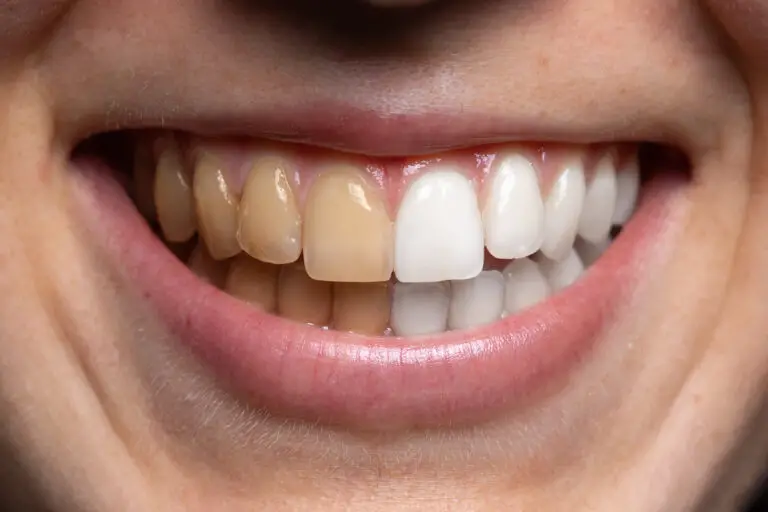
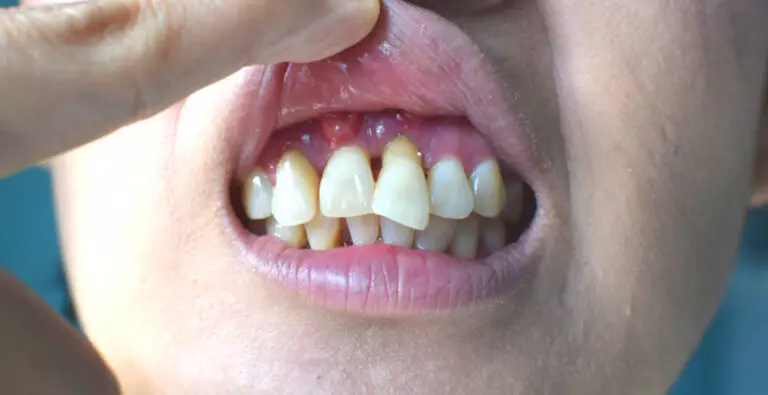
Rotten or decayed teeth can lead to a variety of health issues if left untreated. Here is an overview of some of the most common diseases and conditions that rotten teeth can cause.
Dental abscess
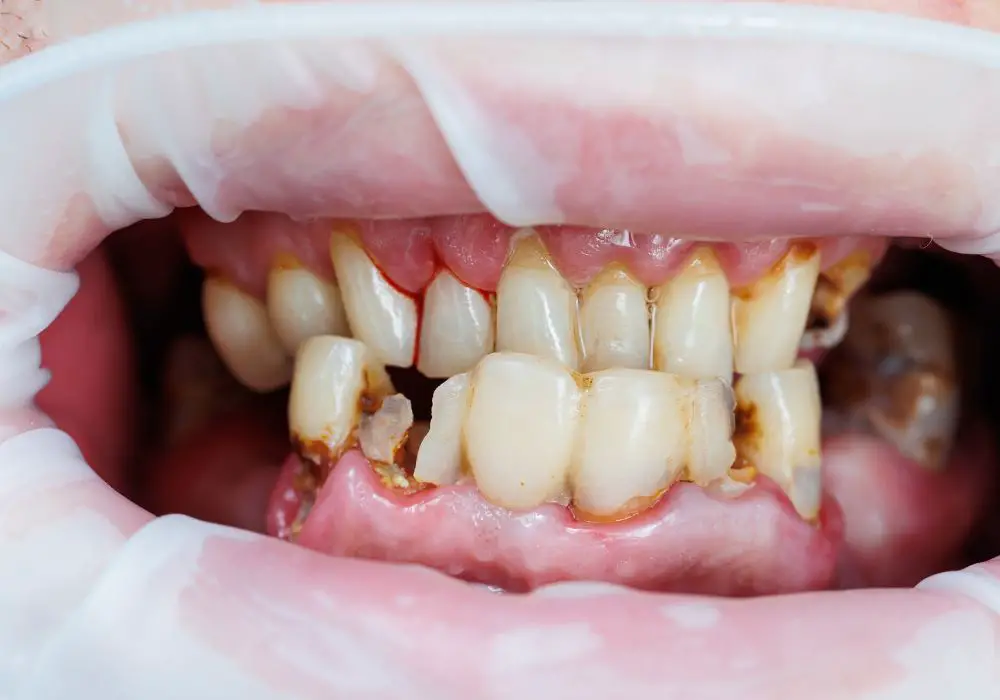
A dental abscess occurs when a pocket of pus forms in the teeth or gums as a result of a bacterial infection. Abscesses are usually caused by severe tooth decay that reaches deep into the tooth and infects the pulp and root.
