Losing bone in the jaw
The jawbone provides crucial support for teeth. When bone density in the jaw diminishes, teeth become loose and vulnerable to loss. This condition, called periodontal disease or gum disease, affects nearly half of adults over 30 in the United States.
As gum disease progresses, the bones, gums and tissue that support the teeth are destroyed. This can eventually lead to tooth loss. Rebuilding lost bone in the jaw may help stabilize teeth and prevent tooth loss.
What causes bone loss in the jaws?
Several factors can contribute to decreased bone density in the jaw:
- Gum disease – Chronic bacterial inflammation destroys gum tissue and bone. The bacteria release toxins that break down the fibers and bone holding teeth in place. As the disease advances, pockets form between the gums and teeth, becoming infected. The body’s immune response causes chronic inflammation, destroying tissue and bone.
- Tooth loss – When a tooth is missing, the bone that formerly surrounded and supported it no longer has a purpose. Without the stimulation from chewing forces, the bone begins to deteriorate and atrophy. The longer a tooth has been missing, the more bone loss occurs.
- Poor nutrition – Diets low in calcium, vitamin D and other minerals contribute to decreased bone mineral density and increase risk of osteoporosis. Nutritional deficiencies reduce bone growth and density throughout the skeleton, including the jawbone.
- Medications – Drugs like oral steroids, anti-seizure medications, immunosuppressants and some cancer therapies weaken bones by inhibiting bone formation and accelerating resorption. The jawbones are especially susceptible.
- Hormonal changes – In women, declining estrogen levels after menopause accelerate bone loss. Up to 20% of total bone mass may disappear in the first 5-7 years after menopause. These reductions in density increase tooth loss risk.
- Health conditions – Diseases like osteoporosis and diabetes mellitus are metabolic disorders that increase overall bone loss and fractures. People with rheumatoid arthritis also frequently experience jawbone destruction.
- Tobacco use – Smoking introduces toxins into the body that destroy bone cells like osteoblasts and osteocytes that maintain jawbone volume and strength. The chemicals in tobacco also limit the growth of new bone tissue.
- Stress – Chronic high stress and elevated cortisol levels activate osteoclasts, cells that break down bone tissue throughout the skeleton. Over time, this reduces bone mineral density. The jaws commonly exhibit severe loss.
Assessing bone loss
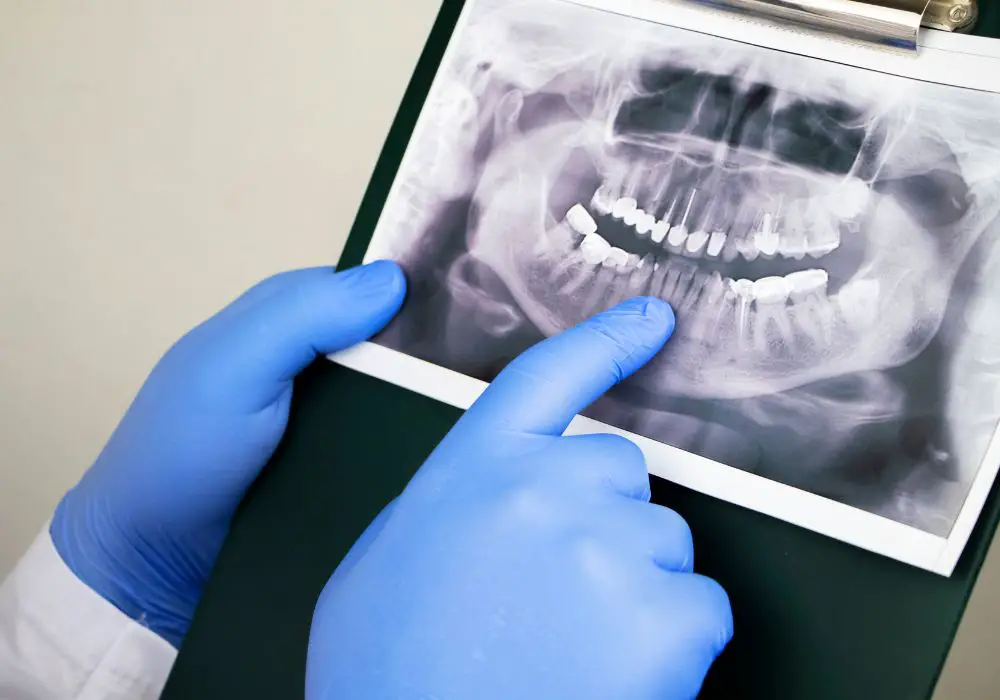
Detecting bone loss early is key to preventing extensive irreversible damage. Dentists have several methods to accurately evaluate bone density and volume in the jaw:
- Visual inspection – The dentist will check for signs of advanced bone loss like loose teeth that shift or change position. Receding inflamed gums, newly exposed root surfaces and teeth appearing longer as gum tissue recedes are red flags.
