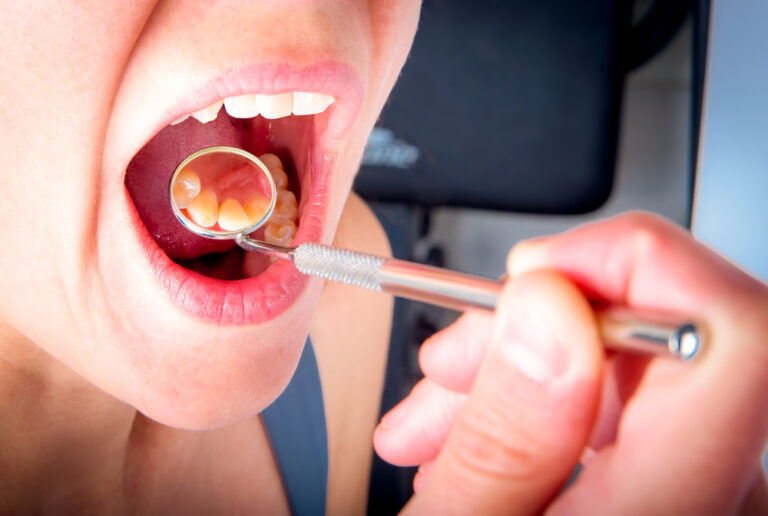
It’s not uncommon to notice an unpleasant odor coming from the back of your teeth. This smell, sometimes described as rotting, fecal, or fishy, can be alarming. But what causes bad breath originating from the back of your teeth? And what can you do about it?
There are a few potential culprits that could cause odors in the back of the mouth. Let’s explore the most common reasons in detail.
Causes of Smell from the Back of Teeth
Food Debris and Bacteria
Food and bacteria are likely the most common sources of bad breath from your teeth.
As you eat, small bits of food get trapped in narrow spaces between teeth and gums. Bits of meat, dairy products, starchy foods, and sugary treats often get stuck. These food morsels start to decay as bacteria break them down, creating gases with a foul, rotting odor.
Bacteria naturally accumulate on the tongue, gums, and teeth – especially when you don’t brush properly. Thick layers of bacteria can build up, forming a biofilm coating called plaque. Common bacteria found in plaque include Streptococcus mutans, Actinomyces, and various gram-negative rods.
These bacteria feast on trapped food particles in your mouth, generating smelly waste products like hydrogen sulfide, methyl mercaptan, cadaverine, and skatole. The sulfur compounds produce a particularly unpleasant, rotten egg-like odor.
Some especially stinky oral bacteria include:
- Porphyromonas gingivalis – a gram-negative anaerobe associated with gum disease. It produces many foul metabolites.
- Prevotella intermedia – gram-negative bacteria linked to inflammation of the gums. It increases in gum pockets.
- Fusobacterium nucleatum – an anaerobic rod abundant in plaque on tooth surfaces. It generates hydrogen sulfide gas.
Without regular brushing and flossing, rotting food debris and smelly bacteria can reside in your mouth for days, gradually worsening breath. The longer debris and bacteria remain, the stinkier breath becomes.
Dry Mouth
Saliva helps cleanse your mouth and wash away bacteria. When saliva production is reduced, bacteria can multiply rapidly.
Conditions that can cause dry mouth include:
- Medications – Antihistamines, decongestants, pain medications, antidepressants, muscle relaxants, high blood pressure medications, and Parkinson’s disease drugs often have dry mouth as a side effect.
- Medical treatments – Radiation therapy to the head and neck and chemotherapy can damage salivary glands, decreasing saliva.
- Autoimmune disorders – Sjogren’s syndrome damages moisture-producing glands, leading to chronic dry mouth. Lupus may also cause dry mouth.
- Diabetes – High blood sugar levels increase fluid loss, contributing to dry mouth.
- Nerve damage – Injuries or conditions affecting the nerves that stimulate salivary glands can inhibit proper saliva production.
- Yeast infections like oral thrush – A fungal overgrowth in the mouth restricts saliva.
- Smoking and tobacco use – Chemicals in tobacco can inflame salivary glands.
- Alcohol use – Alcohol is dehydrating and slows saliva flow.
- Caffeine – As a stimulant, caffeine can make you mouth feel dry.
- Breathing through mouth – Chronic open-mouth breathing due to nasal obstruction can evaporate moisture.
- Stress and anxiety – Stress affects the autonomic nervous system’s regulation of saliva.
With inadequate saliva flow, food and dead cells can sit in the mouth longer. Bacteria feast on these particles, releasing foul gases detected at the back of teeth. Dry mouth provides an environment conducive to uninhibited bacterial growth.
