What are gum pockets?
Gum pockets, also known as periodontal pockets, are spaces that form between your teeth and gums. They are a key indicator of periodontal disease, which affects the tissues that support your teeth.
Periodontal disease occurs when plaque, a sticky film of bacteria, builds up on your teeth. Plaque hardens into tartar, which irritates the gums and causes them to become inflamed. As the gums pull away from the teeth, pockets form in the gaps. These pockets become filled with bacteria, which can further damage gum tissue and jawbone.
The progression of periodontal disease is often classified into stages:
- Gingivitis – This early and reversible stage involves inflammation of the gums with no bone loss yet. With proper hygiene, it can be reversed.
- Early periodontitis – At this mild stage, gum pockets measure up to 4mm in depth. Some minor bone loss may be present. With treatment, it can be stopped.
- Moderate periodontitis – Gum pockets here range from 4-6mm. More bone loss around teeth is apparent. Dentists will recommend treatment to prevent further progression.
- Severe periodontitis – Marked bone loss is present as pockets exceed 6mm. Teeth may loosen or drift. Extensive treatment is needed to save teeth.
- Advanced periodontitis – Deepest pockets form in this stage, often accompanied by abscesses, pus, and severe gum recession. Aggressive treatment is required, but teeth may still be lost.
Normal pocket depth
In a periodontally healthy mouth, the space between the gumline and tooth is typically 1-3 millimeters deep. This is known as a normal pocket. A depth of 1-3mm allows enough space for the gum tissue and bone to firmly support the tooth.
The sulcus is the shallow groove between the gums and tooth surface. In healthy gums, the sulcus typically measures no more than 3mm in depth. The junctional epithelium is a specialized tissue that creates a seal between the tooth and gumline. This attachment forms a barrier to keep bacteria from invading deeper tissues.
In a normal healthy sulcus and junctional epithelium, no inflammation is present. The tooth is securely attached to the bone by collagen fibers of the periodontal ligament. A healthy sulcus provides a tiny but important protective pocket around each tooth.
What is considered a deep pocket?
Gum pockets are considered deep when they measure 4 millimeters or more. Gum pockets this deep provide an environment where more harmful bacteria can flourish.
Here is a breakdown of different pocket depths:
- 1-3mm: Normal
- 4-5mm: Moderate periodontitis
- 6mm or more: Severe periodontitis
According to the American Academy of Periodontology, any pockets measuring 4mm or deeper indicate some form of damage to the tissues supporting the teeth, known as periodontitis.
In moderate periodontitis, subgingival bacteria increase and pockets progress beyond 4mm. At this stage, gum tissues are deteriorating and bone loss is more visible on x-rays. Your dentist will recommend treatment to stop further disease progression.
Pockets exceeding 6mm signify advanced destruction of gum tissue attachment and supporting bone. Teeth may start shifting or feel loose due to the lost support. Extensive treatment is needed to try to regain lost attachment and bone.
The deeper the pocket, the more severe the disease. Deeper pockets tend to harbor more harmful bacteria and can lead to worsening inflammation and accelerated bone loss around teeth.
How deep can pockets get?
