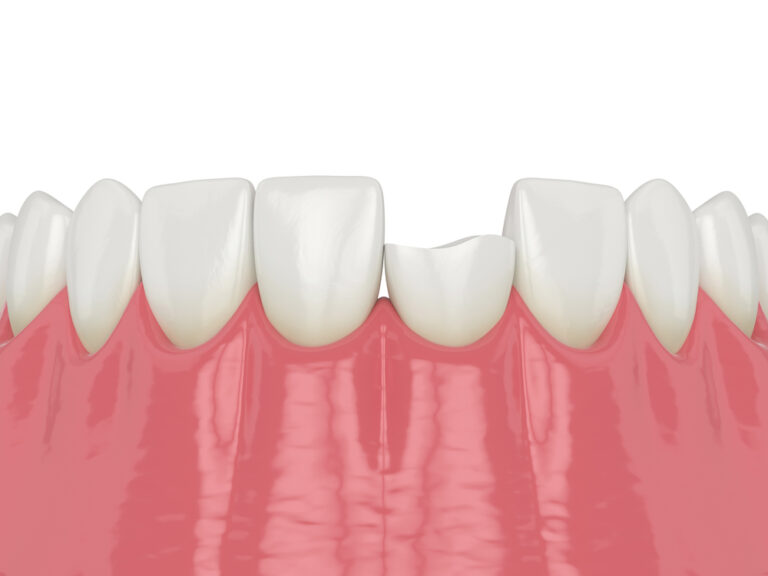
A tooth infection, also known as a dental abscess, occurs when bacteria or fungi invade the pulp of the tooth. The pulp contains nerves, blood vessels, and connective tissue and is located in the center of the tooth surrounded by dentin.
When bacteria invade the pulp, it becomes inflamed and infected. This is often caused by untreated tooth decay, a cracked tooth, improper dental work such as a filling or crown, trauma to the tooth, or advanced periodontal disease. As the infection spreads, it can travel through the tiny root canal system of the tooth and spread to the surrounding jawbone, causing a painful abscess to form.
Common signs and symptoms
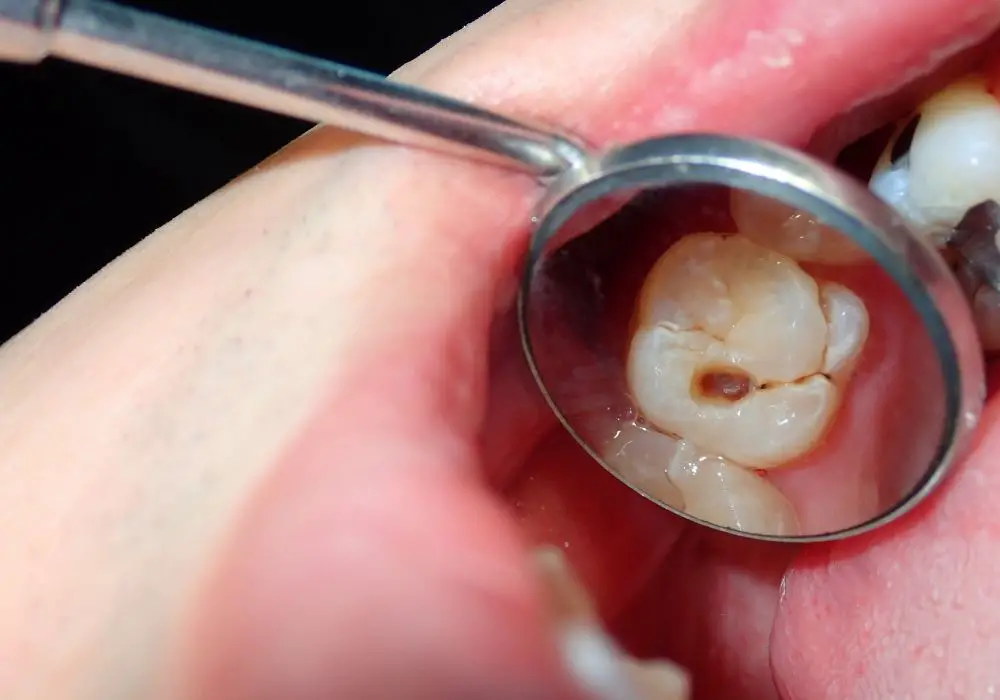
There are several common signs and symptoms of a tooth infection. Symptoms may develop suddenly or slowly worsen over time:
- Tooth pain or sensitivity – Often severe, constant, throbbing pain that can radiate to other areas of the mouth, ears, or head. Pain may be triggered by hot, cold, sweet, or acidic foods and drinks.
