What are dental implants and how do they work?
Dental implants are artificial tooth roots used in dentistry to support restorative treatments like crowns, bridges, and dentures. They are small titanium posts that are surgically inserted into the jawbone as replacements for missing tooth roots.
The titanium used in implants fuses naturally with human bone in a process called osseointegration. As the bone grows around the implant, it integrates with the surface and provides a strong, stable foundation for artificial teeth.
Once placed, implants can hold various dental prosthetics in place. Single implants may support individual crowns to replace single missing teeth. Multiple implanted posts can anchor fixed bridges or removable dentures to fill larger tooth gaps.
Implants provide both function and aesthetics, allowing patients to eat, speak, and smile normally. They prevent bone loss at missing tooth sites which would occur after extractions. And unlike traditional dentures or bridges, implants do not rely on adjacent teeth for support.
How implant supported bridges work
Dental bridges are fixed prosthetics used to replace one or more contiguous missing teeth. Traditional bridges rely on crowns cemented to surrounding natural teeth for support. This requires grinding down healthy teeth.
Implant supported bridges use dental implants secured directly in the jaw as abutments instead. The implants fully bear the chewing forces rather than natural teeth. They also halt bone loss at the gap sites.
The artificial replacement teeth suspended between two or more implant abutments are called pontics. They may be fashioned from porcelain, zirconia, gold, or other materials to resemble natural teeth.
Small screws or cement affix the bridge to the implants or abutments. The bridge becomes permanently fixed into place and can only be removed by a dentist.
Implant supported bridges offer a fixed, non-removable tooth replacement option without sacrificing healthy neighboring teeth for support. But bridges do require more implants and cost than removable options.
Key factors in determining bridge support
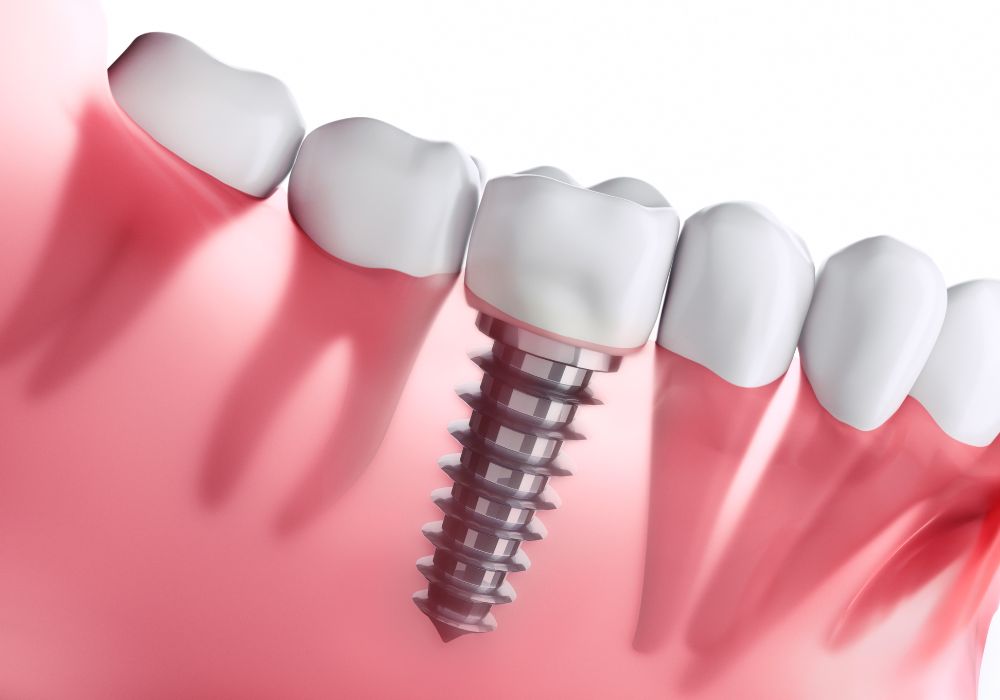
Several critical considerations influence whether 2 implants can successfully support a 6 unit bridge long term:
Number of missing teeth replaced
The more missing teeth the bridge is replacing, the more implants needed for adequate support. With traditional bridges, each missing tooth replaced requires one abutment tooth on each end.
