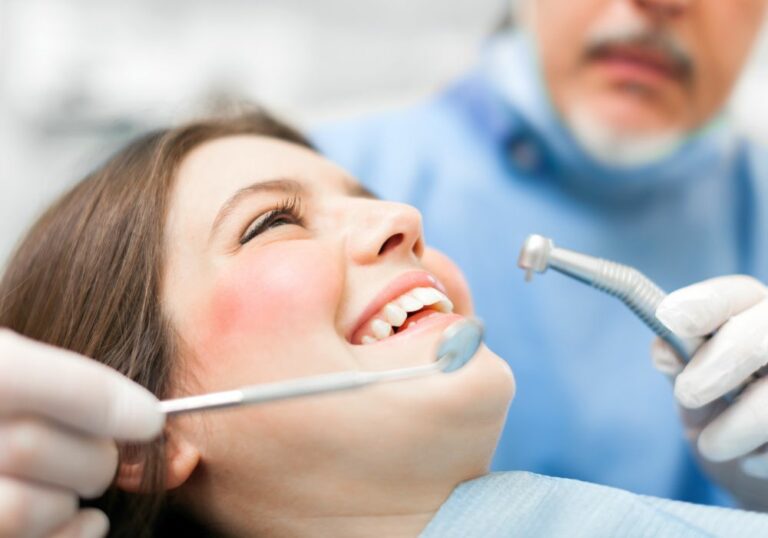
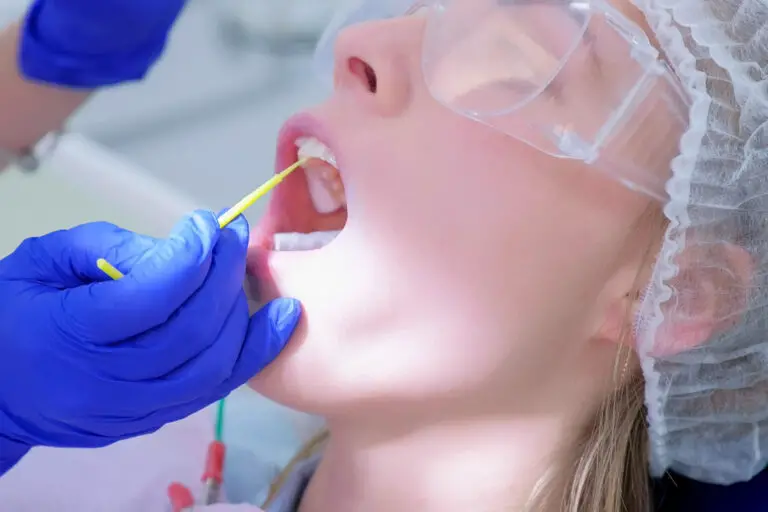
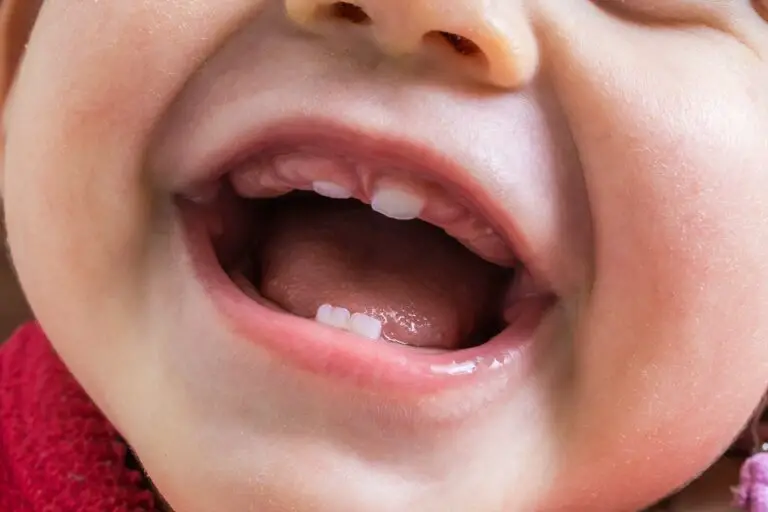
Tooth nerve damage, medically known as dental pulpitis, is a common problem that can result from issues like deep decay, cracks, or trauma. The pulp inside each tooth contains sensitive nerves and vessels that provide sensation and nourishment. When this tissue becomes injured or inflamed, you may experience significant tooth pain and sensitivity. So can this type of damage be healed and repaired? There are some treatment options available to try to rescue damaged dental nerves. However, severe or long-standing pulp infections often cannot be reversed.
