It can be very frustrating when you notice pain or discomfort in just one tooth whenever you eat sugary or cold foods. This type of sensitivity is usually a sign of an underlying dental problem needing attention. Getting to the root cause of why sweets make a specific tooth hurt allows you to find the right solution. This article explores the most common reasons why one tooth may hurt when eating sugary foods along with symptoms, diagnostic methods, treatment options, at-home remedies, and when to see a dentist.
Common Causes of Pain in One Tooth with Sweets

There are several possible causes for pain in a single tooth when consuming sugary foods:
Tooth decay
Tooth decay, or cavities, are the most common reason for discomfort when eating sweets. Cavities are holes formed in the enamel and dentin of a tooth when plaque bacteria consume sugar and release acids that degrade the mineral content of the tooth. Over time, this erosion causes pitting and breakdown of the enamel surface. As cavities grow larger and deeper, they can reach the inner soft pulp layer containing the tooth’s nerves. The exposure of the nerve endings makes teeth extremely sensitive, causing sharp pain when something sweet touches the decayed spot. The pain is often intense but short-lived, subsiding once the sugary food is removed. However, the cavity remains unsightly and vulnerable to further damage if untreated.
Cracked or fractured teeth
Cracks and fractures in a tooth also frequently cause jolts of pain when eating cold, hot, or sugary foods. Cracks allow external stimuli like sugar to penetrate deep into the tooth and reach the inner dentin and pulp layers. This irritation of the inner tooth triggers pain signals. The cracks may be tiny hairline fractures not visible to the eye or large fissures apparent on the enamel surface. Choosing sticky, sugary foods tends to accentuate symptoms as the sugar seeps deep into the cracks. The pain may come and go randomly or only when chewing on the cracked tooth. Fractures left unchecked can lead to infection of the inner tooth pulp.
Dental work like fillings or crowns
After having fillings, crowns, or other restorative work done, teeth often experience temporary sensitivity as they recover from the dental procedures. The preparation work to place fillings and crowns removes some enamel and dentin, exposing microscopic tubules in the dentin that lead to the tooth pulp and nerves. This reduces the insulation protecting the inner tooth layers, making the tooth more reactive to hot, cold, air, and sugary stimuli. Symptoms normally improve over time as the tooth heals and adjusts to the dental work. But sugary foods can still cause irritation during the recovery period, especially if the dental work is defective or ill-fitting.
Receding gums
Receding gums due to gingivitis or periodontal disease is another common source of sugar-induced tooth pain. As the gums pull away from the teeth, they expose more of the tooth root surface. Unlike the crown of the tooth, the root has no hard enamel protecting it. This leaves the root area unprotected and highly sensitive to any food touching it. Sticky sweets are especially likely to get stuck in areas of gum recession, causing sharp pain. The more the gums recede over time, the worse the root sensitivity can become.
Tooth grinding or clenching
Excessive grinding or clenching of the teeth, especially at night, can cause tiny cracks, chipping, and wear patterns. This damage leaves teeth more vulnerable to sensitivity from temperature extremes and sugar. Hard clenching while eating sticky candies or other sweets can exacerbate symptoms. The constant grinding motion also erodes the enamel over time, removing insulation from the inner tooth layers. Allowed to continue unchecked, grinding and clenching lead to progressive loss of tooth structure, worsening sensitivity issues.
Symptoms of One Tooth Pain with Sweets
Some of the most common symptoms that indicate dental issues like cavities or cracked teeth causing sugar sensitivity include:
- Sharp pain when eating candy, ice cream, baked goods, chocolate, or cough drops
- Sensitivity and discomfort localized to one tooth, not the entire mouth
- Brief, shooting pain when the sugary food first contacts the problematic tooth
- Sensitivity that subsides briefly when the sugar is removed
- Lingering mild ache or throbbing after eating sugary foods
- Pain when chewing or biting down on the sensitive tooth
- Noticing holes, pits, cracks, fractures, or leaky fillings on examination of the tooth
- Extreme sensitivity to hot and cold foods or air on the affected tooth
In more advanced cases, additional symptoms may arise indicating pulp inflammation like:
- Spontaneous toothache not necessarily triggered by food
- Prolonged pain lasting for hours after sugar stimulus removed
- Pain disrupting sleep or causing awakening at night
- Swelling of the gums around the tooth
- Bad taste or odor from the tooth
- Drainage of pus from the gumline
These warrant immediate dental care to treat infection and prevent tooth loss.
Dental Exams to Diagnose the Cause

A dentist can perform a series of diagnostic tests and procedures to pinpoint what exactly is causing sensitivity and pain in the problematic tooth when eating sweets.
