What is tooth enamel and why is it important?
Tooth enamel is the hard, outer layer of the tooth crowns. It is the most mineralized substance in the human body, containing mostly hydroxyapatite crystals.
Enamel serves several crucial functions:
- Protects the inner dentin layer from decay and damage. Enamel is the hardest tissue in the body and able to endure biting forces up to 200 lbs per square inch. It prevents bacteria, acids, and trauma from reaching the sensitive dentin layer underneath.
- Provides a smooth, hard surface for chewing food. The crystalline structure of enamel creates a durable, wear-resistant surface that stands up to the friction of chewing and grinding food. This allows teeth to efficiently break down food particles during digestion.
- Helps maintain tooth shape and structure. Enamel forms the visible anatomical crown of each tooth. Its thickness and contours help give teeth their characteristic shapes. Losing enamel can change tooth morphology and affect occlusion (bite).
Enamel is naturally translucent and varies in thickness, from 2.5 to 3 mm on incisors and canines to up to 2 mm on molars. It is thickest at the biting surface and angles of teeth, making these areas most resistant to wear.
Once damaged, enamel cannot regenerate on its own because it contains no living cells. Enamel formation happens in early childhood as specialized ameloblast cells lay down the hydroxyapatite mineral matrix. When the enamel layer is complete, the ameloblasts are lost. This means mature enamel is incapable of self-repair when injured or eroded away.
Keeping enamel intact is crucial for oral health and preventing cavities, enamel erosion, and hypersensitivity. Enamel loss can also affect the aesthetics and structural integrity of teeth. That’s why restoring damaged enamel is an important topic in dentistry.
What causes enamel loss?
Enamel can wear away or erode from various factors during life:
1. Enamel Erosion
Enamel erosion is the chemical dissolution of enamel surfaces due to acid exposure. Common sources of acids that erode enamel include:
- Acidic foods and drinks – citrus fruits, carbonated soft drinks, wine, fruit juices
- Gastric acid from vomiting, gastroesophageal reflux disease (GERD), or bulimia
- Irregular saliva flow – reduced saliva causes inadequate buffering and clearing of acids
In early enamel erosion, the acids first cause subsurface demineralization, creating microscopic pores beneath the intact enamel surface. As erosion progresses, the surface enamel Starts to dissolve, becoming thinner, rougher, and more transparent. Advanced erosion leads to exposure of the underlying dentin as enamel completely disappears.
2. Mechanical Enamel Loss
Physical forces can also abrade and chip away enamel over time:
- Attrition – wearing between opposing teeth, often seen in bruxism (grinding) or with an irregular bite/malocclusion.
- Abrasion – friction from foreign objects like aggressive toothbrush bristles, improper flossing, or habitual chewing on hard objects.
- Abfraction – flexing forces concentrated at the cervical (neck) region of teeth, often seen with heavy biting forces. Can cause V-shaped notches in the enamel.
This mechanical wear causes enamel to gradually thin and chip from its outer surface, especially on the incisal and occlusal edges.
3. Other Causes
- Tooth decay – acid from plaque bacteria that penetrates through the enamel rods and destroys the inner enamel layers.
- Developmental conditions – enamel hypomineralization or hypoplasia that causes inherent structural defects.
These factors degrade the crystalline structure of enamel through a combination of dissolution, chipping, and fracture. This leads to permanent loss of the enamel tissue over time rather than just mineral loss.
Signs that enamel is damaged

How do you know if your enamel is thinning or eroding? Here are some common signs:
- Increased tooth sensitivity – especially to hot, cold, or sweet foods as dentin is exposed.
- Yellowish discoloration as thinner enamel allows dentin color to show through.
