Plaque is a sticky, colorless film of bacteria that constantly forms on teeth. When plaque accumulates and hardens into tartar, it can lead to tooth decay and periodontal (gum) disease. Surprisingly, research over the past couple decades has discovered that poor oral health and gum disease are closely tied to heart disease. So can the actual plaque accumulation on your teeth directly impact your cardiovascular health? Let’s closely examine the connection.
How are oral health and heart disease connected?
Several theories exist about how poor dental health may contribute to heart disease:
Inflammation
Gum disease causes inflammation not just in the mouth but throughout the body. When gums are irritated and bleed, they release pro-inflammatory chemicals called cytokines. These circulate through the bloodstream. The inflammation they cause may promote damage to blood vessels in a couple key ways:
- Inflamed blood vessels allow low-density lipoprotein (LDL or “bad” cholesterol) to accumulate and become oxidized along artery walls. This buildup of plaque is called atherosclerosis. It narrows the arteries, reducing blood flow. This increases risk of heart attack and stroke.
- Inflamed, damaged arteries are more prone to developing blood clots. When a clot blocks a coronary artery, it cuts off blood supply to the heart muscle leading to heart attack.
Bacterial Spread
Harmful oral bacteria commonly found in gum disease like Porphyromonas gingivalis and Streptococcus sanguinis can enter the bloodstream through irritated, bleeding gums. Research shows the presence of these periodontal pathogens within atherosclerotic plaque.
- Once inside arteries, bacteria accelerate inflammation and worsen damage. They may multiply and release toxins that further destroy tissues.
- Bacteria are also thought to destabilize plaque, causing rupture that leads to heart attack. They trigger increased clotting.
- Bacteria that escape plaques and enter the bloodstream can sometimes lead to infection and inflammation in the heart’s inner lining (endocarditis). This damages heart valves.
Immune system interaction
Chronic inflammation in the gums leads to overactivation of immune cells called monocytes. Elevated monocyte levels are associated with atherosclerosis.
- Hyperinflammatory monocytes swarm into blood vessel walls, get stuck, and exacerbate inflammation and plaque buildup.
- Gum disease bacteria foster increased platelet clumping and aggregation. This enhances unwanted clotting that underlies heart attack and stroke.
Key statistics on the oral-systemic link
Numerous studies have uncovered connections between gum disease and increased cardiovascular disease risk:
- Adults with periodontal disease have a 1.5 to 2 times greater risk of developing heart disease compared to those with healthy gums.
- Having periodontal disease increases your risk of stroke by over 2.8 times.
- For every 10% increase in tooth loss, there is an associated 12-40% higher risk of heart disease. The more missing teeth, the greater the risk.
- Successfully treating severe gum disease can result in a 24-52% average reduction in serum CRP levels, an inflammatory marker implicated in heart disease.
How exactly can plaque lead to cardiovascular issues?
Plaque sitting on the surface of teeth doesn’t directly cause heart attacks or stroke. However, the inflammatory cascade and bacteria associated with plaque buildup are suspected to play an important role in cardiovascular disease development. Here are some of the ways plaque may be involved:
Entry point for bacteria
Plaque formation creates an ideal environment for harmful oral bacteria to thrive. As plaque accumulates, especially below the gumline where oxygen is low, it allows periodontal bacteria greater access to the underlying tissues.
- Bacteria can enter the bloodstream more readily through tears or pockets in inflamed, bleeding gums. They can then circulate to the heart and arteries.
Chronic inflammation
Plaque sustains irritation and inflammation in the gums. This promotes the release of cytokines into the blood that cause systemic inflammation.
- Inflamed gums act as reservoirs that constantly leak inflammatory chemicals like IL-6, TNF-a, and CRP into circulation.
- These chemicals spark immune responses that damage and weaken arteries, laying the groundwork for atherosclerosis.
Immune cell disruption
Bacterial toxins from plaque penetrate gum tissues and alter monocyte function. This causes them to become hyperinflammatory and migrate out into the bloodstream.
