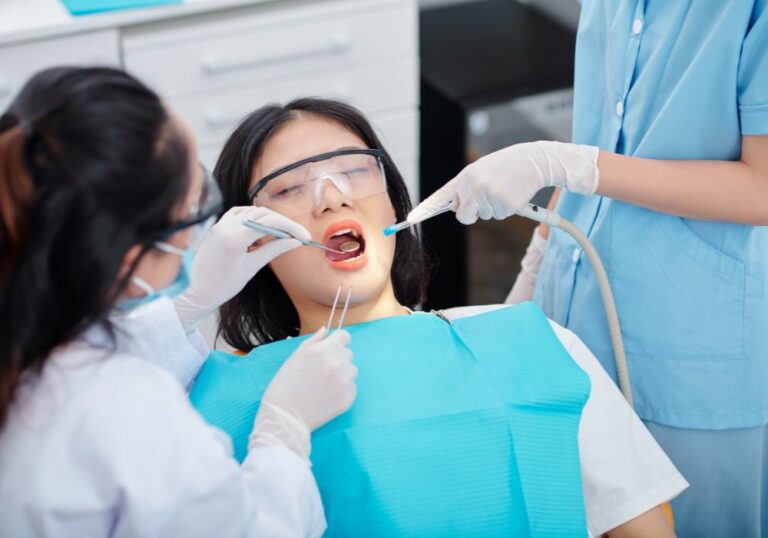
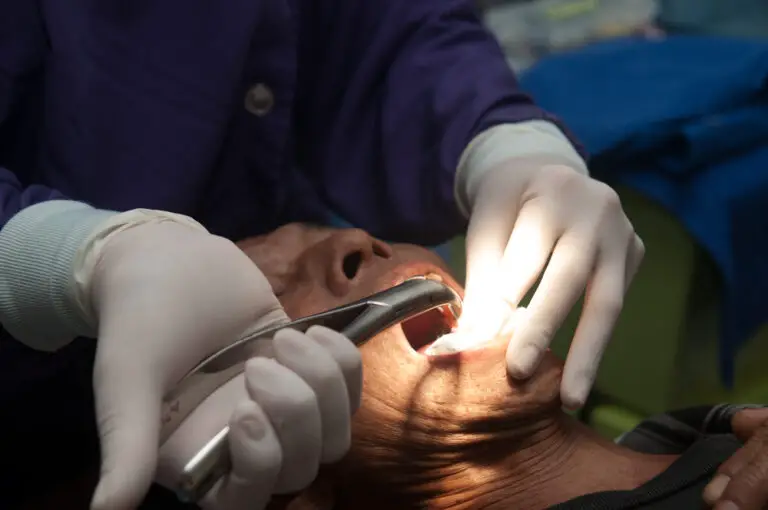
Eye swelling, also known as periorbital edema, is a condition characterized by puffiness or swelling around the eyes. It can involve one or both eyes. While there are many potential causes, some research has found connections between poor dental health and eye swelling.
This article provides an in-depth examination of the possible link between dental issues and periorbital edema. It covers the evidence, underlying mechanisms, symptoms, diagnosis, treatment, prevention, and complications in detail.
