Good oral health is essential to overall health and well-being. Our teeth allow us to chew and digest food properly, speak clearly, and smile confidently. Poor oral health can lead to issues like tooth decay, gum disease, bad breath, and tooth loss. These problems can cause pain, difficulty eating, low self-esteem, and increased risk for other serious health conditions. So while it may be possible to “survive” with bad teeth, maintaining good oral hygiene and seeking prompt treatment is vital for quality of life.
What constitutes “bad teeth”?
There are various conditions that can be described as “bad teeth.” Here are some of the most common:
Tooth decay
Also known as dental caries or cavities, tooth decay occurs when plaque bacteria consume sugars in food and produce acids that erode tooth enamel. If left untreated, decay can cause holes in teeth and toothache. It can eventually lead to infection and tooth loss.
Gum disease
Gum disease begins when plaque builds up along and under the gumline. This causes gums to become inflamed and can lead to gingivitis. If gum disease worsens into periodontitis, the deeper tissues and bone can be damaged, resulting in loose teeth or tooth loss.
Discoloration
Teeth can become discolored or stained from food and drink, smoking, medications, or trauma. Discoloration ranges from yellowish to brown or black. Severely discolored teeth can be unsightly and embarrassing.
Misalignment
Crooked, crowded, or gapped teeth are signs of misalignment. This can increase risk for tooth decay, gum disease, and other problems like speech impediment or jaw pain.
Tooth damage/loss
Teeth that are cracked, chipped, broken, or knocked out partially or fully have structural damage. Complete tooth loss can occur from decay, trauma, or advanced gum disease.
Consequences of leaving bad teeth untreated
Neglecting oral health problems allows them to worsen over time. Potential consequences include:
- Severe tooth decay leading to infection and abscesses
- Gum disease progressing to irreversible bone and tooth loss
- Increasing difficulty chewing, which can cause poor nutrition
- Tooth fracture due to weakened tooth structure
- Spread of infection to other teeth
- Bone loss in the jaw
- Increased risk of heart disease and stroke
- Higher likelihood of dementia
- Poor speech development for children
Leaving bad teeth untreated affects far more than just the mouth. It can seriously undermine both short-term and long-term health.
Is it possible to survive with bad teeth?
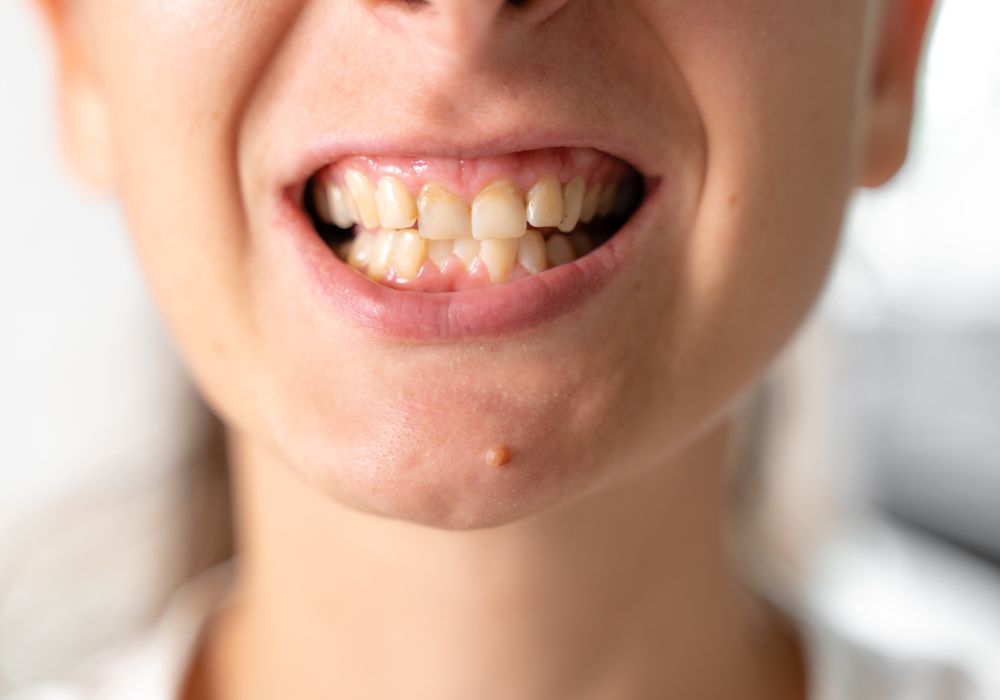
Surviving with bad teeth is possible but not recommended. As mentioned, poor oral health negatively impacts overall wellbeing and quality of life. Here are some key points on survivability:
- Tooth loss: People can survive without any natural teeth if they adapt their diets, wear dentures, or get dental implants. But tooth loss is best avoided.
