Teeth grinding, also known as bruxism, involves involuntary grinding or clenching of the teeth. It often occurs during sleep, called sleep bruxism, but can also happen while awake. Bruxism can lead to other oral health issues if excessive and unchecked. Though there is no definitive cure for bruxism itself, treatments are available to help control symptoms.
Understanding the causes of bruxism
Researchers have not pinpointed any single cause for bruxism. Rather, it appears to result from a combination of physical, psychological, and lifestyle factors:
Physical causes
- Genetics – Studies suggest bruxism runs in families, indicating a potential genetic link. The hereditary structure of the teeth and jaws may promote grinding.
- Neurotransmitter imbalance – Issues with brain chemicals like serotonin and dopamine possibly contribute to bruxism. These chemicals help regulate sleep, moods, and movement.
- Smoking and alcohol – Nicotine from smoking and toxins from heavy alcohol use seem to stimulate the nervous system and trigger jaw and facial tension.
- Medications – Antidepressants, amphetamines, and certain psychiatric drugs are tied to bruxism as side effects. The drugs may overstimulate the nervous system.
- Medical disorders – Conditions like Parkinson’s disease, dementia, epilepsy, and gastroesophageal reflux disease are associated with increased bruxism. The reasons are not always clear.
Psychological factors
- Stress and anxiety – Emotional tension appears to be a major driver of bruxism. Grinding may be an unconscious physical outlet for mental stress. People report more grinding during stressful periods.
- Competitive personality – High-achieving, type A personality types used to striving for success seem more prone to jaw clenching and teeth grinding. It may be tied to perfectionism and frustration.
- Trauma and abuse – Past experiences with trauma, abuse, or neglect have been linked to bruxism, suggesting an underlying psychological component. Grinding may be a residual coping mechanism.
Lifestyle causes
- Caffeine and stimulant use – Excess caffeine from coffee, energy drinks, or medications can stimulate chewing muscles and trigger grinding. Amphetamine drugs markedly increase bruxism.
- Sleep disorders – Conditions like sleep apnea that disturb sleep quality and rhythm tend to cause more sleep bruxism as the body struggles to normalize breathing and brain activity.
- Jaw injury or alignment – Injuries to the temporomandibular joint or misaligned bite due to missing teeth or poor orthodontics can abnormally alter chewing function and provoke grinding habits.
- Gut problems – Issues like reflux and heartburn that interfere with swallowing may lead to changes in mouth and throat muscle activity that prompt grinding behaviors.
Since bruxism arises from various factors, each patient’s specific causes need to be assessed to determine effective treatments.
Recognizing symptoms of bruxism

Signs of possible bruxism include:
- Tooth wear – Excessively flattened, fractured, loose, or chipped teeth suggest grinding forces. Tooth enamel wears down exposing dentin and causing pain.
- TMJ disorders – Earaches, temple headaches, locked jaws, and pain or noises with jaw movement indicate damaged joints and muscles from chronic grinding.
- Check indentations – Awakening with indentations on the cheeks or tongue from teeth indicates nighttime clenching. Damage to the inside of the cheek can also occur.
- Facial pain – Grinding puts strain on the jaw muscles and can cause soreness, tightness, or spasms in the face, temples, and neck area. Pain tends to be worse upon waking after a night of bruxism.
Notify your dentist promptly if you notice any concerning dental changes, mouth pain, or possible grinding signs. Early intervention is key to limit bruxism damage. Keep a log of symptoms to help identify triggers and patterns.
Diagnostic methods for bruxism
Dentists have several methods to analyze and monitor bruxism:
- Clinical dental examination – The dentist visually inspects teeth, gums, and jaw joints for damage indicating grinding. Wear patterns on the biting surfaces can confirm bruxism over time.
- Patient history review – Asking about medical conditions, medications, lifestyle, and symptoms helps identify possible bruxism causes and characteristic patterns like morning headaches or jaw soreness.
- Sleep partner accounts – Bed partners may notice grinding sounds and movements during the night, providing clues about sleep bruxism even if the patient is unaware.
- Home sleep monitors – Small devices worn on the temple or jaw using electromyography (EMG) or audio can record grinding activity during sleep for later analysis.