- Dental X-rays – Intraoral bite wing X-rays show bone levels between teeth. Full mouth series images give an overview of all bone. Panoramic radiographs reveal overall jawbone volume loss. Dentists examine the images for brightness indicating bone loss.
- Clinical measurements – Probing the soft tissue around each tooth with a periodontal probe measures pocket depths, recession levels and clinical attachment levels that quantify bone support and destruction.
- 3D imaging – Cone beam CT scanners provide detailed 3D views of the entire jaw and the bone defects. This helps precisely plan treatment and monitor improvement.
- Laboratory tests – Analyzing biomarkers in gingival crevicular fluid obtained from gum pockets can detect active destruction and inflammation levels.
These diagnostic tools help dentists grade the severity of bone loss and damage to develop an appropriate treatment plan.
Stages of bone loss
Dentists categorize bone loss according to the following stages:
| Stage | Description |
|---|---|
| Stage 1 | Mild inflammation of the gums with no radiographic bone loss visible on X-rays. Bone loss less than 25% of root length. |
| Stage 2 | Moderate gum inflammation with early bone loss around 30% of teeth noticeable on X-rays. Between 25-50% bone loss along tooth roots. |
| Stage 3 | More severe with bone loss radiographically visible around multiple teeth. 50-75% of bone lost around teeth. Teeth may be loose. |
| Stage 4 | Advanced bone loss affecting most teeth, with over 75% of bone lost. Teeth are typically loose and may require extraction. |
The earlier bone loss is detected, the better the chances of rebuilding lost bone tissue before it becomes severe. Ongoing assessments determine whether bone regenerative therapies are succeeding.
Treatment options
Recovering lost bone is crucial for stabilizing teeth and supporting dental implants or other restorations. Several therapies can help regenerate bone in the jaws:
Nonsurgical treatments
- Improved oral hygiene – Thorough brushing twice daily with antibacterial toothpaste, daily flossing, antiseptic mouth rinses like chlorhexidine and regular dental cleanings every 3-6 months all work to remove bacteria-laden plaque that causes gum disease and progressive bone loss.
- Antibiotics – Antibacterial pills like doxycycline hydrate and minocycline hydrochloride reduce infection and inflammation, curbing disease activity and supporting bone regrowth. Localized antibiotic gels placed directly in infected gum pockets also combat bacteria.
- Anti-inflammatory drugs – Over-the-counter NSAIDs like ibuprofen block inflammation, reducing destruction of gum and bone tissues. Some studies suggest a regimen of 400mg ibuprofen 3 times per day may have significant benefits.
- Bone growth factors – Biologically active proteins like enamel matrix derivative applied to exposed tooth roots following deep cleanings stimulate new bone cell growth and formation.
Surgical procedures
- Pocket depth reduction – Folding back the gums, removing infected and damaged tissue down to healthy bone and securing the gums back with sutures physically reduces pocket depth. This supports bone cell regrowth.
