Seeing blood when brushing, flossing, or eating can be upsetting. While minor bleeding can occur occasionally, frequent or excessive bleeding indicates an underlying dental health problem requiring prompt attention.
Gum Disease
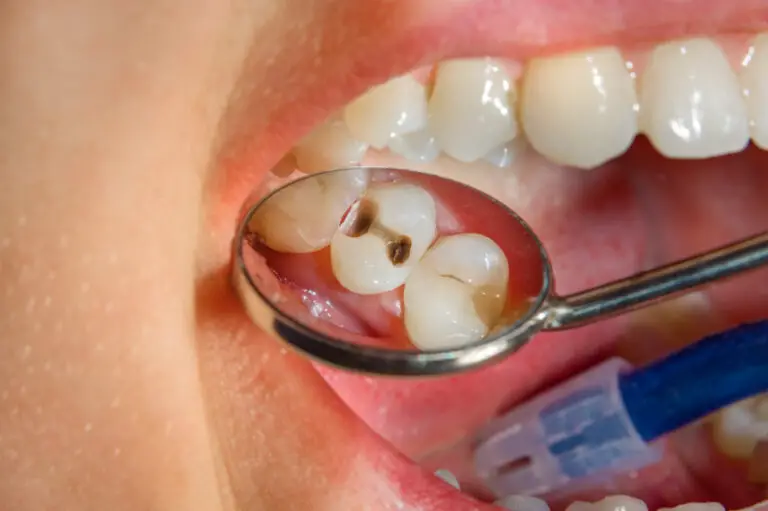
Gum disease, also called periodontal disease, is the most common reason for bleeding gums and teeth. It occurs when plaque – a sticky film containing bacteria – builds up on teeth. The plaque causes inflammation, irritation, and infections in gum tissue that make it easy to bleed.
There are two stages of gum disease:
Gingivitis
This early stage causes red, swollen, and tender gums that are prone to bleeding with brushing and flossing. Other symptoms include bad breath and pus discharge from gums. At this stage, gum disease is reversible with professional treatment and improved oral hygiene.
Periodontitis
The later stage of gum disease where inflammation has spread deeper through gum tissues and bone structure supporting teeth. Symptoms include:
- Receding gums with increased tooth exposure
- Pockets of infection between gums and teeth
- Loose or shifting teeth
- Tooth sensitivity and pain
- Persistent bad breath
- Pus discharge
- Changes to bite alignment
Without treatment, periodontitis causes irreversible damage including permanent tooth loss. The treatments focus on halting disease progression.
Causes and Risk Factors
There are numerous risk factors that can contribute to developing gum disease:
- Poor oral hygiene – Inadequate brushing and flossing allows plaque to accumulate and harden into tartar. This irritates gums and they become inflamed and prone to bleed.
- Genetics – Some people are more susceptible to gum disease due to genetic factors.
- Smoking/tobacco use – Chemicals in tobacco products increase gum disease risk.
- Stress – High stress levels increase cortisol which weakens immune health.
- Hormonal changes – Such as during puberty, menstruation, pregnancy, and menopause due to their effect on oral tissues.
- Diabetes – Less ability to fight infections means greater risk.
- Leukemia and cancer – Cancer treatments can increase risks.
- HIV/AIDS – The infection itself and medications used to treat it.
- Crooked teeth – Harder to keep teeth clean when crowded or misaligned.
- Medications – Some drugs like oral contraceptives, calcium channel blockers, anti-depressants and more.
- Older age – Gum health deteriorates as we age.
Gum Disease Treatment
Treating gum disease aims to reduce plaque buildup and manage infection:
- Professional dental cleaning – To remove hardened plaque and tartar from teeth and gumline. Usually needed every 6 months.
- Scaling and root planing – Cleans deeper under gums and smooths roots to remove bacteria and tartar.
- Medicated mouth rinses – Prescription antiseptic rinses to kill bacteria and reduce inflammation. Chlorhexidine is commonly used.
- Oral antibiotics – May be prescribed short term if infections are extensive.
- Flap surgery – Can access deeper gum tissues and bone to clear out plaque and tartar.