- Polysomnography – This sleep study done at a clinic uses EMG and audio monitors on the face and head to precisely measure bruxism frequency and intensity overnight.
These diagnostic tools help pinpoint the type of bruxism (awake or sleep) and severity to guide appropriate treatment.
Consequences of leaving bruxism untreated
Without treatment, bruxism causes cumulative damage over months and years:
- Enamel loss and tooth fractures – The chewing surfaces gradually erode under heavy grinding forces, leading to dentin exposure, tooth fractures, and eventual tooth loss in severe cases.
- Headaches and migraines – Jaw tension and soreness from bruxism commonly spreads to the head and neck, resulting in frequent headaches. The pain can become chronic and debilitating.
- TMD joint disorders – The temporomandibular joints and masseter muscles bear the force of repetitive grinding. This leads to inflammation, disc displacement, locking jaws, and degenerative joint changes over time.
- Loss of restorative work – Existing dental crowns, bridges, implants, and other restorations often fail prematurely or require replacement due to damage from chronic bruxism.
- Sleep disruption – Bruxism reduces sleep quality. Tooth damage can also eventually make chewing painful and difficult, interfering with proper nutrition.
- Facial deformities – In severe lifelong cases, the excessive wear on particular teeth tilts and realigns the bite, causing distortion of facial features over decades.
These consequences emphasize the importance of early bruxism management. Routine dental cleanings enable catching problems in the early stages.
Management options for bruxism
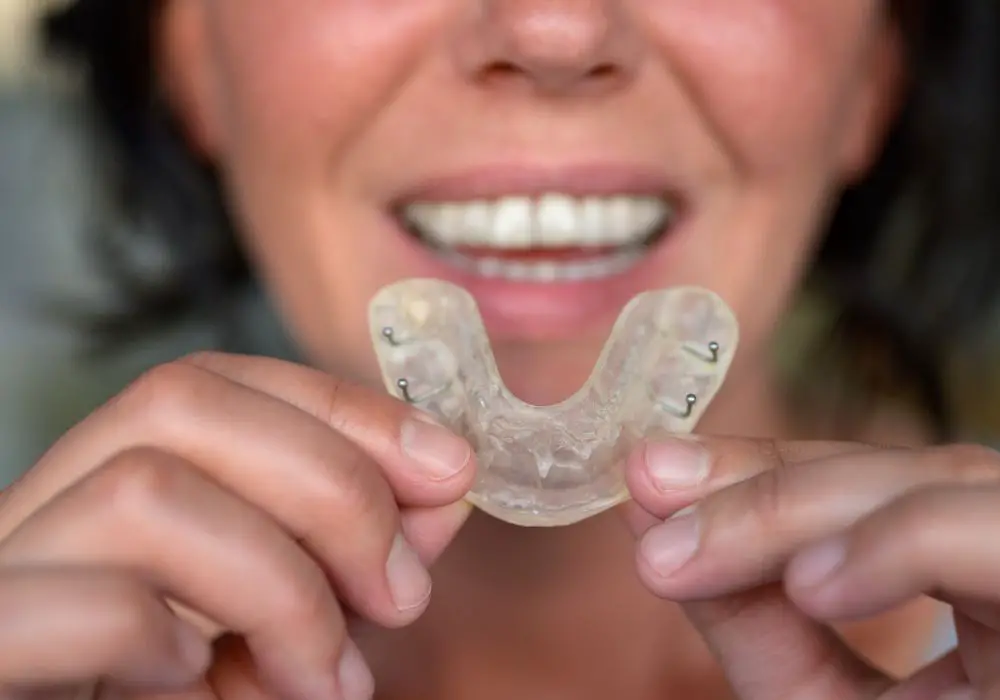
Though not curable, various therapies help minimize bruxism and protect the teeth from further damage:
Dental approaches
- Custom night guards – Also called occlusal splints or mouth guards, these cover the teeth to absorb grinding forces. They are the most common treatment option. Full-arch or smaller night guards are available.
- Botox injections – Botox can temporarily relax the chewing muscles and reduce grinding for 3-4 months before needing re-injection. Some patients experience mild facial weakness.
- Occlusal adjustment – Selectively reshaping the biting surfaces of teeth can distribute forces evenly across the jaw and help reduce strain on certain areas.