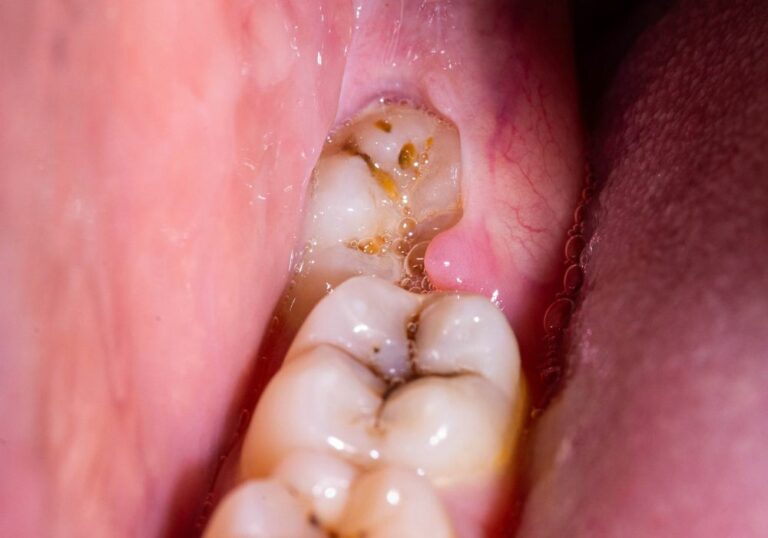
- Chipped or ragged edges on teeth from loss of enamel volume.
- Transparent or discolored spots where enamel has eroded away.
- Exposed dentin appearing as a yellowish layer under thinning enamel.
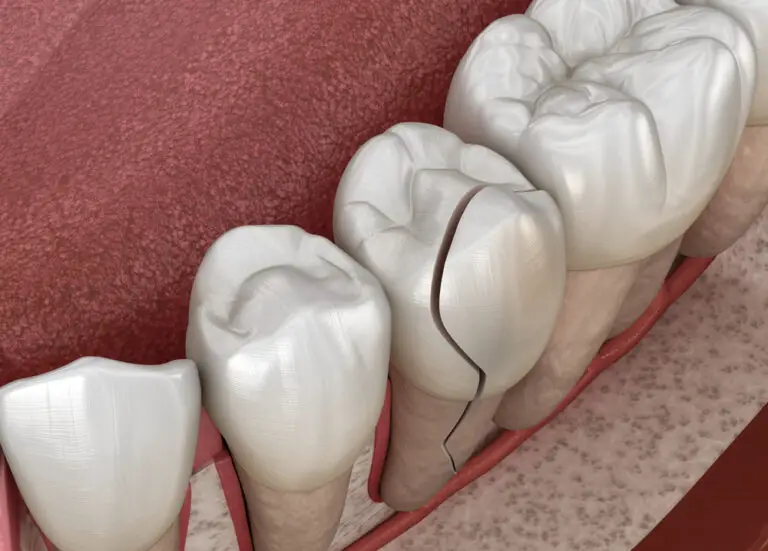
- Visible cracks or fractures extending through the enamel surface.
- Cupping, grooving, or concavities on teeth from abrasion or abfraction.
- Toothdecay and cavities forming more readily as protective enamel is lost.
- Change in tooth shape, flattened cusps, pointed incisal edges.
Pay attention if you notice any of these symptoms – they signify enamel issues. See your dentist promptly for an exam. They will check for areas of decay and damage using magnification, transillumination, and dental radiographs. Early intervention is key to prevent more severe enamel loss.
Can you reverse enamel loss and build it back up?
Unlike other tissues in the body, enamel cannot regenerate or regrow on its own once it is lost. The cells that form enamel, called ameloblasts, are lost after the teeth erupt fully into the mouth. Enamel itself is acellular and contains no living components.
However, there are ways to restore or rebuild enamel through dental procedures. The main approaches are:
1. Remineralization
Remineralization aims to repair early enamel damage before any noticeable loss occurs. It deposits minerals like calcium and phosphate ions back into areas of demineralized enamel to “fill in” microscopic pores and surface defects.
Fluoride is a key remineralizing agent and stabilizes enamel crystals against acid attacks. Products containing fluoride (toothpastes, rinses, gels) or calcium phosphates can promote remineralization if the enamel damage is minor. Your dentist may also prescribe higher concentration fluoride varnishes for home use.
