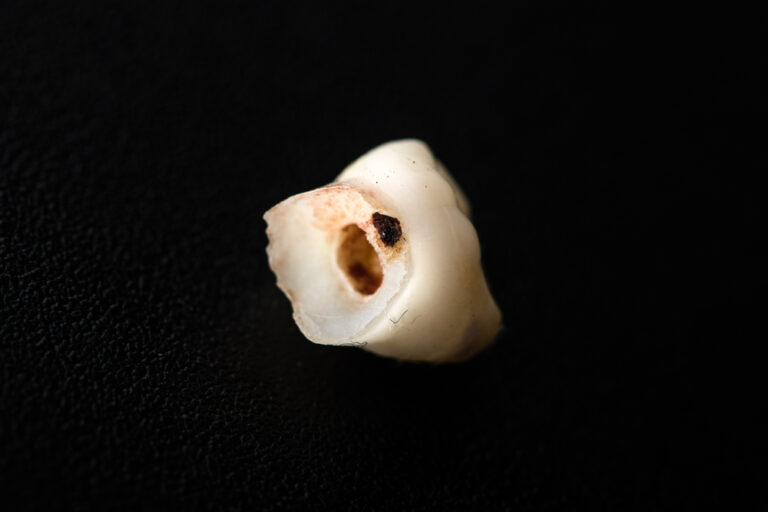
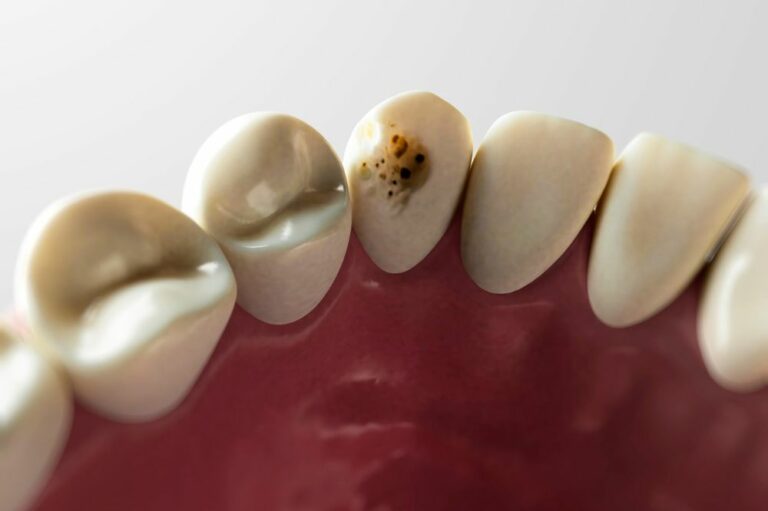
Oral health is extremely important for your overall health and wellbeing. Poor oral hygiene and untreated dental issues like cavities, gum disease, and tooth decay can lead to infections not only in your mouth but also in the rest of your body.
How bad oral health can spread infection?
Your mouth contains millions of bacteria, some helpful and some harmful. When your oral hygiene is poor, harmful bacteria grows and spreads into your bloodstream through:
- Open wounds from tooth decay: Cavities allow bacteria to enter inside the tooth and infect the root and pulp. The pulp contains blood vessels and nerves that provide a pathway for bacteria to enter your bloodstream and spread infection elsewhere in the body. As tooth decay reaches the inner layers of your teeth, it forms a pocket that harbors bacteria.
- Gum disease: Gum disease, also called periodontal disease, causes your gums to pull away from your teeth. This creates empty spaces or pockets that become filled with bacteria. Gum disease also leads to bleeding gums that provide an easy entry point for bacteria to enter your bloodstream.
- Ill-fitting crowns or dentures: Any damage to the soft tissues in your mouth from poorly fitted dental appliances like dentures, crowns, or retainers can allow bacteria to invade and spread through your blood vessels. Cuts or sores allow the bacteria to bypass the body’s natural protective barriers.
Once harmful oral bacteria enters the bloodstream through these pathways, it can travel to other parts of your body and cause infections. The heart, lungs, joints, and bones are most commonly affected by spread of oral bacteria.
How common are infections from poor oral health?
- An estimated 47% of adults aged 30 years or older show signs of gum disease like gingivitis or periodontitis. Gum disease is a very common pathway for oral bacteria to enter the body.
