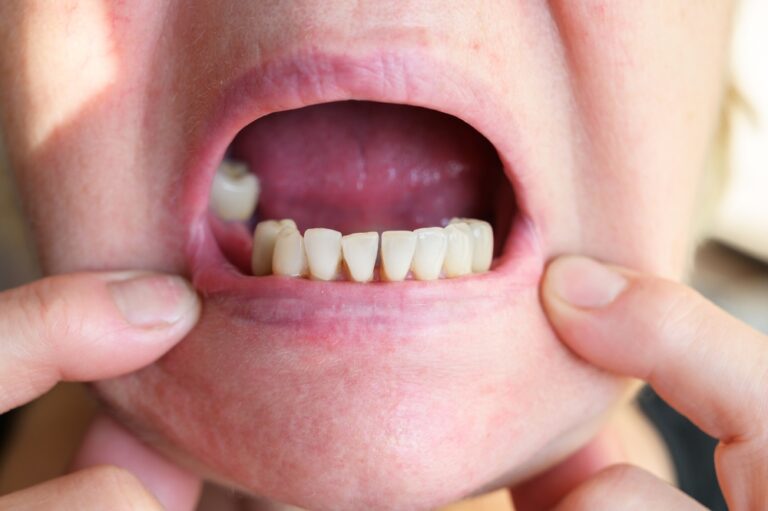
Tooth decay and damage can begin mildly but worsen over time, leading to crumbling, fractured, or even lost teeth. While extracting damaged teeth was once the norm, advances in dentistry now enable repair and restoration of even severely compromised teeth.
With procedures like root canals, crowns, implants, bridges, inlays, onlays, and veneers, patients can often salvage and rebuild cracked, broken, or decayed teeth. This article explores causes of tooth destruction, detailed processes for restoration, aftercare and longevity of repaired teeth, costs, plus factors in deciding between restoration versus extraction.
What Leads to Severe Tooth Damage?
Teeth face constant threats from decay, fracture, trauma, and other harm. Without prevention and treatment, the following issues can lead to severely damaged teeth:
Tooth Decay
- Cavities from poor hygiene, acidic/sugary foods, dry mouth
- Extensive decay into inner dentin and pulp layers
Fractures and Cracks
- Cracked cusps from chewing hard foods or bruxism grinding
- Fractures from sports injuries, accidents, or high impact forces
- Vertical root cracks extending deep below the gumline
Trauma and Injury
- Chipped or broken teeth from falls, accidents, violence
- Clenching or grinding damage over time
- Previous faulty dental work putting stress on teeth
Other Factors
- Gum disease eroding bone support for roots
- Age deterioration and thinning enamel
- Habits like nail biting, ice chewing, pens/pencils
Without treatment, damage progresses. Decay reaches the inner tooth layers, fractures deepen and split roots, chipped areas worsen. At a certain point, restoration becomes necessary to save crumbling, fragmenting teeth.
Options for Repairing Broken, Decayed, or Fractured Teeth
Several tooth-saving options exist. The best choice depends on factors like:
- Amount and type of damage
- Location on the tooth
- Pulp condition
- Number of teeth involved
- Finances and insurance
Possible treatment plans include:
1. Dental Fillings
Fillings repair mild to moderate decay confined to outer enamel. The decay is removed and filled with gold, composite resin, porcelain, or another filler material.
However, fillings have limitations:
- Not effective for extensive damage extending deep into dentin/pulp
- Prone to fractures with substantial loss of tooth structure
- Material shrinkage can lead to secondary decay
2. Dental Inlays and Onlays
Inlays and onlays are indirect fillings made of porcelain, composite, or gold. They are used when decay or damage extends past initial enamel layers.
These restorations fit over remaining tooth structure like a cap for added support and protection.
| Inlays | Onlays |
|---|---|
| For tooth cusp damage | For damage covering multiple cusps |
| Fit inside center of tooth | Cover part or all of chewing surface |
| Made from gold, composite, or porcelain | Made from gold, composite or porcelain |
Inlays and onlays durably restore form and function but require reshaping healthy areas.
3. Dental Crowns
Also called caps, crowns sit over the entire visible section of a tooth. They are necessary when:
- Over 50% of tooth structure is missing
- Following root canals or pulp removal
- Securing dental bridges or implants
Crowns protect and reinforce the remaining structure. Custom-made from ceramic, porcelain-fused-metal, or other materials, they encase the core tooth and recreate the original anatomy.
