What Causes a Front Tooth to Decay?
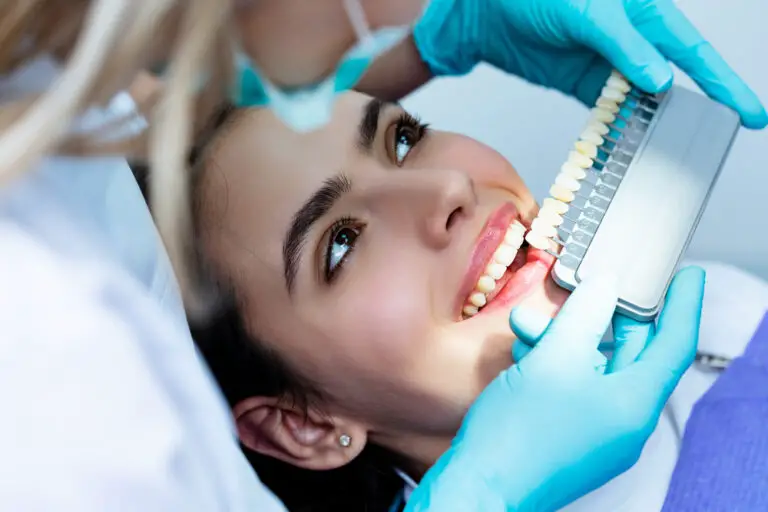
The front teeth are the most visible when we smile and speak. Their health and appearance have a big impact on our confidence. That’s why a decayed or damaged front tooth can be distressing. The good news is that an experienced dentist has several effective options to repair front teeth depending on the extent of the damage.
But before we get into that, what causes a front tooth to go bad in the first place? There are several potential culprits.
Poor Oral Hygiene
This is one of the most common contributors to front tooth decay. When we don’t adequately remove plaque each day by brushing and flossing, it builds up and hardens into tartar. This deposits of plaque and tartar foster growing colonies of bacteria next to the teeth.
Some of these bacteria produce acids as waste products that can dissolve the enamel and matrix of the teeth, leading to caries and cavities. Front teeth are particularly vulnerable as they are the teeth we use most for biting, chewing and tearing food. Food debris tends to collect in nooks and crannies of the front teeth.
Insufficient brushing also allows bacteria to accumulate along the gumline, resulting in inflammation and gingivitis. This can progress to periodontal disease that damages the bones and tissues supporting the teeth.
To avoid decay, the American Dental Association recommends brushing gently twice a day for two minutes with a soft-bristled brush and fluoride toothpaste. Be sure to brush all surfaces – especially just below the gumline. Flossing once daily is also critical to remove plaque between teeth where bristles cannot reach.
Frequent Snacking and Sipping
It’s not just what we eat, but also how often we eat it. Grazing and snacking throughout the day means your teeth are constantly exposed to foods that can damage enamel. Even healthy foods like fruits and yogurt contain acids that soften enamel. Sticky candies cling to teeth surfaces.
Sipping sugary drinks like juices, sports drinks, soda and sweetened coffee exposes teeth to acids and sugars that promote bacteria growth. Each “acid attack” opens pores in the enamel that don’t have time to remineralize before the next snack or beverage. This progressively weakens the structural integrity of enamel, especially near the biting and sipping surface of the front teeth.
Limiting snacks to mealtimes and avoiding constant sipping allows a remineralization period for teeth to recover between eating/drinking events. Drinking water after consuming other beverages can help wash away residue and neutralize acids as well.
Dry Mouth
Saliva sounds like a mere mouth lubricant, but it actually plays a key protective role against tooth decay. It washes away food debris and helps neutralize damaging acids from the foods we eat. Saliva also contains antimicrobial compounds, calcium and phosphate that help reharden and remineralize enamel after acid exposures.
When the quantity or quality of saliva is decreased, teeth are more vulnerable to damage. Hundreds of medications like decongestants, diuretics, antidepressants and pain relievers can interfere with normal saliva flow. Other factors like chronic dehydration, smoking, radiation treatment or health conditions can also cause chronically dry mouth.