- Bone grafts – Particulate graft material packed into bone defects and extraction sockets fills in volume and provides a scaffold for bone cells to populate. Common options include natural bone from the patient, cadavers, cows, pigs or synthetic bone matrix.
- Guided tissue regeneration – Resorbable collagen membranes are placed between the gum and bone, creating a secluded space for bone cells to repopulate without competition from fast-growing soft tissue cells.
- Ridge augmentation – Building up atrophied ridges or jaw segments with bone fillers adds volume and dimensions needed to securely place dental implants.
- Distraction osteogenesis – Using a distractor device, bone segments are gradually separated to stimulate growth of new bone tissue in the opening gap.
With a combination of treatments tailored to the individual, restoring lost bone mass and density is possible in many cases. Proper ongoing oral hygiene and regular dental visits can help maintain bone health over the long term.
Key factors in rebuilding bone
Successfully increasing bone volume and density in the jaw depends on several key factors:
Timing of treatment
Treating bone loss at the very first signs of mild inflammation offers the best chance of regeneration. At later stages, the chronic inflammation can permanently destroy tissues, making rebuilding far more difficult.
Skill of the dentist or periodontist
Specialized surgical skills in techniques like sinus lifts, ridge splits and growth factor applications and experience with advanced regenerative materials and procedures greatly improve outcomes. Board-certified periodontists receive 3+ years of advanced surgical training beyond dental school.
Overall health
Managing systemic conditions like osteoporosis, heart disease, arthritis and diabetes through medication, diet and lifestyle supports bone metabolism and growth. Nutrient intake of calcium, vitamin D and minerals should be optimized.
Commitment to oral hygiene
Daily brushing and flossing to fully remove dental plaque bacteria twice daily is essential for gum health and bone repair and maintenance. Using antiseptic rinses and other aids ensures bacterial control.
Quitting tobacco
Smoking and smokeless tobacco use introduces toxins that inhibit new bone formation. Quitting tobacco is a prerequisite for success of any bone regenerative therapy.
Ongoing dental visits
Seeing a dentist every 3-6 months for professional cleanings, with periodic x-rays to check bone levels, ensures early detection if any new breakdown occurs so treatment can begin promptly.
With diligent daily oral care, tobacco cessation, and close dental monitoring, rebuilding bone lost to gum disease is an achievable goal for many patients.
New frontiers in bone regeneration
Exciting new research is expanding possibilities for jaw bone regeneration:
- Growth factor combinations – Using platelet-derived growth factor (PDGF) and bone morphogenic protein (BMP) in tandem shows promise for more robust bone fill, especially in extraction sockets.
- Platelet-rich plasma (PRP) – Concentrated growth factors from the patient’s own blood, containing proteins like PDGF, TGF-B and others, may enhance healing when added to graft material.
- Stem cell therapy – Implanting cultured adult mesenchymal stem cells can stimulate growth of bone, gums, periodontal ligament fibers and cementum. Research is ongoing seeking the ideal stem cell lines.
- Gene therapy – Introducing bone-regenerating genes into graft areas or host cells via viral vectors may enhance osteoblast proliferation and bone formation.
- Induced periodontal ligament stem cells – These specialized stem cells derived from the patient’s extracted teeth can effectively regrow periodontal ligament tissues, cementum and alveolar bone when re-implanted.
- 3D-printed scaffolds – Custom 3D-printed porous structures made of various polymers and ceramics allow bone cells to efficiently adhere, populate and repair defects.
- Alloplastic bone grafts – Synthetic bone substitutes like hydroxyapatite, tricalcium phosphate, bioactive glass and calcium sulfate reduce complications, costs and graft failure rates compared to natural bone options.
Though still emerging, these cutting-edge techniques could become mainstream options for more predictable and effective bone regeneration where gum disease has caused significant loss.
