Having a gritty feeling between your teeth when you floss can be unpleasant and concerning. But in most cases, it is not a serious dental issue and can be resolved with improved flossing habits. Understanding the common causes of gritty flossing sensations can help you achieve cleaner, healthier teeth and gums.
What Factors Lead to Grit Between Teeth During Flossing?
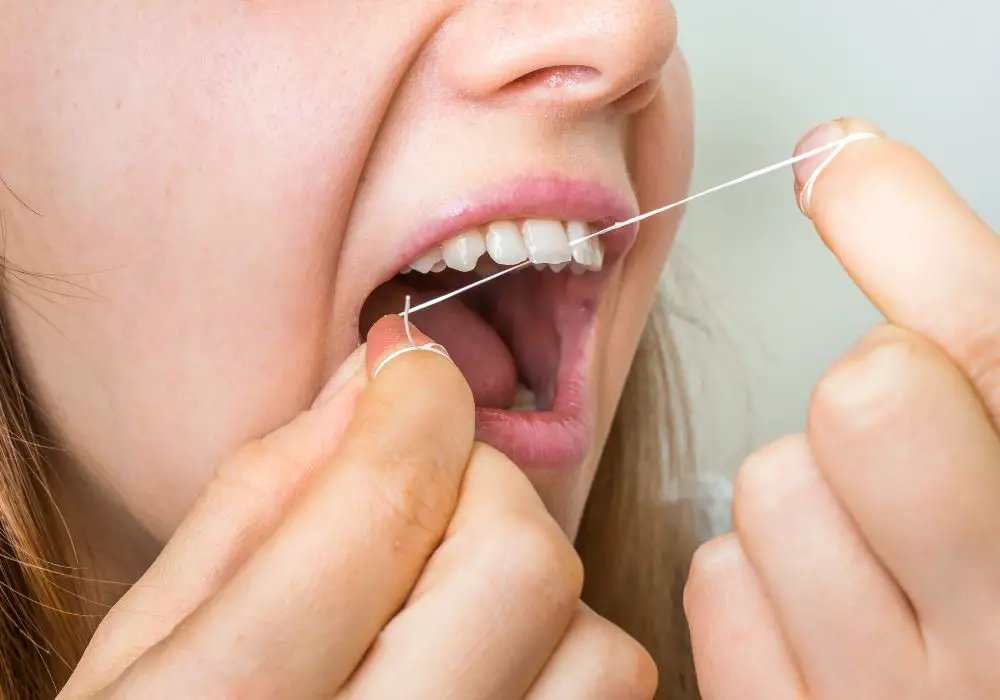
There are several potential explanations for experiencing a gritty texture when you floss your teeth:
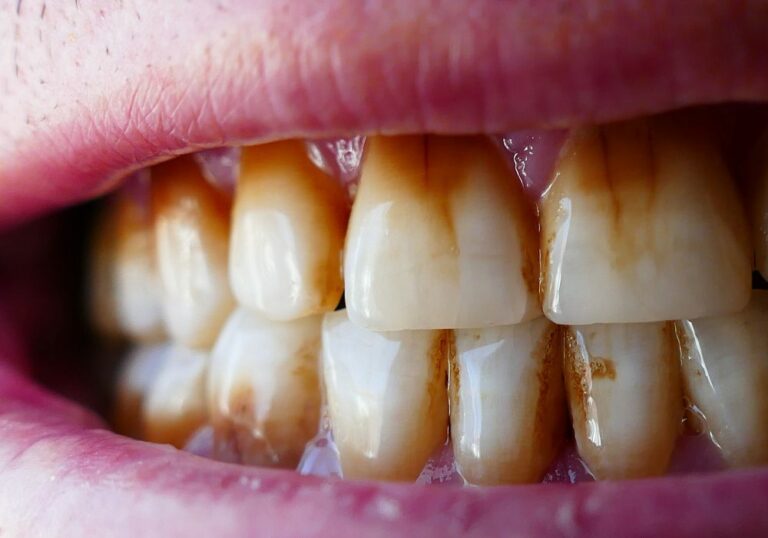
Accumulation of Plaque and Tartar
Plaque is a sticky film of bacteria that constantly forms on tooth surfaces. When left undisturbed, plaque hardens into tartar or calculus. Both plaque and tartar can irritate gums and cause a gritty feeling during flossing. The texture comes from the rough surface of the calcified plaque and tartar deposits.
Tartar is more likely to accumulate in areas that are difficult to keep clean:
- Along the gum line
- In crevices between teeth
- Around fillings or dental appliances
- Near salivary gland duct openings
- Below the gum line, where brushing and flossing can’t reach
To prevent gritty buildup, it is essential to floss thoroughly once per day. This removes plaque from between teeth before it turns into tartar. However, only a professional dental cleaning can fully remove tartar below the gums.
Trapped Food Particles and Debris
It’s common for pieces of food to become lodged tightly between teeth, especially in the back molars. Foods prone to getting stuck include:
- Popcorn kernels
- Seeds (sesame, poppy, etc.)