What causes tooth nerve damage and symptoms to develop?
A number of different dental problems can lead to nerve inflammation and pulp tissue damage. Understanding the most common causes is helpful for prevention and prompt treatment.
Dental decay
Tooth decay that extends deep enough will inevitably reach the pulp tissue inside. Bacterial acids and irritation cause inflammation of the nerves. Mild decay may only cause slight sensitivity, but deeper cavities can lead to severe spontaneous pain.
Cracked teeth
Cracks and fractures in teeth can form due to trauma, grinding, or chewing hard items. These cracks may start out painless but worsen over time. The fracture lets bacteria in and puts pressure on the pulp, resulting in inflammation and infection.
Dental trauma
Injuries that chip, crack, or displace teeth often expose the sensitive pulp inside. This crushing trauma causes damage to the nerves and blood vessels. Bleeding pulp tissue is also vulnerable to bacteria.
Grinding and clenching
Chronic grinding and clenching wears down enamel over time, allowing easier access to inner pulp. Exposed dentin tubules cause sensitivity as well. Eventual pulpitis develops.
Prior dental work
Previous fillings, crowns, or root canal treatments that were too extensive or went too deep could damage the dental pulp. This leads to progressive irritation and infection.
Gum recession
Receding gums expose more tooth root. Since cementum covering the root is thinner than enamel, decay and sensitivity develop more readily. Exposed root surfaces have limited protection.
In each case, the common factor is bacterial exposure combined with pressure and irritation of the sensitive pulp tissue inside the tooth. This causes inflammation of the nerves and blood vessels which leads to the characteristic symptoms.
Pain when eating or drinking
The first sign is often sharp pain when consuming hot, cold, sweet, or acidic foods and drinks. This indicates mild inflammation of the pulp’s sensitive nerves.
Temperature sensitivity
Lingering pain after a hot or cold stimulus is removed signifies inflamed nerves. This is an early stage of pulpitis.
Unprovoked pain
As pulpitis worsens, you may feel throbbing or pounding tooth pain spontaneously without any trigger. This severe inflammation impacts nerve endings.
Pain when chewing
Biting or chewing can cause flare-ups in an infected tooth with inflamed pulp. Pressure on the tooth is painful.
Swelling and drainage
A abscess at the tooth’s root tips indicates advanced infection. Pus puts additional pressure on the tooth pulp.
Dark discoloration
In later stages, the damaged pulp may die, causing the tooth to darken and deteriorate.
Can you reverse mild pulp damage before it becomes severe?
If pulpitis is caught early while still mild and localized, it is sometimes possible to calm the inflammation and prevent it from getting worse. However, this requires prompt treatment.
Treating minor sensitivity
For mild temperature sensitivity from small areas of exposed dentin, topical fluoride and sealing the area with dental bonding can remineralize the tooth and calm nerves.
Handling early decay
If decay is treated quickly before it reaches deep into the pulp chamber, a sedative filling may resolve mild inflammation.
Monitoring cracks
Minor cracks can be sealed and monitored to see if symptoms resolve before the pulp becomes severely damaged.
However, delaying treatment allows the problem to advance. Severe infection and necrosis eventually develop, requiring root canal treatment or extraction.