Gum Disease
Gum disease occurs when plaque deposits inflame the gums. This early stage is known as gingivitis. As the disease worsens to periodontitis, deep pockets form between the gums and teeth.
These infected pockets harbor destructive anaerobic bacteria, which thrive in the low oxygen environment beneath the gumline. Toxins and enzymes released by these bacteria irritate gums and rot away tooth structures.
Eventually, the gum pulls back from the tooth, forming even deeper pockets up to 9mm deep. Bacteria and dead cells accumulate in these voids. Putrefaction of this debris produces foul sulfur gases.
As gum disease advances, odors from festering bacteria and rotting food particles in these pockets can produce bad breath originating in the back of the mouth. The deep gum pockets become reservoirs for foul odors.
Tongue Coating
The tongue’s rough, bumpy surface provides an ideal habitat for odor-causing bacteria to cling to. These microbes thrive on the moist, warm environment of your tongue.
They feed on food particles trapped between the tiny crevices and dead epithelial cells shed from the tongue’s surface. This provides nutrition for rapid bacterial proliferation.
A white or yellowish tongue coating often develops, comprised of bacteria, food debris, dead cells, and mucus. These large formations are called tongue plaque. Studies show that those with tongue coating have more volatile sulfur compounds linked to bad breath.
This foul-smelling gunk trapped between the papillae (tiny bumps) on your tongue can lead to unpleasant smells coming from the back of your throat. Bacteria residing on the tongue are released when you breathe, sending stinky gases over your taste buds.
Tonsil Stones
Tonsil stones, also called tonsilloliths or tonsiliths, are clusters of debris and bacteria that become lodged in the tonsils’ nooks and crannies.
These masses are composed of food particles, mucus, dead cells, and sulfur compounds produced by bacteria. The anaerobic bacteria reduce sulfur into hydrogen sulfide gas, which produces the classic rotten egg odor.
Tonsil stones become coated with minerals like calcium and magnesium from saliva, which helps harden them into calcified clusters.
Since your tonsils are located at the back of the throat, tonsil stones can be a major source of bad breath originating from the rear of the mouth. The stones smell especially putrid when dislodged.
Solutions for Smelly Breath from Back Teeth

If you’re plagued by bad breath from the back of your teeth, try these self-care tips:
- Brush thoroughly twice a day – Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least 2 minutes, angling the bristles under the gumline to dislodge trapped germs. Replace your brush every 3-4 months.
- Floss at least once daily – Flossing removes food particles and plaque from tight spaces between teeth that brushing misses. For maximum effectiveness, use a mint-flavored floss that has fluoride.
- Scrape your tongue – Using a tongue scraper helps remove bacteria coating the tongue. Scraping twice a day is more effective than brushing the tongue.
- Rinse with an antibacterial mouthwash – Look for mouthwashes with cetylpyridinium chloride to help kill germs. Don’t use mouthwash as a substitute for brushing and flossing, however.
- Drink plenty of water – Staying hydrated helps produce more saliva, which naturally washes away bacteria and odors.
- Limit dry mouth triggers – Avoid or reduce intake of foods, beverages, and medications that restrict saliva flow. Always stay hydrated. Use a humidifier if the air is very dry.
- Quit smoking and limit alcohol – Smoking makes your mouth more hospitable to odor-causing bacteria. And alcohol dries out the mouth.
- Avoid pungent, sulfur-rich foods like garlic and onions – The breakdown products that cause these foods’ characteristic odors get transferred to your breath. Parsley, mint, and citrus fruits can help freshen breath after eating these foods.
These simple yet effective measures can help freshen your breath by removing bacteria, food particles, and tongue coatings – the primary culprits of bad mouth odor. But if an unpleasant smell coming from the back of your throat persists despite good oral hygiene, see your dentist or physician.
Your dentist or doctor can identify any underlying medical conditions contributing to bad breath, such as diabetes, reflux disease, or sinus infections. Specialized testing can help pinpoint the types and concentrations of odor-causing bacteria inhabiting your mouth. This enables targeted treatment.
Professional dental cleaning scrapes away hardened plaque, tartar, and bacteria on teeth and along the gumline that regular brushing can’t reach. Your dentist may also recommend prescription antimicrobial mouthwashes to reduce certain oral bacteria.
For gum disease, professional plaque removal is paired with deep cleaning below the gumline. Antiseptic chip treatments help fight infection in periodontal pockets. Severe gum disease may require surgery to remove diseased tissue and reduce deep pockets.