However, remineralization has limitations:
- It cannot rebuild enamel where significant tissue loss has already occurred. Once the crystals are completely dissolved away, theminerals have no framework to attach to.
- The remineralized enamel is not as mechanically strong as original enamel. The repaired hydroxyapatite crystals are smaller and arranged in a more disorganized structure.
- Deeper lesions and cavitated areas will not remineralize effectively. Bacteria and plaque acids will continue degrading the enamel from underneath.
For milder cases, remineralization can help arrest early caries and strengthen enamel against erosion. But where cavities have penetrated deep into enamel, direct restorations are needed to structurally replace lost tissue.
2. Direct Restorations
Direct restorations involve placing tooth-colored filling materials into areas where enamel has eroded or decayed away:
- Composite resin fillings – Bonded directly into the tooth cavity and sculpted to match natural enamel. Requires less removal of healthy enamel compared to traditional amalgam fillings. Excellent aesthetic results.
- Dental inlays/onlays – Indirect restorations custom-fabricated from porcelain or composite resins and cemented into place. Less tooth reduction than crowns and provide excellent function for larger cavities.
- Dental crowns – Encircle the entire visible portion of the tooth. Necessary for more extensive decay involving multiple tooth surfaces, as an abutment for dental bridges, or to reinforce weakened teeth.
These materials mechanically lock into the remaining enamel and dentin, rebuilding lost structural integrity. With good oral hygiene and no untreated decay, direct restorations can last 5-15 years before replacement is needed.
3. Enamel Microabrasion
Microabrasion is a conservative technique that removes a microscopic layer of outer enamel. It is done with an abrasive compound under controlled conditions.
This can improve enamel appearance by:
- Removing superficial intrinsic stains that cannot be removed by bleaching alone.
- Smoothing away surface irregularities, defects, or shallow discolorations in intact enamel.
Microabrasion only modifies the outer 10-100 microns of enamel so is only suitable if enamel is largely undamaged. It does not rebuild or regenerate lost enamel thickness.
4. Dental Bonding
Bonding improves aesthetic concerns by applying tooth-colored composite resin material directly onto the intact enamel surface. It can:
- Repair small chips or gaps in enamel
- Change subtle aspects of tooth shape/proportionality
- Cover intrinsic stains in the enamel layer
- Close small diastemas (gaps between teeth)
Like microabrasion, bonding only modifies the enamel surface. It does not regenerate lost enamel volume where cavities or erosion has occurred. The composite resins are not as durable as natural enamel.
Are there any new treatments to regrow enamel?

Regenerating true enamel after substantial loss requires reforming the entire organic matrix and hydroxyapatite crystal structure. Researchers are exploring methods to recreate enamel tissue:
- Amelogenins – Enamel proteins that control crystal shape and organization during embryonic development. Studies show amelogenin proteins applied to enamel defects can guide remineralization and improve enamel thickness.
- Stem cell regeneration – Stem cells from dental pulp, gingival tissue, urine, and other sources are studied for their ability to differentiate into ameloblast-like cells that deposit enamel. This approach is still in the experimental stage.
- Biomimetics – Synthetic enamel substitutes aim to mimic the intricate microstructure of natural enamel. These materials could potentially be applied to rebuild enamel but are not yet clinically viable.
- Fluoride – Highly concentrated fluoride varnishes containing calcium phosphate salts or polyphosphates are designed to encourage deeper remineralization and stimulate arrested enamel crystals to grow.
However, true biological enamel regeneration is not yet possible. These cutting-edge treatments are still in early research stages and face challenges like unpredictable crystal growth and poor mechanical strength. But they offer hope for enamel self-repair in the future.
What is the best way to restore eroded enamel?
The ideal treatment plan depends on factors like:
- Amount of enamel already lost
- Condition of remaining tooth structure
- Location and extent of enamel deficiency
- Aesthetic and functional considerations
Milder cases of surface wear or small defects may be treated with remineralization therapies or conservative techniques like microabrasion or bonding.