Abscesses can be extremely painful and must be treated as soon as possible to prevent the infection from spreading. Potential complications of a dental abscess include:
- Spreading infection in the jaw, mouth, or neck
- Difficulty swallowing or breathing
- Bone loss in the jaw
- Sepsis or blood poisoning if the infection spreads through the bloodstream
Symptoms of a dental abscess
- Severe, throbbing toothache
- Sensitivity to hot and cold temperatures
- Fever and chills
- Swelling around the cheek, jaw, or neck
- Bad breath
- An abnormal taste in the mouth
- Gum inflammation and tenderness
Treating a dental abscess
A dental abscess requires professional dental treatment. The infected tooth is treated with a root canal procedure to remove diseased pulp, followed by drainage of the abscess to relieve pressure. Antibiotics may also be prescribed to control the infection. In severe cases, the tooth may need to be extracted. Prompt treatment is essential to stop the abscess from worsening.
Periodontal disease
Periodontal disease, also called gum disease, is an infection of the gums and bone that surround and support the teeth. It’s caused by a buildup of plaque on the teeth. As plaque continues to build, it can form tartar that irritates the gums.
The mildest form of the disease is gingivitis. More severe periodontal disease causes gums to pull away from the teeth, forming pockets that become infected. Pockets of bacteria can damage the bone and connective tissue holding teeth in place. When left untreated, periodontitis can cause tooth loss.
Symptoms of periodontal disease
- Red, swollen, tender gums
- Gums that bleed easily, including when brushing and flossing
- Gums that have pulled away from the teeth
- Persistent bad breath
- Pus between teeth and gums
- Loose or separating teeth
- Changes in the way teeth fit together when biting down
Treating periodontal disease
Periodontal disease requires professional cleaning and treatment. Options include:
- Deep cleaning below the gumline to remove plaque and tartar
- Antibiotics or antimicrobial mouth rinse to control infection
- Flap surgery to clean roots and rebuild bone
- Tissue grafts to rebuild gums
- Extractions if teeth are loose or damaged
With early treatment, further gum and bone loss can be prevented. But damage from advanced disease can’t be reversed.
Tooth decay
Tooth decay, also called dental caries or cavities, occurs when foods containing carbohydrates (sugars and starches) are left on the teeth. Bacteria in the mouth digest these carbohydrates and produce acids that attack the tooth enamel.
As tooth decay advances, it penetrates through the enamel and eats into the sensitive dentin underneath. Untreated decay can reach the pulp and cause severe infection and abscesses.
Symptoms of tooth decay
- White, brown or black staining on any surface of the teeth
- Sensitivity to hot or cold food and drinks
- Mild to sharp pain in the affected tooth that may come and go
- Cavities beginning as small holes in the enamel that get bigger over time
- Fracturing or chipping of the enamel
- Bad odor from the decayed area
Treating tooth decay
Early tooth decay can be reversed with brushing, flossing, fluoride treatments, dental sealants, and dietary changes. Once decay has progressed, it requires professional dental intervention. Options include:
- Fillings to remove decay and restore teeth
- Root canals if decay has infected the pulp
- Crowns to cover severely damaged teeth
- Tooth extractions when other treatments are not possible
Regular dental exams and cleanings are essential for finding and treating tooth decay in its early stages before it causes irreparable damage.
Oral thrush

Oral thrush is a yeast infection of the mouth caused by an overgrowth of the Candida fungus. Candida is normally present in the mouth in small amounts. When conditions allow it to grow uncontrolled, thrush develops.
