Tooth decay, known in the medical field as dental caries or cavities, is among the world’s most prevalent chronic diseases. It affects people across all ages and demographics. According to the CDC, over 90% of adults aged 20-64 have experienced decay in their permanent teeth. Untreated caries can lead to infection, tooth loss, and potentially serious systemic health issues.
But while highly common, tooth decay is also highly preventable in most cases. And even after cavities develop, modern dentistry offers several techniques to stop and even reverse early stage decay. This in-depth article explores the causes of tooth decay, risk factors, preventive strategies, and both non-invasive and restorative treatments to halt the destruction of this all-too-common dental disease.
Causes and Progression of Tooth Decay
Tooth decay is fueled by acid attacks that gradually dissolve away enamel and dentin. But where does this acid come from? And how exactly does it damage teeth? Here’s a closer look at the biological processes behind cavities.
Role of Oral Bacteria
Our mouths contain a diverse microbiome with over 700 species of bacteria. Most are harmless. But a few bad actors drive the onset and progression of dental caries. Streptococcus mutans and Lactobacillus are the prime culprits.
These and other cariogenic (cavity-causing) bacteria feed on fermentable carbohydrates – namely sugars and refined starches. As they metabolize carbohydrates, their digestive process releases acid as a byproduct. The bacteria then use these organic acids to dissolve minerals from the tooth surface.
Some of the acids produced include:
- Lactic acid
- Formic acid
- Acetic acid
- Propionic acid
These acids easily dissolve the mineralized tissues of teeth – the hard outer enamel and the underlying dentin layer.
Demineralization
The first stage of cavity formation is demineralization – acids dissolve the mineral content of enamel, causing it to soften and develop tiny pores and flaws. The enamel surface becomes weak and vulnerable to further attack.
Enamel is composed mainly of:
- Hydroxyapatite – a crystalline calcium phosphate mineral
- 96% inorganic materials
- 4% water and organic material
But fluoride from foods, water, and dental products converts some hydroxyapatite into fluorapatite – which is less soluble and more resistant to acid dissolution.
If the acidic environment continues unabated, enamel will eventually crack, chip, and cavitate. The damage then spreads inward to the softer dentin layer underneath.
Destruction of Tooth Layers
Enamel is the hardest substance in the human body. But its mineral content gets progressively less dense moving toward the enamel-dentin junction. In early decay, acids first demineralize this outermost enamel which has the highest mineral content.
Once the enamels weakest areas are penetrated, the fungus-shaped rods that comprise enamel start to break and collapse. The intricate architecture of enamel rods unravels, and pores fuse together into ever-larger holes. Cavities form.
The thinner enamel at the enamel-dentin junction is highly vulnerable to acid dissolution. The demineralization process then advances into the collagen-rich, reparative dentin. This soft, bonelike tissue composes the bulk of the tooth. Demineralization in dentin occurs rapidly. The porous dentin matrix provides little resistance to bacterial enzymes and acids diffusing inward.
As decay reaches the inner pulp chamber, connective tissue, nerves and blood vessels become inflamed. Bacteria and bacterial toxins invade the pulp, causing infection, abscesses, pain and eventual necrosis. From here, tooth loss is imminent without intervention.
Are Cavities Reversible?
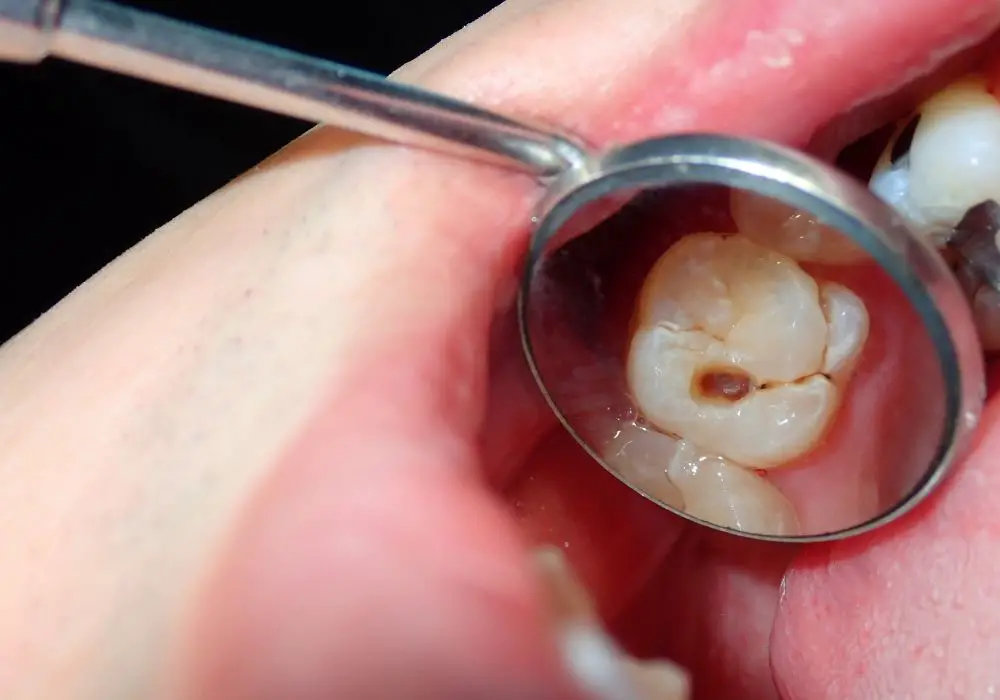
The early stages of dental caries confined to enamel demineralization may be halted or remineralized before a frank cavity forms. But once decay penetrates through enamel into dentin, restoration is needed to stop its progression.