- Monocytes swarm into blood vessel walls, accelerating the formation of harmful arterial plaque.
- Platelets also become stickier in response to plaque bacteria toxins, increasing risk of blood clots.
How are cavities and gum disease linked to cardiovascular issues?
Cavities and periodontal disease are the two main dental conditions associated with heart problems. Here is an overview:
| Type of Oral Health Issue | Effects | Heart Disease Risks |
|---|---|---|
| Cavities | – Allow bacteria to enter bloodstream from decayed teeth – Cause pulpal inflammation inside teeth | – Atherosclerosis – Increased risk of ischemic stroke |
| Gum Disease | – Bleeding gums leak bacteria into bloodstream – Chronic inflammation releases cytokines | – 50% higher risk of CVD – 2-3X greater chance of heart attack – Increased atherosclerosis and arterialThickness |
Key takeaway: The inflammation and bacteria from diseased gums and cavities seem to play an important role in damaging arteries and increasing clotting. Treating oral health issues may substantially lower cardiovascular risks.
Additional risk factors connecting mouth and heart health
Below are some other factors that may help explain the close association between poor dental health and cardiovascular disease:
- Medical conditions – Diabetes and heart disease reduce blood flow and wound healing. This promotes gum inflammation and bacterial growth. Gum disease is worse in those with these conditions.
- Medications – Drugs for heart disease like diuretics, calcium channel blockers, and beta blockers reduce saliva flow. Dry mouth increases cavity risk.
- Lifestyle – Unhealthy diet, smoking, and chronic stress negatively impact both gum and heart health. They are risk factors common to periodontal disease and cardiovascular disease.
- Age – With older age, dental health often declines while cardiovascular disease typically becomes more common.
- Inflammation – Systemic inflammation from any source, including gum disease, joint issues, and obesity, impacts the entire cardiovascular system.
Can treating dental plaque and gum disease help your heart?
Given the close association between oral bacteria and inflammation with atherosclerosis and heart attack risk, treating dental disease could provide cardiovascular benefits. Here is some of the evidence:
-
Successfully treating periodontal disease:
- Slowed atherosclerosis progression by 5-12% in coronary arteries
- Reduced key inflammation markers CRP and IL-6 by 24-52%
- Lowered risk of heart attack and stroke by 20-30%
-
Getting regular dental cleanings:
- Reduced risk of heart attack by 23-61% in various studies
- Helped maintain lower CRP in those at risk for stroke and heart attack
-
When people with heart valve abnormalities or prior heart infection undergo tooth extraction, it reduces systemic inflammation.
While more research is underway, current evidence suggests maintaining good oral hygiene and treating dental disease may benefit the heart in those at risk for cardiovascular issues.
5 ways to reduce plaque buildup and support a healthy heart
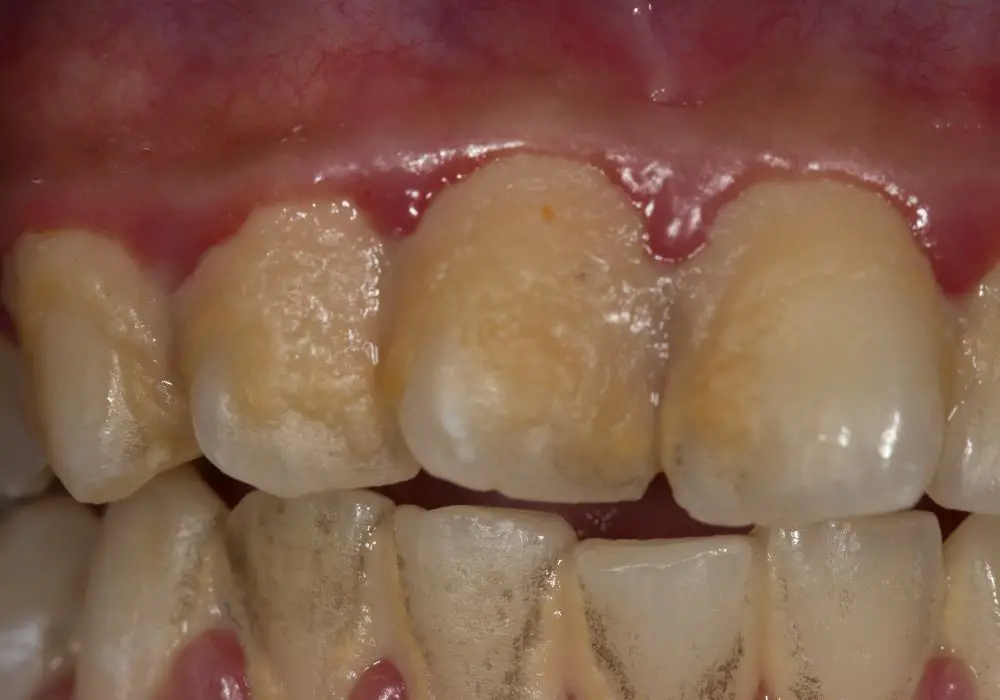
Here are five proven strategies to lower oral plaque accumulation and bacteria to help reduce cardiovascular risks long-term:
1. Brush thoroughly twice daily
Brush at least twice per day for 2 minutes to physically remove plaque from tooth surfaces. Ensure you reach all areas. Use proper technique. Electric toothbrushes may improve plaque removal.
2. Floss once daily
Gently floss between teeth to clear plaque and debris from areas your toothbrush misses. This helps prevent gum inflammation and pockets.
3. Use antimicrobial mouthwash
Rinsing daily with mouthwash containing chlorhexidine, essential oils, or cetylpyridinium chloride reduces overall oral bacteria and plaque that cause gingivitis.
4. Get professional cleanings
See your dentist for cleanings every 6 months. They will remove hardened calculus above and below the gumline and spot signs of oral disease early.
5. Limit sugary foods and drinks
A sugary diet promotes plaque bacteria growth and tooth decay. Restrict sugary foods and rinse mouth with water after eating sweets to neutralize acids.
Making oral hygiene and regular dental care a priority can effectively minimize plaque and harmful mouth bacteria that contribute to cardiovascular inflammation and damage according to research. A healthy mouth supports a healthy heart.
Frequently Asked Questions
1. What is dental plaque made of?
Dental plaque is a biofilm composed mainly of bacteria that adheres to the tooth surface. It also contains salivary proteins, bacterial byproducts like proteins and polysaccharides, food debris, and live and dead immune cells. There can be hundreds of bacterial species.
2. Which is generally worse for cardiovascular health – cavities or gum disease?
Studies show gum disease poses a greater cardiovascular risk than cavities. The inflammation and bacteria from bleeding, inflamed gums seem to have more systemic impact. However, cavities also allow oral bacteria to enter blood so poor dental health overall negatively affects the heart.
3. Can plaque suddenly break free from teeth and directly cause a heart attack?
It would be extremely rare for a piece of plaque to detach from a tooth and travel directly into the heart to cause a heart attack. However, plaque does harbor inflammation-causing bacteria that enter the bloodstream over time. This contributes to factors that can eventually trigger heart attack like atherosclerosis and clots.
4. If I get a dental cleaning, will my heart disease risk immediately drop?
Getting a single dental cleaning itself won’t instantly decrease heart disease risk. However, getting consistent, thorough professional cleanings every 6 months can help keep bacteria and inflammation levels lower long-term. This chronic reduction in oral inflammation may gradually reduce factors that contribute to cardiovascular disease over years.
5. Is coronary artery disease the only type of heart condition linked to poor dental health?
Poor oral hygiene has been tied to increased risk of many cardiovascular conditions beyond just coronary heart disease. Research shows associations with stroke, heart attack, aortic atherosclerosis, congestive heart failure, and even infection of the heart (endocarditis). Keeping the mouth free of plaque and dental disease supports total cardiovascular wellness.