- Around 64 million Americans have untreated tooth decay, which allows cavities to worsen over time and bacteria to thrive inside them.
- Dental procedures like tooth extractions, root canals, dental implant placement, and deep cleanings also allow bacteria to spread into bloodstream and surrounding tissues. Proper sterilization of dental equipment and antibiotics help prevent infections from such invasive procedures.
- Oral bacteria is found in dangerously high levels in people who have a history of recent heart attacks, unstable angina, or stroke. This shows the prevalence of how oral bacteria can spread to the cardiovascular system.
- One study showed that 86% of angina and heart attack patients had oral streptococci bacteria present in their heart valves and artery plaques.
- Up to 20% of total bacteria present in the lungs of pneumonia patients matches the bacteria from dental plaque samples. This suggests spread of oral bacteria to lungs is common.
Major types of infections caused by poor oral health
Here are some common and serious infections poor oral health can cause in the body when harmful bacteria spreads beyond the mouth:
Endocarditis
- What is it? Endocarditis is a rare but life-threatening infection of the inner lining of the heart or the heart valves caused by bacteria spreading from the mouth into the blood. Although uncommon, its mortality rate is high even with treatment.
- Who is at risk? People who already have damaged or artificial heart valves, congenital heart defects, artificial joint implants, or a past history of endocarditis are at highest risk. Intravenous drug users who share needles are also at increased risk of endocarditis.
- Effects: Symptoms include fever, fatigue, shortness of breath, heart murmurs or palpitations. Small clumps of bacteria can get deposited on heart valves and damage them severely. If untreated, the infection can spread rapidly and cause heart failure, stroke, or prove fatal.
- Link to oral health: Bacteria from gum disease, tooth decay/abscesses, or even routine dental procedures can enter the bloodstream and make their way to heart valves, especially if already damaged. Maintaining good oral hygiene and taking antibiotics before invasive dental procedures reduces the chances of bacteria spread to the heart.
Respiratory infections
- What is it? Bacterial infections like pneumonia, acute bronchitis, chronic obstructive pulmonary disease (COPD) exacerbations, and lung abscesses caused by microbes that spread from the oral cavity to the lungs.
- Who is at risk? Elderly people, hospitalized or chronically ill patients, those with weakened immune systems, patients on ventilators are most at risk. Patients undergoing anesthesia for dental procedures can also inhale bacteria into lungs.
- Effects: Effects include coughing, excessive phlegm, wheezing, fever, chest pain, breathlessness. It can prove fatal in high-risk people.
- Link to oral health: Harmful bacteria from the mouth can be inhaled or aspirated into the lungs or spreads through the bloodstream. Maintaining good oral hygiene helps reduce the overall bacterial load in the mouth. Controlling coughing and rinsing mouth before dental procedures reduces aspiration risk.
Joint infections
- What is it? Bacterial joint infections like infectious arthritis are caused by spread of oral bacteria to hip, knee, or other joints through blood. This is especially likely in those who already have inflammatory joint diseases.
- Who is at risk? Those with pre-existing joint conditions like arthritis, rheumatoid arthritis, joint replacements or injuries, or orthopedic implants are most prone to these infections.
- Effects: Symptoms include severe joint pain, stiffness, swelling, heat, redness, drainage, and difficulty moving the joint. It can permanently damage cartilage and bone if bacteria is not cleared promptly.
- Link to oral health: Multiple studies show people with gum disease have higher presence of periodontal bacteria traced in their synovial joint fluid. Treating gum disease reduces the bacterial load and helps lower chances of it spreading to joints.
Diabetes complications
- What is it? Poor oral health worsens diabetes outcomes. Periodontal bacteria can increase inflammation and insulin resistance. Diabetes reduces immunity and makes gum disease worse.
- Who is at risk? Those with poorly controlled diabetes are more prone to severe oral infections. Gum disease is more common and worsens faster in diabetics.
- Effects: Worse glycemic control, higher rates of kidney disease, heart disease, and stroke in diabetics with periodontitis. Pre-term birth risk higher in women.
- Link to oral health: Managing oral health is important part of overall diabetes care. Treating gum disease and establishing oral hygiene improves glycemic control in diabetics.
How to prevent infections from poor oral health?