Visual oral examination
The dentist will first thoroughly examine the tooth visually, looking for obvious signs of decay like pits and holes in the enamel or brown or white spot lesions. They will also check for cracks, chips, defective old fillings, large fillings or crowns that may be trapping food, and receding gum tissues.
Exploring problematic areas
Using a dental instrument, the dentist will probe any cracks, pits, leaky fillings, and areas of gum recession. This allows them to feel for softness, stickiness, or other signs of decay not visible on the surface.
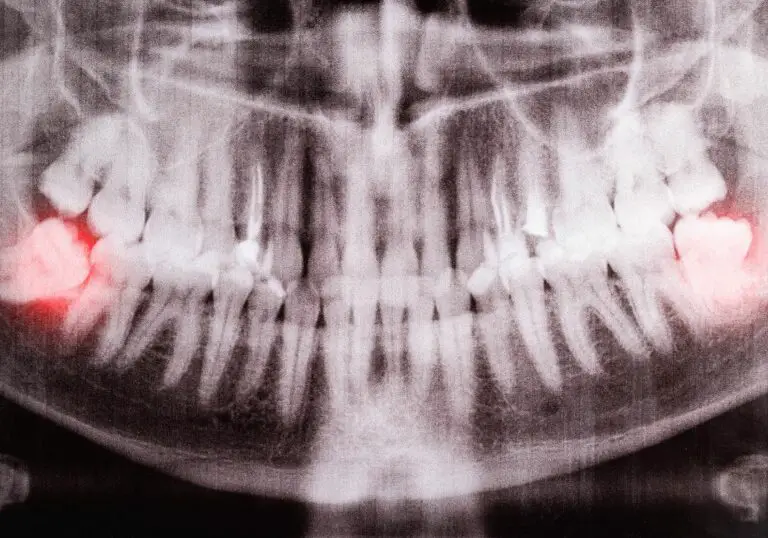
Dental x-rays
X-rays allow the dentist to see below the enamel into the deeper layers of the tooth. X-rays are crucial for finding cavities forming between teeth, infection inside a tooth, and cracks or fractures that cannot be seen on visual exam. They may take bite-wing x-rays focused on back molars or periapical films to get a complete image of an entire tooth and surrounding bone.
Testing reaction to cold
Applying a cold stimulus like a cold air jet onto the suspect tooth isolates and determines how sensitive it is to cold. A strongly positive reaction indicates pulp inflammation and nerve damage.
Percussion testing
Gently tapping the tooth with a dental instrument applies pressure to the tooth. If this causes severe discomfort or pain, it indicates an underlying infection or abscess.
Checking for high spots
The dentist may run dental floss between teeth with fillings or crowns to check for “high spots” where food is getting trapped and causing irritation.
Analyzing gum health
Examining for signs of gingivitis, receding gums, and periodontal pockets that could contribute to root sensitivity.
Saliva testing
Checking saliva flow and pH. Insufficient saliva or high acidity increase risk of cavities.
This comprehensive dental exam pinpoints the origin of sensitivity to guide appropriate treatment.
Professional Treatment Options for Relief

Based on exam findings and diagnosis, the dentist will recommend the best treatment plan to resolve your tooth pain with sweets:
Treating decay
If cavities are present, the decayed portions will be removed and the holes properly filled to cover exposed dentin. For small areas of demineralization, fluoride treatments or specialized toothpaste may be prescribed to remineralize the enamel before it progresses to a cavity.
Replacing old fillings
Any defective fillings with gaps or cracks allowing food and sensitivity need replacement with new, properly contoured fillings that seal out sugar stimuli.
Root canals
For extensive decay or cracks causing inflamed and infected pulp, a root canal will be performed. This removes the diseased pulp, cleans inside the roots, seals and fills the interior of the tooth to stop further infection.
Nightguards and bite adjustment
Nightguards protect against tooth grinding and cracks. Bite adjustment corrects high spots trapping sugar against teeth. Less invasive options before pursuing crowns.
Gum grafting procedures
Grafting can cover exposed sensitive root surfaces by taking gum tissue from elsewhere in the mouth and suturing it into areas of recession.
Tooth extractions
Severely cracked, fractured, or decayed teeth that cannot be restored will be extracted to prevent worsening damage and infection. Implants may replace extracted teeth.
Crowns and veneers
Crowns reinforce and protect badly damaged teeth from further fracture. Veneers cover worn enamel prone to sensitivity.
Following the dentist’s post-treatment instructions for diet, oral hygiene, and use of prescription desensitizing products will aid recovery and help manage sensitivity.