More significant enamel loss, typically involving dentin exposure, requires direct restorations:
- Shallow cavities – resin composite fillings
- Extensive decay – indirect inlays/onlays or crowns
Porcelain or ceramic restorations offer excellent aesthetics and durability. But whenever possible, saving natural enamel through remineralization is preferred.
For severely damaged teeth, full coverage crowns may be the only option. But removing substantial tooth structure further weakens the remaining enamel. The decision depends on individual factors assessed during a dental exam.
Ongoing preventive care combined with early restorative intervention provides the best outcome. Regular exams help detect enamel issues when damage is still minimal and reversible.
How can you prevent enamel loss in the future?

Alongside professional treatment, daily home care is vital to defend and strengthen enamel. Prevention strategies include:
1. Gentle, effective oral hygiene
- Use a soft-bristled toothbrush and avoid abrasive brushing motions.
- Choose non-abrasive toothpaste – those for sensitive teeth are ideal.
- Take care flossing near restorations or worn enamel.
2. Diet modifications
- Limit acidic foods and carbonated or sugary drinks.
- Avoid excessive citrus, juice, wine, soda. Drink water to help neutralize acids.
- Rinse with water after reflux episodes.
3. Stimulate saliva flow
- Chew xylitol gum to increase saliva flow after meals.
- Use saliva substitutes if dry mouth is an issue.
4. Fluoride application
- Use fluoride toothpaste twice daily.
- See your dentist for prescription strength fluoride gels or varnishes.
- Consider daily fluoride rinses.
5. Dental check-ups
- Get exams every 6 months to check for demineralization or decay under the enamel.
- Early detection means using less invasive treatments to restore enamel.
6. Address bruxism/grinding
- Ask your dentist about a night guard if you grind your teeth.
- Relaxation techniques and stress reduction may help curb grinding habits.
Protecting your natural enamel from further damage is the top priority. Follow-up with your dentist regularly so they can monitor areas of concern. Saving enamel now prevents more complex restorations later.
Frequently Asked Questions
Can enamel grow back naturally once lost?
No, enamel cannot regenerate on its own after it is lost because it contains no living cells. Only the intact outermost layer can remineralize and repair early subsurface damage. True enamel regeneration requires extensive cellular growth and mineralization, which current treatments cannot yet achieve reliably.
Do whitening toothpastes help restore enamel?
Toothpastes marketed as “enamel-restoring” or “enamel-repairing” contain ingredients for extrinsic stain removal and remineralization. While helpful, they cannot rebuild enamel lost to erosion, decay, or fracture. At best, special abrasives may lightly bleach superficial stains. Typically, the mineral content is insufficient to replace enamel minerals leached away by disease. Restorative dental work is still needed in areas of significant enamel loss.
Can chipped enamel fully heal and regenerate?
No, a fractured piece of enamel will not grow back together unless it is a microscopic crack. Enamel cannot mend large chips or fractures on its own. Fragments can sometimes be bonded back into place by a dentist, but the joint will remain weaker than original enamel. Larger chips often need dental fillings or crowns to structurally rebuild the missing volume. Remineralization helps strengthen the edges but cannot regenerate the lost enamel portion.
How long do enamel restorations last?
With good oral hygiene and regular dental care, direct resin restorations can last 5-15 years before replacement is needed. Well-made indirect restorations like ceramic onlays may last 15-30 years. Factors affecting longevity include material quality, patient biting forces and occlusal wear, ongoing decay risk, and diligent home care. Regular exams help dentists detect failing restorations early for repair or replacement while still manageable.
What fluoride treatment works best for remineralizing enamel?
In-office professional applications of higher concentration fluoride gels or varnishes provide the most potent remineralizing effects. Prescription home care fluoride gels are also available. For daily use, over-the-counter toothpastes with stannous fluoride or prescription-strength sodium fluoride (5000 ppm) work better than standard fluoride pastes. Fluoride mouthwashes likewise aid remineralization. Your dentist can recommend products suited to your individual enamel needs.