Medications or oral appliances can increase saliva production if dry mouth is an issue. Your doctor may adjust any medications that are restricting saliva flow.
Tonsil stones may warrant removal by an otolaryngologist. If they continue forming, tonsillectomy can permanently prevent foul-smelling tonsil stones.
With diligent oral hygiene, treatment of any underlying conditions, dietary adjustments, and help from your dentist and doctor, you can successfully tackle foul odors coming from the back of your teeth and enjoy fresher breath.
Frequently Asked Questions
What is the white stuff on the back of my teeth?
The white material on the rear surface of teeth is usually plaque – a sticky film of bacteria, food debris, saliva, and dead cells. Without thorough daily brushing and flossing, plaque builds up and starts to harden into tartar due to mineralization. This plaque and tartar provide a prime breeding ground for smelly bacteria on back teeth.
Why does my breath smell like poop?
Breath that smells like feces is often caused by gut bacteria. Partially digested food moves from your intestines into the bloodstream and eventually gets expelled when you exhale. Medical conditions like acid reflux, metabolic disorders, kidney disease, and liver problems can make this worse.
Oral bacteria produce trace amounts of fecal-smelling compounds. And poor oral hygiene also contributes to poop-smelling breath. Deficient brushing allows more bacteria and the smelly metabolites they produce to build up.
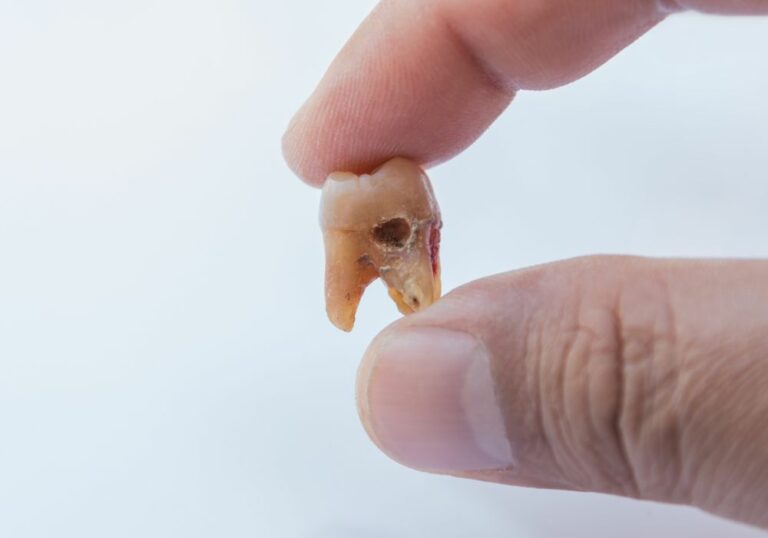
Do dental problems cause bad breath?
Absolutely. Gum disease creates deep, infected pockets around teeth that collect rotting food particles and odorous bacteria. Tooth decay and dental infections also breed smelly bacteria. Poor fitting crowns, bridges, and dentures with gaps provide crevices for bacteria to hide. And ill-fitting or unclean dentures provide porous surfaces for bacteria to proliferate.
What home remedies freshen breath?
Effective home remedies for bad breath include brushing and flossing thoroughly, using antibacterial mouthwash, drinking plenty of water, scraping the tongue, quitting smoking, and avoiding pungent trigger foods.
Baking soda helps neutralize acids and odors. Essential oils like peppermint, eucalyptus, and tea tree have antimicrobial effects. Drinking green tea inhibits bacteria growth. Chewing fruits like apples, pears, and citrus scrubs bacteria and provides freshening acids.
When should I see a doctor for bad breath?
You should make an appointment with your healthcare provider if bad breath persists for over 2 weeks despite meticulous oral hygiene and hygiene. Foul odors can signal an underlying medical condition needing treatment, like chronic sinusitis or diabetes.
See a doctor promptly if you notice bad breath along with other concerning symptoms, such as unexplained weight loss, fever, or stomach pain. A doctor can identify any related health issues and provide medications or other therapies to reduce bad breath.
Conclusion
Unpleasant smells coming from the back of your teeth and throat can have several causes. But practicing good daily oral hygiene is the first line of defense against bad breath originating in your mouth. If you take care of your teeth and gums yet odor persists, see a dentist or doctor to get to the bottom of what’s causing your bad breath.
With professional help, diagnostic testing, and treatment, you can pinpoint the source of foul odors in your mouth. By addressing any underlying dental or medical issues, as well as fine-tuning your oral care routine, you can successfully tackle bad breath and enjoy fresher breath from back to front.