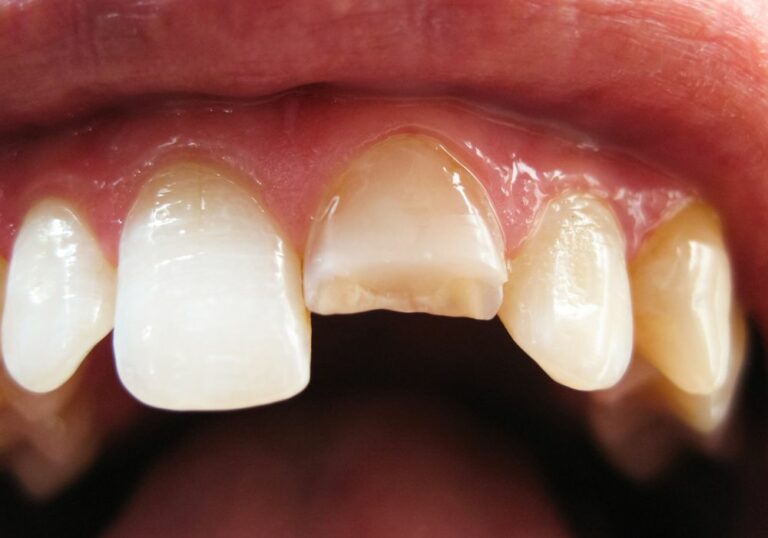
Receding gums and loose teeth are common oral health issues that affect many adults. This concerning symptom can have many complex causes and lead to additional problems if left untreated.
What’s Happening in Your Mouth?
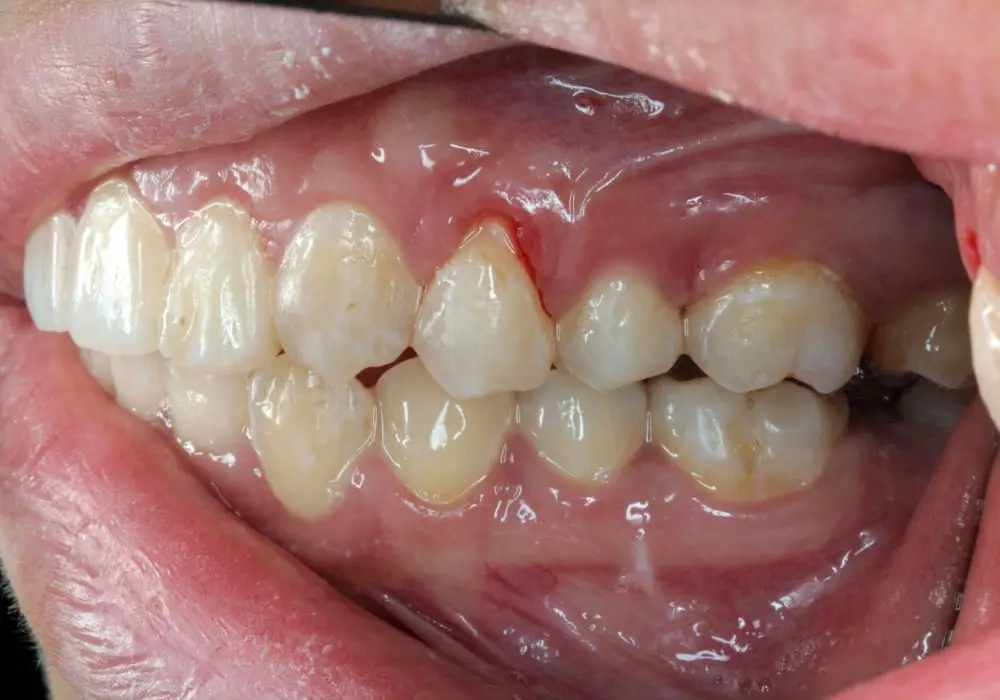
First, it’s helpful to understand what is occurring inside your mouth when you have receding gums and loose teeth.
Healthy gums fit snugly around teeth in a scalloped shape and provide a sealed protective barrier. Specialized gum tissue called the gingiva adheres to the tooth surface on one side and to the bone underneath on the other side.
This attachment begins to break down when gums become inflamed and infected by bacterial plaque buildup. The gums start pulling away from the base of the teeth, exposing vulnerable tooth roots and creating gaps called periodontal pockets.