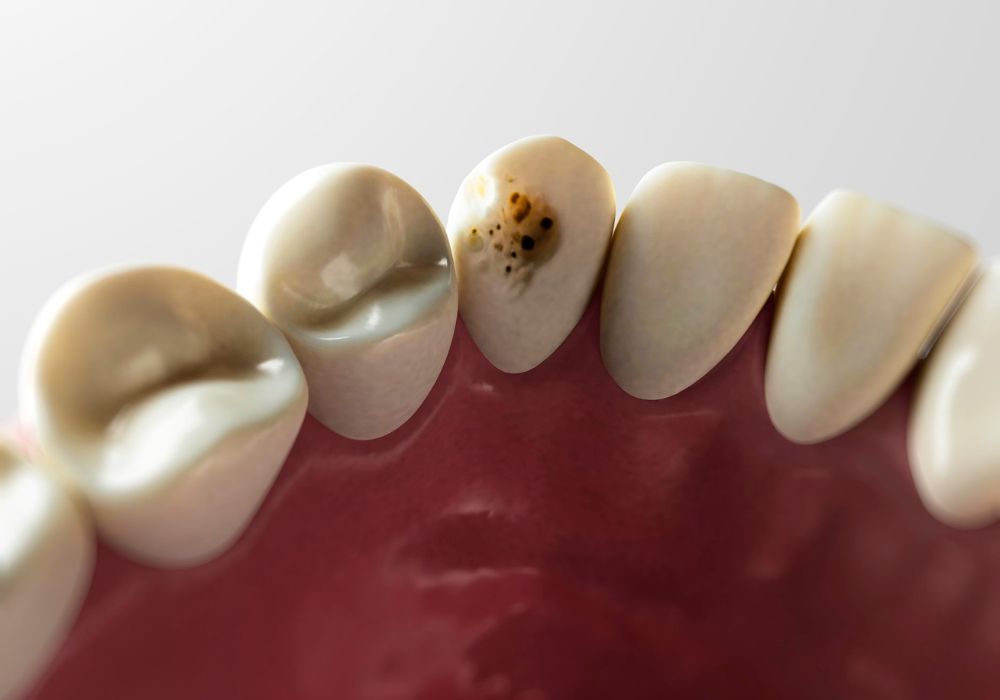
- Tooth discoloration – The tooth may darken, turn grayish, or develop brown/yellow hues.
- Swelling – The gums around the tooth may become inflamed, reddened, and very tender. The face, cheek, or neck may swell.
- Pus discharge – Yellow or white thick pus may drain from the gums around the tooth. A bad taste or odor is common.
- Gum recession – The gums may pull away from the tooth, exposing more of the root.
- Loosening of the tooth – It may feel slightly loose or wiggly.
- Fever and chills – A low-grade fever, fatigue, and body aches sometimes occur with a tooth infection.
If the infection spreads it can lead to complications like facial cellulitis, cavernous sinus thrombosis, Ludwig’s angina, and sepsis. Prompt dental treatment is essential.
Determining if the tooth can be saved
If you notice signs of a possible tooth infection, promptly contact your dentist for an exam. Do not delay seeking care. The dentist will evaluate the tooth visually, tap on it to test for sensitivity, look for drainage, and take x-rays. The x-rays allow them to see below the surface to determine the extent of infection and damage.
Based on their examination, they will advise you if the infected tooth may be treated and saved or if extraction is necessary. Here are some key factors they will consider:
- Extent of infection – How far has the infection spread into the tooth, root, gum tissues, and jawbone? Infections limited to the pulp have the best prognosis.
- Amount of bone loss – Severe loss of the bony socket around the tooth makes saving it less likely. The infection can destroy bone.
- Tooth location and function – Front teeth or premolars have a better chance of being saved given their visibility and role in chewing. Heavily infected back molars often require removal.
- Your symptoms – Severe, unrelenting pain and swelling usually indicates a serious infection requiring extraction. Mild cases are often treatable.
- Your medical history – People with conditions like diabetes, cancer, or HIV are at higher risk for dental infections spreading. Extraction may be safer.
- Tooth integrity – Can the remaining tooth structure adequately support a filling or crown? Extensive decay weakens the tooth prognosis.
- Cost considerations – Root canal is cheaper than extraction and replacement, but not if the tooth ultimately can’t be saved.
With evaluation and x-rays, your dentist will determine if attempting to save the tooth is appropriate or if removal is the wiser option. Do not attempt “home remedies” or wait to see if symptoms subside on their own. Prompt professional assessment and treatment are crucial.