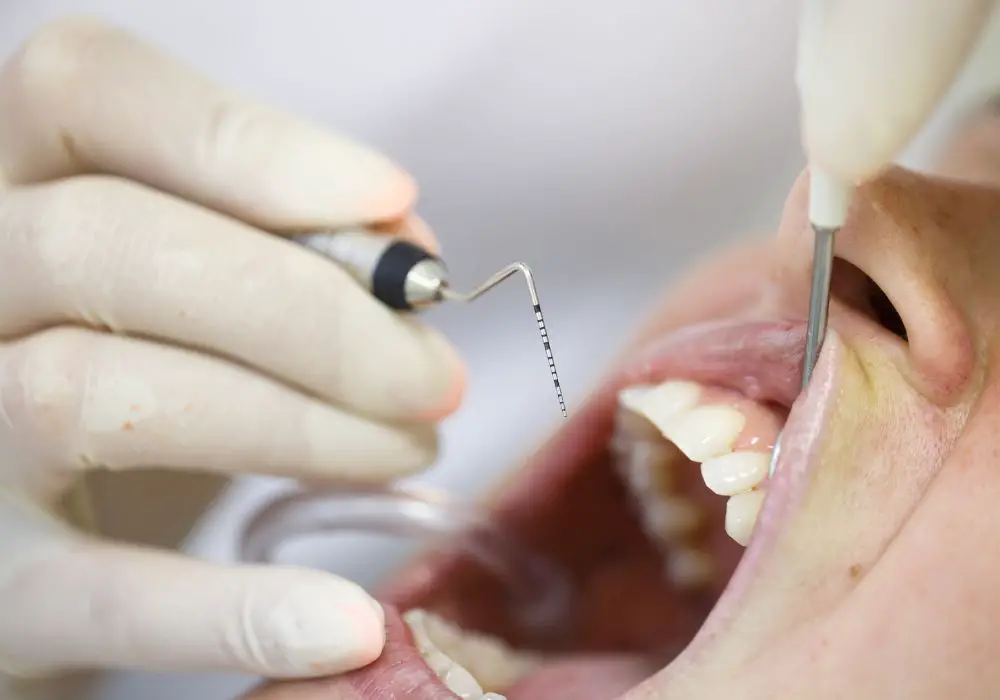
How deep can gum pockets get? Gum pockets can range from 1-3mm to well over 10mm in severe cases of periodontitis.
Here are some examples of very deep gum pockets:
- 7-9mm: At this depth, gum disease is severe and ongoing destruction of bone is happening around the tooth. Tooth loss is likely without treatment.
- 10mm or more: Pockets this deep indicate advanced periodontitis with severe bone loss and inflammation. Teeth become very loose and can no longer be saved.
According to clinical studies, the deepest pocket depths recorded in patients with chronic periodontitis can exceed 10mm and even reach over 12mm in some cases. Ultrasonic probes that measure even deeper than traditional probes have detected pockets up to 16mm deep.
As pockets start to exceed 7mm and especially 10mm, the tooth’s prognosis becomes very poor. At these depths, there is extreme loss of the underlying bone holding the tooth in place. Very deep pockets also contain copious amounts of harmful bacteria that are difficult or impossible to fully eliminate.
What causes deep gum pockets?
There are several possible causes of abnormally deep gum pockets:
- Poor oral hygiene: Not properly brushing and flossing allows plaque to build up and harden into tartar along and under the gumline. This can cause gums to become inflamed and pull away from the teeth.
- Genetic susceptibility: Some people are at higher genetic risk for gum disease and thus develop deeper pockets more readily. Certain genes can negatively impact the immune response to bacteria.
- Smoking/tobacco use: Smoking is a major risk factor for periodontal disease. The over 3,000 chemicals in tobacco smoke and tobacco products damage blood vessels in the gums. This reduces their ability to fight infection and heal.
- Clenching/grinding teeth: This excessive force can traumatize the gums and accelerate tissue damage. It is often worse in cases of crooked, misaligned teeth. Night guards may help.
- Crooked teeth: Teeth that are crowded, spaced poorly, or out of alignment can create areas where plaque easily collects and builds up. This raises chances of gingivitis and periodontitis.
- Hormonal changes: Fluctuations during puberty, menstruation, pregnancy, and menopause can increase gum sensitivity and irritation. Prompt treatment can prevent worsening.
- Stress and anxiety: Chronic stress contributes to inflammation and impacts the severity of periodontitis. Managing stress is important.
- Diabetes: Poor blood sugar control increases susceptibility to oral infections. Meticulous hygiene and blood sugar management is key.
- Medications: Some drugs like phenytoin for seizures, calcium channel blockers, and cyclosporine can cause overgrown gums more prone to periodontitis. Consult your dentist and doctor.
- Poor-fitting crowns or dentures: Dental appliances that do not fit properly can rub on the gums and contribute to irritation, infection, and pocket formation. Prompt adjustments and excellent care of appliances is required.
