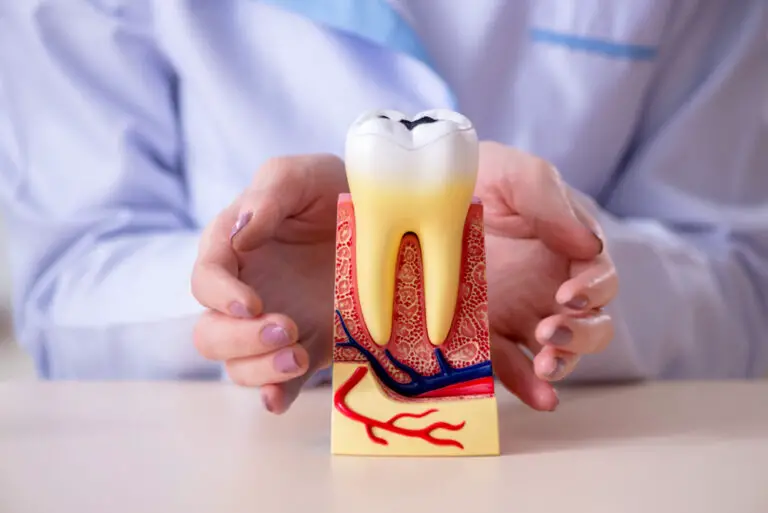
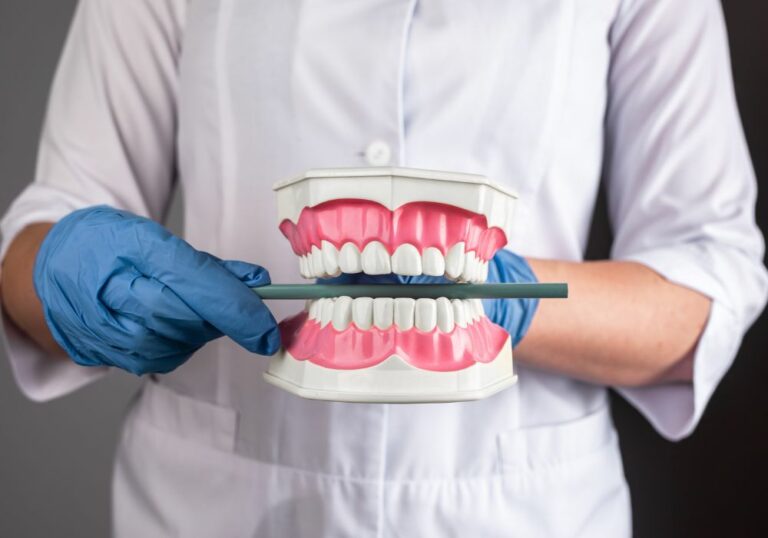
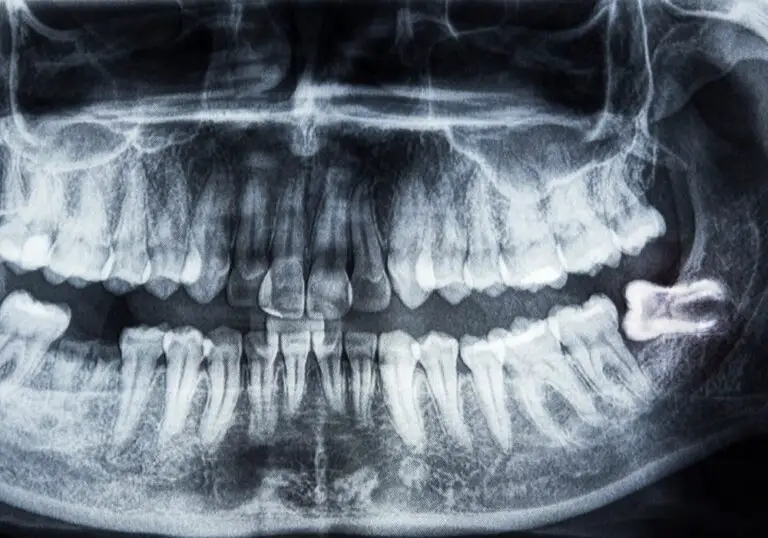
Losing all of your natural teeth is an unfortunate reality for many adults. According to the CDC, about 120,000 Americans become edentulous each year. As the population continues to age, those numbers are projected to grow. For the millions who suffer complete tooth loss, getting dentures is often the go-to solution to restore their smiles and ability to eat.