Remineralization
Exposing weakened enamel to minerals like fluoride, calcium and phosphate can rebuild and harden its surface. These minerals redeposit into the microporous spaces created during demineralization. This process is called remineralization.
Fluoride is especially effective for remineralization as it converts hydroxyapatite to stronger fluorapatite. Topical fluorides also exert antibacterial effects.
Some sources of remineralizing fluoride include:
- Fluoridated toothpaste, mouthwash, gels
- Professionally applied fluoride treatments
- Fluoridated drinking water
- Fluoride releasing dental restorations
Calcium and phosphate salts likewise restore lost minerals. However, saliva cannot concentrate them well. Thus, technologies like amorphous calcium phosphate (ACP) are often used to intensify and localize their delivery along with fluoride.
But if the onslaught of acids continues, remineralization will fall behind demineralization. The decay process will overwhelm and outpace repair efforts. More invasive treatments become necessary to stop cavities.
Non-Invasive Treatment for Early Decay
Detecting and treating demineralized areas or small cavities early allows remineralization and other non-invasive therapies to repair the damage before resorting to traditional fillings or crowns. Some of these minimally invasive techniques include:
Dental Sealants
Sealants are thin plastic coatings applied to the chewing surfaces of back teeth. They penetrate pits and fissures to deprive bacteria of their protected breeding ground. Sealants also create a physical barrier that starves bacteria by blocking their food source.
Sealing over early lesions or undetectable demineralization prevents further progression. Sealants also undergo microleakage less often than traditional fillings. They are highly effective at preventing cavities in children and teens.
Silver Diamine Fluoride
SDF can arrest, harden, and disinfect existing cavities by microbiological and chemical means. This clear liquid solution of silver particles in ammonia water is simply brushed on affected areas.
SDF works in three ways:
- Silver ions act as a broad antimicrobial, killing acid-producing bacteria.
- Silver and fluoride ions together remineralize softened tooth structure.
- Silver ions bind to proteins in carious dentin inhibiting bacterial enzymes and metabolic activity.
Clinical studies show SDF stops around 70% of cavities from expanding. It is an inexpensive and non-invasive application for young, anxious, or special needs patients.
Ozone Therapy
Applying ozone gas locally can halt decay by oxidizing and annihilating acid-producing microorganisms in early lesions. In one study of initial occlusal cavities, ozone arrested the lesions in 97% of cases after 90 days.
However, ozone cannot rebuild lost tooth structure. It must be followed up with remineralization therapy.
Atraumatic Restorative Treatment (ART)
ART involves manually removing decayed enamel and dentin using hand tools only – no drill or anesthesia required. The cleaned and shaped cavity is then sealed with an adhesive filling like a resin or glass ionomer.
Compared to traditional rotary drilling, ART better preserves healthy tooth structure. It triggers less inflammation, pain, and anxiety as well. ART can be used for small cavities in children. It also serves well for treating caries in areas with limited dental care resources.
Treating Extensive Decay
Non-invasive methods have their limitations. If caries lesions are too advanced, fail to respond, or penetrate too deeply, more aggressive intervention is indicated. Traditional fillings and dental crowns remain the standard of care for large or severe cavities.
Drill and Fill Cavities
When decay is rampant and Pierre Fauchard’s seminal book, The Surgeon Dentist: A Treatise on Teeth, was published in 1728, the treatment options were downright medieval. They included:
- Bloodletting
- Blistering agents
- Purgatives
- Potions containing everything from burnt roses to human skulls
- Gruesome tooth extractions and transplants between individuals
While some remedies seemed barbaric, Fauchard did introduce early operative dentistry – advocating the use of instruments and more scientific techniques to treat tooth decay.
In the 19th century, amalgam filling material was developed and rotary drills were introduced. By 1890, G.V. Black’s concepts of cavity preparation cemented the foundation of oral surgery and restorative dentistry practiced today.
