Losing tooth structure and experiencing dental trauma is distressing. When teeth become damaged, it’s natural to wonder if there are ways for them to heal or regenerate. This in-depth guide examines the causes of tooth damage, prognosis for natural regrowth, and all the available treatment options.
What Causes Teeth to Become Damaged?
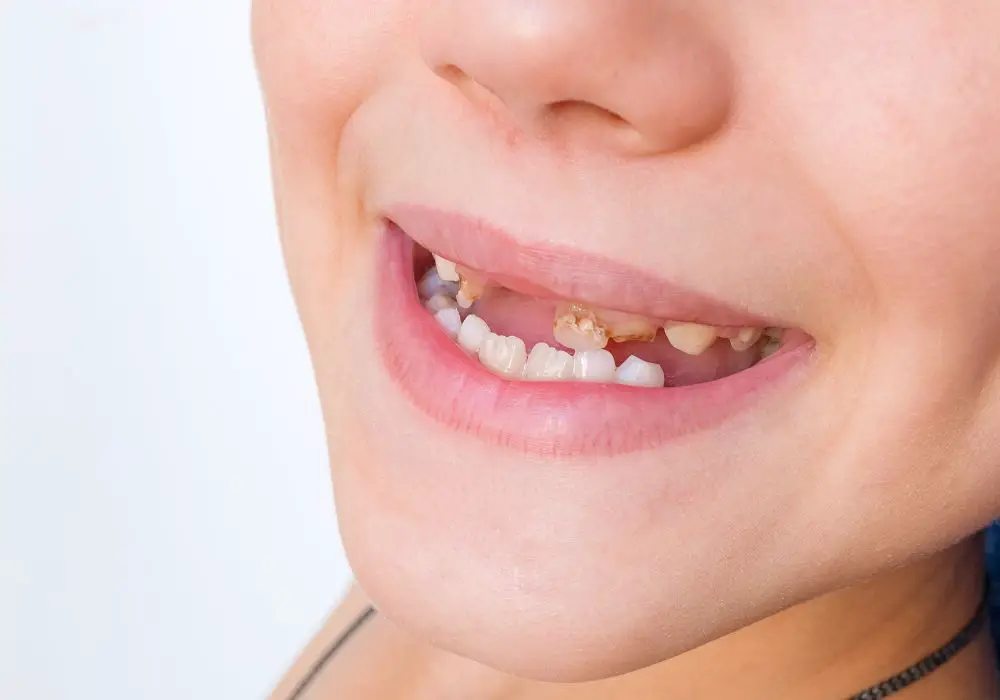
Teeth face threats to their structural integrity on a daily basis. Some common causes of damage include:
- Tooth decay – Bacteria and acidic foods erode enamel and dentin leading to caries and cavities. Left untreated, decay reaches the inner pulp tissue.
- Physical impact – Sports injuries, vehicle accidents, falls and blows to the mouth knock teeth out of place or cause fractures.
- Grinding and clenching – Constant compressive forces chip and crack teeth over time.
- Chewing hard items – Biting on ice, nuts, hard candy or other hard foods can crack enamel.
- Improper dental work – Overly aggressive drilling or improper use of dental tools during fillings or other treatments can weaken tooth structure.
- Periodontal disease – Gum infection erodes underlying bone leading to loose, mobile teeth prone to damage.
- Habits – Nail biting, opening items with teeth, and chewing on pens cap off enamel.
- Aging – Enamel naturally wears thin over decades of use, increasing susceptibility to chipping and fracture.
Knowing the root causes of dental damage allows you to minimize risk factors whenever possible through preventive care. But when damage does occur, what are the options? Can damaged teeth ultimately regrow to their natural state?
Factors That Influence Tooth Regrowth Potential
Several factors affect whether a damaged tooth can spontaneously heal or regenerate when injured:
- Type of tooth tissue injured – Enamel cannot regenerate since it lacks living cells. Dentin and pulp have some reparative capacity.