Signs and symptoms of deep pockets
Signs and symptoms of deep gum pockets may include:
- Gums that bleed easily such as when brushing or flossing
- Gums that are pulling away or receding from the teeth
- Persistent bad breath
- Pus discharge around one or more teeth
- Teeth that feel loose, are shifting, or are sensitive to hot/cold foods
- Changes in bite as teeth drift due to loss of supporting bone
- Exposed tooth roots due to receding inflamed gums
- Deep craters or increasing spaces between teeth
- Sudden teeth sensitivity when previously not sensitive
It is important to note that in early stages, pockets often progress with no obvious pain or symptoms. Many patients are not aware as pockets form and gradually deepen. Getting regular periodontal probing and exams is essential to check for increasing pocket depth.
Complications from deep pockets

If deep gum pockets are left untreated, a number of serious oral health problems can occur:
- Progressive bone loss: Continuing destruction of the jawbone around teeth as infection spreads. This can lead to tooth loosening and loss.
- Gum recession: Gums chronically shrink away from the teeth as inflammation and pockets persist. This exposes sensitive root surfaces prone to decay.
- Tooth loss: With advanced bone loss, teeth can become so unstable they require extraction.
- Systemic inflammation: Bacteria from deep infected pockets enter the bloodstream and travel throughout the body, increasing inflammatory chemicals linked to heart disease, stroke, and diabetes.
- Oral infections: Bacteria trapped deep in pockets can spread and cause painful abscesses in the gums and jawbone, requiring antibiotics and drainage.
- Tooth migration: Without bone support, teeth begin to shift and change position, negatively altering bite.
- Difficulty eating: As more teeth loosen or are lost, chewing ability is impaired. Nutrition can suffer.
The longer deep pockets persist, the more rapid and irreversible the damage becomes. Early treatment is key.
Diagnosing pocket depth
Dentists use a standard instrument called a periodontal probe to measure and diagnose pocket depths during an examination. This thin metal probe is gently inserted into the space between the tooth and gumline. Based on the millimeter markings on the probe that remain visible above the gumline, pocket depth is determined.
Typically, probing is performed at six sites around each tooth. These include the spaces between back teeth and the front, back, and sides of other teeth. This allows dentists to determine the depths of pockets around all teeth. In a healthy mouth, all measurements should be 1-3mm.
Probing is often done annually at preventive cleanings to screen for periodontitis. If any sites exceed 3mm, a full set of probing measurements around all teeth will be taken, and then repeated over subsequent visits to track any changes. X-rays may also be used along with probing to evaluate bone levels around teeth.
Ideally, dentists should evaluate probing under anesthetic for the most precise readings. However, probing without anesthesia is more routine. Gums should still be able to contract against the probe to allow accurate pocket depth measurements.
Treatment for reducing deep pockets
If probing reveals any pockets 4mm or greater, treatment is warranted to reduce pocket depth and prevent additional bone and attachment loss. Options may include:
- Scaling and root planing: A deep cleaning above and especially below the gumline to remove bacterial plaque, tartar, and damaged tissue. Performed over two or more visits.
- Laser therapy: Laser energy kills bacteria inside pockets and promotes healing. Often used with scaling and planing.
- Antimicrobials: Prescription antiseptic rinses or antibiotic pills to reduce bacteria.
- Flap surgery: Gum tissue is lifted and unhealthy tissue removed. Bone irregularities are reshaped and gums repositioned to close pockets.
- Gum grafts: Healthy gum tissue grafted over exposed roots with deep pockets to re-create attachment.
- Bone grafts: Natural or synthetic bone placed in areas of severe bone loss to regenerate support for teeth.
- Growth factors: Special proteins applied to stimulate growth of new bone, gum tissue, and periodontal ligaments.
- Extraction: Hopeless teeth with extreme pocket depths and bone loss may need removal if loose.
- Regular dental cleanings: Usually every 3-4 months along with daily oral hygiene to manage bacteria and inflammation.
Can receding gums grow back?
Unfortunately, receding gums do not grow back on their own once they have shrunk away from the teeth. Because receding gums are a common result of periodontitis and increased pocket depth, treating the underlying disease is the first priority.