Medical treatments
- Muscle relaxants – Drugs like benzodiazepines help relax the jaw muscles and limit nighttime bruxism. Drowsiness, nausea, and dependency issues should be considered.
- Cognitive behavioral therapy (CBT) – CBT aims to modify stress responses, manage anxiety, and change bruxism-related thought patterns through counseling. It may help reduce grinding linked to psychological factors.
- Meditation and yoga – These relaxation practices reduce whole-body stress responses. By lessening anxiety and tension, they may decrease bruxism originating from mental stress.
- CPAP machines – For patients with sleep apnea, using a continuous positive airway pressure (CPAP) device can improve sleep and oxygenation, which might minimize bruxism.
- Medication adjustment – Under a doctor’s guidance, discontinuing or changing medications known to cause bruxism as a side effect may provide relief in some cases.
Patients often try a combination of therapies to control bruxism based on their comfort level and lifestyle factors. Consistency is key – teeth grinding can recur when treatment is stopped. Work closely with your dentist to monitor your symptoms and adjust approaches as needed.
Can bruxism be cured completely?
While treatments can help reduce its effects, there is currently no permanent cure that will completely eliminate bruxism or its underlying causes. That’s because the origins – genetics, brain physiology, emotions, and behaviors – are intrinsic and difficult or impossible to change entirely.
For example, someone born with a hereditary tendency for a misaligned bite or anxious personality cannot readily alter those risk factors. Or someone taking medications that cause bruxism as a side effect may not be able to switch medications due to other health conditions.
Eliminating the root causes would in theory cure bruxism. But realistically, these causes of teeth grinding can only be managed to various degrees, not removed entirely. For now, symptom control via mouth guards, muscle relaxants, therapy, etc. remains the standard approach. More research is still needed to determine if directly modifying genetic, neural, and physiological processes could someday cure bruxism.
Long-term outlook for living with bruxism
Despite not being curable in the traditional sense, bruxism is widely manageable with today’s treatments. By finding an effective management regimen and sticking to it diligently, people can achieve good long-term outcomes. Key tips for living with bruxism include:
- Scheduling regular dental cleanings and exams to monitor for grinding damage
- Consistently wearing a custom night guard each night to protect teeth
- Learning stress management and relaxation techniques to reduce anxiety
- Treating related sleep disorders, reflux, and other medical conditions
- Avoiding dietary triggers like alcohol, caffeine, and chewing gum
- Doing jaw and neck stretches and massages to relieve muscle soreness
- Using mobile apps to become more aware of daytime clenching habits
While bruxism may fluctuate day-to-day, having an effective long-term treatment plan makes living with the condition much smoother. Patience and consistency are vital. With proper management, people with bruxism can maintain excellent dental and overall health.

Frequently Asked Questions
At what point is bruxism considered a disorder?
Occasional teeth grinding during stress is normal. But frequent, intense grinding that damages teeth or causes facial pain is considered a disorder requiring treatment. There is no strict threshold, but if grinding happens most nights or causes symptoms, seek dental help.
Does teeth grinding worsen with age?
The prevalence of bruxism seems to follow an inverted U-shaped curve. It peaks between ages 20-50 during adulthood when job, relationship, and life stresses are greatest, then gradually declines with age as these stresses lessen in later years.
Can Botox provide a permanent cure for teeth grinding?
No, while Botox injections temporarily limit grinding, they do not cure bruxism. Botox paralyzes chewing muscles for 3-4 months but the underlying causes remain. Grinding typically returns once the Botox effects wear off, necessitating repeated injections. For some, Botox offers temporary symptom relief.
Are there any home remedies to cure bruxism?
Unfortunately, there are no proven home remedies that can cure bruxism altogether. Methods like vitamin therapy, herbal supplements, or acupuncture have little evidence of effectiveness. The most reliable approach involves dental treatments like night guards and medical therapies like muscle relaxants as needed.
Can hypnosis or behavioral conditioning permanently stop teeth grinding?
Hypnosis aims to induce a deep relaxed state to reduce stress and curb grinding habits. However, its effects are temporary and variable. The same goes for behavioral conditioning techniques. While these methods may help reduce bruxism to some degree, they do not provide a definitive cure.