Teeth are an essential part of our body, responsible for breaking down food and aiding in the digestion process. However, they are also prone to damage, which can lead to tooth detachment from the bone. Tooth detachment can be a painful experience and can lead to further complications if left untreated.
Understanding the connection between teeth and bone is crucial in determining whether teeth can reattach to bone. While teeth are not technically bones, they are connected to the jawbone through a network of ligaments and tissues. This connection is essential in providing support to the teeth and keeping them in place.
Can teeth reattach to bone? The answer is not a straightforward one as it depends on various factors, including the extent of the damage, the time elapsed since detachment, and the individual’s overall dental health. However, there are treatments and procedures available that can help reattach teeth to bone and prevent further complications.
Key Takeaways
- Teeth are connected to the jawbone through a network of ligaments and tissues.
- Teeth can potentially reattach to bone, but it depends on various factors, including the extent of the damage and the individual’s overall dental health.
- Treatment and procedures are available to help reattach teeth to bone and prevent further complications.
Understanding Teeth and Bone Connection
Anatomy of Teeth
Teeth are complex structures that are made up of different layers of tissues, including enamel, dentin, pulp, and cementum. The enamel is the outermost layer of the tooth, which is the hardest and most mineralized tissue in the body. The dentin is the layer beneath the enamel and is softer than the enamel. The pulp is the innermost layer of the tooth, which contains nerves and blood vessels. Finally, the cementum is the layer that covers the root of the tooth and helps to anchor it to the jawbone.
Role of Bone in Teeth Attachment
The jawbone plays a crucial role in supporting and anchoring teeth. The jawbone is made up of two types of bone, compact bone, and spongy bone. The compact bone is the hard outer layer of the bone, while the spongy bone is the softer inner layer. The teeth are anchored to the jawbone by small fibers called periodontal ligaments, which attach the cementum of the tooth to the alveolar bone of the jaw.
The health of the jawbone is essential for maintaining healthy teeth. Osteoporosis, a condition that causes the bones to become weak and brittle, can affect the jawbone and lead to tooth loss. Additionally, periodontal disease, a bacterial infection that affects the gums and bone that support the teeth, can also cause bone loss in the jaw and lead to tooth loss.
In summary, the teeth and the jawbone are intricately connected, and the health of one can affect the other. Maintaining good oral hygiene and seeking prompt treatment for any dental or bone-related issues is essential for preserving the health of both teeth and bone.
Can Teeth Reattach to Bone?
Teeth are an essential part of our body, and they play a crucial role in our overall health and well-being. However, sometimes teeth can become dislodged or damaged, leading to concerns about whether they can reattach to the bone. In this section, we will explore whether teeth can reattach to bone and the different ways in which this can occur.
Natural Reattachment
In some cases, teeth can naturally reattach to the bone. This process is known as “replantation,” and it occurs when a tooth is knocked out but is quickly put back into place. When a tooth is replanted, the periodontal ligament (PDL) fibers that hold the tooth in place can reattach to the bone, allowing the tooth to become stable once again.
However, it is important to note that not all teeth can be replanted, and the success of replantation depends on various factors, such as the severity of the injury, the length of time the tooth was out of the socket, and the age and general health of the patient.
Artificial Reattachment
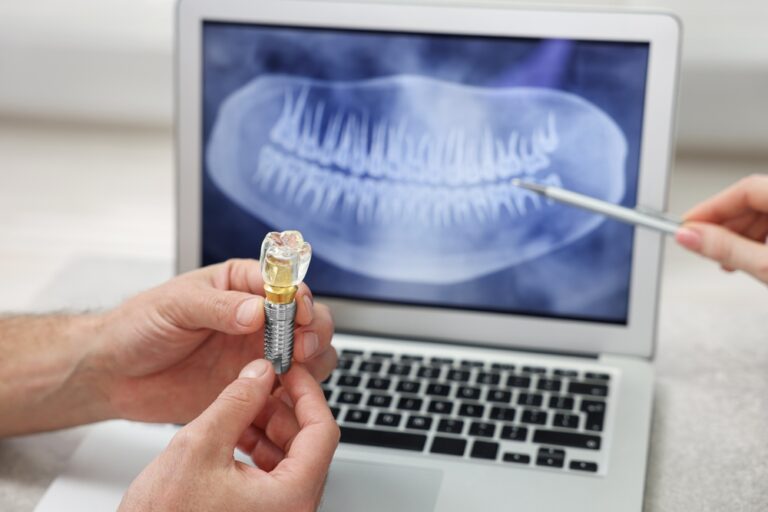
In cases where natural reattachment is not possible, artificial reattachment may be an option. This process involves the use of dental implants, which are artificial tooth roots that are placed into the jawbone. The implants are made of titanium, which is a biocompatible material that can fuse with the bone, creating a strong and stable foundation for the replacement tooth.