Treating an infected tooth
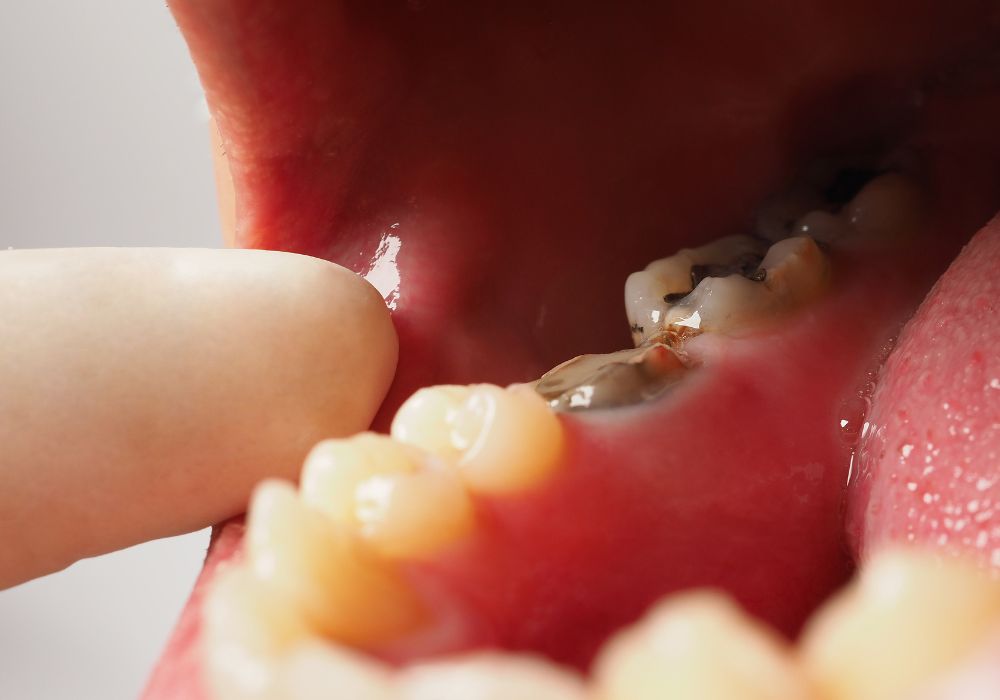
If the dentist confirms the infected tooth can be restored, treatment will begin right away. Here are the typical procedures used to treat a tooth infection:
Root canal treatment
The primary treatment for an infected tooth is a root canal procedure. This involves drilling into the tooth, removing the infected soft pulp tissue, disinfecting and sealing the inner tooth structures, and sealing up the access hole.
The steps commonly include:
- Local anesthesia is administered to fully numb the tooth and surrounding area.
- A tiny hole is drilled through the biting surface of the tooth into the pulp chamber.
- Infected tissue is removed from the pulp chamber and root canal(s) with special tiny instruments.
- The entire root canal system is thoroughly cleaned, shaped, and disinfected using medicated irrigation solutions.
- The cleaned out chamber and root canal are permanently filled and sealed with an inert rubbery material called gutta percha.
- A temporary restoration or crown is placed to completely seal the access hole while the tooth heals.
- A follow-up appointment is required to receive the final crown or filling restoration.
Root canal treatment is very effective for disinfecting the inner tooth and stopping the infection. It may take 1-3 appointments depending on factors like infection severity and how many roots the tooth has. Symptoms generally start improving after the first visit.
Medications
The dentist will often prescribe antibiotics like penicillin or amoxicillin to help fight the tooth infection while root canal treatment is done. Anti-inflammatory drugs can also help reduce swelling and discomfort. Pain medications like ibuprofen are recommended as needed. Use medications only as directed and complete the full course.
Follow-up care
After treatment, practicing excellent oral hygiene and avoiding chewing on the tooth during the healing process are important. See your dentist as recommended for evaluations to confirm the tooth is healing properly. They will also take follow-up x-rays and replace the temporary filling with a permanent one once healed. Report any renewed pain or symptoms immediately.
When treated promptly and cared for diligently, root canal treatment can effectively treat an infected tooth and allow it to heal and function normally again. But delaying care raises the risk of extraction becoming necessary.
When extraction is required
In some moderate to severe cases, the dentist may advise extracting the infected tooth as the only option. Reasons the tooth may be deemed non-salvageable include:
- The pulp chamber is inaccessible due to extensive fractures or crown damage.
- There is substantial deterioration of the tooth structure and surrounding bone.
- The infection persists despite root canal attempts.
- The tooth cannot be restored well due to fragility or gaps in remaining structure.
- Medical conditions like heart disease make extraction the safer option.
- The costs of other treatment options are prohibitive.
Extractions are performed under local anesthesia. The dentist will gently loosen the tooth and remove it completely. They may use instruments like elevators and forceps for a simple extraction. Surgical extractions are more complex, involving incisions in the gums to remove bone and divide the tooth if needed.
The resulting gap left by an extracted tooth requires careful consideration. Leaving a missing tooth space long term allows your other teeth to shift and promotes chewing problems and bite issues. Discuss options like dental implants, bridges, or partial dentures with your dentist to determine the optimal way to replace the lost tooth.
Can an infected tooth heal on its own?