Diagnosing the stage and severity of pulpitis
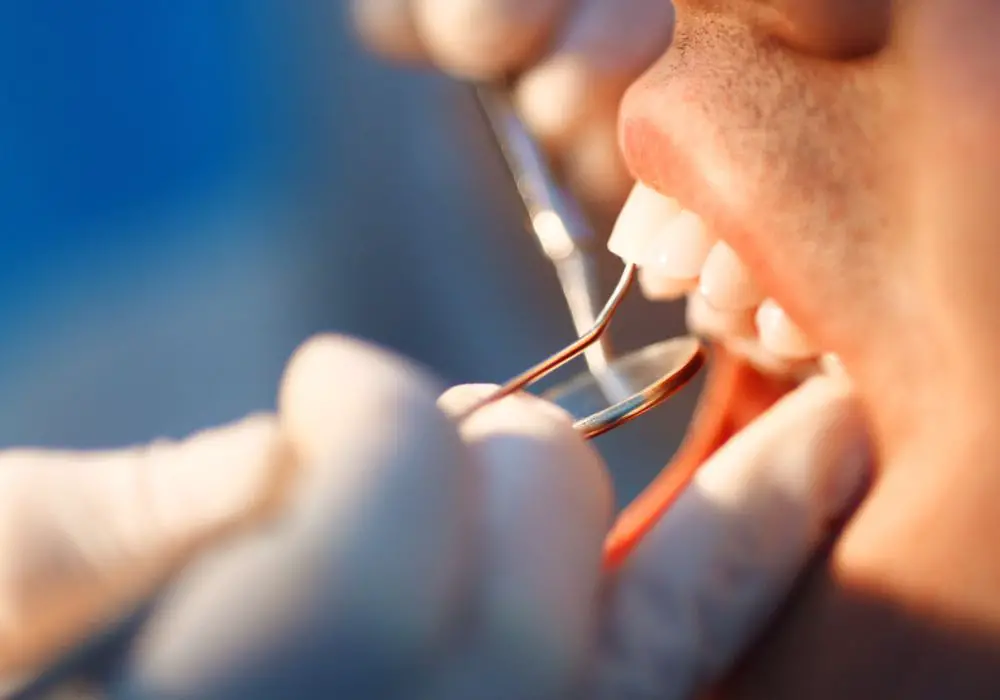
In order to select appropriate treatment, dentists must determine whether pulpitis is reversible or has become irreversible. Diagnostic testing helps assess pulp vitality and the health of nerves.
Clinical examination
The dentist checks for signs like swelling, sinus tracts, cracks, pain on percussion, and dark discoloration that indicate pulp infection.
Dental radiographs
X-rays show the depth of decay and its proximity to the tooth pulp. Signs of infection like bone loss are also visible.
Cold stimulus testing
Placing cold on the tooth triggers a response in still-vital pulp tissue. No sensation can mean the nerve is necrotic.
Electric pulp testing
Electrical current elicits a response in healthy nerves. No reaction indicates non-vital tissue that requires root canal therapy.
Laser Doppler flowmetry
This measures blood circulation within the pulp to assess inflammation and vitality. Reduced blood flow is a negative sign.
Options for treating reversible pulpitis
If caught early, pulp damage may be reversible with conservative treatment to settle inflammation and promote healing.
Removing decay
Eliminating infected decay is the first priority. This reduces the source of bacteria causing inflammation. Any pulp pressure is also relieved.
Applying fluoride
Fluoride has antibacterial effects and stimulates repairing dentin. High-concentration fluoride may encourage healing.
Using pulp-calming medicaments
Capping the pulp with a sedative dressing like zinc oxide eugenol or calcium hydroxide can soothe inflamed nerves.
Watching carefully
If symptoms resolve after medicated fillings, the tooth can be sealed. But if pain lingers, further treatment is warranted.
Conservative therapy aims to save the tooth and calm reversibly inflamed pulp. But infection can only be reversed in the early stages.
Treating infected, irreversible pulpitis
Once pulpitis has become irreversible, more intensive endodontic procedures are required to address the diseased pulp.
Root canal therapy
This completely removes the inflamed and infected nerve tissue and blood vessels. The tooth interior is disinfected and sealed.
Pulpotomy
When decay is localized in the crown, removing just the diseased coronal pulp may help save the root.
Apexification
Immature infected teeth require special treatment to encourage continued root development. Calcium hydroxide aids this.
Pulp regeneration techniques
Experimental methods aim to regrow new pulp tissue using disinfected tooth roots as scaffolds. This approach is still under development.
While root canals are the standard solution for irreversible pulpitis, regeneration may someday offer renewed options.
The timeline for healing after dental pulp treatments
How long pulp healing takes depends greatly on the severity of inflammation and type of treatment:
- For mild irritation treated only with bonding, sensitivity may resolve in days to weeks.
- With minor decay removed and a sedative filling placed, healing may begin in a few days but take months to fully complete.
- Reversible pulpitis often resolves in 4-8 weeks with ideal treatment.
- Irreversible pulpitis requires root canal therapy. Pain relief is immediate but the tooth remains permanently numb afterward.