At the same time, inflammation eats away at the underlying jawbone support structure. As bone density decreases, teeth lose their firm foundation and start to loosen and shift.
Causes of Gum and Bone Damage
Why does the gingiva recede and the bone deteriorate leading to mobile teeth? There are a number of contributing factors:
- Gum disease – Bacterial plaque inflames the gums, starting the recession. Left untreated, inflammation and infection continues destroying gum and bone.
- Poor hygiene – Inadequate brushing and flossing causes plaque and tartar accumulation that feeds gum disease.
- Smoking and tobacco – Chemicals constrict blood vessels reducing oxygen and nutrients to gums. This cell damage hinders healing.
- Clenching and grinding – Chronic force on teeth strains gums and wears down bone eventually loosening teeth.
- Age – Gums naturally loosen and bone density decreases as we get older.
- Hormones – Fluctuations during puberty, menstruation, pregnancy, and menopause influence gum sensitivity and health.
- Diabetes – High blood sugar increases vulnerability to infections like gum disease that damages gums and bone.
- Medications – Some drugs cause overgrowth or swelling of gum tissues that can mimic or mask gum disease.
- Crooked teeth – Misaligned teeth distribute chewing force unevenly increasing wear and tear.
- Fillings and crowns – Improperly fitted restorations can create ledges that are hard to clean and harbor bacteria.
Cascading Dental Problems
Progressing gum recession and loose teeth lead to many other dental issues:
- Tooth decay – With gums shrinking downward, more of the tooth root surface is exposed. Unlike enamel, the cementum covering roots is softer and more prone to cavities and decay.
- Tooth sensitivity – Receding gums no longer insulate and protect nerve fibers in the roots from hot and cold stimuli resulting in pain sensitivity.
- Tooth mobility – The periodontal ligament that allows teeth some natural, healthy movement stretches and weakens. Teeth shift more freely in their sockets.
- Tooth loss – Bone deterioration can reach a point where a tooth’s anchorage fails entirely and the tooth falls out or requires extraction.
- Bone loss – Inflammation destroys not only the bone immediately surrounding the tooth but can lead to loss of the wider jawbone shape.
- Bite changes – As teeth shift and space collapses, bite alignment and occlusion are altered. This impairs chewing ability.
- Infection – Gum pockets harbor bacteria that can spread and lead to abscesses, cysts and systemic infection requiring antibiotics.
- Digestion issues – Impaired chewing function makes it difficult to break down food properly, reducing nutrient absorption.
- Pain – Bone and root exposure cause symptoms of sensitivity and aching, especially when consuming hot or cold foods and drinks.
- Low self-esteem – Missing, loose or unsightly teeth can diminish self-confidence and social comfort.
Diagnosing Gum Recession and Loose Teeth

When you visit your dentist with concerns about receding gums or loose teeth, they will conduct a detailed examination to make a diagnosis including:
- Medical history review – Checking for any health conditions or medications contributing to symptoms.
- Oral examination – Visual inspection for signs of gum disease, plaque buildup, swelling, and decay. Using a periodontal probe to measure pocket depth around each tooth.
- X-rays – Dental radiographs show bone levels, tooth root integrity, and pathology.
- mobility testing – Wiggling teeth with dental instruments to assess looseness.
Based on these findings, your dentist will determine the cause and extent of gum recession and tooth mobility. From this, the most appropriate treatment recommendations can be made.
Treatment Options for Gum Disease and Loose Teeth
The goal of treatment is to resolve any infection and inflammation, prevent further tissue and bone loss, and attempt to tighten and stabilize teeth. Based on exam findings and diagnosis, your dentist may recommend:
- Improved daily plaque control – Careful brushing, flossing, antiseptic mouthwash to manage bacteria.
- Professional cleaning – Regular deep cleanings to reduce built-up calculus deposits that irritate gums.
- Gum disease therapy – Deep root planing and scraping, sometimes with antimicrobials.
- Oral antibiotics or antimicrobial rinses – To reduce bacterial levels in infected gum pockets.
- Flap surgery – Lifting gum tissue to remove built-up tartar from roots and bone then suturing gums back down tightly.
- Gum grafts and regeneration – Surgical gum and bone tissue grafts to cover exposed roots and stimulate regrowth.
- Bone grafts – Added bone implanted around teeth to fill in defects and strengthen stability.