- Extent of injury – Minor loss of enamel may regrow via smoothing. But significant loss requires restoration. Exposed pulp unlikely to heal.
- Direction of crack or fracture – Vertical root fractures have poorer prognosis than horizontal cracks across chewing surfaces.
- Patient age – Younger teeth have greater healing potential due to robust blood supply and stem cells.
- Patient health – Those with diabetes, autoimmune disorders, or poor oral hygiene have lower regrowth potential.
- Prescription medications – Some drugs like antihistamines reduce saliva flow needed for natural remineralization.
- Presence of infection – Decay, abscess or periodontal disease inhibits natural healing capacity.
No two dental injuries are alike, so your dentist will assess all these factors to determine prognosis. But in general, minor damage to enamel or dentin can sometimes self-repair while more extensive loss of tooth structure cannot regrow on its own. Let’s explore why…
Tooth Anatomy and Ability to Regenerate
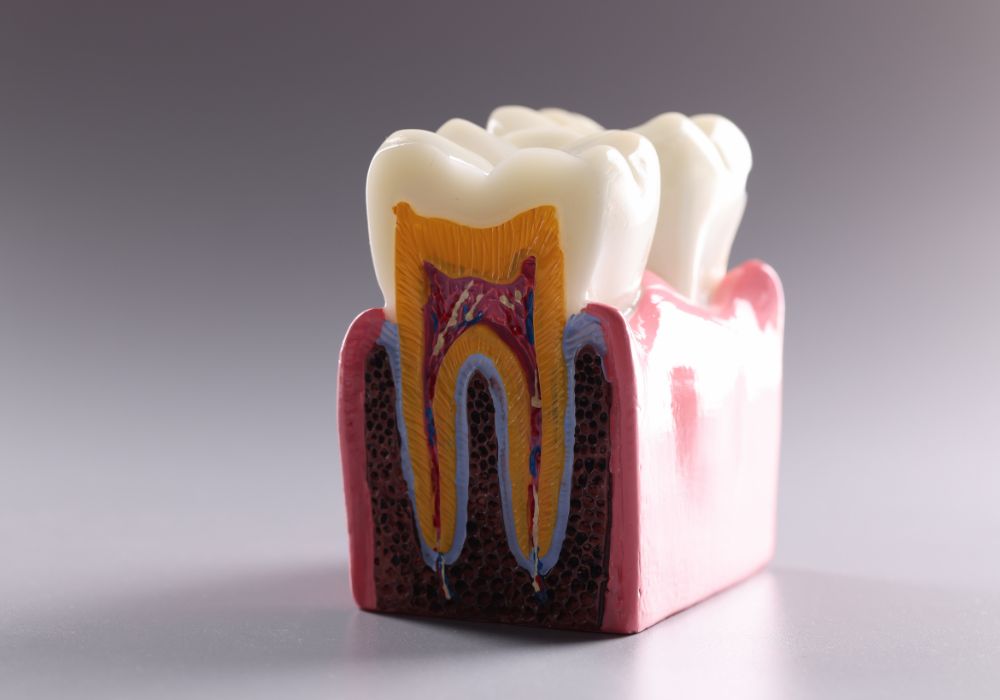
Teeth are composed of three layered materials with different regenerative capacities:
Enamel
Enamel forms the hard, white outer surface of the tooth crown. It is comprised of hydroxyapatite crystals that provide rigid strength. However, enamel lacks living cells and blood vessels. Once damaged, it cannot self-repair or regenerate. At best, minor enamel defects may slightly smooth out over time.
Dentin
Softer dentin material lies beneath enamel and makes up the bulk of each tooth. It contains microscopic tubules with fluid and living cells called odontoblasts that can lay down new dentin tissue. This gives dentin some ability to naturally regenerate when damaged. However, its capacity to fully restore significant structural loss is limited.