Maintaining bone density

Once bone density is restored, ongoing meticulous maintenance is vital. Patients must strictly follow excellent oral hygiene with regular dental visits for exams. Dentists will monitor bone levels clinically and radiographically, intervening early if any new breakdown is found.
To help preserve jaw bone density long-term:
- Brush thoroughly with a soft bristle or electric toothbrush and fluoride toothpaste, holding the brush at a 45-degree angle to clean along the gumline, twice per day for 2 minutes each time.
- Floss at least once daily, curving around each tooth to remove plaque from between teeth down to the gumline.
- Use antiseptic mouthwash like 0.12% chlorhexidine gluconate daily to reduce bacteria.
- Have professional dental cleanings and periodontal maintenance done every 3-6 months based on individual disease severity and risk.
- Consider additional dental office antibacterial treatments like localized antibiotic chips or photodynamic therapy to control bacteria.
- Maintain a balanced, nutritious diet with adequate intake of calcium, vitamin D and minerals like magnesium and zinc that support bone metabolism.
- Take supplemental calcium citrate and vitamin D3 if needed to meet daily required intake levels.
- Exercise regularly to stimulate bone growth through weight-bearing and resistance training.
- Get tested and treated for osteoporosis, a major cause of bone loss.
- Have dental x-rays taken at least once per year to check bone levels and look for signs of new disease. Identify problems early.
- See the dentist promptly for any signs of returning gum inflammation, sensitivity or loose teeth. Quickly treating any recurring periodontal infection prevents further irreparable bone damage.
Properly caring for restored areas and unaffected bone is the key to preventing further deterioration and permanent tooth loss due to periodontal disease.
Conclusion
Advanced gum disease can extensively destroy the supporting bone around teeth, but significant regeneration of lost bone volume and density can be achieved with current treatments. Excellent daily oral hygiene, tobacco cessation, diet and nutrition management, professional dental care and early intervention are all critical keys to successfully rebuilding bone lost due to periodontal disease. Emerging biologic regenerative therapies on the horizon also show great promise to further enhance capabilities for more predictable bone formation. With a customized treatment plan and diligent lifelong maintenance care, restoring bone lost to periodontitis is an attainable goal for most patients committed to oral health.
Frequently Asked Questions
Can gum disease cause permanent bone loss?
Yes, advanced periodontal disease often leads to severe irrecoverable bone loss that is impossible to fully regenerate without extensive surgical procedures. The chronic inflammatory disease process permanently damages the tissues supporting the teeth, including alveolar bone. That’s why early prevention and treatment of gum disease before it progresses is critical.
How do dentists rebuild lost bone in the jaw?
Dentists have a range of surgical techniques to regenerate bone. These include bone grafts to introduce graft material into defects, ridge augmentation to increase bone volume, guided tissue regeneration using barrier membranes to exclude soft tissue from bone sites, distraction osteogenesis which mechanically expands bone, and more.
What materials are used for bone grafting in the jaw?
Natural bone from the patient’s own jaw, cadaver bone, bovine or porcine bone can be used. Synthetics like hydroxyapatite, beta-tricalcium phosphate, demineralized bone matrix (DBM) or bioactive glass act as osteoconductive scaffolding. Bone morphogenic proteins (BMPs) or other growth factors are sometimes added to accelerate formation.
How long does it take to regenerate bone in the jaw?
With bone grafting, significant mineralization and bone fill can occur within 2-4 months. But complete maturation and hardening of the regenerated bone typically takes 9-12 months. Having realistic expectations on the extensive healing timeframe is important.
Can you build bone density in the jaw without surgery?
In milder cases caught very early, nonsurgical options like improved hygiene, antibiotics, anti-inflammatory drugs and growth factor proteins may help regain a small amount of lost bone. But for the vast majority of patients, surgical bone grafting procedures are required for any significant regeneration of lost bone volume or density.