What Causes Full Tooth Loss?
There are a number of reasons people end up losing all their natural teeth. Some of the most common include:
- Gum disease – Periodontitis is the #1 cause of tooth loss in adults. When severe gum inflammation and infection persists, it can destroy the tissues and bone supporting the teeth. This eventually leads to tooth loss.
- Tooth decay – Untreated dental caries can decay a tooth to the point it cannot be saved. If decay is rampant, multiple teeth may need extraction.
- Poor oral hygiene – Failing to brush and floss properly allows plaque buildup. This increases the risk for both dental caries and periodontitis.
- Trauma or injury – Accidents and sports injuries can knock out teeth or fracture them beyond repair. Multiple traumas can lead to losing all teeth.
- Medical conditions – Diseases like diabetes make gum infections worse and impair healing. Some medications also cause excessive dry mouth, ramping up decay risk.
- Substance abuse – Long-term use of drugs or alcohol abuse increases odds of oral health problems. Meth mouth is notorious for destroying teeth.
- Genetics – Some people are just prone to weaker teeth or accelerated bone loss around teeth for hereditary reasons.
- Financial barriers – Inability to access or afford dental care means tooth problems go untreated, eventually resulting in extractions.
Who Is a Candidate For Complete Dentures?
In general, if you have lost all natural teeth in both upper and lower jaws, or even in just one arch, you are likely a candidate for complete dentures. However, there are certain factors the dentist considers when determining candidacy:
- Oral health – Any oral infections should be fully resolved. Gum disease requires treatment before denture placement.
- Medical status – Severe chronic diseases like uncontrolled diabetes may compromise healing after extractions.
- Anatomy – Adequate bone and healthy oral tissues are needed to support dentures. Some bone grafting may be required.
- Restorative needs – Either or both arches may require dentures depending on your unique needs.
- Lifestyle – Activities with high trauma risk may make dentures inadvisable. Manual dexterity issues can also affect use.
- Patient expectations – Goals for esthetics, phonetics, and function should align with denture capabilities.
With careful case assessment, planning, and patient compliance, most edentulous people can successfully adapt to and benefit from complete dentures.
Overview of the Complete Denture Process