- Granola
- Rice
- Meat fibers
- Corn
- Nuts
- Candy
- Chewing gum
The food particles create friction against the floss, giving a gritty feeling as they become dislodged. Saliva and beverages don’t adequately rinse out these stuck bits. Regular flossing is required to clear the debris.
Erosion and Damage to Tooth Enamel
Enamel is the hard, mineralized surface layer that protects each tooth. When enamel erodes from disease or excessive acid exposure, it becomes more porous and rough in texture. Loss of smooth, sound enamel can give teeth a noticeable gritty or sandy feeling.
Enamel erosion can result from:
- Frequent consumption of acidic foods and drinks – citrus, tomatoes, soda, juice, wine, etc. The acids dissolve the mineral content of enamel.
- Stomach acid from gastroesophageal reflux disease (GERD) or bulimia. Acid reflux brings stomach contents back up into the mouth.
- Teeth grinding (bruxism), which wears down enamel.
- Overly-aggressive brushing, especially with a hard bristle toothbrush. This abrades the enamel.
- Inadequate fluoride, which strengthens enamel crystalline structure.
- Genetic predisposition to weaker enamel.
Damaged enamel is also more prone to developing cavities, requiring prompt dental treatment.
Receding Gums and Exposed Tooth Roots
Gingivitis, the early stage of gum disease, causes inflammation and receding gums due to plaque buildup. As gums recede down the tooth, it exposes more of the tooth root surface. Unlike enamel, the cementum covering roots has a naturally coarse, ridged texture. Flossing across this gritty exposed root surface can create uncomfortable friction.
In addition to flossing, proper brushing and professional cleanings are needed to treat gingivitis before it progresses to advanced periodontal disease. Your dentist can help regrow healthy gums to cover more of the root.
Xerostomia (Dry Mouth)
Adequate saliva flow is vital for flushing away food debris, neutralizing mouth acids, and keeping tissues lubricated. Saliva deficiency from dry mouth allows plaque bacteria to thrive. It becomes easier for tartar, food, and bacteria to accumulate in a dry oral environment. The resulting buildup feels gritty when scraped by floss.
Causes of dry mouth include:
- Many prescription and OTC medications – antihistamines, diuretics, antidepressants, pain meds
- Damage or surgery to salivary glands
- Diseases like diabetes, Parkinson’s, Alzheimer’s
- Radiation cancer treatment
- Autoimmune disorders (Sjogren’s syndrome)
- Habitual mouth breathing during sleep
- Anxiety or depression
- Tobacco use
Managing dry mouth requires addressing the underlying cause and increasing hydration. Your dentist or doctor can recommend appropriate saliva substitutes and oral hygiene aids.
When Should I Make a Dental Appointment About Gritty Flossing?
Occasional mild grit between teeth generally isn’t worrisome on its own. But schedule a prompt dentist visit if you notice:
- Frequent or severe gritty, rough sensation that keeps recurring
- Bleeding or painful gums during flossing
- Halitosis – persistent bad breath
- Visible plaque, tartar, or gum recession
- Tooth sensitivity, decay, or erosion
- Unexplained dry mouth symptoms
Your dentist can assess the cause and recommend targeted treatments to restore gum health and enamel strength. Leaving gritty flossing problems unchecked allows them to worsen over time. Early intervention is key to preventing extensive tooth decay or advanced periodontal disease.
How to Reduce Grit Between Teeth and Gums
Practicing excellent oral hygiene is the first line of defense against that unpleasant gritty flossing sensation. But tackling more severe cases requires professional help. Here are some tips to minimize grit and promote dental health:
Floss Thoroughly Once Daily
- Insert floss fully between teeth, curving it around each tooth’s base near the gums. Floss up-down several times.
- Don’t just floss front teeth. Reach way back to the molars, using floss threaders if needed.
- Use waxed floss, which glides between tight teeth easier than unwaxed varieties.
- Try flosses with texture (fuzzy, ribbed) to grip and remove plaque.
- Rinse mouth with water after flossing to wash away dislodged particles.
Regular flossing clears out plaque and debris before they calcify into rough tartar. It keeps your gums healthy and helps prevent food from packing tightly between teeth.
Brush Properly Twice Daily
While flossing focuses on tooth surfaces between teeth, brushing targets outer surfaces:
- Use a soft-bristled toothbrush with a pea-sized amount of fluoride toothpaste.
- Brush for 2 full minutes, gently massaging all surfaces of teeth and gums.
- Take extra time on the back molars and along the gum line where gritty buildup occurs.
- Avoid abrasive brushing motions that could damage enamel.
- Replace toothbrush every 3-4 months when bristles appear frayed.
Rinse with Antimicrobial Mouthwash
Swishing daily with mouthwash reaches areas that brushing and flossing may miss. The germ-killing ingredients help control bacteria that form plaque and tartar. Use mouthwash as the final step after brushing and flossing.