At-Home Remedies to Soothe Sensitivity
There are several simple home remedies you can try as well to help minimize tooth sensitivity as you recover from dental work:
- Use desensitizing toothpaste – Formulas containing potassium nitrate or stannous fluoride help relieve sensitivity
- Rinse with baking soda and water – Soothes inflammation and neutralizes acids
- Avoid acidic and sugary foods/drinks – Prevent irritation until sensitivity subsides
- Take over-the-counter pain relievers before eating if needed
- Try sensodyne, Orajel, or benzocaine gels – Temporarily numb sensitivity
- Wear a nightguard if grinding – Protects teeth from worsening cracks/damage
- Drink plenty of water – Helps neutralize acids and stimulate saliva flow
- Chew sugar-free gum – Increases saliva flow to remineralize and lubricate teeth
- Use a soft brush and brush gently – Prevents abrasion damage to sensitive teeth
- Floss carefully around sensitive areas – Avoid snapping floss onto the gums
- See your dentist for prescription strength toothpaste or medicated gels if OTC products are inadequate
With the appropriate combination of professional dental care and vigilant home care, you can successfully treat the cause of sugar sensitivity and prevent it from recurring.
When to Visit the Dentist

Make an appointment with your dentist promptly if you experience any of the following:
- Frequent or growing discomfort when consuming sugary, cold, or acidic foods
- Sensitivity or pain localized to a particular tooth and not improving
-Visible pits, stains, cracks, fractures, or holes in a tooth
- Extreme hot/cold sensitivity on one tooth
- Chipping or wearing of the tooth enamel
-Pain when biting or chewing
- Bleeding, redness, swelling, or receding gums
- Constant bad breath or pus around the affected tooth
- Tooth pain that disrupts sleep or daily functions
- Symptoms that over-the-counter remedies can’t resolve
Letting sugar-induced dental pain go unchecked allows decay, cracks, and infections to progress. The dentist can properly diagnose and treat the underlying problem for lasting relief, whether it is cavities, cracked teeth, defective fillings, gum disease, or other issues. Don’t delay seeking help for a painful problem tooth.
When is Emergency Dental Care Needed?
Seek emergency dental treatment immediately if you experience:
- Severe, spontaneous toothache not subsiding
- Prolonged, intense pain for hours after eating sweets
- Tooth pain radiating to your jaw, ear, or head
- Tooth trauma from a hit or fall causing fracture or dislocation
- Swelling in the gums or face around the painful tooth
- Bleeding or pus discharge from the gums
- A severely cracked or loose tooth
- Difficulty breathing or swallowing
These severe symptoms indicate pulp infection and abscess development requiring urgent dental intervention to preserve the tooth and prevent dangerous spread of infection. Prompt specialist emergency care can save an infected tooth.
Questions and Answers about Sweet Sensitivity
Q: Why would only one tooth hurt and not all of them when I eat candy or ice cream?
A: Factors like tooth decay, cracks, gum recession, and dental work tend to impact individual teeth differently at various spots in the mouth. So sensitivity is usually confined to just problematic teeth with underlying issues, rather than all teeth.
Q: My tooth hurts briefly when I eat sugar but then feels fine afterward. Should I be concerned?
A: Yes, any sensitivity or pain when eating hot, cold, or sugary foods warrants an exam. It likely indicates a cavity or crack reaching the inner layers of your tooth. Seeking prompt treatment prevents worsening damage.
Q: Can I stop the pain by avoiding sugary foods without seeing a dentist?
A: Eliminating sweets prevents annoying the sensitive tooth temporarily but won’t resolve the underlying problem. Without treatment of the cause, whether it’s decay, cracked enamel, or receding gums, the pain will inevitably recur and intensify over time.
Q: If I have a crown placed on the painful tooth, will that stop the sensitivity permanently?
Crowns reinforce and protect damaged teeth. But if they are not sized and contoured precisely, sugars can still seep beneath and cause pain. Well-fitted crowns should prevent sensitivity if the inner tooth and roots are healthy. But other pre-existing issues like gum disease can still cause discomfort.
Q: My tooth hurts briefly when chewing sugar but it doesn’t bother me otherwise. Do I still need a root canal?
Not necessarily. Slight irritation upon eating sugar may indicate a minor crack or small area of decay rather than extensive nerve damage requiring a root canal. But your dentist should evaluate the tooth thoroughly to determine if you need root canal treatment or a simpler filling.
Conclusion
In summary, pain localized to one tooth when consuming sugary or cold foods usually indicates underlying decay, fracture, gum recession, or dental work causing sensitivity. It should never be ignored, as the problem will only worsen without professional treatment. See your dentist promptly for an exam and diagnosis. With appropriate treatment like fillings, crowns, grafting, root canals, nightguards, extractions or other solutions, you can restore health and functioning to the tooth, allowing you to eat sweets comfortably again. Don’t live with annoying sugar-induced dental pain. A smile should be sweet, not painful!