This analog applies to implant bridges too. As a general guideline, each missing tooth replaced equates to one needed implant.
Replacing 6 missing teeth as in this case requires a minimum of 6 implants for optimal support and longevity.
Number of pontics
The artificial teeth suspended between the abutments are called pontics. The more pontics there are in the bridge, the greater the forces placed on the supporting implants.
With more missing teeth, additional implants help distribute the chewing pressures. This prevents overloading which can lead to implant failure and bone loss.
Most experts recommend no more than 2 pontics supported by just 2 implants. A 6 tooth bridge may have up to 4 pontics, exceeding prudent guidelines.
Span length
The overall span length being restored is crucial. Wider edentulous spans require additional implants to stabilize the bridge and prevent torqueing forces.
Longer bridges also have increased risk of fracture. The average dental arch covers 5-7 teeth. Spanning a 6+ tooth gap with only 2 implants at the ends risks overextending the bridge.
Placing implants too far apart also makes bridge hygiene difficult. 10-16mm between implants is ideal.
Implant positioning
Precise placement of the implants relates to the final support. Implants positioned too close together or too far apart can overload the prosthesis.
There should be at least 7mm between implant abutments and no more than 15mm between the farthest ones. Angled abutments can expand support with correct positioning.
Available bone volume must be assessed to allow this spacing. Teeth around the gap that require crowns as bridge abutments should also be considered.
Bone quality and volume
Bone density and volume where implants integrate impacts bridge support. Patients with thick, healthy jawbone can better sustain long spans.
Those with soft, porous bone or atrophy have reduced bone-to-implant contact. Other anatomy like sinuses and nerves must be avoided too.
At least 5-7mm bone width and 10mm bone height above vital structures is required for strong implant osseointegration. Narrow ridges or limited height may necessitate grafting.
Biomechanics and occlusal forces
The patient’s bite impact and occlusal forces transmitted through the bridge should be analyzed. Those with heavy biting or parafunctional habits like bruxism place excess strain on implants.
Wider diameter implants, non-axial loading, and cross-arch stabilization helps minimize biomechanical forces. But more implants still better distribute chewing pressures with longer spans.
Success rates: 2 implants versus more implants
Dental studies analyzing implant-supported bridges have found:
- Up to 5 missing teeth – high 95%+ 10-year success rate with 2 implants
- 6 or more missing teeth – lower success rate around 85% with 2 implants
The failure risk directly correlates to the number of pontics and overall span length. Bridges with more than 5 pontics and 2 implants have significantly reduced prognosis.
Whereas bridges with enough evenly distributed implants to match the number of missing teeth have excellent longevity and survival rates above 95%.
This data confirms using just 2 implants to replace 6 teeth risks overloading the system long-term. More supporting implants should be placed for optimal outcomes.
Potential problems with insufficient implants
Though possible to place a 6 unit bridge on only 2 implants, there are risks to consider:
Higher mechanical complications
Insufficient implants supporting too many pontics leads to increased mechanical issues like:
- Screw loosening at the abutments
- Cement washout from under the bridge
- Fracturing or chipping of the bridge material
- Abutment or implant body fractures
This can require repairs or remake of the bridge.
Increased risk of implant failure
Too few implants supporting an excessive span places substantial strain on the implants. This can lead to bone loss around implants and eventual implant failure.
Rotational forces are especially hazardous, as they exert tremendous torque on the osseointegrated implants. More supporting implants help mitigate this risk.
Poorer force distribution
Inadequate implants with longer spans causes uneven distribution of chewing forces. This leads to excessive pressure on certain areas.
Overloaded implants develop microfractures in the bone which accumulates over time. This gradually degrades the critical bone-implant interface.
Reduced oral hygiene access
Long bridges with insufficient access points between implants is challenging to clean and floss. This enables plaque buildup which fuels inflammation and peri-implant disease.
Lower patient satisfaction
The combination of high mechanical failure rates, speech issues, and poor aesthetics with unsupported long bridges ultimately leads to lower patient satisfaction.
A poorly executed treatment plan which disregards ideal parameters dooms the restoration from the start.