With good oral hygiene, crowns may last 10-15 years or longer before replacement is needed. They are the treatment of choice for fractured, decayed, or broken teeth not amenable to other options.
4. Root Canal Treatment
If tooth decay or damage extends internally into the pulp and root canals, the nerve may become infected and abscessed. Root canal treatment is done to remove diseased pulp, clean and shape the canals, then fill and seal them.
Afterward, an onlay, crown, or other restoration is required to seal the tooth. Together, root canal treatment and protective capping can rescue even severely compromised teeth.
5. Dental Implants
Dental implants act as artificial tooth roots for permanently replacing missing teeth. The implant screw fuses to the jawbone and supports a realistic porcelain crown.
Implants are the optimal choice when natural teeth are unrestorable due to:
- Severe structural loss
- Advanced fractures or decay
- Failure of previous root canals
- Periodontal disease with substantial bone loss
With success rates over 95%, implants offer a permanent and esthetic solution.
6. Dental Bridges
A dental bridge spans between two healthy teeth on either side of a missing one. The bridge is cemented into place and includes:
- A false replacement tooth fused between two crown abutments
- Crowns on the adjacent anchoring teeth for support
While bridges do not protect original tooth structure, they offer an option for replacing hopelessly damaged or already lost teeth.
7. Dental Veneers
Veneers are thin porcelain facings that fit over the front and outer surfaces of teeth. They improve aesthetics by masking:
- Stained or discolored teeth
- Permanently chipped teeth
- Minor gaps or irregularities
However, veneers do not restore or reinforce damaged inner tooth structure. They are a superficial option for front teeth with only cosmetic flaws.
When Tooth Extraction Is Necessary
Despite advanced restorative options, some cases of severe tooth destruction still require extraction:
- Unrestorable decay affecting most of the tooth structure
- Extensive damage well below gumline
- Failed previous root canals with reinfection
- Severe periodontal disease with major bone loss
- Other issues making restoration unfeasible
Hopeless teeth that cannot adequately support restorations may need to be removed. Implants can replace the extracted teeth if desired.
The Tooth Restoration Process
The processes involved in repairing and capping damaged teeth take precision and skill. Key steps include:
Damaged Tooth Preparation
The target tooth is numbed with local anesthetic before reshaping. Decay and fractures are removed to leave only healthy tooth structure. The tooth is reduced in size/shape to accommodate a well-fitting restoration.
Impressions and Temporary Restoration
An impression is taken of the prepared tooth and sent to the dental laboratory. A temporary restoration is fitted to protect the tooth for the 1-2 weeks until the permanent one is fabricated.
Permanent Restoration Placement
At the bond appointment, the dentist checks fit and aesthetics of the new crown, onlay, etc. It is tried in, adjusted as needed, then permanently cemented into place.
Proper tooth preparation and a precision restoration ensure maximum longevity and function.
Caring for Restored Teeth
Getting damaged teeth restored is the first step. Ongoing care and maintenance are key to avoiding recurring issues. Recommendations include:
- Practice meticulous oral hygiene – Brush gently 2-3 times daily with toothpaste for restored teeth and floss thoroughly each day. This prevents decay and infection around restorations.
- See your dentist regularly – Get professional cleanings and exams every 6 months to catch any problems early. Have x-rays taken annually to check for new decay.
- Protect from further damage – Wear a mouthguard during sports to shield restored teeth. Use a nightguard if you grind your teeth.
- Avoid chewing or biting with pressure – Go easy on hard, crunchy, chewy, and sticky foods which could crack restored teeth.
- Quit smoking – Smoking stains restorations and increases plaque buildup and decay risk. The heat can also cause bonding failure.
- Repair minor damage immediately – Small fractures in restorations should be repaired before they worsen. Letting them progress risks expensive re-treatment.
With diligent home care and dental maintenance, restored teeth can function optimally for years before needing repair or replacement. Monitor them closely and seek prompt care for any emerging problems.
Longevity of Dental Restorations
With proper placement, care, and upkeep, quality dental restorations can last many years. However, they are not permanent and will require replacement at some point.
