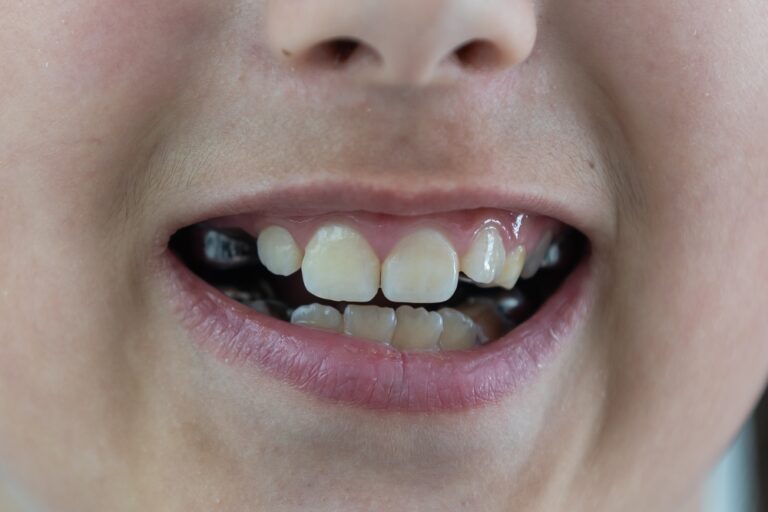
A dead tooth, also known as a non-vital tooth, is a tooth that has undergone pulp necrosis. This means that the soft tissue inside the tooth (the pulp) has died due to infection or trauma. When the pulp dies, the tooth loses its main blood and nerve supply. As a result, it can no longer sense hot or cold temperatures, pain, or perform normal functions like the surrounding healthy teeth.
Some common causes of a dead tooth include:
- Severe tooth decay that reaches the pulp
- Cracks or chips in the tooth that expose the pulp
- Trauma to the tooth, such as a hard hit that disrupts blood flow
- Prior dental procedures like root canals
Over time, a dead tooth that is not treated turns brittle and is prone to fracture. It may change color, often becoming darker than surrounding teeth. The lack of a blood supply also makes a dead tooth more susceptible to infection. That’s why it’s important to get dead teeth treated promptly by a dentist.
Can a dentist detect a dead tooth on an X-ray?
Yes, a dentist can often detect signs of pulp death on an X-ray. Here are some of the key things they look for:
- Loss of bone density: Healthy teeth maintain the surrounding jawbone density. A dead tooth no longer stimulates the bone cells, so density fades on an X-ray.
- Widening of the ligament space: The periodontal ligament anchors the tooth root to the bone. This space widens when the tooth loses vitality.
- Presence of infection: Dying pulps are prone to infection. An X-ray may show signs of infection like cysts or abscesses at the root tips.
- Change in appearance of the root canal: The pulp chamber and root canal system have a distinct radiolucent (dark) appearance on an X-ray when the pulp is alive. Once the pulp dies, the canal may fill with tissue debris that looks irregular.
- External root resorption: This shows up as irregular destruction or blunting of the root tips. It occurs when the body detects the dead tooth and tries to expel it by dissolving the root.
- Presence of filling material or posts: Teeth that have had previous root canal procedures will contain radiopaque filling material or posts that indicate pulp death.
How can a dentist confirm a dead tooth diagnosis?
While X-rays provide very useful information, a dentist will also perform additional tests to confirm that a tooth is non-vital. These include:
- Cold testing: This is done by applying a cold stimulus like chilled air or an ice stick to the suspect tooth. Healthy teeth should sharply sense these temperature changes. Dead teeth will not respond.
- Electric pulp testing: A small electric current is passed through the tooth to stimulate the nerve. Normal teeth will react immediately. Dead teeth will not respond.
- Percussion testing: Tapping lightly on the tooth with a dental instrument. Dead teeth often exhibit exaggerated pain responses.
- Probing the gums: Gum recession and periodontal pockets around dead teeth may indicate infection.
- Staining: A non-vital tooth that is still intact may not change color. But staining agents like methylene blue can often be absorbed into the pores of dead teeth, causing discoloration that confirms loss of vitality.
If a tooth does not respond to any of these tests, the dentist can definitively diagnose it as non-vital and begin planning appropriate treatment.
How is a dead tooth treated by a dentist?
