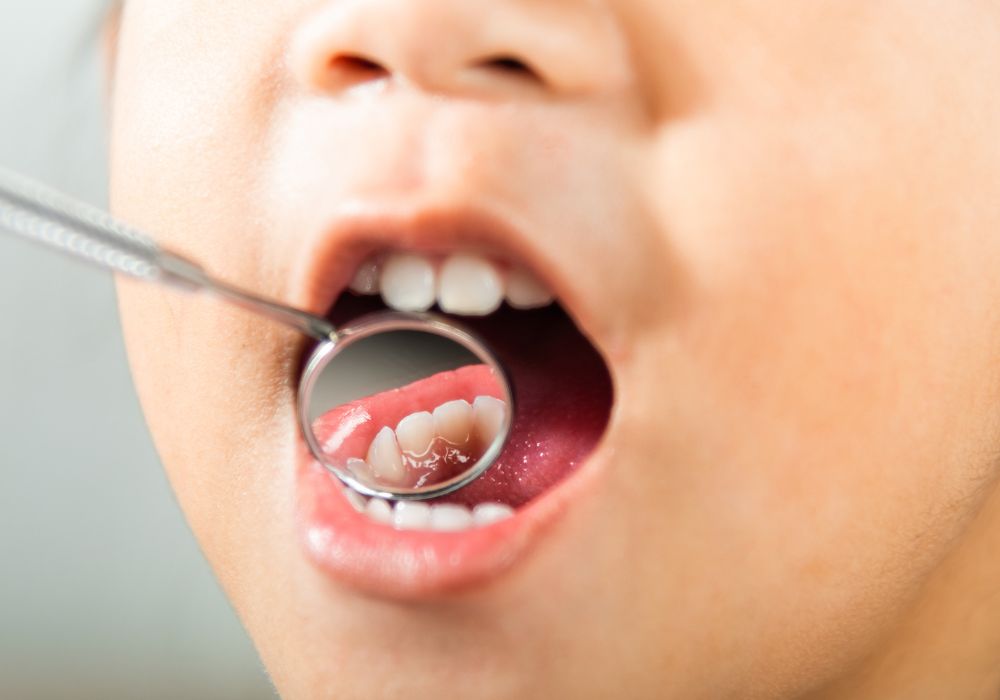
While all people are susceptible to cavities, certain individuals have higher risk with more frequent decay:
Tooth Structure
Some individuals naturally have softer enamel that demineralizes faster when exposed to oral acids. Enamel thickness, porosity, and mineral content varies, affecting cavity susceptibility. The quality of tooth structure you are born with impacts decay risk. Premolars often have higher rates of cavities than other teeth.
Saliva Composition
Saliva contains crucial minerals like calcium, phosphate, and fluoride that rebuild and strengthen enamel after acid attacks. It also has buffering capacity to neutralize acids. People with lower calcium and phosphate counts have reduced remineralization capacity and higher decay rates. Some have saliva that does not effectively regulate pH.
Diet and Snacking Habits
Frequent intake of sugary or acidic foods and drinks substantially elevates caries risk. Starchy processed snacks like crackers and chips also promote cavities by sticking to teeth longer. Excessive snacking creates repeated acid attacks without recovery time. Limiting fermentable carbohydrates is beneficial.
Oral Hygiene Habits
Failing to brush properly at least twice a day or clean between teeth with floss allows plaque to thrive unchecked, especially in hard-to-reach areas. Poor oral hygiene provides optimal habitat for increasing bacterial populations. Deliberate oral care, especially after meals and sugary snacks, reduces acids.
Genetic Factors
Research suggests certain people may have a genetic predisposition to weaker enamel or teeth more prone to decay. However, genetics alone without poor diet and oral hygiene seldom causes rampant cavities. Lifestyle and behavior often override genetic susceptibility.
Age Extremes
Very young children who lack motor dexterity and oral awareness tend to get more cavities. Elderly adults also have higher rates due to medication-related dry mouth, gingival recession, and inability to practice effective hygiene. The very old and very young have more difficulty controlling dietary and brushing habits.
