For most of us, it’s nearly impossible to drink a hot cup of coffee or bite into a cold ice cream cone without experiencing intense sensations in our teeth. The nerves embedded in the dental pulp allow teeth to respond to temperatures, pressure, pain, and other stimuli. So what happens when those nerves become damaged or diseased? Can they be removed or destroyed to eliminate pain and save the tooth? In this article, we’ll explore the reasons, procedures, effects, risks and answers to common questions about removing dental nerves through root canal treatment.
What are dental nerves and why do we have them?
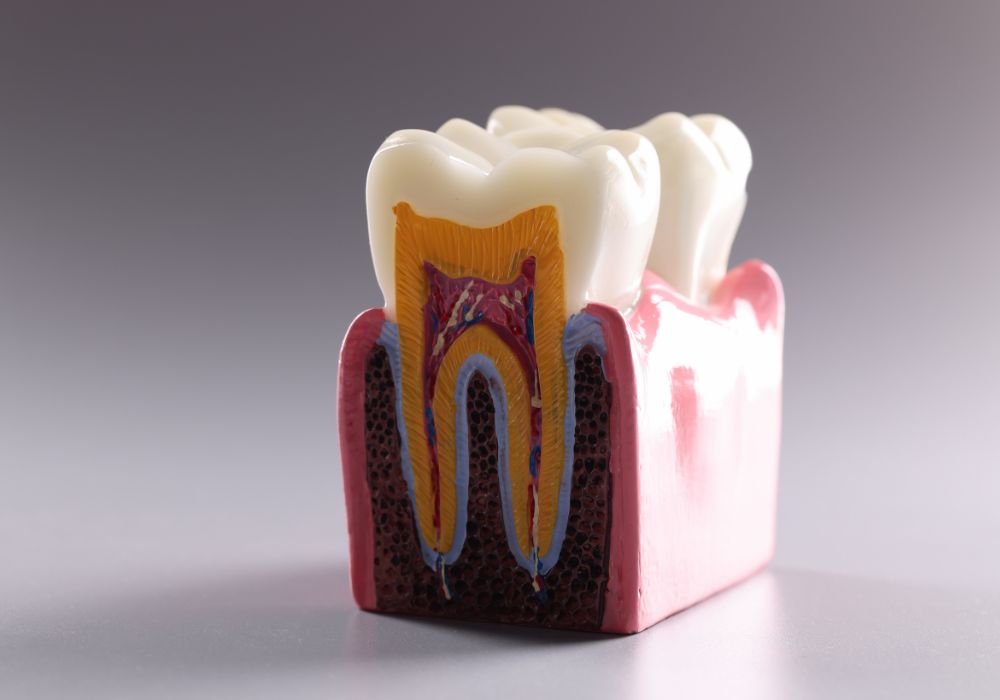
Teeth contain a bundle of nerves and blood vessels in the center called the pulp. The pulp extends from the crown of each tooth down through the roots into the bone. This pulp allows sensations and nutrition to reach the dentin and enamel that make up the main structure of the tooth.
More specifically, the dental pulp contains nerve fibers that connect to the trigeminal nerve, which is the main sensory nerve of the face. Via these connections, sensations including temperature, pressure, vibration, and pain can be detected in each tooth and transmitted to the brain.
Having these nerves embedded in our teeth serves many critical functions:
- They allow us to sense hot, cold, sweet, sour, pressure, and pain from foods contacting our teeth. This gives us important feedback on what is in our mouth.
- They protect teeth by triggering pain when damage or infection occurs. The pain alerts us to seek treatment.
- They provide nutrition and oxygen to keep the inner dentin layer of the tooth alive and healthy.
- They aid in remineralization of enamel after attacks from plaque acids.
- They generate dentin throughout life to maintain the tooth structure.
So in summary, the network of nerves in our teeth is vital for providing sensation, protection, nutrition, and maintaining the tooth’s structural integrity. Losing these nerves impairs the tooth both defensively and nutritionally.
Why would dental nerves need to be removed?
Given the importance of dental nerves, they are only removed or intentionally destroyed in teeth when absolutely necessary. Some common reasons dentists will perform procedures to remove tooth nerves include:
Root canal treatment
This is the most common reason for removing dental nerves. When decay, trauma, or cracking of a tooth allows bacteria to infect the pulp, it becomes painfully inflamed, a condition called pulpitis. Root canals are performed to remove the infected or dead pulp, clean the inside of the tooth, and seal it off to retain the tooth safely.