Without sufficient lubricating saliva, dry mouth provides an environment ideal for unrestrained bacterial growth, acid attacks andfaster progression of cavities. Experts recommend drinking more water, limiting caffeine/alcohol, chewing sugarfree gum and using a humidifier to moisten air at night to help combat dry mouth.
Aggressive Brushing
You might think you’re doing your mouth a favor by scrubbing extra hard when brushing, but overly vigorous brushing over time can cause enamel damage in a couple ways.
First, it can wear down the protective enamel layer, revealing the softer, more decay-prone layer of dentin underneath. Secondly, aggressive brushing combined with abrasive toothpastes can cause microscopic roughness on the enamel surface that makes teeth more vulnerable to bacterial adhesion and plaque accumulation. This leads to a higher susceptibility to decay.
A gentle, circular massaging motion is recommended, paying close attention to the angulation of bristles to brush just below the gumline without striking the teeth directly. Soft or extra-soft bristle brushes are ideal. An automatic toothbrush with pressure sensors can also help ensure optimal brushing intensity.
Grinding and Clenching
Some people have a habit of forcefully grinding or clenching their teeth, which places heavy wear and tear on the teeth. This is especially common at night during sleep. The constant pressure and friction wears down the enamel and can fracture restorations. It also chips away at the biting edges, exposing softer dentin and tiny cracks that provide harbors for bacteria.
Using a custom nightguard can help minimize grinding damage. Occlusal splints and relaxation techniques may also help limitclenching. Addressing root causes like sleep disorders, anxiety, nutritional deficiencies or medication effects might further reduce grinding and clenching habits.
Dental Work
While fillings, crowns and other dental work aim to repair teeth, they can potentially contribute to further tooth breakdown in some cases. This occurs because:
- Fillings are softer than natural enamel and more prone to chipping, cracking or fracturing over time.
- The margins between fillings/crowns and natural tooth structure provide microscopic gaps where bacteria can enter and cause recurrent decay.
- Preparing a tooth for a crown removes 30-50% of remaining tooth structure, weakening the underlying support.
- Mismatched dental materials can set up galvanic currents and electrochemical reactions that slowly damage teeth.
Regular dental exams help detect failing restorations early before significant tooth structure is lost. Well-designed, high quality dental work should last many years, but will likely need replacement at some point due to material wear and breakdown.
Developmental Conditions
Some people may be more prone to cavities due to tooth/jaw alignment issues or abnormalities in tooth anatomy, tooth eruption timing or thickness of enamel. For example, deep anatomical grooves and pits on the biting surfaces allow food and bacteria to become trapped. Insufficient enamel thickness from delayed permanent tooth eruption also increases risk.
If a genetic predisposition is suspected, the dentist may recommend more frequent exams, earlier intervention and targeted preventive therapies like dental sealants to help strengthen at-risk front teeth.
What Are the Symptoms of a Rotten Front Tooth?
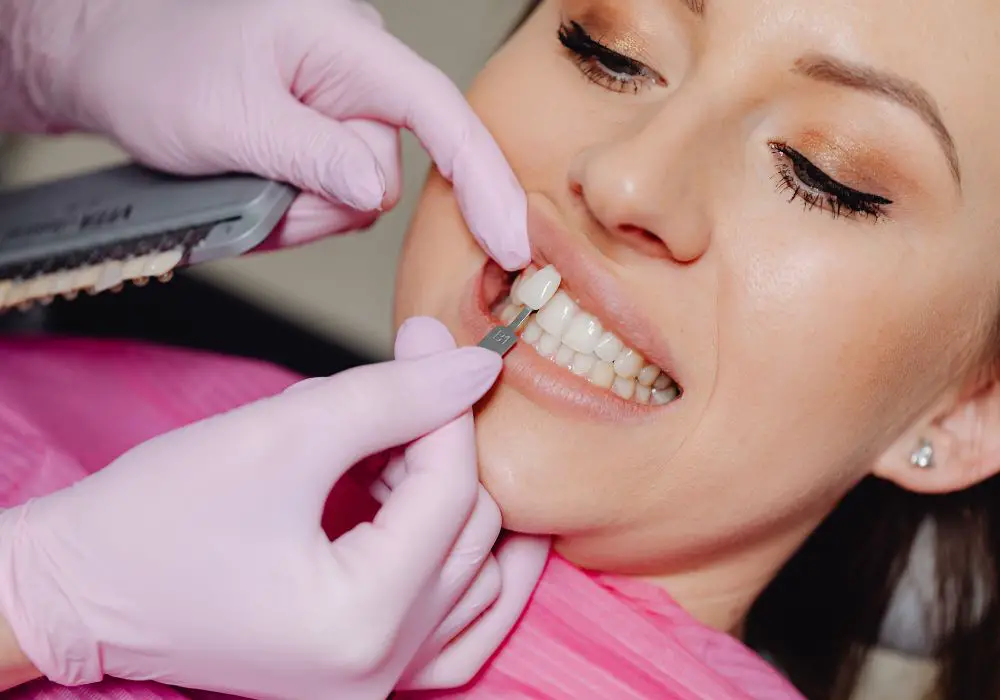
How can you tell if your front tooth is starting to decay or suffer internal damage? Look for these common warning signs:
Color Changes