Evidence linking dental problems and eye swelling
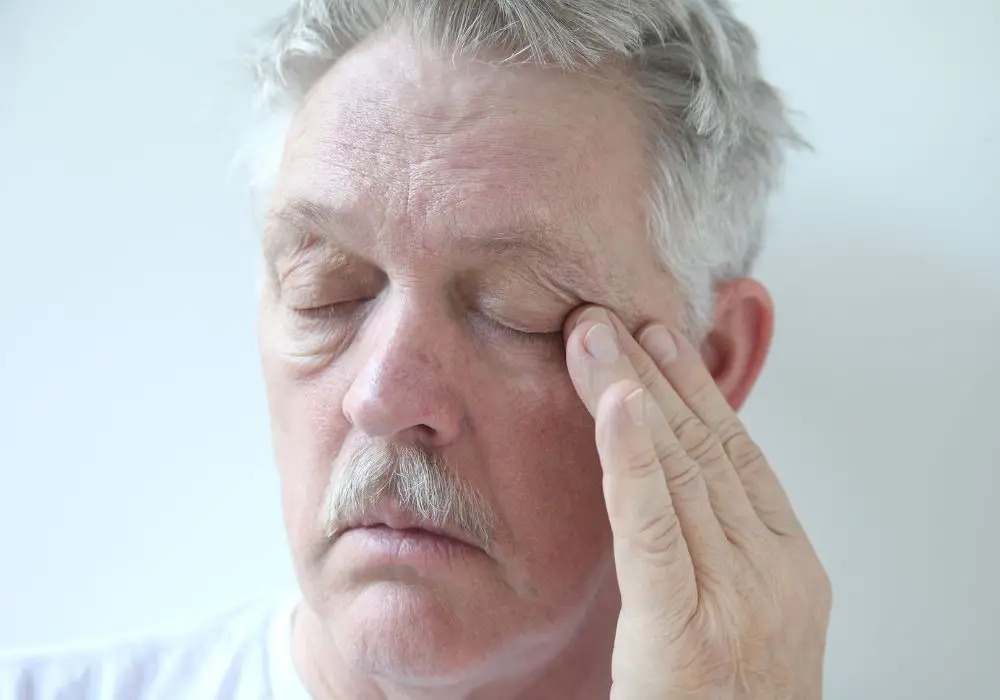
Though limited, there are some studies demonstrating an association between tooth infections and swelling around the eyes:
- A 2011 case report described severe facial and periorbital edema in a 9-year old girl. Her symptoms were ultimately traced to an abscess of the primary lower right first molar tooth. CT imaging showed inflammation spreading from theDecayed tooth root area into the surrounding bone and tissue. The swelling and symptoms entirely resolved after the tooth was extracted.
- A 2013 study examined 51 patients hospitalized for swelling of the face and eyes (periorbital edema). They found that prior root canal treatments, chronic periapical dental abscesses around tooth roots, and periodontal disease were significantly associated with the swelling. 82% of the eye swelling patients had previous endodontically-treated teeth and signs of infection around the tooth roots.
- A case report in 2013 highlighted two patients who came to the ER with recurrent unilateral periocular swelling and were found to have odontogenic infections. One had an abscess below a decayed molar and the other had a periodontal abscess. After the infected teeth were treated, the swelling and symptoms resolved.
- Some studies suggest around 4-10% of facial swelling cases seen in emergency departments originate from odontogenic infections like tooth abscesses. Periorbital edema is commonly associated.
While limited, these studies demonstrate odontogenic infections like dental abscesses do seem capable of spreading and causing facial and eye swelling for some patients. More rigorous research is still needed to fully establish correlation.
Possible mechanisms explaining the linkage
Researchers have proposed three key mechanisms to explain how dental issues could potentially lead to periorbital swelling:
1. Spread of infection from tooth to facial regions
Abscesses and infections around the tooth root can spread beyond the initial site as swelling and inflammation enlarge.
- Periapical abscesses – These abscesses occur at the root tip of the tooth, usually due to untreated tooth decay or failed root canal treatment. The collection of pus and inflammation can burrow into the surrounding jawbone.
- Periodontal abscesses – These abscesses involve the gums and tissues surrounding the tooth root. They can spread into bone as well.
As the infection from dental abscesses expands, it can rarely travel up through the bones around the eye and into adjacent facial soft tissue. This enables oral bacteria from the original dental source to seed areas around the eye, causing swelling and inflammation.
2. Spread of infection into maxillary sinus
The maxillary sinuses are located above the upper teeth and drain into the nasal cavity.
- Odontogenic infections from upper back molar and premolar teeth can sometimes spread directly into the maxillary sinuses. This results in sinusitis.
- Pressure and inflammation in the sinuses caused by infection and pus could contribute to swelling and pain around the eyes.