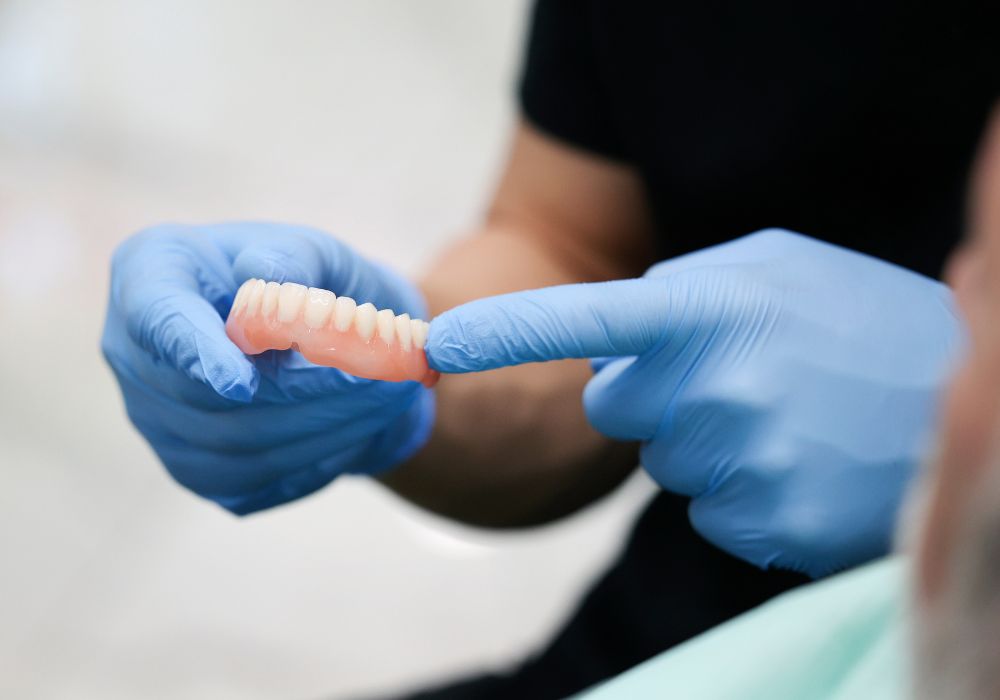
Getting dentures made is a multifaceted process involving several key steps:
Impressions and Records
The dentist takes precise impressions of the edentulous ridges and jaw relationships. Bite registration, facial measurements, and lip support needs are also recorded. Preliminary models are created to assess bone shape and volume.
Design and Arrangements
Based on records, the dentist maps out the optimal denture tooth selection, size, and arrangement to fulfill esthetic and functional objectives.
Try-ins
Trial dentures are inserted to evaluate their fit, retention, comfort, occlusion, and aesthetics. The patient provides feedback on any needed adjustments before final processing.
Extractions and Healing
Any remaining hopeless teeth are extracted before final dentures are made. Time is allowed for complete healing of extraction sites, usually several months.
Final Dentures and Delivery
Master impressions are taken of healed ridges. Final dentures are fabricated, then adjusted as needed chairside before being delivered to the patient.
Post-Insertion Care
Several follow-up appointments are needed to ensure the patient is adapting well to the new dentures and wearing them correctly. Refits and relines may be required within the first year as the jawbones undergo remodeling changes.
Options for Replacing a Full Set of Teeth
For patients undergoing complete tooth loss, traditional removable full dentures are not the only option. Depending on the individual case and patient preferences, some alternatives may include:
Implant-Retained Dentures
Dentures can be securely anchored in place using a select number of dental implants surgically placed in the jawbone. This prevents slippage and provides superior stability and chewing function compared to regular dentures.
All-on-4® Prostheses
Four dental implants strategically placed in the jaw can support a non-removable prosthesis of replacement teeth. The teeth are permanently fixed to the implants as a full arch restoration. No denture is needed.
Same-Day Teeth
Utilizing CAD-CAM technology, a full arch of replacement teeth can sometimes be milled and inserted immediately following extractions. This newer protocol skips the healing phase and lets patients leave with a temporary fixed prosthesis the same appointment.
Dental Bridges
If adequate natural tooth roots remain, they may be prepared to support a fixed dental bridge to replace missing teeth instead of opting for a removable partial or full denture.