Factors impacting average longevity include:
- Patient habits – Teeth grinding, nail biting, chewing on pens, and similar behaviors increase stress on restorations.
- Oral hygiene – Poor brushing and flossing leads to decay, which damages restorations and supporting teeth.
- Regular dental visits – Routine professional care helps early detection of any issues needing repair.
- Restoration material – Gold, porcelain, and ceramic last longer than composite resins.
- Restoration quality – Precision impressions, proper bonding, and expert placement increase durability.
- Jawbone health – Periodontal disease progressively weakens bone support for restorations.
With optimal conditions, the following average longevities can be expected:
| Restoration Type | Average Longevity |
|---|---|
| Dental fillings | 5-10 years |
| Inlays/onlays | 5-15 years |
| Dental crowns | 10-15+ years |
| Fixed dental bridges | 7-15+ years |
| Root canal treatments | 8-12+ years |
| Dental implants | 15-25+ years |
Your restorations may need replacement sooner or last longer depending on your unique situation. Work with your dentist on a timeline for monitoring and replacing restorations as needed.
Costs of Tooth Restoration Procedures
Restoring damaged or lost teeth is an investment in your health and smile. Prices vary based on your location, dental office, materials utilized, and insurance coverage. Some general cost ranges are:
- Dental fillings – $150-$300 per filling
- Inlays/onlays – $650-$1,500 per tooth
- Metal crowns – $800-$2,500 per tooth
- Porcelain crowns – $800-$3,000+ per tooth
- Root canal treatment – $400-$2,000 per tooth
- Dental implants – $1,500-$6,500+ per implant
- Fixed bridges – $700-$15,000 total
Many dental insurance plans cover a portion of restorative and prosthetic costs. CareCredit and other financing options can also help cover out-of-pocket fees.
To maximize value, choose high-quality materials from reputable labs and skilled clinicians. While costlier initially, durable materials like lithium disilicate crowns may save money long-term through their longevity and stain resistance.
Deciding Between Tooth Restoration and Extraction
In cases of advanced tooth destruction, whether to attempt restoration or proceed directly to extraction is a key decision. Factors to weigh include:
- Amount of healthy tooth left – Insufficient tooth structure eliminates some restoration options.
- Additional complications – Prior failed root canals, severeperiodontal disease, and fracture extent may rule out repair.
- Restoration feasibility – Not all damage patterns, locations, or forces can be predictably restored.
- Infection presence – Persistent infections may need extraction to fully resolve.
- Tooth prognosis – Likelihood a restoration will provide substantial durable function based on factors.
- Patient wishes – Some patients prefer extraction over lengthy restoration procedures despite tooth-saving potential.
- Finances – Implants and major work may be cost prohibitive despite being technically possible.
If extracted, adjacent and opposing teeth are also evaluated for increased stress risk. Replacing the space with an implant or bridge ideally follows shortly after extraction.
Through comprehensive planning, even extremely damaged and crumbling teeth can often gain new life through meticulous restoration work. In cases where extraction is chosen or unavoidable, reliable tooth replacement options allow restoration of your smile. Partner closely with your dentist to determine the optimal treatment path for your needs.
Frequently Asked Questions
Are root canals absolutely necessary before crowns?
It depends on the health of the inner pulp. If it is decayed or inflamed, a root canal is needed to prevent further infection. If the pulp is healthy, a crown can be placed directly.
Do crowns and veneers look and feel natural?
Quality crowns and veneers fit seamlessly and mimic natural tooth color/translation very closely. Patients typically adapt to the feel soon after placement. Improvements in materials continue to enhance aesthetics and comfort.
Can bridges be used instead of implants for multiple missing teeth?
Bridges can fill spaces of 2-3 adjacent missing teeth by extending crowns off neighboring teeth. However, bridges have drawbacks like greater strain on anchor teeth and lower long-term success compared to non-connected implant crowns.
Will teeth adjacent to extractions also need crowns?
Teeth next to extractions often endure increased forces that make crowns advisable. Your dentist can evaluate the need for reinforcement based on occlusion and function following extraction.
Are there ways to reduce tooth restoration costs?
Options like choosing amalgam over porcelain fillings, metal over zirconia crowns, or waiting for dental school clinics can lower some costs. Dental tourism is risky. Discounts shouldn’t compromise material quality. Carefully weigh cost vs value tradeoffs.