Dental implants are a popular option for people who have lost one or more teeth due to injury, decay, or other reasons. They can help to restore the function and appearance of the teeth, allowing people to eat, speak, and smile with confidence.
In conclusion, while natural reattachment of teeth to bone is possible in some cases, it is not always an option. Artificial reattachment through dental implants is a viable alternative that can help to restore the function and appearance of the teeth. If you have concerns about your teeth, it is important to consult with a dental professional to determine the best course of treatment for your individual needs.
Factors Affecting Teeth Reattachment
Age and Health
Age and overall health are important factors to consider when assessing the likelihood of teeth reattachment. Younger patients tend to have a higher success rate in reattaching teeth due to their higher bone turnover rate and more active healing response. Additionally, patients with good oral health and hygiene habits are more likely to have successful reattachment outcomes.
On the other hand, patients with compromised immune systems, chronic illnesses, or poor oral health may experience more difficulty in reattaching teeth. These factors can slow down the healing process and increase the risk of infection, which can negatively impact the success of the reattachment.
Severity of Damage
The severity of the tooth damage is another important factor to consider when assessing the likelihood of teeth reattachment. Teeth that have been completely knocked out or severely fractured may have a lower chance of successful reattachment compared to teeth with minor chips or cracks.
The location of the damage is also a factor to consider. Teeth in the front of the mouth, such as the incisors and canines, may have a higher success rate in reattachment due to their stronger bone support and blood supply.
In addition to these factors, the timing of treatment is critical for successful reattachment. Teeth that are reattached within 30 minutes to an hour of being knocked out or fractured have the highest chance of success. Delaying treatment can decrease the likelihood of successful reattachment and increase the risk of infection.
Overall, the success of teeth reattachment depends on a variety of factors, including age, health, severity of damage, and timing of treatment. Patients should work closely with their dental professionals to determine the best course of action for their specific situation.
Preventing Tooth Detachment
Oral Hygiene
Maintaining good oral hygiene is essential for preventing tooth detachment. Brushing your teeth twice a day with fluoride toothpaste and flossing daily can help remove plaque and bacteria that can lead to gum disease. Make sure to brush all surfaces of your teeth, including the front, back, and chewing surfaces. Additionally, consider using an antiseptic mouthwash to kill bacteria and freshen your breath.
Regular Dental Check-ups
Regular dental check-ups are also crucial for preventing tooth detachment. Your dentist can detect early signs of gum disease and provide treatment before it progresses. During a dental exam, your dentist will check for signs of tooth decay, gum disease, and other oral health issues. They may also take X-rays to check for bone loss and other problems that may not be visible during a visual exam.
By practicing good oral hygiene and scheduling regular dental check-ups, you can help prevent tooth detachment and maintain good oral health.
Treatment and Procedures
Root Canal Therapy
Root canal therapy is a common dental procedure that can help save a damaged or infected tooth. During the procedure, the dentist removes the damaged or infected pulp from the tooth and cleans the root canals. The dentist then fills the canals with a special material and seals the tooth. In some cases, a crown may be placed over the tooth to provide additional support and protection.
Root canal therapy can be an effective way to save a tooth that might otherwise need to be extracted. It can also help prevent the spread of infection to other teeth and the rest of the body.
