Losing sensation in a tooth due to nerve damage can happen for many reasons. But once tooth nerves die or are removed, can they ever be regenerated? In this in-depth guide, we’ll explore what causes tooth nerves to die, the implications of losing tooth nerve supply, and potential ways nerve tissue may regrow in the future.
Anatomy of Tooth Nerves
Before learning about tooth nerve damage, it helps to understand the anatomy of the nerves inside teeth.
Each tooth contains soft tissue in the central chamber called dental pulp. This pulp contains blood vessels, connective tissue, and sensory nerve fibers that provide the tooth with nutrition, sensation and pain signaling.
A network of microscopic tubules located throughout the dentin layer of the tooth connect the pulp to the enamel and cementum layers of the tooth surface. These dentinal tubules allow temperature, pressure and pain signals to transmit from the exterior of the tooth to the nerve fibers contained in the pulp.
The healthy pulp and nerve supply are necessary for proper tooth function in several ways:
- Provide vital nutrients – The blood vessels in the pulp deliver nutrients and oxygen that maintain the dentin and allow the tooth to remineralize.
- Sense stimuli – The nerve fibers detect hot, cold, pressure, and pain signals at the tooth surface and transmit these sensations to the brain. This allows you to feel and respond to stimuli.
- Trigger protective responses – Nerve signals prompt reflexes to prevent further damage, like pulling away from extreme heat or cold on a tooth’s surface.
- Enable repair – The pulp contains stem cells that can differentiate into other cell types to help repair dentin or form reparative dentin in cases of injury.
Losing these vital functions that tooth nerves provide can impact oral and even systemic health. Next we’ll look at how tooth nerves become damaged in the first place.
What Causes Tooth Nerve Damage?

A variety of conditions, diseases and injuries can damage the living pulp tissue and nerve supply inside teeth:
Tooth Decay
Cavities allow bacteria to invade a tooth and infect the pulp. The inflamed pulp responds with increased blood flow and nerve signaling. Left untreated, the bacteria can overwhelm and kill the tooth’s nerves.
Periodontal (Gum) Disease
Chronic gum infections damage the bone and ligaments supporting the tooth. As these shrink away, spaces open up at the base of the tooth that allow bacteria to reach the root canals and pulp tissue.
Developmental Defects
Sometimes teeth develop with thin enamel or abnormal anatomy that results in pulp exposure, leading to inflammation and nerve death. An example is dens invaginatus, where a tooth forms with an extra canal running through the middle into the pulp chamber.
Tooth Grinding and Clenching
Constant pressure from teeth grinding or clenching (bruxism) can traumatize the dental pulp over time, narrowing and calcifying the root canals. This progressively cuts off the tooth’s blood supply.
Cracked and Fractured Teeth
Cracks allow bacteria to seep deep inside a tooth, infecting and killing the pulp. Split or fractured teeth often shear off the tooth’s nerve supply immediately.
External Injury
Trauma from sports collisions, car accidents, falls and blows can crack teeth, displace them in the socket, or entirely avulse (knock out) teeth. This severs blood vessels and damages pulp tissue.
Prior Dental Work
Multiple fillings, veneers, crowns or orthodontic movement can repeatedly irritate the dental pulp. Teeth previously treated by a dentist are more prone to nerve issues.
Aging
Over time, the pulp canal spaces narrow and become more calcified. This reduces blood flow and leads to pulp cell death as we age. Older teeth are much more susceptible to nerve damage.
Identifying and promptly treating the causes of pulp irritation is key to preventing total nerve death and maintaining tooth vitality when possible. But what happens when the tooth nerves are too damaged and die completely?
Signs Your Tooth Nerve Has Died
How can you tell if the nerve supply and pulp tissue inside a tooth are no longer viable? Dead or necrotic tooth nerves result in the following signs:
Loss of Sensation
Since the nerve fibers are destroyed, you’ll notice the tooth does not hurt or respond to temperature changes. Even severe stimuli like ice or scalding heat cause no reaction.
No Pain from Cavities
Decay that would normally trigger pain in vital teeth with live nerves may go unnoticed. The dead tooth just feels hollow or numb to any irritation.
Dark Tooth Discoloration
With no blood circulating inside, the dentin darkens and the tooth may turn grey, black, or yellowish. In back molars, the crown may even look charred.
Slow Separation from Bone
A common late sign is the tooth starting to detach and loosen as infection spreads into the surrounding bone socket.
Widening of Periodontal Ligament Space
On x-rays, the bony socket around the dead tooth root appears hazy and the ligament space widens as bone loss occurs.
Abscess Formation
Pus-filled abscesses in the gums or jaw indicate rampant infection from necrotic tooth roots. There may be swelling, foul odors, and drainage from fistulas.