What are signs and symptoms of a cavity?
Cavities produce a variety of warning signs and symptoms depending on their severity, location, and extent of nerve involvement:
- Toothache – Sharp pain when eating or drinking something sweet, hot, or cold. Pain is acute at first, then lingers for several seconds or more.
- Tooth sensitivity – Brief, sudden tooth pain from hot, cold, sugary, or acidic foods and drinks. Sensitivity to pressure or temperature changes when chewing.
- Visible pit/hole on tooth surface – Appears as a dark brown, black or chalky white spot. Cavity is visible as damage penetrates through enamel into dentin.
- Pain when biting down – Ache or discomfort when teeth make contact during chewing or eating. Pain when releasing bite pressure.
- Lingering pain after removing stimulus – Tooth discomfort continues for a time after irritant is gone.
- Gum inflammation – Red, swollen, or tender gums near affected tooth. Sign of spreading infection.
- Halitosis – Foul odor on breath from pus discharge associated with an abscess.
- Loose teeth – Advanced infection causing supporting bone loss and tooth mobility. Tooth feels slightly wobbly.
- Sinus symptoms – Infection from an upper tooth can cause sinus pressure, congestion, and facial pain.
- Difficulty eating – Discomfort or pain while chewing hard or crunchy foods due to significant decay.
- No symptoms – Early and middle stages of caries often produce no noticeable symptoms, making examination important.
How are cavities diagnosed?
Dentists use a combination of the following methods to detect and diagnose caries:
- Visual exam – Carefully scanning all tooth surfaces and probing with an explorer tip for holes, cracks, or soft spots. Staining solutions can help reveal early demineralization.
- Dental x-rays – Bite wing x-rays show decay between teeth. Panoramic and periapical x-rays visualize deeper lesions. Helpful for identifying small or hidden areas of decay.
- Fiber-optic transillumination – Bright light is directed on the tooth to detect subtle shadows indicating subsurface decay.
- Fluorescence detection – Using laser fluorescence to measure enamel hardness and detect softer, demineralized areas indicating early caries.
- Electrical conductance – Testing differences in conductance between sound enamel and decayed areas. Decay conducts less electricity.
- Tactile probing – Use of dental explorer on tooth surfaces to feel for stickiness or softening.
Assessing caries risk factors also influences diagnosis. Past decay rates, diet, medications, and hygiene habits give insight into susceptibility. Diagnostic data guides appropriate treatment for each patient’s needs and cavity severity.
What are the stages of cavity progression?
Cavities begin as microscopic lesions that enlarge gradually if unchecked. The stages of cavity progression include:
Early – Surface demineralization just in enamel. Appears as faint white spot lesion. Often asymptomatic. Reversible at this stage through remineralization.
Moderate – Enamel cavity extending into dentin layer. Light-medium brown area visible on tooth surface. Tooth may become mildly sensitive. Restorable through fillings.
Advanced – Large cavity penetrating deep into inner dentin, nearing pulp. Tooth structure is severely undermined. Pain, infection, abscesses occur. Still restorable in many cases via root canals.
Severe – Inner pulp chamber infected with irreversible pulpitis. Significant bone loss around tooth. Requires extraction if other treatment fails.
The faster treatment is obtained, the better chance of reversing the decay or minimizing tooth damage. Catching lesions early prevents the extensive destruction seen in advanced cases.
How are cavities treated?
Several effective options exist for treating cavities based on the size and location:
- Fluoride – Fluoride applied professionally or using daily rinses helps remineralize early white spot lesions, preventing progression to cavities.
- Sealants – Plastic coatings adhered to chewing surfaces, sealing off pits and fissures vulnerable to decay. Prevent bacteria harboring.
- Fillings – Removing decayed inner material using a drill and replacing with metal, porcelain, or composite resin material to fill the hole.
- Crowns – Covering severely compromised teeth with artificial caps cemented over them to protect remaining structure. Used when most of original enamel and dentin are damaged.