The Advantages and Disadvantages of Complete Dentures
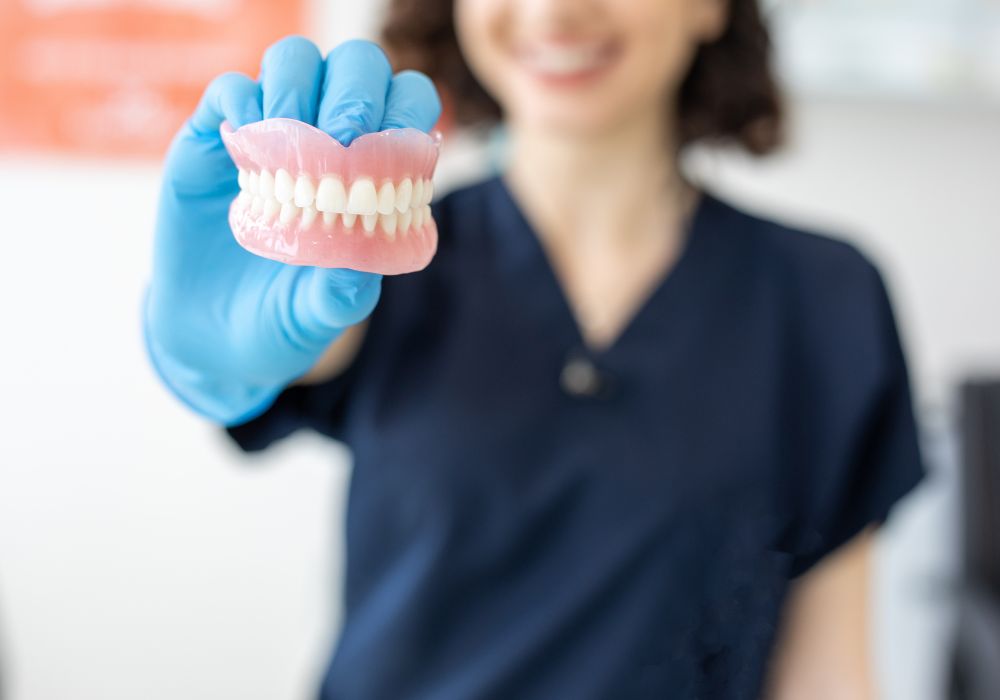
There are both benefits and downsides associated with getting full dentures to restore the entire upper and/or lower arches:
Advantages
- Relatively low cost tooth replacement option
- Replaces all missing teeth in one or both arches
- Restores facial esthetics and ideal occlusion
- Improves chewing, speech and confidence
- Existing dentures easily repaired or remade
- Only requires minor oral surgery for extractions
- Can be used temporarily before getting implants
Disadvantages
- Period of discomfort and adaptation required
- Ongoing need for denture adhesives
- Higher risk of irritation or sores
- Fluid and soft food diet usually needed
- Difficulty eating hard, sticky foods
- Jawbone resorption reduces fit over time
- Lower dentures prone to looseness/movement
- Can trigger gag reflex in some wearers
- May limit types of physical activities
By understanding the pros and cons, patients can decide if complete dentures are right choice for them. Alternatives may be considered based on individual circumstances.
Key Steps for Caring for Complete Dentures
To help ensure dentures remain functional and oral health is supported, patients should:
- Rinse dentures after eating – This prevents food debris buildup that can lead to staining, bad breath, and increased plaque on dentures.
- Remove and clean dentures daily – Use liquid hand soap or a recommended denture cleaner and soft bristle brush to gently clean dentures each day. Avoid stiff brushes and strong chemicals.
- Soak dentures overnight – Soaking allows oral tissues to rest, unless otherwise advised by the dentist. Use cool clean water or a mild cleansing solution.
- Visit the dentist routinely – See your dentist every 6 months even without natural teeth. They will examine oral tissues and determine if denture refits, rebases or replacements are required.
- Avoid long-term denture adhesive use – Using adhesive constantly to improve retention indicates improper fit. Have the dentist adjust, reline or remake ill-fitting dentures.
- Watch for signs of irritation – Red, inflamed or ulcerated gums under dentures must be evaluated promptly for needed adjustments.
Following proper at-home denture care and routine dental visits ensures you get the most out of your custom appliances. Be sure to alert your dentist to any concerning symptoms or issues with your dentures.
Conclusion
For those who have lost all of their natural teeth, getting dentures can be an effective and affordable way to restore your smile, chewing ability, and confidence. With proper planning and care, complete dentures can provide years of reliable service. However, they do have some inherent limitations. Working closely with your dentist to evaluate all tooth replacement options and select the best treatment plan based on your needs, preferences, and overall health is key to making sure you end up with a smile you are happy with and dentures that fit you well and enhance your quality of life. With realistic expectations and good oral care, dentures can successfully restore functionality for people dealing with complete tooth loss.