Preparing a tooth for placement of a crown
Crowns require extensive reshaping and shaving down of a tooth. This can often expose the top portion of pulp tissue inside the tooth. To prevent pain and infection, a root canal may be done to remove the pulp before covering with a crown.
Preventing pain from extensive decay
If a cavity has reached deep into the pulp, the exposed nerves can cause severe pain. Doing a root canal provides pain relief and prevents infection as the decayed area is being repaired.
Cracked or fractured teeth
Cracks and fractures that extend deep into the tooth may sever or damage pulp tissue. A root canal removes the injured pulp to help save the fractured tooth.
Prior to dental implant placement
If a tooth needs to be extracted for replacement with an implant, the dentist may do a root canal first. This prevents pain during extraction and retains bone at the site.
Orthodontic tooth movement
Teeth that are pushed beyond their natural position during braces can compress and damage the pulp. Root canals may be done to allow for further movement without pain.
Teeth grinding or clenching damage
Chronic mechanical force on teeth from grinding or clenching can traumatize the pulp overtime. Removing the nerves provides relief from sensitivity.
So in most cases, the dental nerves are removed when they become infected, inflamed or at high risk of damage. This helps retain the tooth and prevent further pain.
How are nerves taken out of teeth?
The process of removing the nerve tissue from within a tooth is called a root canal treatment or endodontic treatment. It is a common procedure done by general dentists or root canal specialists called endodontists. Here are more details on how it is performed:
1. Local anesthetic
The area around the tooth is numbed by injection of a local anesthetic like lidocaine. This prevents any pain sensation during the procedure. Profound numbness is confirmed before proceeding.
2. Tooth isolation
The tooth undergoing treatment is completely isolated from the rest of the mouth using a rubber sheet called a dental dam. This protects it from saliva and bacteria that can interfere with the procedure.
3. Accessing the pulp chamber
A small opening is drilled through the biting surface of the tooth. This provides access to the pulp chamber in the center of the tooth where the nerves are located.
4. Pulp removal
Fine specialized dental instruments like finger pluggers and tiny files are used to carefully remove all the living and dead pulp tissue from the chamber and root canals. Water irrigation helps flush debris out.
5. Shaping and cleaning canals
The root canals are shaped with files to open them up for decontamination. They are flushed with disinfecting solutions like sodium hypochlorite to kill any lingering bacteria.
6. Final disinfection
The pulp chamber and canals are given a final rinse with EDTA to remove debris and a final disinfecting with chlorhexidine. This ensures bacteria are eradicated.
7. Obturation
The clean and open root canal system is packed tightly with an inert rubber material called gutta percha. This seals the canals closed.
8. Temporary restoration
A temporary filling is placed over the access hole drilled in the tooth to seal it.
This clinical process allows thorough cleaning, disinfecting and sealing of the tooth interior after pulp tissue removal. The tooth can then function without any nerve sensations.
Are there alternative options to removing dental nerves?
Whenever tooth nerves become inflamed, infected, or at risk of damage, dentists first consider any alternative treatment options that may allow preserving the living pulp:
- Pulp capping – If the pulp is just exposed but not yet infected, it may be possible to cover it with a protective dressing that allows it to recover.
- Pulpotomy – In some cases, only the inflamed pulp in the chamber is removed while the canal pulp remains protected and vital.
- Medications – Antibiotics, steroids, and fluoride agents may resolve mild inflammation and allow the pulp to heal.
- Bonding and fillings – Small exposed areas may be sealed with bonding and strips to re-cover the pulp.
However, if the pulp tissue is dying or severely infected, a full root canal is likely necessary to remove it entirely and prevent further issues. Alternatives carry a higher risk of failure.
An experienced dentist will be able to determine if less invasive options are appropriate on a case by case basis. But root canal therapy tends to offer the most predictable and effective resolution when the nerves are too far gone.
What is it like living without sensation in the treated tooth?