Pulp
At the center of the tooth is the pulp chamber containing soft tissue called the dental pulp. This consists of connective tissue, blood vessels, and nerves. The pulp plays a vital role in stimulating dentin production and overall tooth health. However, if exposed to bacteria, it readily becomes infected and inflamed. Damaged pulp tissue cannot adequately regenerate to a healthy state on its own without treatment.
In summary, enamel cannot regrow at all while dentin and pulp have only modest natural regenerative capacity when severely injured or infected. Next, let’s survey all the available options for professionally treating damaged teeth.
Professional Restorative Treatments for Damaged Teeth
The recommended treatment option depends on factors like:
- Amount of remaining healthy tooth structure
- Location and extent of damage
- Presence of pain or infection
- Cost considerations
- Patient preferences for aesthetics
Here are common professional solutions for restoring damaged teeth:
Dental Fillings
Fillings repair small to medium cavities or defects. The dentist first cleans out decayed material and then fills the space with metal amalgam or tooth-colored resin composites. Fillings help prevent further decay in the affected area.
Dental Crowns
Also known as caps, crowns fully surround the entire visible portion of the tooth above the gumline. The dentist drills down the tooth and then covers it with a custom-fitted crown restoration made of porcelain, ceramic, metal alloys or a combination of materials. Crowns strengthen and reinforce teeth with extensive structural loss.
Root Canal Therapy
When tooth decay or trauma exposes the soft pulp tissue, bacteria rapidly infect it. To save the tooth instead of extracting it, an endodontist performs a root canal procedure. This involves removing the infected pulp, cleaning and disinfecting inside the canals and tooth roots, then sealing the space with filling material.
Tooth Extractions
In cases of severe tooth damage where other options are not feasible due to extreme decay, fracture, or periodontal disease, extraction may be necessary. This surgically removes the problem tooth. It is replaced with a dental bridge, implant, or denture to restore the gap.
Dental Implants
Implants act as an artificial tooth root anchored in the jaw bone. The implant fuses with the bone in a process called osseointegration. A lifelike artificial crown is then affixed to the implant post to complete the restoration. Implants provide a permanent replacement for single missing teeth.
Dental Bridges
This restoration uses adjacent natural teeth as anchors to hold an artificial tooth in place where one is missing. The supporting teeth are crowned, and a false tooth is fused between them. The bridge essentially bridges the gap left by the lost tooth.
| Restoration | How it Works | Pros | Cons |
|---|---|---|---|
| Fillings | Remove decay & fill hole with amalgam or composite | Less tooth removal <br> Prevent more decay | Eventual replacement needed <br> Risk hitting nerves |
| Crowns | Cover over entire visible tooth | Reinforce weak teeth <br> Improve appearance | Require significant tooth removal <br> Higher cost |
| Root Canal | Remove infected pulp & seal canals | Save severely damaged tooth | Tooth becomes brittle <br>Risk of reinfection |
| Extractions | Surgically remove tooth | Eliminate source of infection | Area of bone loss <br> Gap in smile |
| Implants | Screw titanium post into jaw for crown | Look, feel & function like natural teeth | Surgical procedure <br> Higher upfront cost |
| Bridges | Use adjacent teeth to anchor false tooth | Maintain shape of smile | Higher decay risk <br> May need replacement |
Table 1: Comparison of restorative options for damaged teeth
Beyond these common treatments, emerging biomedical research offers hope that biologically regenerating damaged teeth may someday be possible. But for now, these are the standard professional solutions.
Can Damaged Teeth Ultimately Regrow? Regeneration Research.
As we’ve covered, enamel cannot regenerate and the capacity of dentin and pulp tissue to regrow is limited. Can modern science find ways to biologically regrow damaged teeth more effectively? Researchers are exploring innovative new approaches to tooth regeneration and engineering including:
Enamel Matrix Proteins
Enamel matrix derivative proteins applied to damaged teeth may encourage limited new enamel deposition by mimicking natural developmental processes. However, true complete enamel regrowth has not yet been achieved.