- Bone and tissue grafts – Help regenerate lost bone and gum tissue damage from periodontitis.
- Laser therapy – Laser light can remove infected gum tissue and improve healing.
- At home care – Includes brushing, flossing, rinsing daily to control bacteria between dental visits.
The goal is to treat gum disease in early stages before major bone and tooth loss occur. Even in late stages, progression can be halted with aggressive plaque removal and infection control.
Tooth Trauma

Injuries and trauma to the teeth and gums often cause bleeding as well. Examples include:
- Cracked teeth – Cracks expose inner tooth layers and nerves that bleed easily when irritated.
- Chipped teeth – Breaking off chunks of tooth can lead to pain and bleeding.
- Sports injuries – Blows to the mouth from sports often cause bleeding cuts. Prompt dental treatment is needed.
- Accidental biting – Chewing too aggressively can bite the cheek or tongue. The bleeding wounds are painful.
- Tooth grinding – Aggressive teeth grinding (bruxism) can damage enamel and irritate gums to bleed.
These types of dental injuries must be treated quickly. Crowns, fillings, or tooth extractions may be necessary depending on severity. Wearing mouthguards during sports can help prevent trauma.
Tooth Sensitivity
Sensitive teeth are also prone to bleeding when exposed to hot, cold, sweet foods, brushing, flossing or even air. Common causes of sensitivity include:
- Receding gums – With age, gums recede and expose delicate tooth roots easily irritated.
- Gum disease – Inflamed gums are hypersensitive to touch and pressure.
- Cracked teeth – Fractures in enamel expose nerves and make teeth extremely sensitive.
- Worn enamel – Acidic foods and aggressive brushing wears down enamel over time.
- Tooth grinding – Grinding and clenching wears down enamel and strains gums.
Treating underlying causes of sensitivity like gum disease, worn enamel, and cracks can reduce bleeding. Dentists also recommend desensitizing toothpaste, gentle brushing, fluoride treatments, and dental sealants to help manage sensitivity.
When to See a Dentist?
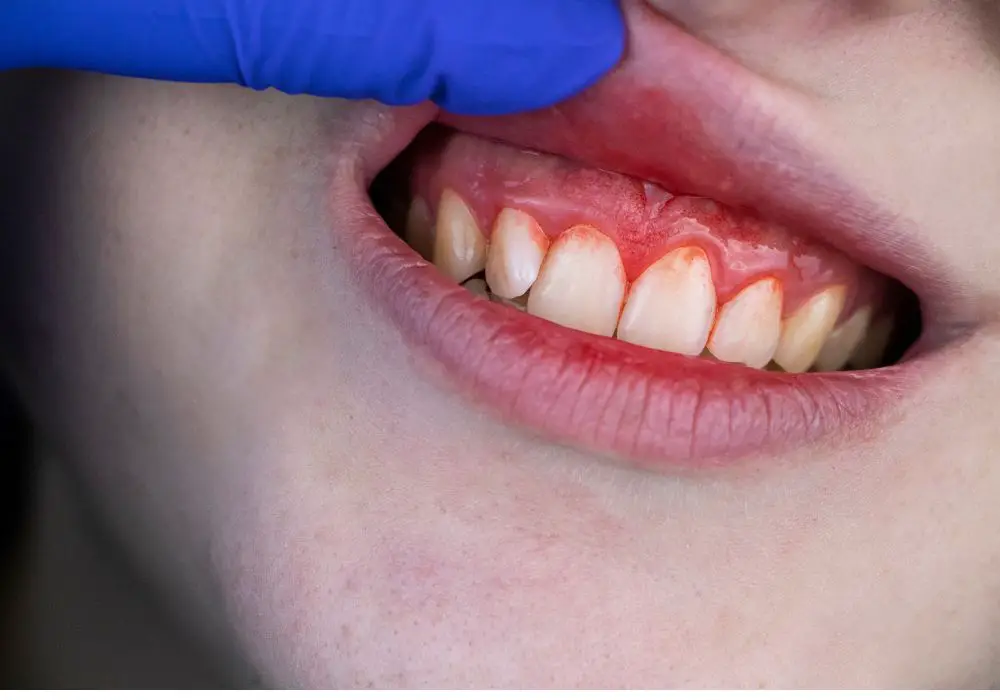
It’s crucial to get any persistent bleeding evaluated promptly by a dentist. Bleeding from gums or teeth is not normal. See a dentist if you notice:
- Bleeding when brushing or flossing on a regular basis
- Frequent bleeding from hot, cold or sweet foods/drinks
- Spontaneous bleeding without any stimulation
- Sudden onset of tooth or gum pain
- Red, swollen, or inflamed gums
- Loose teeth
- Persistent bad breath and pus discharge from gums
Bleeding related to gum disease will only worsen without professional treatment. Trauma and injury also require immediate dental attention to avoid complications like infections and tooth loss. It’s essential to see a dentist right away for bleeding teeth.