Procedures like gum grafting can then be done to replace lost gum tissue and cover exposed root surfaces if needed. During grafting, a small amount of gum tissue is removed from the roof of the mouth or from donor sites in the gums. The graft material is then carefully sutured over areas of recession.
In some cases, synthetic membranes or collagen-based tissue substitutes may be used instead of natural grafting material to stimulate new tissue growth.
With a successful graft, gum coverage of the tooth roots is restored. As blood supply re-enters the grafted sites, the tissue adapts and becomes tightly bound to the teeth. This can recreate the normal gingival margin around teeth. Dentists typically focus on grafting procedures after periodontitis has been stabilized with treatment.
Ongoing oral hygiene and regular dental cleanings are still required after grafting to manage bacteria and prevent additional recession. Quitting smoking also optimizes outcomes.
Good oral hygiene for managing gum pockets

Daily oral hygiene practices are critical for managing increased pocket depth and preventing further gum recession. Excellent home care includes:
- Brushing gently twice daily with a soft or extra-soft toothbrush. Take care not to brush aggressively and recede gums further.
- Flossing once daily to clear bacteria from between teeth. Use caution when flossing near bleeding or painful gums.
- Using antiseptic rinses with ingredients like cetylpyridinium chloride to reduce plaque.
- Rinsing daily with warm salt water to promote healing.
- Replacing toothbrushes every 3-4 months or sooner if bristles appear frayed. Electric toothbrushes may help reduce plaque and gingivitis.
- Eating a balanced diet low in sugary foods and carbohydrate overload to avoid plaque formation.
- Quitting smoking and tobacco products to support gum health and response to treatment.
- Taking any prescribed antibiotics as directed to fully eliminate infections.
Daily oral self-care combined with professional treatment is the most effective way to gain control over gum disease and restore supporting structures. The earlier increased pocket depth is managed, the better the outcomes.
Frequently Asked Questions
How can I tell if I have deep gum pockets at home?
You cannot tell just by looking. Gum recession can occur with minimal symptoms. Regular dental checkups for probing are needed, along with notifying your dentist of any gum swelling, bleeding, or tenderness which could indicate developing pockets.
What happens if I ignore deeper pocket measurements?
Neglecting increased pocket depth of 4mm or more allows the infection process to worsen. Ongoing irreversible bone loss eventually leads to tooth loosening and tooth loss. Research also links untreated periodontitis to increased systemic inflammation and higher risks of heart disease, diabetes complications, and certain cancers.
Can gum pockets come back after treatment?
Yes, new or recurring pockets are possible over time after treatment, especially if oral hygiene is poor. Risk factors like smoking and diabetes must be controlled. Getting professional cleanings every 3-4 months, along with excellent daily brushing and flossing can help sustain results long-term after pocket reduction therapy.
Is antibiotic therapy the solution for deep pockets?
Antibiotics may be appropriate short-term for treating active infections associated with deep pockets. However they cannot eliminate pockets entirely. Antibiotics are just one part of managing advanced periodontal disease, along with deep cleanings, laser therapy, gum surgery, oral hygiene, and ongoing monitoring.
What is the recovery like after gum grafting?
With proper care, gum grafting recovery takes several weeks. Swelling subsides within 7-14 days. Stitches dissolve in 1-2 weeks. Tenderness typically improves significantly after 1 month. Complete tissue healing, maturation and regeneration may continue for 4-6 months. Avoid disturbing grafted areas during healing.
Conclusion
Gum pockets exceeding 3-4mm signify developing periodontitis that warrants treatment intervention. Left unchecked, pockets often progress in depth, resulting in irreversible bone loss around teeth. This can ultimately lead to tooth loosening and tooth loss in advanced disease. Getting regular periodontal examinations and probing is crucial for early detection and treatment of increasing pocket depth before extensive damage occurs. Properly managing periodontal disease also helps reduce systemic health risks. With professional treatment combined with daily oral hygiene, gum pocket depth can be reduced and controlled to preserve the teeth.