- Biologic drug therapy – Anti-inflammatory proteins applied to gums to stimulate localized healing.
- Splinting loose teeth – Stabilizing mobile teeth together with dental splints.
- Bite adjustment – Realigning teeth to distribute chewing forces more evenly.
- Tooth extraction – Removing non-restorable teeth damaged beyond repair.
- Dental implant – If tooth was extracted, implant-supported replacement after bone heals.
The prognosis depends on multiple factors including the stage of disease, your oral hygiene diligence, and how well you respond to interventions.
Prevention Is Key
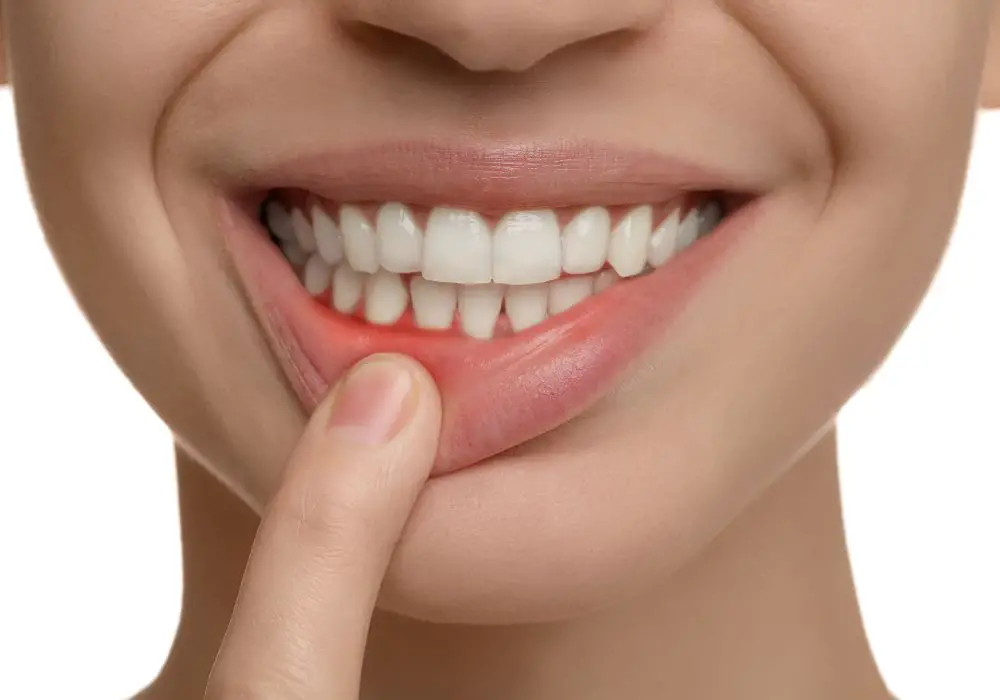
While excellent treatment options exist for receding gum and loose teeth, prevention is always preferable. Practicing excellent daily oral hygiene and getting regular professional care can help stop problems before they progress. Promptly treating gingivitis can also halt its development into severe periodontitis and its deteriorating effects on gums and bone. With vigilant prevention and care, your gums and teeth can stay healthy and firmly in place.
Frequently Asked Questions
Q: Why do my gums bleed when I brush?
A: Bleeding is usually a sign of inflammation from gum disease. Brushing too hard, inadequate flossing, and buildup of bacteria can all irritate gums and make them prone to bleeding. See your dentist to treat any infection and learn proper at-home care.
Q: Can receding gums grow back?
A: If caught at an early stage, treating gum disease can help tighten and reattach receding gums so they appear to “grow back.” More advanced recession requires grafting. Proper dental care helps prevent further recession.
Q: Do loose teeth always have to be extracted?
A: Not necessarily. Unless the tooth is severely damaged, treatments aim to tighten and save it. But some long-term loose teeth do eventually require extraction if beyond repair.
Q: Can gum disease be cured?
A: While gum disease cannot be cured permanently, its progression can be stopped and controlled.Provided patients diligently follow daily care instructions and get regular professional cleanings, the disease often can be well-managed over the long term.
Q: Am I too old to benefit from gum disease treatment?
A: Not at all. No matter your age, treating gum disease can help stabilize infection and inflammation, tighten teeth, minimize additional bone loss, and make your mouth more hygienic and comfortable. It is never too late to benefit from improved gum health.