The standard technique to treat extensive decay includes:
- Administering local anesthesia around the affected tooth
- Using a high-speed drill and hand instruments to fully excavate all soft, damaged, and infected tooth structure
- Shaping and smoothing the resultant cavity to create retention and prevent further decay
- Disinfecting the preparation with an antimicrobial rinse
- Selecting and placing a suitable dental filling material to restore form and function
- Trimming, carving, and polishing the hardened filling for proper contour and occlusion
Advantages of Dental Fillings
- Highly effective at stopping decay and preventing recurrence
- Restores strength, integrity, and usage of the tooth
- Suitable for cavities too large for non-invasive methods
- Filling materials are durable, esthetic, and inexpensive
Disadvantages of Dental Fillings
- Invasive procedure requiring anesthesia
- Unpleasant drilling causes heat and pressure damage to healthy pulp
- Up to 70% of tooth structure removed to gain access and retention
- Brittleness and microleakage can lead to secondary decay
- Replacement eventually required as fillings age and degrade
Crowns
When decay is extensive, a filling leaves too little natural tooth structure. A full coverage crown is placed instead. The tooth is reduced in size then fitted with a cap that fully encases the outer surface.
Crowns provide a durable, impervious seal. However, they involve aggressive removal of healthy enamel and dentin. With a proper oral hygiene routine, both traditional fillings and crowns may last 10-15 years or longer before replacement is needed.
Can Cavities Recur After Fillings?
Yes, it’s possible for decay to return and form secondary or recurrent caries under, around or over a filling or crown. Some reasons caries may recur include:
Residual Bacteria
- Not all bacteria were removed when the cavity was originally excavated
- Bacteria may invade along the filling margins
- Rough filling edges harbor plaque
Poor Oral Hygiene
- Plaque buildup allows new decay adjacent to the restoration
Defective Fillings
- Fillings crack, wear down, loosen, or exhibit marginal leakage
- Bacteria and fluids sneak underneath
Repeated Acid Challenges
- Persistent frequent snacking keeps pH low
Xerostomia
- Reduced saliva flow limits remineralization
Getting cavities filled early before extensive enlargement, maintaining excellent oral hygiene, and adopting preventive behaviors reduces recurrence risk. But some potential for new decay around old fillings persists in most patients throughout life.
Evidence-Based Measures to Prevent Cavities

Preventing the colonization and proliferation of pathological oral bacteria is the key to thwarting tooth decay from the start. Both the frequency and duration of acid attacks must be limited to maintain healthy enamel.
Here are some of the most important, scientifically proven ways to prevent caries from forming:
Remove Plaque Daily
Tooth brushing and interdental cleaning is essential to disrupt the plaque biofilm and reduce the cariogenic microbial load. Brushing mechanically removes acid-producing bacteria before they can colonize and multiply.
Fluoride Exposure
Topical fluorides strengthen enamel making it more resistant to demineralization. Fluoride also promotes remineralization and inhibits bacterial enzymes. Fluoride used consistently is a powerful cavity-fighter.
Diet Modification
Reducing consumption of fermentable and acidic foods limits the substrate these bacteria need to thrive. Limiting acidic beverages and constant between-meal snacks provides remineralization periods.
Dental Sealants
Sealing vulnerable pit and fissure surfaces denies acid-producing bacteria their protected niche needed to advance decay.
Disrupt Biofilms
Agents like chlorhexidine, xylitol, and SDF alter bacterial adherence and metabolic activity.
Saliva Stimulation
Chewing sugar-free gum or using a lozenge after meals brings salivary pH back to neutral faster. Saliva washes away bacteria and provides calcium and phosphate ions.
Routine Dental Visits
Early detection of demineralization before cavities enlarge limits damage. Regular cleanings also remove heavy plaque below the gumline.
A multipronged approach combining proper homecare, professional treatment, and sensible dietary habits offers the best protection against tooth decay. But for existing cavities, the non-invasive interventions discussed earlier provide hope for arresting and repairing the damage before resorting to the dentist’s drill.
Frequently Asked Questions
Here are some common patient questions about tooth decay along with brief answers:
Q: What food causes the most cavities?
A: Sticky candies like taffy and gummies that adhere and linger on teeth. Starchy snacks like chips and crackers also damage teeth.
Q: Can I get cavities in my baby teeth?
A: Yes, infants can develop caries soon after teeth erupt. Babies should see a dentist after the first tooth appears or by age 1.
Q: Do sour candies cause cavities?
A: Not likely – many sour candies are low in sugar. But they do temporarily soften enamel. Sticky, sugary candies pose a higher cavity risk.
Q: Can tooth decay go away naturally?
A: Early stage decay in enamel may reharden with excellent oral hygiene and fluoride. But once decay penetrates deeper layers, professional treatment is required.
Q: How can I relieve a toothache?
A: First, rinse with warm salt water to relieve irritation. Floss to dislodge any trapped food. Take over-the-counter pain relievers compatible with your medical history. Schedule a dental visit promptly to treat the cavity causing discomfort.
Q: If I stop eating sugar, will my cavities disappear?
A: No, avoiding all sugars and carbs alone won’t cure existing cavities. But limiting sugar intake does reduce the frequency and impact of acid attacks. See your dentist to treat active decay.
Q: Why do my fillings need to be replaced?
A: Fillings wear down over time, crack or come loose. Margins allow new decay. After 10-15 years, replacement is often needed. Newer bonding techniques give better longevity than old silver fillings.