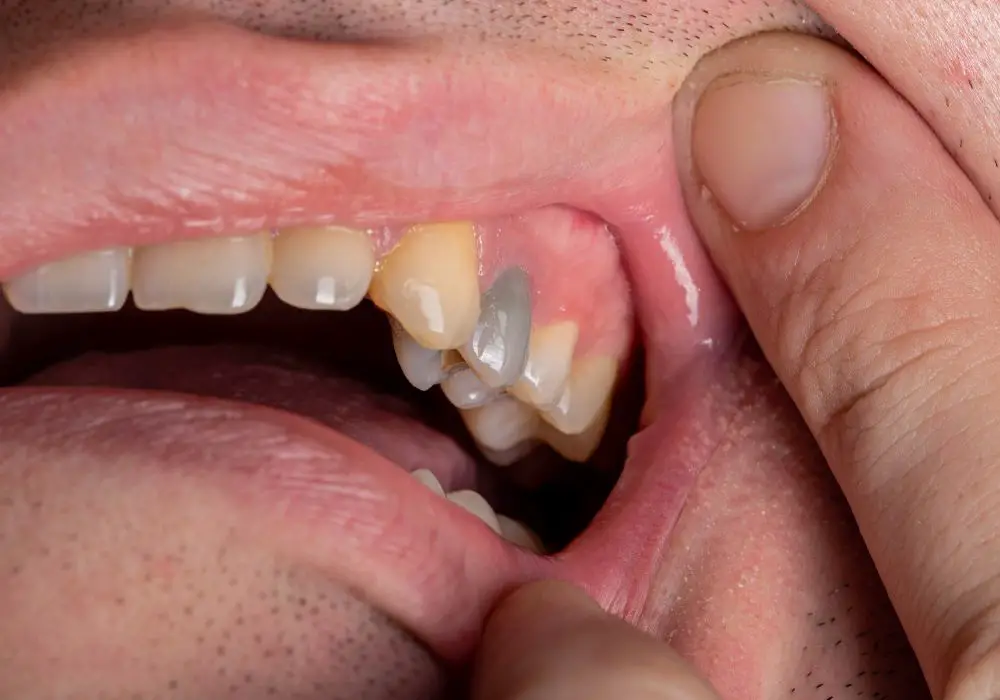
Depending on the severity and the patient’s symptoms, a few treatment options exist for managing a dead tooth:
- Root canal therapy: This is the most common treatment for saving a dead tooth. The dentist drills into the tooth, removes the infected or dead pulp, disinfects and shapes the root canal space, and seals it with filling material. A crown is placed afterward to strengthen the tooth.
- Extraction: Removing the dead tooth is necessary if it is severely damaged or infected. This eliminates the diseased tooth and allows the area to heal. It is later replaced with a dental implant or bridge.
- No treatment: If the dead tooth is free of symptoms and not bothering the patient, a dentist may recommend just monitoring it at regular checkups without treatment. However, risks like fracture and infection remain.
Leaving a dead tooth untreated for a long time can lead to severe pain, dental abscesses, and spread of infection to other teeth and tissues. That’s why prompt care from a dentist is important. With the right treatment, many dead teeth can be restored and retained for years of continued function.
Can a general dentist perform root canal treatment on a dead tooth?
Most general dentists are trained and experienced in performing root canal therapy. However, some patients may be referred to an endodontist, a dental specialist focusing specifically on root canal treatment and pulp care.
Here are some factors a dentist may consider when deciding where to refer a patient for root canal treatment:
- Complexity of the case: Endodontists receive advanced education and treat difficult cases daily. Signs like calcified canals, curved roots, or roots blocking sinus cavities point to specialist care.
- Retreatment cases: Re-doing old, previously filled root canals or treating teeth with posts/crowns often requires an endodontist’s specialized tools and skills.
- Patient needs: Anxious patients or those with extensive dental phobia may be better managed by an endodontist. Their offices offer options like sedation dentistry.
- Special imaging needs: Some complex root canal cases may require 3D imaging like CBCT scans to visualize the anatomy. Endodontists have access to these tools.
- Prior failure: If a general dentist attempted root canal treatment but was unsuccessful in relieving symptoms, an endodontist can revise the case.
However, endodontic referrals are not always necessary. Many general dentists can assess the case, determine their ability to treat it, and perform root canals themselves on teeth with uncomplicated canal anatomy. The key is choosing an experienced clinician you trust to handle your specific needs.
Does a dead tooth eventually fall out on its own?