One of the first visual clues is a loss of the light, semi-translucent appearance of a healthy front tooth. As enamel erodes away, the tooth color shifts from white towards yellow, brown or blackish hues. The discoloration may occur in spots or affect the entire tooth.
Interior changes to the pulp also influence color. A tooth that has suffered trauma or advanced, untreated decay may turn grey to reflect necrosis (death) of the pulp tissue inside.
Visible Holes
Small, early caries might appear as white, yellow or brown spots on the tooth surface. As they enlarge, actual holes or pits become visible as the enamel is eaten through. These tiny cavities don’t involve pain at first, though they may look unsightly.
Chipping or Fracturing
When decay, cracks, excessive wear or prior dental work has weakened the structural integrity of a front tooth, it becomes prone to chipping and fracturing. This occurs as outer enamel layers break away, often while biting down on something hard or crunchy.
The exposed inner dentin is softer and more vulnerable to bacteria and additional damage. Quick action is needed to seal off the exposed area before rapid decay sets in.
Temperature Sensitivity
As enamel thins, the inner dentin layer becomes exposed in places. Dentin contains thousands of microscopic tubules leading to the inner pulp that register hot and cold sensations. You may notice sharp pain or tingling when eating or drinking hot or cold foods that lingers after the stimulus is gone.
Toothache
Dental pain is often a late-stage indicator of advanced tooth decay. A tooth ache signifies infection and inflammation in the pulp. Without treatment, the pressure of the infection can lead to agony, facial swelling and fever. Toothaches require prompt dental attention.
Gum Swelling
Infection around the root can cause the gum tissue around a rotten tooth to become inflamed, enlarged and tender. This is the body’s defensive response to contain the spread of bacteria. Gum swelling is the body’s way of signaling it’s time to see the dentist.
Can a Dentist Fix a Rotten Front Tooth?
The good news is that an experienced general dentist has a toolbox of ways to restore damaged front teeth in most cases. The best approach depends mainly on how far the decay process has progressed. Let’s review the common front tooth repair options available:
Dental Fillings
If the decay is small and localized, a tooth colored composite resin filling may be placed to fill the space. Composite resin is matched to the hue of the surrounding tooth for discrete restorations. It bonds directly to the etched tooth structure for support.
For larger cavities, an amalgam filling made from silver, tin, copper, zinc and mercury may be used instead. Amalgam holds up well to the heavy biting forces in back teeth. Modern versions contain only enough mercury to bind the metals, releasing little vapor.
Both options halt further decay and cosmetically improve the smile. However, fillings are less durable than natural tooth structure. They need monitoring and eventual replacement as they can crack, chip and collect bacteria over time.
Root Canal Treatment
When tooth decay or trauma affects the soft pulp inside, a root canal is needed to save the tooth. This involves drilling an access cavity through the biting surface into the pulp chamber. The infected or damaged pulp is removed and the chamber is cleaned and disinfected.
It is then sealed using rubber-like filling material called gutta percha. A temporary crown is placed while a custom fitted crown is made to restore form and function. With proper care, a root-canaled tooth can last many years.