However, more research is needed to determine the frequency of sinus involvement in cases of odontogenic periorbital swelling.
3. Trigeminal nerve inflammation
The trigeminal nerve supplies sensation to the face as well as the teeth.
- It is hypothesized that dental infections cause inflammation and irritation of the branches of the trigeminal nerve. This could spread to the ophthalmic division, causing periorbital edema and pain.
However, there is lack of sufficient evidence to confirm this mechanism at this time.
While these explanations are biologically plausible, more research is still needed to fully understand the exact mechanisms in cases of eye swelling linked to dental disease.
Associated symptoms
When a dental infection does spread and cause periorbital swelling, additional symptoms may accompany the puffy eyes. These can include:
- Swelling and inflammation on one side around the eyelid and eye area, or sometimes on both sides
- Eye pain, especially pain with eye movement
- Redness of the conjunctiva and around the eyelids
- Sensation of pressure around the eyeball and forehead
- Headache centered around the affected side
- Toothache or pain from the problematic tooth with dental disease
- General swelling and edema on the same side of the face as the infected tooth
- Fatigue and malaise
- Fever in some cases
- Vision changes if swelling is severe. Usually temporary blurriness or double vision.
The eye swelling tends to come on relatively quickly over several hours to days if due to a spreading dental infection. Pain around the eye may indicate a secondary infection as well. Prompt evaluation is recommended for any unexplained eye swelling.
Is a dental infection causing eye swelling a dental emergency?

Yes, if you develop any type of facial or periorbital swelling along with tooth pain or dental symptoms, it should be treated as a dental emergency.
Here’s why immediate dentist evaluation and treatment is crucial:
- It allows early treatment to stop the infection from worsening and spreading further in the tissues around the eyes where it can do more damage.
- It helps avoid potentially serious complications that can arise from infection around the eye and sinuses. Vision loss is possible in rare cases.
- It relieves pain and swelling more quickly.
- It helps protect your oral health by treating the source of infection. Ideally the problematic tooth can be saved with prompt care.
- Antibiotics and dental treatment work together to eliminate the infection at the root cause – the tooth. This allows the eye swelling to steadily resolve.
Do not wait with a suspected dental infection, as urgent assessment and care is important for the best outcome.
Diagnosing the cause of eye swelling
When a patient presents with periorbital swelling, physicians will conduct an examination and take the person’s history to try to identify potential causes:
- They will look for signs of infection and assess eye movements and vision.
- Lab tests may be ordered to check for inflammation and infection.
- Imaging like CT scans can look for eye or sinus abnormalities.
- The patient will be asked about any recent illnesses, injuries, insect bites, and other symptoms that could explain the swelling.
If there are any dental symptoms like tooth pain or sensitivity, prompt referral to a dentist is recommended. A comprehensive dental examination can help pinpoint if a tooth issue is contributing to the eye swelling.
As part of this exam, the dentist may:
- Evaluate the teeth, gums, bite, and oral soft tissues looking for signs of infection like swelling, redness, or pus.
- Order x-rays like periapical or panoramic views to visualize the tooth roots and surrounding bone. Signs of infection or abscesses here can indicate an odontogenic source.
- Assess tooth pulp vitality. Teeth with diseased or infected pulp may not respond normally to cold/heat tests.
- Tap gently on teeth to check for pain, which could signal infection.
- Referral to an endodontist may be needed for advanced testing of tooth pulp status.
- Examine previous dental work like root canals or extractions that appear associated with swelling. Failed endodontic treatments can cause abscess.
With this dental detective work, the source of infection can often be traced to a particular tooth requiring treatment. The dentist will communicate findings and coordinate care with the patient’s other providers.
Treatment approach
Once a tooth issue is identified as the likely source of swelling around the eyes, treatment focuses on:
- Eliminating the odontogenic infection
- Allowing the periorbital swelling and inflammation to steadily subside
- Preventing further spread of infection toward the eyes or sinus
- Restoring long-term dental health
Typical aspects of treatment include:
-
Antibiotics – Prescription of broad spectrum antibiotics targeting common oral bacterial pathogens. This helps control dissemination of infection to the eyes and face. Antibiotics may be given intravenously initially if infection is severe.