- Decay: With modern dentistry, severe tooth decay can often be treated by fillings, crowns, or root canals. However, infections may eventually require extraction.
- Gum disease: This can be managed with good hygiene and professional cleanings. But progressive bone loss can still lead to loose teeth.
- Discoloration: While unsightly, tooth discoloration alone doesn’t affect health. But it should be examined to rule out decay.
- Misalignment: Crooked teeth typically don’t directly affect survival. But orthodontics might be needed to prevent other oral health issues.
- Pain: Dental pain from decay, gum disease, damage, or loss can be excruciating but not life-threatening. Although it can severely impact eating abilities and quality of life.
The bottom line is that while you can continue living with poor oral health, there are likely to be significant effects on your overall health, nutrition, speech, pain levels, and self-esteem. Proper dental care is always recommended.
Risk factors for bad teeth
Certain factors can increase risk for poor oral health and “bad teeth.” Being aware of these risk factors allows people to take preventive action:
- Poor dental hygiene: Insufficient brushing, flossing, and professional cleanings allow decay and disease.
- Unhealthy diet: Excess refined carbohydrates and sugar promote tooth decay.
- Dry mouth: Reduced saliva flow increases cavities and gum disease. Caused by medicines, health conditions, aging.
- Enamel issues: Poor enamel formation in childhood increases lifetime decay risk.
- Tobacco use: Smoking and chewing tobacco stain teeth and increase gum disease.
- Grinding teeth: Wearing down tooth enamel raises sensitivity and decay risk.
- Genetics: Some people inherit increased susceptibility to tooth decay or misaligned teeth.
- Health conditions: Diabetes, eating disorders, reflux disease, HIV/AIDS, and others affect oral health.
- Medications: Hundreds of prescription and over-the-counter medicines impact oral health.
- Drug/alcohol abuse: These substances increase risks for enamel erosion, gum disease, tooth grinding.
Recognizing personal risk factors allows you to modify behaviors, get preventive dental care, and avoid the development of “bad teeth.”
Tips for better oral health and survival
If you currently have bad teeth, or want to prevent them in the future, here are some evidence-based tips:
- Brush teeth thoroughly twice daily with fluoride toothpaste
- Floss once daily to remove plaque from between teeth
- Get professional cleanings and exams every 6 months
- Limit sugary and acidic foods and beverages
- Drink water and chew sugar-free gum to produce more saliva
- Don’t smoke or use other tobacco products
- Get dental issues treated early before they worsen
- Wear a night guard if you grind your teeth
- Take good care of any dental prosthetics like dentures
- Follow any special oral hygiene guidelines if you have health conditions or take meds that increase decay risk
- Eat a balanced diet rich in whole grains, dairy, fruits and vegetables
Prioritizing prevention and promptly treating any problems as they arise are keys to avoiding bad teeth and maintaining good oral health. With proper home care and professional treatment, you can survive and thrive.
Can bad teeth heal themselves?
Unfortunately, most dental problems do not heal themselves and require professional treatment. Here’s an overview:
- Tooth decay: Cavities do not heal on their own. They require fillings or possible root canals/crowns if neglected.
- Gum disease: This progresses without treatment. Professional cleanings and antibiotics are needed to halt damage.
- Tooth damage: Chipped or cracked teeth do not heal and often get worse over time, eventually requiring crowns or extraction.
- Misalignment: Crooked teeth typically get more crowded. Orthodontic intervention is needed to straighten teeth.
- Discoloration: Teeth do not regain their natural color on their own. Whitening treatments are needed to lighten stains.
The body is not able to rebuild tooth enamel or heal gum tissue that is diseased. Seeking regular dental care is crucial to treating issues promptly before they can worsen and cause permanent tooth loss. With today’s modern treatments, even severely damaged teeth can often be restored.
When to see a dentist immediately
While most oral health issues can wait to be addressed at your regular dental visits, some require emergency or urgent treatment. See a dentist right away if you experience:
- Severe toothache
- Bleeding gums that won’t stop
- Painful swelling in mouth, jaw, or gums
- Sudden tooth loosening or tooth loss
- Difficulty breathing or swallowing
- Trauma causing teeth to crack, break, or be knocked out
- Significant decay or damage to several teeth
- Unbearable sensitivity or pain from hot/cold foods
- Red, swollen, painful bumps in mouth
Leaving these acute issues unchecked can allow infections to spread and cause serious health consequences. Having a dentist evaluate urgent symptoms prevents complications and additional dental damage. In certain situations, an emergency room visit may be required for pain relief until a dental appointment is available.
Overcoming dental phobia and anxiety
Many people avoid or delay dental care due to phobia or anxiety. This allows oral conditions to worsen. There are several techniques to make dental visits easier:
- Find an understanding dentist willing to ease you slowly into care.
- Take an oral sedative prescribed by your dentist before appointments.