Drink Plenty of Water
Staying hydrated is key for producing cleansing saliva. Shoot for 8 glasses of water per day. Avoid dry mouth-provoking beverages like alcohol, caffeine, soda, and fruit juice.
Limit Acidic Foods and Sugars
Frequent exposure to acids damages enamel, while sugar feeds plaque bacteria. Reduce consumption of citrus fruits, juices, tomatoes, wine, soda, and candy. Rinse with water after eating to dilute acids.
Get Professional Cleanings
Only a dental hygienist can fully remove plaque, tartar, and stains from all tooth surfaces and below the gum line. Get a cleaning and exam every 6 months to prevent major gritty buildup.
See Your Dentist
If you still battle grit long after improving your oral hygiene routine, consult a dentist. They can identify any underlying problems and suggest treatments such as fluoride applications, antibacterial rinses, gum grafting, or enamel restoration.
With diligent home care and regular professional cleanings, your teeth should feel smooth and slick when flossing. Don’t ignore frequent gritty sensations that could signal issues needing more intervention. Let your dentist help you achieve and maintain the cleanest mouth possible.
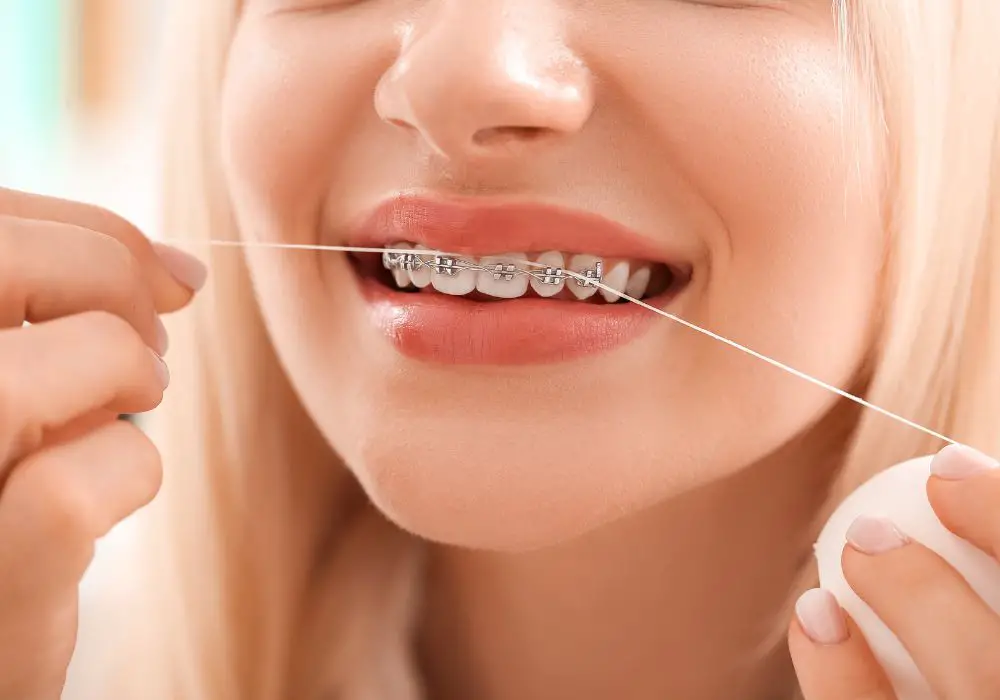
Frequently Asked Questions About Gritty Teeth and Flossing
Here are answers to some common patient questions about dealing with roughness and grit when flossing:
What’s the best floss to use for gritty teeth?
Flosses with texture work best to grab and dislodge gritty plaque buildup. Options include waxed floss for easy glide, or textured flosses with ridges or fuzzy surfaces. Dental tape can slip more easily between tight teeth.
How can I tell if grit is from tartar versus damaged enamel?
Carefully look at the floss after removal – tartar scrapes off as white material on the floss. If the floss itself seems frayed or ground down, that indicates roughened enamel. Prod your gums to check for receded areas or sensitive spots.
Is it possible to remove tartar buildup myself?
Maybe minor surface tartar, but calcified layers below gum level require professional scaling tools. Attempting to scrape off tartar risks damaging enamel or roots. Leave extensive buildup removal to your dental hygienist.
What foods help strengthen enamel to prevent erosion?
Foods high in calcium (milk, yogurt, cheese), phosphorous (meat, eggs, fish), and fluoride (tea, seafood) help reinforce enamel. Crunchy fruits and veggies also stimulate saliva to remineralize enamel.
How can I tell if a medication is causing my dry mouth and gritty teeth?
Tell your dentist about all medications you take, both prescription and over-the-counter. They can determine which may reduce saliva flow as a side effect. Your doctor or pharmacist can then suggest lower-risk alternatives.
Don’t brush off gritty, rough sensations when flossing. Work to identify the source of the problem through improved oral hygiene and dental visits. Addressing grit early prevents more extensive dental disease and treatment later on.