Teeth that have undergone root canal treatment and removal of their nerves function quite differently than natural teeth with vital pulp. Here are the main differences patients notice:
- No pain – Pain from inflammation, infection, or injury is completely eliminated. This provides relief in previously painful teeth. However, pain can still occur from pressure on other structures like the ligament.
- No thermal sensitivity – Hot, cold, or sweet foods and drinks will not trigger any sensitivity or discomfort in the tooth. It becomes unable to sense temperatures.
- No tactile sensation – Touch, pressure, vibration, texture, etc can no longer be perceived by the tooth. Things like brushing feel different.
- Feels hollow – With the inner pulp gone, the tooth may feel abnormally empty or hollow, especially when biting down.
- Deadened feeling – Overall the tooth feels deadened without the vital sensations from the nerves. Adjacent teeth may feel more intense.
- Increased brittleness – The treated tooth becomes much more brittle and prone to cracking without the pulp tissue inside.
So lack of sensations takes adjustment, but the tooth can still perform functions like biting and chewing. Patients must be diligent about self-examination since the tooth’s defenses are impaired. Using a crown helps strengthen and protect the nerve-free tooth.
Are there any risks or complications?
While routine, root canal treatments do come with some inherent risks and potential complications to be aware of:
- Treatment failure – Root canals fail in 5-10% of cases due to persistent or recurrent infection. This may require re-treatment or extraction.
- Crown failure – Without a crown, the root canal tooth is prone to fracture. Cracked crowns also raise infection risks requiring treatment.
- Tooth fracture – The increased brittleness makes root canal teeth more likely to crack or break over time.
- Reinfection – If sealing is incomplete or degrades, bacteria can reinfect the canal requiring additional treatment.
- Adjacent pain – Nerves in adjacent teeth may become hypersensitive or painful.
- Nerve injury – Lingering numbness, pain, or tingling can occur if nerves of the jaw joint or face are damaged during treatment.
- Extraction – Severe complications may ultimately require the tooth to still be pulled to resolve issues.
With proper technique, restoration, and aftercare, risks remain low with root canals. But they do fundamentally change and weaken the tooth for life. Making an informed decision with your dentist helps ensure the best outcome.
Frequently Asked Questions
Can a root canal treated tooth still cause pain?
After full healing, a root canal treated tooth should not cause pain. Removing the infected nerve tissue eliminates pain from pulpitis. However, some causes of discomfort can still occur:
- Infection – A failed root canal may have persistent bacteria causing soreness. Additional treatment is needed.
- Pressure on ligament – Biting hard things may cause aching from the periodontal ligament.
- Cracks – Undetected cracks in the tooth can cause pain with chewing.
- Restoration issues – Problems with dental work on the tooth may cause discomfort.
So while a successfully healed root canal removes pulp pain, other sources of pain are still possible over time.
How permanent is a root canal treatment?
With proper disinfection, obturation, and a good coronal restoration, a root canal treated tooth can potentially last a lifetime. However, the tooth does become more brittle so bites on hard foods or trauma raise the risk of complications like reinfection or fracture. Ongoing care and avoidance of excessive biting forces help improve the longevity.
Do you need a crown after a root canal?
Placing a crown over a root canal treated tooth is highly recommended for optimal longevity and function. The crown protects the tooth from fractures, further decay, and helps prevent reinfection of the canal. Without a crown, failure rates are higher. Most dentists advise getting a crown done within 1-2 months after the root canal.
How long does a tooth last after root canal?
With optimal care and restoration, the average survival time of a root canal tooth is often 10 years or longer. Proper technique by an experienced endodontist can maximize success rates. However, harsh oral conditions or lack of protective restoration lowers average survival times. Continued care and maintenance helps root canal treated teeth last as long as possible.
Can a failed root canal be redone?
If a root canal fails due to persistent infection or reinfection, retreatment may be attempted to save the tooth. The canals are reopened, cleaned, disinfected, and re-sealed. However, the prognosis depends on the level of damage. Heavily infected teeth may still require extraction if beyond saving.
Conclusion
While dental nerves provide vital protective sensations, severe inflammations or infections can necessitate their surgical removal through root canal treatment. This procedure retains the tooth and eliminates pain. Patients must adjust to lack of sensations from the treated tooth and take precautions to prevent complications. Working closely with your endodontist and getting proper restorations can help maximize the longevity and function of teeth after root canal.