-
Dental procedures – The dentist will perform needed dental procedures on the infected tooth/teeth to address the source of infection. This could involve:
- Root canal treatment – This can remove infected dental pulp and save a tooth with irreversible pulpitis or a chronic apical abscess.
- Tooth extraction – Unrestorable teeth may need extraction if decay is too advanced or periodontal disease too severe. This eliminates the infection.
- Draining abscesses – Incision and drainage of any accessible periapical or periodontal abscesses around tooth roots.
- Further procedures like apicoectomies may be considered if needed.
-
Warm compresses – The patient can be instructed to apply warm, damp washcloths or compresses to the affected eye. This helps improve drainage and circulation to minimize swelling and discomfort.
-
Medications – Oral NSAIDs, analgesics and corticosteroids may be prescribed to reduce inflammation and eye pain. Antibiotic eye drops are used if conjunctivitis is present.
-
Sinus treatment – If sinuses are involved, medications like nasal steroids, decongestants, and sinus rinses may be recommended. In some severe cases of odontogenic sinusitis, surgery may be required.
With the infection-source tooth addressed, the periorbital swelling can steadily resolve over several days to a week as long as treatment is followed.
Potential complications
Prompt and appropriate treatment helps avoid serious complications and long term issues from odontogenic periorbital infections. However, potential complications to monitor include:
- Vision loss or changes – Compression on the optic nerve from severe swelling or infection can cause temporary or permanent vision loss or deficits. However, this is very rare with early treatment. Mild temporary vision changes like blurriness are more common.
- Worsening infection – If left untreated, the infection could spread into deeper facial planes, the sinuses, or cranial spaces. This could have life-threatening consequences like meningitis, cavernous sinus thrombosis, or brain abscess. Aggressive IV antibiotics and surgery may be required.
- Orbital abscess or cellulitis – The eye infection extends into deeper orbital tissues, requiring intravenous antibiotics and possible surgical drainage.
- Chronic sinusitis – A sinus infection persists and becomes chronic due to underlying anatomical defects. This may call for sinus surgery like Caldwell-Luc operation.
- Tooth loss – The infected tooth cannot be salvaged and is lost, requiring restoration with bridges, implants, etc.
While quite rare with timely treatment, continued monitoring and follow up is prudent given potential complications if swelling worsens.
Prevention tips

You can help minimize the risk of advanced dental infections that could spread and cause periorbital edema by:
- Brushing properly twice a day and flossing once daily. Good oral hygiene helps prevent dental disease.
- Seeing your dentist for professional cleanings and checkups every 6 months. Allows early detection and treatment of issues.
- Getting cavities filled quickly before they progress. Avoid having severely decayed teeth needing root canals or extraction.
- Obtaining prompt care for any tooth pain, swelling of the gums, or dental sensitivities. Don’t delay with possible infections.
- Completing recommended dental work like root canals, tooth extractions, or gum disease treatment on schedule.
- Using daily oral rinses if susceptible to gingivitis or abscesses.
With good oral health habits and regular dental care, you can lower chances of dental infections occurring and spreading. Seek early attention for dental symptoms and comply with all prescribed treatment.
Conclusion
While the data is still limited, there appears to be a connection between some severe tooth infections and the development of swelling around the eyes (periorbital edema). The most plausible mechanisms involve the spread of bacteria and inflammation from more advanced infections of the teeth, gums or tooth roots into the surrounding facial region near the eye.
In most cases, swelling also affects other facial areas on the same side as the problematic tooth. Additional symptoms like eye pain, redness, headache and vision changes can occur as well. Prompt dental and medical treatment is key to resolve the infection and allow the swelling to subside without complication. While concerning, odontogenic eye swelling often carries a good prognosis when properly managed. Prevention involves maintaining dental health with good oral hygiene habits and regular professional care.