Catching nerve death early based on these warning signs can prevent complications and save the tooth. But left too long, the tooth eventually requires extraction.
Why Can’t Tooth Nerves Regenerate on Their Own?
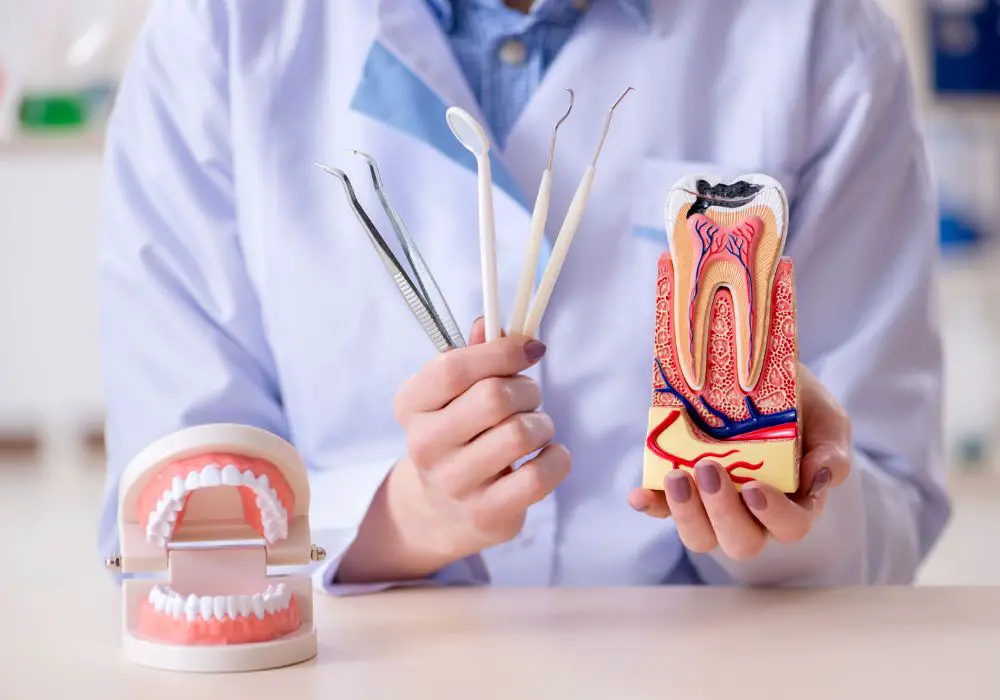
Once tooth nerves and pulp tissue die, they do not regenerate naturally. This is due to the unique challenges of the oral environment:
- No blood supply – Without blood vessels, the pulp chamber lacks the nutrients, oxygen, and stem cells needed to regrow.
- Rigid surroundings – The pulp is encased in stiff, mineralized layers of dentin and enamel that offer no room for expansion.
- Persistent infection – Bacteria rapidly invade and overwhelm the dead space, preventing healing.
- No stem cells – Dental pulp contains no stem cells itself capable of reforming into specialized cell types.
- Age – Older teeth have less regenerative capacity and blood supply available to repair damage.
- Trauma – Injury that causes pulp death also destroys the scaffolding and signals necessary to reorganize tissue growth.
For these reasons, the lost sensory functions of cleaned-out root canals and extracted teeth are never restored. At least by natural means alone. Next, we’ll explore some regenerative approaches attempting to regrow tooth nerves.
Emerging Techniques to Regenerate Tooth Nerves
Modern dental research is investigating methods to engineer and regrow functional dental pulp complete with nerves, blood vessels and connective tissue. This field is known as regenerative endodontics.
Potential ways to achieve tooth pulp regeneration include:
Stem Cell Therapy
Introducing specialized stem cells into cleaned and disinfected root canals could allow the cells to reform pulp tissue, if also supplied with growth factors and a scaffold for structure. Dental stem cells could come from:
- Healthy pulp tissue of other extracted teeth
- Dental follicle stem cells from wisdom teeth extractions
- Stem cells from bone marrow or fat tissues
- Induced pluripotent stem cells synthesized from skin cells
Challenges include getting enough stem cells to populate the entire pulp space and ensuring the regenerated tissue mimics natural pulp and innervates the dentin.
3D Cell Printing
Printing living stem cells, growth factors, and biomaterials like collagen directly into a prepared root canal is another promising approach. The precision of 3D bioprinting potentially allows controlled regeneration of vascularized pulp with nerves.
However, vascularization to support printed pulp tissue, inhibiting bacterial contamination, and difficulty printing small intricate root canal spaces currently limit practical applications.