You can take certain steps to maintain good oral hygiene and prevent the spread of harmful bacteria from the mouth to the body:
- Brush teeth twice daily using proper technique – Place your toothbrush at a 45-degree angle towards your gums. Gently move it in circular motions to clean all surfaces of your teeth. Use a soft or medium bristle toothbrush. Be sure to reach all areas including behind molars, bottom incisors, and along the gumline. Use a fluoridated toothpaste. Brush for 2 minutes each time.
- Floss at least once daily – Use proper flossing technique to remove any food debris and plaque between teeth and below the gumline. Flossing helps remove bacteria that your toothbrush cannot reach.
- Use antiseptic mouthwash – Mouthwash reduces the overall bacteria load in the mouth and reaches areas your brush cannot. Use an alcohol-free mouthwash at least twice a day.
- Visit dentist every 6 months for dental cleanings and checkups – Professional cleanings remove hardened tartar above and below the gumline that you cannot remove by regular brushing and flossing. See your dentist promptly if you notice any oral health issues.
- Get cavities, tooth decay, and gum disease treated promptly – This prevents further spread of bacteria into inner layers of your teeth and destroys existing infections. Monitor children carefully for tooth decay.
- Ensure proper fit of crowns, dentures, retainers – Ill-fitting dental appliances can damage your gums and oral tissues. This allows bacteria easy entry into your tissues and bloodstream.
- Take antibiotics before invasive dental procedures – Your dentist may prescribe antibiotics before procedures like dental implants, root canals, or tooth extractions especially if you have any heart conditions. This prevents bacteria being released into the bloodstream during the procedure.
Here is a table summarizing tips to prevent infections from poor oral health:
| Prevention Tips | Details |
|---|---|
| Brush properly twice daily | Use fluoridated toothpaste, gentle circular motion to clean all surfaces |
| Floss once daily | Reach under the gumline to remove debris between teeth |
| Use antiseptic mouthwash | Reduces overall oral bacteria load |
| Regular dental visits | Cleanings every 6 months, address any issues promptly |
| Treat dental issues early | Fix cavities, infections before they worsen |
| Ensure proper fit of dental appliances | Ill-fitting dentures, retainers can damage tissues |
| Antibiotics before invasive procedures | Take antibiotics as prescribed before dental surgery |
| Don’t smoke/use tobacco | Increases risk of gum disease, oral cancer |
| Limit sugary foods/drinks | Reduces tooth decay risk |
| Eat calcium/vitamin C rich diet | Strengthens teeth and immunity against infections |
FAQ on oral health and infections
Here are answers to some frequently asked questions about how poor oral health can cause infections in the body:
Q: Which medical conditions increase the risk of infections spreading from the mouth?
A: Conditions like diabetes, rheumatoid arthritis, HIV/AIDS, cancer treatments, organ transplants and chemotherapy increase susceptibility to oral infections spreading in the body. People with artificial joints/valves, or any condition that compromises immunity are at higher risk.
Q: Are root canals safe? Can they spread infections?
A: Modern root canal treatments when done properly under sterile conditions are very safe. Dentists thoroughly disinfect the canal, use antibiotics, and seal it off with filling material to prevent any infection spread.
Q: What daily oral health habits help prevent infections in the body?
A: Brushing teeth and tongue twice daily, flossing once daily, using antiseptic mouthwash, eating a balanced diet low in sugars, avoiding smoking/tobacco, staying hydrated, and regular dental cleanings and checkups help maintain good oral hygiene.
Q: How long can oral bacteria last in bloodstream to cause infections elsewhere?
A: Harmful oral bacteria can typically survive in the bloodstream for 10-30 minutes after entering through a cut, open cavity, or gum disease. The quicker it reaches target areas like heart valves, the higher the risk of localized infection. Prompt treatment helps clear bacteria before permanent damage.
Q: Should I take antibiotics before every dental procedure?
A: Antibiotics are only recommended before certain invasive dental procedures like dental implant placement, root canals, or if you already have a high-risk cardiac condition. For routine fillings or cleanings they are not required. Check with your dentist about your specific health status.
Good oral health is essential to prevent bacterial infections from spreading from the mouth to the entire body. See your dentist regularly every 6 months and adopt daily home oral hygiene practices like brushing, flossing, and antiseptic mouthwash use. Take prompt care of any dental issues like abscesses, gum disease or ill-fitting dental appliances to protect your overall health.