Poor oral hygiene and chronic conditions like diabetes or HIV can increase the risk for thrush. But the main culprit is reduced immunity. Dentures and orthodontic appliances also create surfaces for Candida to take hold.
Rotten teeth provide ideal conditions for Candida to thrive due to their rough surfaces, limited blood supply, and occlusion from saliva.
Symptoms of oral thrush
- White lesions or coating in the mouth, on the tongue, gums, tonsils or inner cheeks
- Redness or soreness
- Loss of taste
- Cottony feeling in the mouth
- Cracking at the corners of the mouth
- Difficulty eating or swallowing
Treating oral thrush
Mild thrush cases may clear up on their own with improved oral hygiene. But medication is typically needed, including:
- Antifungal mouthwashes, lozenges or tablets
- Antifungal cream for dentures
- Medicated mouthwash containing nystatin
- Oral fluconazole for severe infections
Treating any underlying condition, like diabetes or HIV, is also necessary. Without fixing the root cause, thrush will likely keep recurring.
Cracked tooth syndrome
Cracked tooth syndrome refers to a variety of symptoms caused by small fractures in teeth. Cracks can form in healthy teeth due to trauma, grinding, clenching, or the natural aging process. But teeth weakened by severe decay are at much higher risk.
Even tiny cracks that are invisible to the eye can allow bacteria and fluids to seep in and irritate the tooth’s inner pulp. This irritation causes intermittent pain when eating or biting down.
Over time, cracks tend to worsen, often eventually causing pulp infection, tooth fractures, or loss of teeth.
Symptoms of cracked tooth syndrome
- Sharp pain when chewing or biting, especially when biting down
- Pain that is temporary and disappears after pressure is released
- Pain when exposed to temperature extremes
- A noticeable chip or fracture in the tooth’s surface
- Swelling around the gum of the affected tooth
- Tooth discoloration
Treating cracked tooth syndrome
Minor cracks can be monitored or treated with dental bonding. More extensive cracks require a filling or crown to stabilize the tooth.
For severe cracks causing pulp inflammation, a root canal treatment may be necessary to remove the infected pulp and prevent abscess. Extraction is the only option if the tooth cannot be repaired.
Oral cancer
Oral cancer refers to any cancerous growth that occurs in the mouth or throat. It most commonly begins as a lesion or sore that does not heal.
Risk factors for oral cancer include smoking, excessive alcohol use, and human papillomavirus (HPV) infection. But poor oral hygiene and untreated tooth decay also make the mouth more vulnerable to cancer growths.
The abrasive surfaces and limited blood supply caused by severe decay create an environment favorable to the development of cancer.
Symptoms of oral cancer
- Sores, lesions, or ulcers that bleed easily and do not heal
- Pain, tenderness, or numbness anywhere in the mouth or lips
- White, red, or speckled patches in the mouth
- Loose teeth with no clear cause
- Difficulty swallowing, speaking, or chewing
- Lumps or thickening of tissue in the mouth, neck, or cheek area
Treating oral cancer
Oral cancer requires immediate medical intervention. Treatment options depend on the location, size, type, and stage of the cancer, and may include:
- Surgery to remove malignant growths and affected tissue
- Radiation to destroy cancer cells and shrink tumors
- Chemotherapy drugs to kill cancer cells
- Immunotherapy to boost the immune system against cancer cells
- Targeted therapy to block the growth of cancer cells
Early detection drastically improves survival rates for oral cancer. So any persistent sore or mouth lesion should be examined by a dentist right away.
Impacted wisdom teeth
Wisdom teeth are the third and final set of molars that emerge in late adolescence or early adulthood. They are located at the very back of the mouth.
When wisdom teeth become impacted, meaning they do not have enough room to erupt through the gums, it can lead to pain, swelling, infection, and damage to nearby teeth. Food and bacteria easily become trapped under partly erupted wisdom teeth, allowing cavities and decay to develop.
Symptoms of impacted wisdom teeth
- Pain or soreness around the jaw, ears, or back teeth
- Inflammation, swelling, or tenderness of the gums
- Headaches or jaw stiffness
- Damage or decay in adjacent teeth
- Inability to open the mouth fully
- Visible tooth trapped below the gumline
Treating impacted wisdom teeth
If impacted wisdom teeth are decayed or causing problems, they typically require extraction. Your dentist will refer you to an oral surgeon for removal under anesthesia to prevent complications.