Closely following up on pulp symptoms after treatment is key. Worsening pain likely means further therapy is warranted.
Can damaged dental pulp fully regenerate?
The nerves and blood vessels inside the pulp have limited ability to completely regenerate once severely damaged or infected.
Natural healing processes
Mild injuries may heal via:
- Stem cells forming new odontoblast cells
- Nerve sprouting into newly formed reparative dentin
- Increased blood flow bringing nutrients
Limits of regeneration
But pulp tissue cannot regenerate itself after:
- Extended decay and bacterial infection
- Necrotic, infected tissue
- Surgical removal of all pulp during root canals
Experimental techniques
Emerging methods aim to regrow dental pulp by utilizing disinfected root canals as scaffolds for new tissue growth. More research is still needed.
While regeneration shows promise, root canals still remain the standard of care for resolution of diseased pulps. Avoiding damage through preventive dental care remains key.
Can cracked teeth be repaired and nerve damage healed?
Cracks that extend into the pulp cause inflammation and infection of the nerves. Options for cracked teeth include:
- Minor cracks – Early sealing and protection may allow healing of mild damage. But further treatment is usually eventual.
- Moderate cracks – If the fracture is not too severe, crown placement stabilizes the tooth and protects the pulp.
- Extensive cracks – These typically worsen until the tooth requires root canal treatment or extraction. Repairing severe cracks is difficult.
Preventing cracked teeth through protecting from grinding and avoiding chewing hard items like ice is ideal. Damaged nerves cannot be reliably regenerated.
Does a root canal remove all tooth nerve endings?
Yes, root canal treatment cleans out all pulp tissue and nerve endings from inside the tooth. This includes both healthy and infected nerves alike.
- All nerves and blood vessels are permanently removed from the chamber and root canals.
- The tooth becomes completely numb afterward since pulp provides sensation. It relies on surrounding bone for any remnants of feeling.
- Future regenerative techniques aim to regrow new dental pulp in disinfected roots. But for now, numbness is irreversible after root canals.
Since root canals are currently the only option for severe damage, prevention is key. Protecting your natural healthy tooth nerves from injury remains imperative.
FAQs
Q: Can damaged tooth nerves ever fully heal or regenerate after severe injury?
A: With current endodontic techniques, once dental pulp becomes severely inflamed or infected the damage generally cannot be reversed or fully heal. Root canal treatment is necessary to remove the diseased nerve tissue. However, emerging regenerative therapies aim to regrow damaged dental pulp in the future.
Q: Is it typically painful when tooth nerve damage first starts to heal after treatment?
A: It is not usually painful as pulp healing begins after minor injury or reversible inflammation. Discomfort from temperature sensitivity should steadily improve over days to weeks. However, if the pulpitis was irreversible, more invasive treatment like a root canal is required to eliminate the infected tissue and nerves.
Q: How long does it normally take for tooth nerve damage to begin healing after treatment?
A: Early healing can begin within 1-2 days after removing decay and irritation from a mildly inflamed pulp. But complete healing of damaged nerves often takes a minimum of 4-8 weeks, and sometimes 3-4 months for full resolution of symptoms. Quick treatment is key before extensive infection develops.
Q: Can cracked teeth be reliably repaired and have their nerve damage healed?
A: Cracks reaching the tooth pulp invariably infect the nerves, and this damage ultimately proves very difficult to reliably reverse or heal. Minor cracks may sometimes be stabilized, but often worsen over time. Preventing cracked teeth through protection from grinding is ideal, since current techniques cannot regenerate damaged nerves.
Q: Do root canals remove all the tooth nerve endings and are they then permanently gone?
A: Yes, root canals completely remove all nerve tissue and pulp blood vessels from inside a tooth. This includes both healthy and diseased nerves. The tooth becomes permanently numb afterward. Future regenerative methods may enable pulp regrowth after disinfection, but current root canal therapy results in permanent numbness.
In summary
While some minor or reversible pulp inflammation can heal after prompt treatment, severe tooth nerve damage usually cannot be reversed or regenerated using current techniques. Avoiding dental decay and cracks through diligent home care and professional treatment is essential for maintaining the vitality of dental nerves. Research into pulp regeneration brings hope for the future. But for now, prevention and early intervention remain paramount for enabling healing and repair of injured tooth pulp.