Growth Factor Delivery
Growth factors are proteins that can signal immature stem cells to differentiate into specialized pulp cells. Delivering combinations of growth factors like TGF, VEGF, and NGF into cleaned canals may be able to kickstart pulp regeneration.
Challenges include limited diffusion of growth factors through dentin, a short half-life, and getting a properly sequenced delivery of multiple factors.
Scaffold Implantation
Natural collagen or synthetic biomaterials implanted into prepared canals can act as a scaffold for endogenous stem cells to attach and reform pulp tissue upon.
Yet cell adhesion and migration deep into implants, biocompatibility issues, and scaffold degradation rates make this difficult to accomplish reliably.
While still experimental, these pioneering approaches offer hope for regenerating tooth nerve fibers, overcoming the innate challenges teeth face in healing themselves.
Procedures for Treating Dead Tooth Nerves
What should you do if a dentist determines the nerve inside your tooth is dying or already necrotic? Depending on the level of infection and structural integrity remaining, recommended treatments include:
Root Canal Therapy
The standard procedure is to remove all infected and dead pulp tissue from inside the tooth roots. The empty canals are cleaned, shaped, and sealed with an impervious filling to prevent reinfection.
Though the tooth loses sensation, it can still be restored with a buildup and crown for lasting function. Modern advances like operating microscopes, ultrasonic cleaning, and bioceramic seals enable very high root canal success rates today.
Apicoectomy
If infection persists at the tooth root tips after a root canal, an apicoectomy can be performed to surgically remove the inflamed tissue and seal the ends. This salvages the tooth and stops further infection.
Pulpotomy
In immature teeth with health pulp in the roots but inflamed or infected pulp in the crown, a pulpotomy removes just the diseased crown pulp and leaves the root pulp intact to encourage continued root development and tooth vitality.
Pulp Capping
If the pulp is only mildly inflamed and not yet necrotic, medicated pulp capping materials placed over small exposed pulp areas can encourage healing, regeneration, and nerve preservation.
Tooth Extraction
If the tooth cannot be saved with endodontic treatment or repair due to severe infection, fractures, or periodontal damage, complete extraction will be required. This fully removes the hazard and allows site preservation for eventual implant placement.
Leaving dead, infected tooth nerves untreated risks complications like chronic infection spreading to the jawbone, nearby teeth, and other body systems. Prompt dental treatment is key.
Frequently Asked Questions
Can a root canal tooth cause pain years later?
Yes, in some cases tooth pain can recur years after having a root canal procedure. This may happen due to:
- Residual bacteria sealed inside the tooth that multiply and reinfect through tiny leaks.
- A new crack or fracture in the tooth that allows bacteria to penetrate into the roots again.
- Development of a new infection near the root tip if the canal was not fully sealed to the end.
Retreatment to fully clean and re-seal the root canal system or apicoectomy surgery to remove infected tissue can stop the pain and save the tooth.
How long does a dead tooth last before falling out?
This depends on the individual tooth, how severely infected it is, and how much bone support remains around the dead roots. With no treatment, a necrotic tooth may slowly loosen and fall out on its own within 1-2 years typically. In some cases severely infected teeth deteriorate sooner.
Can a dentist tell if a tooth is dead based on color?
Darkening tooth color alone does not definitively indicate a dead tooth nerve, as many other factors can cause tooth discoloration. However, a grey, black or brown lifeless appearance in combination with other signs like no pain response strongly suggests pulp necrosis. The dentist will also check for widening of the periodontal ligament space around the suspect tooth root on x-rays.
What is the survival rate of a root canal treated tooth?
With modern techniques, root canal success rates are very high. The treated tooth can be retained in normal function for many years after. A systematic review of studies found an 89% survival rate of endodontically treated teeth at 8-10 years followup. With a crown placed, 10 year survival rates exceeded 95% for root filled teeth.
Can dental pulp be regenerated?
At present, natural regeneration of dental pulp and nerves after necrosis is not possible. However, ongoing research into advanced methods of regenerative endodontics shows promising potential for regrowing functional, innervated pulp tissue in cleaned-out root canals in the future.
Conclusion
Tooth nerve damage leading to pulp death can occur due to dental decay, trauma, aging, and other causes. Without blood flow and stem cells, lost dental nerve fibers and pulp tissue do not regenerate on their own once destroyed. While this leaves the tooth without sensation, modern root canal therapies can successfully retain the tooth for continued use.
Emerging biomedical techniques offer hope that we may eventually unlock the means to fully regrow living, sensory dental pulp after necrosis or removal. By better understanding the unique regenerative challenges teeth face and pioneering solutions to them, the potential exists to restore natural tooth nerve function.