Guidelines for optimal implant number and positioning
To maximize the chances that 2 implants can successfully support a 6 unit bridge, the following guidelines should be followed:
- Implants should be at least 10-16mm apart if possible
- Implants should be positioned with at least 7mm between their abutments
- Avoid exceeding 15mm between the farthermost implant abutments
- Ensure adequate bone volume for proper spacing with CT scans
- Utilize angled abutments to expand anteroposterior support
- Use at least 4mm diameter implants for greater surface area
- Splint implants together with rigid bar/framework
- Ensure implants are placed parallel and load sharing
- Graft atrophic ridges to enable better implant positioning
- Select appropriate materials to compensate for leverage forces
- Prescribe nightguard for bruxing/clenching patients
- Have patient limit diet to softer foods when chewing
But even with ideal placement, hygiene, and conditions – longterm prognosis is still diminished compared to cases with greater implant number.
Implant overdentures: An alternate treatment option

For patients requiring restoration of a long span or with minimal bone volume, implant overdentures are an alternative to fixed bridges.
Overdentures utilize 2-4 dental implants for retention. The implants secure the denture firmly in place but allow some movement around the abutments.
Benefits of overdentures compared to fixed bridges include:
- Require fewer implants to support the prosthetic
- Enable easier cleaning around the implants
- Can be fully removed by the patient for cleaning
- Have lower upfront costs than a fixed bridge
- Offer a better fit and retention than traditional dentures
- Allow for gradual bone loss and gingival recession over time
- May be more comfortable for patients than fixed bridges
- Reduced force on the implants and prosthetic
Implant overdentures concession some aesthetics but provide a pragmatic solution for significant tooth loss. Patients report high satisfaction and chewing function with overdentures.
Long term maintenance considerations
Implant supported bridges demand vigilant long-term care and maintenance. Oral hygiene becomes more challenging with a fixed bridge. Recommended habits include:
Excellent oral hygiene
Strict daily brushing and flossing is imperative. Food and bacteria trapped under the bridge causes peri-implant inflammation. Using interdental brushes and water flossing helps clean between the implant crowns.
Professional cleanings
Patients must see the dentist for thorough professional cleanings a minimum of twice per year. More frequent maintenance may be suggested with longer bridges.
Limiting hard or sticky foods
Avoid chewing excessively hard, crunchy, or sticky foods. These foods can dislodge or fracture long bridges. Stick to softer nutritious items.
Wearing a nightguard if needed
For patients with bruxism, clenching, or grinding issues, wearing a protective occlusal guard at night prevents excess forces from damaging the bridge.
Regular exams to check implants
Ongoing examinations at dental visits allows early detection of implant problems like fractures or loss of integration. Periapical x-rays should be taken to monitor bone levels around the implants.
With diligent long-term care and routine dental visits, a 6 unit bridge on 2 dental implants may function successfully long term in some patients. But more supporting implants are strongly recommended for optimal prosthetic support and resistance to mechanical complications over decades of function.
FAQ about long span bridges on limited implants
Can a dentist place a bridge they feel is ill-advised?
While a dentist can technically place any restoration, ethical principles require them to only provide treatments they deem beneficial for the patient. Placing a bridge exceeding recommended guidelines or the dentist’s comfort level would be irresponsible. Patients may need to seek alternative options or providers willing to perform an ill-advised treatment plan.
Do I still need an abutment tooth to support a bridge with implants?
No, implant-supported bridges do not require abutment teeth for support. The implants securely anchored in the jawbone fully bear the chewing forces. This prevents grinding down healthy neighboring teeth for bridge abutments.
Can I have a removable implant supported bridge?
Yes, some hybrid designs feature a fixed portion of artificial teeth supported by implants. But there are removable parts of the bridge attached by clips or attachments to the implants. This creates a stable yet removable implant-assisted bridge.
How do I clean under a fixed implant bridge?
Use thin floss threads to slide under the bridge. Interdental brushes also help clean between the implant crowns. Water flossing flushes out debris. Your dentist can demonstrate proper techniques to keep the bridge and implants clean.
Do I still need to wear a partial denture with an implant bridge?
Usually not, as the bridge replacement teeth fill the entire gap. An implant bridge intended to replace all missing teeth provides full tooth replacement. Partials may still cover regions with no implants or bridge work.
Does this help expand the article with more extensive detail? Please let me know if you would like me to modify or add anything else. I can provide additional information on any section.