It would be extremely rare for an infected tooth to heal on its own without treatment. Since the infection is embedded deep within the tooth’s interior layers, the immune system cannot effectively reach and eliminate the infection alone.
Some people may try home remedies like rinsing with salt water or using cloves for temporary pain relief. But these cannot cure the actual infection. Over-the-counter pain medicine only masks symptoms. Without professional dental treatment, the infection will persist indefinitely.
If an infected tooth is left untreated, eventual tooth loss is highly likely. The infection will continue worsening and spreading until it destroys the tooth completely. Do not attempt to wait out a tooth infection or hope it heals spontaneously. Seek prompt dental care for the best chance of saving your tooth.
Preventing tooth infections
While some causes of tooth infections like trauma are unavoidable, diligent oral health care and dental care can reduce your risks:
- Brush thoroughly twice a day and floss once daily to lower oral bacteria.
- Use antiseptic mouthwash to reduce bacteria between teeth.
- See your dentist regularly for cleanings and checkups to find issues early.
- Have cavities filled before they extend deeply towards the pulp.
- Address cracks in teeth quickly before bacteria can enter the inner layers.
- Wear a mouthguard during sports to protect teeth from trauma and infection risk.
- Limit consumption of sugary foods and acidic drinks that can erode enamel.
- Quit smoking, as it impairs healing after dental procedures.
- Control chronic conditions like diabetes that increase infection susceptibility.
With diligent oral hygiene and preventive dental care, you can keep your teeth healthy and hopefully avoid serious tooth infections. But even with great care, infections can sometimes still occur. Remember to see your dentist promptly if you notice any symptoms of possible infection. Early intervention gives you the best chance of treating the infection and saving your tooth.
Frequently Asked Questions
Can I wait a few days to get an infected tooth treated?
No, you should not wait to seek treatment for an infected tooth. Even waiting a few days allows the infection time to worsen and spread into the bone surrounding the tooth. This can lead to serious complications and reduce your chances of saving the tooth. It is important to see a dentist immediately for antibiotics and root canal treatment or extraction to stop the infection before extensive damage occurs.
How long can an untreated tooth infection last before becoming serious?
This varies, but most untreated tooth infections will eventually become serious if left alone. The infection can smolder indefinitely inside the tooth, often flaring up into abscesses that discharge pus. It usually spreads into the bone within weeks to months. Seeking prompt treatment is critical, as a chronic, untreated tooth infection has a high likelihood of eventually becoming a severe problem requiring extraction.
Can I take antibiotics without having the infected tooth treated?
You should not rely only on antibiotics without also receiving dental treatment for an infected tooth. Antibiotics alone cannot eliminate the infection inside a tooth – the source of the infection must be treated directly. Taking only antibiotics can temporarily reduce some symptoms, but it will not resolve the infection. Combining antibiotics with root canal or extraction of the infected tooth is essential for a complete cure.
What home remedies help an infected tooth?
There are no home remedies capable of curing an established tooth infection. However, you can use remedies like ice packs, coconut oil pulling, warm saltwater rinses, cloves, or over-the-counter pain relievers to temporarily relieve discomfort until you can see a dentist. Good oral hygiene is also important. Home remedies should not be used as substitutes for professional treatment.
Can an infected toothache go away and come back?
Yes, the pain from an infected tooth can fluctuate or seem to disappear at times, only to return later. This occurs because the infection may temporarily drain or discharge pus, relieving pressure and pain. But the infection itself remains active inside the tooth’s pulp, and the pain eventually recurs when more pus and pressure build back up in the confined space. The tooth requires treatment even when symptoms subside temporarily.
How do you disinfect an infected tooth yourself?
There is no effective way to fully disinfect an infected tooth at home on your own. The infection is contained inside layers of the tooth that you cannot access or clean adequately on the surface. Effective disinfection requires professionally drilling into the tooth and pulp to remove all infected tissue and bacterial biofilm, irrigate the inner tooth chambers, and inject antibacterial solutions. Only your dentist has the tools and training to properly disinfect an infected tooth from the inside out.
When is a tooth infection considered an emergency?
A tooth infection is generally considered a dental emergency if you have swelling of the face or throat, trouble breathing or swallowing, severe uncontrollable pain, or other systemic symptoms like high fever. These can indicate a serious spreading infection that needs immediate attention to prevent complications. Otherwise, most tooth infections require prompt but not necessarily emergency treatment within 24-48 hours by a dentist to prevent worsening damage.
Can an infected baby tooth be saved?
It is rarely recommended to do root canal treatment on an infected baby tooth. Baby teeth that become severely decayed or infected are usually extracted since they will eventually fall out. However, if it is a molar important for chewing or preventing crowding it may be treated. The dentist will evaluate whether trying to save it is appropriate based on the risks and benefits for the child. But extraction is the typical choice for an infected baby tooth.