Prevention Tips
Practicing good oral hygiene and having regular dental cleanings can help prevent excessive bleeding. Try these tips:
- Brush teeth gently 2x daily with soft bristle brush. Avoid aggressive scrubbing.
- Floss teeth once daily to remove plaque from gumline.
- Use antiseptic mouth rinses to reduce plaque bacteria.
- Have professional cleanings every 6 months.
- Don’t smoke or use tobacco products.
- Drink water after eating and drinking to rinse away food debris.
- Limit sugary and acidic drinks and foods that erode enamel.
- Eat a balanced diet rich in fruits, vegetables, dairy and lean proteins.
- Manage health conditions like diabetes that increase gum disease risks.
- Reduce stress levels which impair immune defenses.
- Avoid teeth grinding and clenching by managing stress and wearing a mouthguard.
- Wear a mouthguard during sports to prevent dental injuries.
With diligent oral care and regular dental treatment, gum disease can be prevented and bleeding minimized. But if bleeding persists, never delay seeing a dentist promptly.
Common Questions

What causes my teeth to bleed when I floss?
Gum bleeding when flossing is typically caused by inflammation in the gums from plaque buildup. Plaque irritates gums and causes swelling. Flossing scrapes off hardened plaque but also aggravates inflamed gums leading to bleeding. If not removed regularly, plaque hardens into tartar that worsens gum irritation.
Why do my teeth hurt from cold and bleed?
Sudden sharp tooth pain from hot or cold foods indicates tooth sensitivity. This happens when the outer enamel layer gets worn down, often from acidic foods or aggressive brushing. It exposes the inner dentin layer which contains tubes that transmit pain signals to nerves when stimulated. Dentin also lacks enamel’s protection so is prone to bleed when irritated.
Is it normal for teeth to bleed after a cleaning?
It can be normal to notice some bleeding or tender gums for 24-48 hours after a dental cleaning. As hardened plaque and tartar get scraped off from above and below the gumline, it causes slight irritation to gum tissues. However, if bleeding persists more than a couple days or is heavy, see a dentist to rule out infection or gum disease.
What does it mean if a tooth bleeds without anything touching it?
Spontaneous bleeding from a tooth that is not provoked by any stimulation is abnormal and requires prompt dental evaluation. It likely signals issues like an abscess, advanced gum disease destroying tissue, or a fractured tooth with exposed nerves. Don’t brush or floss the area before seeing a dentist.
When is bleeding from a tooth considered an emergency?
See a dentist immediately if you experience heavy bleeding, bleeding lasting several hours, or bleeding accompanied by severe throbbing toothache. These signal a dental emergency like a tooth abscess, advanced infection, or trauma. Bleeding indicates infection and nerve inflammation requiring urgent dental care to prevent complications.
Summary
Mild bleeding when flossing or eating crunchy foods occasionally is normal. But recurrent bleeding indicates gum disease, sensitivity issues, or trauma needing prompt dental evaluation. Proper oral hygiene and regular dental cleanings help prevent most bleeding causes. See a dentist right away for any persistent tooth bleeding, pain, or oral infections. With professional treatment, excellent home care, and addressing risk factors, you can have healthy gums and prevent excessive bleeding episodes.