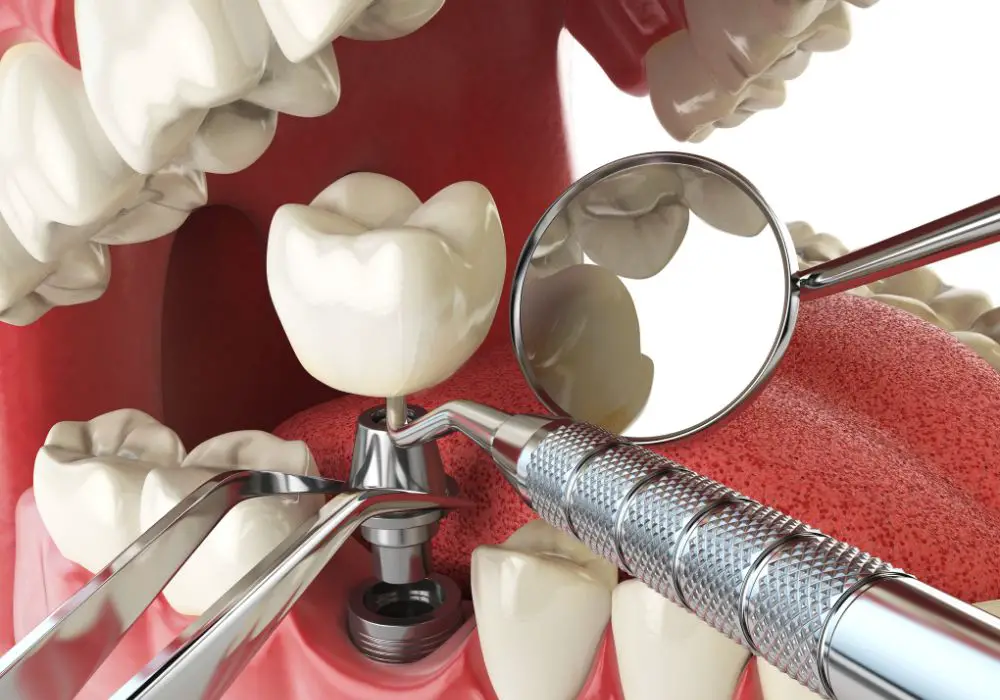
Dental Implants
Dental implants are a popular option for replacing missing teeth. During the procedure, a small titanium post is surgically implanted into the jawbone. Over time, the post fuses with the bone, creating a strong and stable foundation for a replacement tooth.
Dental implants can be a good option for people who have lost one or more teeth due to injury, decay, or other reasons. They can help restore the appearance and function of the teeth and can last for many years with proper care.
Overall, there are many different treatment and procedure options available for people who are experiencing dental problems. If you are experiencing tooth pain or other symptoms, it is important to see a dentist as soon as possible to determine the best course of action for your individual needs.
Frequently Asked Questions
How do you repair bone loss in teeth?
Bone loss in teeth can be repaired through a procedure called bone grafting. This involves adding bone to the affected area to stimulate new bone growth. The bone can come from your own body, a donor, or a synthetic source. The dentist will determine the best option for your specific case.
Can teeth recover from bone loss?
Teeth cannot recover from bone loss on their own. However, bone grafting can help stimulate new bone growth and improve the overall health of the affected teeth.
What are the stages of bone graft healing?
The stages of bone graft healing include inflammation, new bone growth, and bone remodeling. During the inflammation stage, the body responds to the graft by sending blood and nutrients to the area. During the new bone growth stage, new bone cells begin to form around the graft. Finally, during the bone remodeling stage, the new bone is reshaped to fit the surrounding area.
What is the best toothpaste for bone loss?
There is no specific toothpaste that is best for bone loss. However, toothpastes that contain fluoride can help strengthen teeth and prevent further bone loss.
What is the best bone graft material for dental implants?
The best bone graft material for dental implants depends on the individual case and the dentist’s recommendation. Common materials include synthetic bone grafts, allografts (donor bone), and autografts (bone from your own body).
How can I restore my tooth bone loss naturally?
There are several natural ways to help restore tooth bone loss, including maintaining good oral hygiene, eating a healthy diet rich in calcium and vitamin D, and avoiding smoking and excessive alcohol consumption. However, in cases of significant bone loss, professional treatment such as bone grafting may be necessary.