- Root canals – Removing infected, irreversibly inflamed pulp tissue. Cleaning and sealing interior root canals and chamber. A crown protects the tooth afterwards. Necessary when deep decay extends into pulp.
- Antibiotics – Prescribed short term for abscessed teeth to eliminate infection prior to definitive treatment. Potent topical antibiotics placed directly in certain decayed teeth.
- Extractions – Removing extensively damaged, non-restorable teeth. Remaining bone is smoothed and closed with stitches. The space can be replaced with a bridge, implant, or removable partial denture.
Proper technique with use of dental dams prevents further decay around restorations. Timely diagnosis and treatment ensures cavities are caught before tooth loss occurs.
What is the best way to prevent cavities from forming?
Preventing cavities relies on disrupting disease factors that cause them. Key prevention methods include:
- Brush teeth thoroughly twice daily – reduces acidic plaque bacteria and food debris. Prevent buildup in grooves and near the gumline.
- Floss between all teeth daily – removes plaque from tight contacts where cavities start.
- Use a fluoride toothpaste – fluoride strengthens enamel, making it more acid resistant.
- Limit sugary foods and drinks – reduces fuel for the bacteria to produce enamel-eroding acids.
- Avoid frequent snacking – provides a constant acidic challenge. Limit snacks to mealtimes when saliva flow is higher.
- Rinse daily with fluoridated, antibacterial, pH balancing mouthwash – reduces bacteria counts between brushing.
- Chew xylitol gum – xylitol inhibits S. mutans bacteria that cause cavities. Stimulates saliva.
- Follow a non-acidic diet – avoid acidic foods that erode enamel like citrus, carbonated drinks, and vinegar.
- Get dental cleanings and exams every 6 months – professional calculus removal. Identify lesions early.
- Use prescription strength fluoride if high risk – provides extra protection against demineralization.
Daily oral hygiene plus twice-yearly dental visits offer the best defense against cavities! Catching early lesions and maintaining tooth integrity prevents more complex restorations later on.
Frequently Asked Questions
1. Can cavities remineralize without going to the dentist?
Early stages of decay confined to enamel can remineralize with improved hygiene and fluoride exposure. But once a distinct cavity hole forms, involving the dentin layer, professional intervention is required. Fillings, crowns, or other restoration methods are necessary to remove infection and rebuild the tooth structure.
2. Should I avoid all sweets if I’m prone to cavities?
Complete sugar avoidance is not necessary, but moderation and frequency control is key. Try to limit sugars to mealtimes when saliva flow is higher rather than chronic snacking. Quickly brush after sweets. Focus on fresh fruits over candy and rinse well. Sugars do provide energy, so balance is important.
3. Why do cavities form under fillings and crowns?
Decay recurring under existing restorations is common. Bacteria and debris at the junction between the tooth and filling can still cause acids and decay. Cracked fillings also provide a path for invasion. Getting replacements promptly before more tooth structure is lost is important. Using dental dams during placement protects adjacent areas.
4. Should I take antibiotics for a cavity?
Antibiotics are rarely needed for a typical cavity. However, a large abscess with infection spreading into surrounding oral tissues does require a short course of antibiotics in conjunction with drainage and definitive treatment. Topical antibiotic pastes placed inside deep cavities help eliminate bacteria before restorative work.
5. Can vitamins or supplements help remineralize early decay?
Yes, certain supplements can aid remineralization. Calcium and vitamin D are needed for enamel regrowth. Fluoride rinses, varnish, and toothpastes promote remineralization. Xylitol gum increases saliva flow to enhance the mouth’s natural ability to rebuild minerals. But supplements alone will not reverse established cavities without professional treatment.
6. Why does tooth decay get worse with age?
The cumulative effects of cavity risk factors make teeth more prone to decay as we age. Enamel becomes thinner and more porous over time. Gingival recession exposes more root surface. Older adults often experience dry mouth and take more medications. Manual dexterity declines, so they cannot brush as effectively. However, practicing excellent lifelong hygiene minimizes increased risk.