Extraction
Unfortunately, some front teeth with severe decay and weak remaining tooth structure cannot be repaired, especially if bone loss is also present. Extraction is then required, which involves complete removal of the tooth and roots. Ideally an implant to replace the missing tooth follows soon after extraction.
Crowns
After root canals, teeth become brittle and prone to cracking without a proper covering. A crown covers and envelops the remaining tooth above the gumline to add strength and prevent recontamination of the inner chamber.
A damaged front tooth without enough intact structure to support a filling may also receive a crown. The enamel-like porcelain fused to a gold, ceramic or zirconia base recreates the natural appearance. The crown restores the tooth for biting, chewing and speech.
Teeth Whitening
If decay is minimal but front teeth have become stained and darkened over time, a whitening procedure may be all that’s needed to refresh the smile. Peroxide-based bleaching lightens teeth 4-8 shades on average. In-office treatments performed by a dentist are the most dramatic.
Dental Implants
This high-tech treatment offers the closest thing to the original tooth. It involves surgically implanting a titanium screw into the jawbone that fuses over 3-6 months. A lifelike porcelain crown is attached atop the implant to precisely fill the gap left by the missing front tooth. Dental implants have the highest long-term success rate of all tooth replacements.
Dental Bonding
For minor damage like small chips, cracks or gaps between front teeth, dental bonding may be used as a quick cosmetic fix. After roughening the enamel, the dentist applies a putty-like resin that is shaped and hardened using a curing light. Bonding is an affordable way to repair slight flaws with natural-looking results.
What Influences the Repair Approach for Front Teeth?
In determining the ideal treatment plan for a decayed front tooth, the dentist must carefully assess and weigh several factors including:
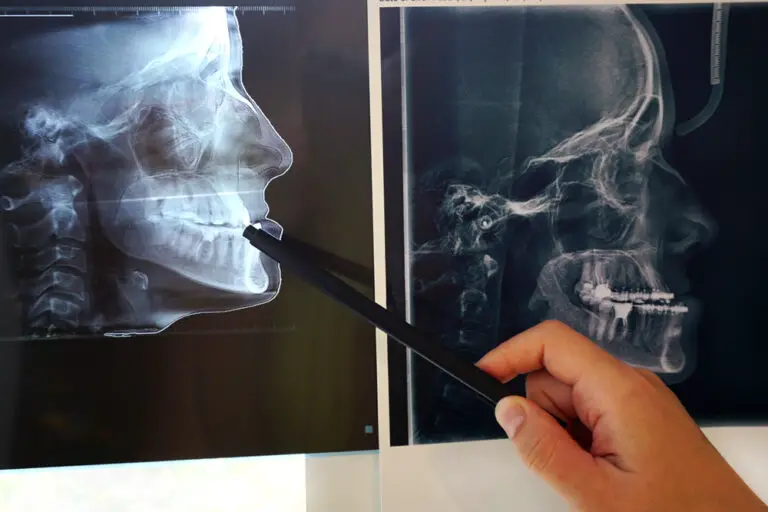
- Extent of Decay – Small cavities may be resolved through fillings, while pulp involvement or major structure loss limits reparative options. X-rays help evaluate the depth of decay.
- Remaining Tooth Structure – Teeth with intact biting edges and minimal structural loss have a more favorable restorative prognosis. The strength of the remaining enamel and dentin impacts which solutions are possible.
- Bone Condition – Weak, atrophied or missing bone makes a tooth poor candidate for repairs. Solid bone is essential to support and retain restorations. Implants require adequate bone levels for success.
- Symptoms – The presence or absence of pain, sensitivity, swelling, infection, looseness and mobility determine appropriate next steps. Mild, asymptomatic decay may be monitored, while severe cases require urgent care.
- Adjacent Teeth – Nearby healthy teeth help share chewing stresses. Their condition and spacing are considered when planning treatment.
- Patient Age – Young teeth have large pulp chambers and thinner enamel that make root canals more predictable. Mature teeth have less pulp space and thicker, more brittle walls prone to cracking.