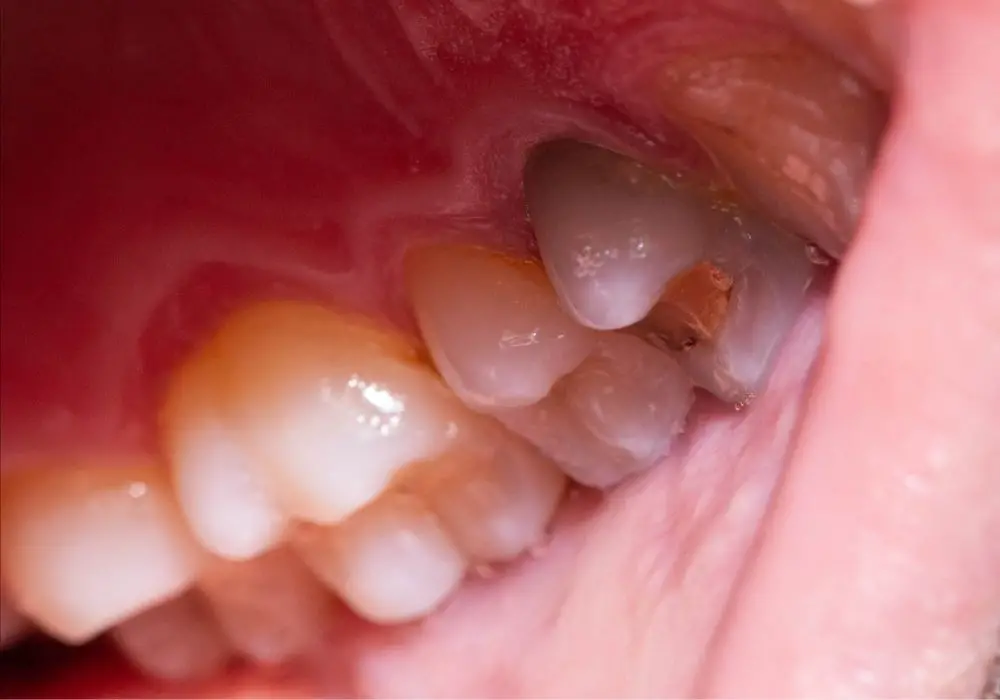
A dead tooth will not simply fall out on its own. It is still anchored in the bone by the periodontal ligament. However, a non-vital tooth that is left untreated for many years may eventually become so weakened or infected that it has to be extracted.
Here is the progression if a dead tooth is not cared for properly:
- Infection worsens: Bacteria invade the vacant pulp space and spread inflammation to the bone around the roots.
- Destruction: The infection causes loss of supporting bone. Pockets form as the ligament detaches.
- Abscess: A pus-filled sac called a periapical abscess develops at the infected tooth’s root tip. Pressure builds.
- Fistula: The abscess may drain its pus by tunneling through the gum, causing a sore called a fistula. More bone loss occurs.
- Loosening: With advanced bone loss, the tooth starts to loosen and detach from its socket.
- Loss of the tooth: Finally, it may fall out or have to be pulled if it is dangerously loose. This process can take many months or even years.
Leaving a dead tooth to reach this level of destruction is never a good idea. It allows the infection to spread and damage other teeth and tissues. That’s why a dentist’s timely intervention is key.
Frequently Asked Questions about dead teeth on X-rays:
Can you tell if you have a dead tooth without seeing a dentist?
Sometimes, if the tooth is discolored or causes exaggerated pain when eating or brushing. But many dead teeth show no obvious outward symptoms. Testing by your dentist is the only way to confirm. An X-ray and clinical exam are needed for a certain diagnosis.
Do dead teeth always turn dark or change color?
Not always. If the tooth still has an intact crown and enamel layer, it may maintain a normal color for some time. Discoloration is more likely if the tooth structure is already compromised by large fillings or cracks that allow staining agents inside the porous dentin layer once the pulp dies.
How fast can an X-ray show a tooth is dying or dead?
It may take some time after pulp death before clear radiographic signs manifest. But within 2-4 weeks, a dentist should start seeing early signs like ligament widening. Severe infections may become rapidly apparent. In other cases, it can take months for abscesses or bone loss to develop and be visible.
Can you save a tooth with a dead nerve and no pain?
Yes, it is still possible to save a tooth even if the nerve is dead and there are no obvious symptoms yet. Performing a root canal promptly to clean out infection and prevent it spreading gives the tooth the best long-term prognosis. Leaving it untreated allows further destruction.
Does a dark spot inside a tooth always mean it is dead?
Not necessarily. Some dark spots visible on X-rays are benign findings like accessory pulp canals or mineralized tissues. There are also natural variations in pulp chamber size. Correlating X-ray findings with clinical tests is needed to determine if a tooth is necrotic. Follow your dentist’s advice regarding any suspicious areas seen.