Sometimes partially impacted wisdom teeth are monitored if they are not currently problematic. But given their high risk for future decay and infection, most dentists recommend proactive removal.
Osteomyelitis
Osteomyelitis is an infection of the jaw bone caused by untreated tooth and gum infections. It occurs when bacteria or fungi from cavities, tooth decay, or advanced periodontal disease spread from the tooth’s pulp or roots into the jaw.
The infection causes inflammation in the bone tissue, reducing blood flow in the area and slowing the body’s ability to fight infection. Pus and abscesses develop in the infected regions, and tissue and bone death can occur.
Symptoms of osteomyelitis
- Severe tooth pain that transitions into constant, throbbing jaw pain
- Swelling, drainage, and tenderness in the jaw
- Difficulty opening the mouth and chewing
- Numbness or tingling sensation in the jaw, lips, or face
- Tooth loosening or loss
- Fever and fatigue
- Bad breath
Treating osteomyelitis
Osteomyelitis requires aggressive antibiotic therapy, sometimes administered intravenously in the hospital. Diseased teeth are extracted to remove the source of infection. Dead bone tissue may need to be surgically removed (debrided) to allow healing. With prompt treatment, the infection can usually be controlled before it causes permanent bone damage. But prevention through good oral care is key.
Key takeaways
- Rotten, decayed teeth provide a welcoming environment for infection and disease to take hold in the mouth.
- Dental abscesses, periodontal disease, tooth decay, thrush, and cracked teeth are among the most common problems caused by poor oral hygiene.
- If left untreated, these conditions allow infection to spread from the mouth to the jaw, neck, and other areas of the body.
- Severe dental infections can also increase vulnerability to oral cancer or osteomyelitis of the jaw bone.
- Practicing good daily oral hygiene and getting regular dental exams and cleanings are essential for preventing painful, expensive, and potentially serious health consequences of rotten teeth.
Frequently Asked Questions
Q: How quickly can tooth decay progress if left untreated?
A: Tooth decay spreads rapidly if not treated. What starts as a barely noticeable white spot can become a large cavity in just a few months. Small cavities take 3-12 months to develop into larger cavities. From there, untreated decay can destroy a tooth in less than a year. The pace depends on the individual and presence of risk factors like a sugary diet. But in general, decay is a quickly advancing condition.
Q: Can a rotten tooth just fall out on its own?
A: No, a rotten or decayed tooth will not simply fall out on its own. As tooth decay undermines the enamel and eats into the sensitive inner structures, it can certainly damage a tooth to the point where it becomes loose or fragile. But it requires surgical extraction by a dentist to fully remove the affected tooth. Allowing decay to progress to natural tooth loss is extremely dangerous, given the likelihood of serious infections spreading throughout the mouth and jaw.
Q: How are deep dental abscesses treated?
A: For dental abscesses that extend deep into the tooth and jaw tissues, the first step is a root canal treatment. This involves drilling an opening through the top of the tooth to reach the infected pulp. The pulp and nerves are removed and the insides of the roots are cleaned and disinfected. Next, the tooth is extracted to provide decompression and drainage of the abscess. Remaining infection may be drained surgically through the gum. Antibiotics are used alongside dental treatment to control the infection. Healing may take several weeks to months.
Q: What is the fastest way to improve gum health?
A: The quickest way to start reversing gum disease is through professional deep cleaning to remove plaque and tartar above and below the gumline. Improving daily oral hygiene is also key. Effective brushing and flossing will continue fighting plaque buildup after the deep cleaning. Antimicrobial mouthwash can provide added protection against the bacterial infection causing gum inflammation. As gums heal, inflammation and bleeding should steadily decrease. Within a few weeks, healthier gums that are pink rather than red or swollen should be apparent.
Q: How long does a dental crown typically last?
A: With proper care, a dental crown generally lasts 5-15 years before needing replacement. However, crowns placed on badly decayed teeth or to restore teeth already weakened by cracks may only last 5 years. Proper oral hygiene and regular dental visits help crowns last toward the longer end of that timeframe. But eventually the damage below the crown is likely to necessitate a new one. Getting decay treated early before a crown is needed can extend the life of a tooth for decades.