- Patient History – Factors like past dental work, occlusion, causes of damage, and susceptibility to problems guide treatment planning.
- Patient Desires – Cosmetic concerns, financial status, time constraints and willingness to actively save a tooth weigh on options presented.
- Clinician Skill – Some dentists pursue advanced training in root canals, extractions, implants and complex reconstructions that can increase chances of saving severely damaged teeth.
Step-by-Step Process for Fixing a Rotten Front Tooth
Repairing and restoring a damaged front tooth involves a series of meticulous steps. Here is an overview of the typical treatment progression:
Initial Exam
The dentist first performs a visual inspection under bright lighting and magnification to assess the overall condition of the tooth and surrounding structures. They probe for softness that indicates decay and use an explorer to check for cracks or openings.
Percussion and sensitivity testing further identifies problems with the inner pulp. The patient’s oral hygiene and habits are reviewed. X-rays allow evaluation of the decay depth, root health, bone support and proximity to other structures.
Impressions of the teeth may be taken to analyze the bite. The findings help determine the scope of damage and best options for repair.
Anesthesia
Local anesthesia is typically administered via injection to completely numb the area being treated. This allows the dentist to remove decay and prepare the tooth without causing discomfort. The numbing effect usually lasts 1-2 hours.
Isolation
A rubber dam is often placed to isolate the tooth and prevent contamination from saliva. This square sheet has a hole that fits around the tooth being worked on. It provides a clean, dry operating field for higher quality restorations.
Decay Removal
The dentist uses hand instrumentation and/or a dental drill to remove all diseased and damaged portions of the tooth. Decay must be fully excavated down to strong, healthy tooth structure to prevent recurrent decay under restorations.
Protecting the Pulp
If caries removal is deep and nearly reaches the pulp chamber, a liner like glass ionomer cement is applied to help stimulate the pulp’s natural healing ability and prevent further irritation. A sedative dressing may be placed to calm inflammation before final restoration.
Tooth Preparation
The tooth structure is shaped by the dentist using burs to allow proper seating and bonding of the restoration. Undercuts that help anchor inlays, crowns or veneers are created.
Bite Adjustment
With inlays and crowns, the bite must be carefully analyzed. The dentist has the patient bite down on articulating paper to mark any spots of premature contact with other teeth. These high points are adjusted using a diamond bur to ensure even distribution when chewing.
Impression Taking
A mold or optical scan is taken of the prepared tooth to create a blueprint for fabricating the laboratory-crafted restoration. The form is checked against the adjacent and opposing teeth to verify fit.
Temporary Restoration
A temporary filling or crown is secured in place to protect the tooth while the permanent restoration is being custom made. Temporaries maintain space, function and aesthetics in the interim.
Placement of Final Restoration
At a follow-up visit, the dentist ensures proper color matching and fit, then uses bonding agents and cement to securely adhere the new inlay, onlay, crown, veneer or implant crown for a functional bite and natural look.
Polishing and Occlusion
Bite and contacts are carefully verified again. The restoration is shaped, contoured and polished until all surfaces are smooth. Minor adjustments eliminate any high spots causing premature contacts as the bite settles in.
Ongoing monitoring and at-home oral hygiene are critical for longevity of restorations. With proper maintenance and care, repaired front teeth can function normally for many years.
Cost for Repairing Front Teeth
The costs to restore damaged front teeth depends on the specific treatment needed:
- Simple Cavity Filling – $200-$300
- Root Canal Therapy – $700-$1200
- Pulp Capping – $150-$350
- Gum/Bone Grafting – $600-$1200
- Fiber Post – $300-$500
- Core Buildup – $150-$350
- Crown – $1000-$3000
- Veneer – $925-$2500
- Implant – $4000-$5000
Many dental insurance plans help pay a portion of these procedures. For example, they may cover 50% of allowable rates for fillings and root canals after a deductible is met. More advanced treatments like crowns, bridges and implants may only be covered at a lower rate if at all.
Out-of-pocket costs are influenced by the patient’s particular dental benefits. Payment plans and low or no-interest dental financing programs can make care more affordable. Prompt treatment is wise, as extensive damage leads to higher restoration costs.