- Use distraction techniques like music headphones during procedures.
- Ask your dentist to thoroughly explain treatments beforehand so you know what to expect.
- Consider “medically anxious” dentistry, which offers nitrous oxide and other accommodations.
- Have a trusted friend or relative accompany you to appointments for moral support.
- Focus on what outcome you want (like a cavity fixed or cleaner teeth), not the procedure itself.
- Practice deep breathing and relaxation techniques to stay calm.
- Request frequent breaks during longer treatments if needed.
Seeking regular dental care is essential for your health, even if you have anxiety. With patience and the right help, you can overcome fear and get your oral health back on track.
Should you get dental insurance with bad teeth?
Getting dental insurance can make receiving and affording needed treatments much more feasible if you currently have bad teeth that require extensive restoration. Here are some factors to consider:
- Coverage for “pre-existing conditions” – Most dental insurance plans cover pre-existing problems like decay and gum disease as long as you meet any waiting periods.
- Type of plan – Dental HMO plans cost less in premiums but restrict treatment options. PPO plans cost more but allow you to use any dentist.
- Annual maximum benefit – Most dental plans have an annual limit ranging from $1000-$2500. Make sure it will adequately cover your expected costs.
- Major treatment coverage – Many plans only cover 50% of major work like crowns, dentures, or implants. Review your copay responsibility.
- Orthodontic coverage – If you require braces or aligners, verify that the plan covers orthodontics.
- Premium cost – Weigh monthly premiums vs. out-of-pocket costs to find an optimal balance.
- Waiting periods – Most plans impose waiting periods for certain treatments, typically 3-6 months for basic care up to 12+ months for major restorative work.
Having dental insurance can significantly offset the cost of needed care. But review your specific plan details closely to ensure adequate coverage.
Dental tourism for severe dental problems
Some patients with extensive dental issues pursue dental tourism for major restorative or reconstructive treatments. Key aspects include:
- Cost savings – Treatment abroad can cost 20-40% less after travel expenses. But results vary greatly.
- Travel required – Dental tourism requires time off and travel to another country. This includes extra planning.
- Varying standards – Other countries may have lower dental care standards, laws, and liability limitations. Do your due diligence.
- Communication – Language and cultural barriers may make conveying needs more difficult. Use a facilitator.
- Follow-up – Complications or adjustments often cannot be addressed locally, requiring a return trip.
Dental tourism works best for simpler, isolated treatments. It likely does not make sense for complex full-mouth restorations. Work with experienced facilitators and vet providers thoroughly. While savings are possible, the lowest prices often reflect lower quality.
Overview of full mouth restoration
Those with severe tooth decay, gum disease, or other extensive dental issues may need full mouth restoration for a healthy, functional smile. This extensive treatment can include:
- Deep cleanings to treat and halt gum disease
- Tooth extractions for severely damaged or unsalvageable teeth
- Bone and ridge augmentation to support dentures or implants
- Root canals and crowns to save compromised teeth
- Dental implants to replace missing teeth and support bridges
- Dental bridges and dentures to fill any remaining gaps in the smile
- Veneers, crowns, or bonding to improve aesthetics
Full mouth restoration is typically done in phases over weeks or months to allow healing between procedures. While the process is lengthy and costly, it provides the foundation for renewed oral health, function, and an attractive smile. Ongoing hygiene care and maintenance are then required to protect that investment.
Frequently asked questions
Can I survive without teeth?
Yes, it is possible to survive without any natural teeth as long as you are able to consume a soft, nutritious diet, and replace missing teeth with well-fitted dentures or dental implants to allow proper chewing and nutrition. However, losing all teeth can significantly affect quality of life.
Is tooth loss inevitable as you age?
No, tooth loss is not an inevitable part of aging. Maintaining excellent oral hygiene and obtaining prompt treatment for problems can allow you to keep your natural teeth for life. Teeth are not inherently destined to fall out as you get older.
Can chewing gum help bad teeth?
Sugar-free gum can help strengthen teeth and improve oral health by increasing saliva production which washes away food and neutralizes acids. Look for gum containing xylitol, which inhibits cavity-causing bacteria. However, gum cannot treat underlying conditions like tooth decay, which requires professional dental treatment.
Are dental problems genetic?
Genetics can be a factor in some dental issues like crooked teeth or soft enamel that chips more easily. But in general, oral health has more to do with lifestyle habits. Even with genetic susceptibility, good hygiene and avoiding sugary foods can minimize problems.
Should I avoid sugar completely with bad teeth?
While excess sugar certainly contributes to cavities, you do not need to eliminate it completely. Just limit sugary foods to mealtimes, choose less sticky sweets like dark chocolate, always rinse afterwards, and balance it out with plenty of tooth-healthy foods high in water and minerals. Moderation is key.