Stem Cell Regeneration
Stem cells harvested from dental pulp or other sources have shown potential to stimulate new dentin formation when applied to damaged teeth. This takes advantage of stem cells’ ability to differentiate into specialized dentin-producing cells.
3D Tooth Printing
This emerging technique prints live stem cells and biological materials onto a tooth-shaped scaffold. The goal is to eventually generate a living, functional bio-tooth replacement for dental implants. But much more research is needed.
Gene Therapy
Introducing genetic material via viral vectors shows promise for upregulating genes involved in natural tooth development. This may someday enable regrowing dental tissues.
While still highly experimental, these cutting-edge regrowth approaches give hope that science may one day find ways to biologically regenerate damaged teeth more effectively than current treatments.
Protecting and Caring for Teeth

Since extensively damaged teeth cannot yet be regrown, prevention is key to maintaining your natural dentition for life. Excellent oral hygiene and early intervention protect tooth integrity. Be proactive with these tips:
- Brush properly twice daily with fluoride toothpaste and floss once daily.
- Use antibacterial mouthwash to eliminate disease-causing oral bacteria.
- Limit sugary and acidic drinks and snacks that erode enamel.
- Wear a sports mouthguard to shield teeth from injury.
- Have professional cleanings every 6 months to remove harmful tartar buildup.
- See the dentist as soon as a chip or crack appears for prompt repair.
- Opt for tooth-colored fillings and bondings to aesthetically restore minor defects.
- Know your risk factors and take action to prevent damage from grinding, gum disease, etc.
- Research emerging biomedical approaches that may enable true tooth regeneration one day.
With diligent daily care and awareness of new treatment innovations, you can maximize preservation of your natural smile for years to come.
Conclusion
Severe trauma or disease can destroy tooth structure beyond the limited natural capacity to remineralize or regenerate. Enamel and dental pulp tissue cannot meaningfully regrow once lost. While experimental research offers hope for more biological regeneration in the future, currently the only ways to restore badly damaged teeth are through professional dental treatments like fillings, crowns, implants, extractions, and bridges. These aim to prevent further deterioration and restore the form and function of damaged teeth. Going forward, preventing damage proactively through excellent hygiene and prompt intervention when problems do arise gives you the best chance of maintaining your natural dentition for a lifetime.
FAQs About Damaged Teeth
Do teeth heal themselves?
Teeth have a limited ability to self-repair. Enamel cannot heal, but small areas of lost dentin may slowly regenerate over time. However, deeply damaged teeth with infected nerves or extensive structural loss cannot meaningfully heal without professional treatment.
Can dentists repair cracked teeth?
Yes, minor stress cracks and hairline fractures can often be stabilized and saved through fillings, inlays, onlays or crowns. The prognosis depends on the location and depth of the crack. Badly split or fractured teeth may still require extraction, but dentists will try to repair restoratively if possible.
How long does a fractured tooth take to heal?
True healing involves regrowth of lost dentin tissue which occurs slowly over months. With minor fractures, pain and sensitivity should gradually ease over several weeks as the underlying pulp calms down. The tooth may always remain weaker though. More severe fractures require restoration work to stabilize the tooth.
Can a dead tooth be saved?
If the tooth pulp tissue dies due to trauma, decay or injury, root canal therapy can still save the tooth. This removes the infected or dead pulp. The remaining tooth structure can still be retained through a filling or crown. However, the tooth becomes more brittle over time.
Do adult teeth grow back when pulled?
No, adult teeth do not grow back after being extracted. Lost roots cannot regenerate, and enamel/dentin lack adequate regenerative capacity. But lost teeth can be replaced with dental implants, bridges or dentures to restore chewing function and aesthetics. It’s best to save and repair damaged teeth when possible.