Frequently Asked Questions
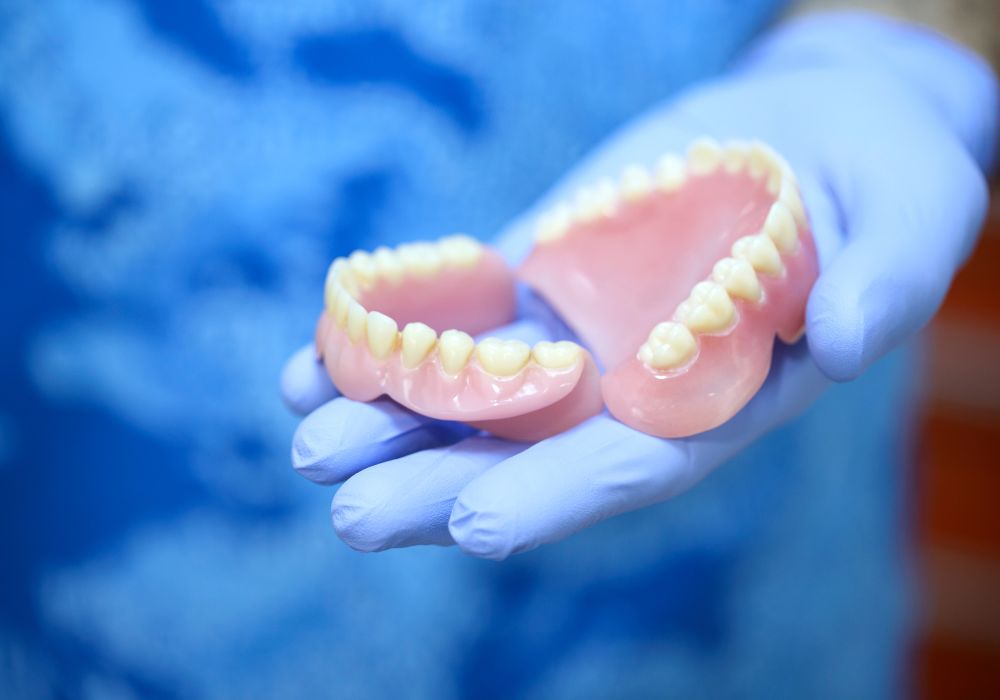
Q: Can dentures be made the same day teeth are extracted?
A: Immediate dentures placed at the time of extractions are no longer recommended. A period of several months is required after extractions for complete healing before taking final denture impressions. However, a temporary set can be worn during this transition.
Q: How long does it take to get used to wearing dentures?
A: Most patients require a period of adaptation that ranges from several weeks to a few months as they adjust to their new dentures. Getting comfortable with insertion, removal, chewing, and other functions takes practice and patience. Speaking normally also requires time to relearn.
Q: Do dentures always need to be replaced eventually?
A: Over a period of 5-7 years, the jawbone and gums shrink and change shape. This means even well-fitted dentures will require relining or rebasing for a renewed proper fit. Complete remakes of ill-fitting dentures are sometimes necessary for optimal functionality.
Q: Can dentures allow me to eat a normal diet?
A: Dentures may require some adjustments in food choices and preparation at first. But with practice, they should allow you to enjoy a variety of nutritious foods. Starting with soft, moisture-rich foods helps the transition to dentures. Your dentist can recommend the best diet strategies.
Q: Why do the lower dentures seem to slip more than the upper?
A: The lower jaw has less bony surface for suction-style retention compared to the upper arch. Also, the lower denture flanges sit against muscular moveable tissue instead of firmer palatal tissues, leading to increased movement and loosening problems.