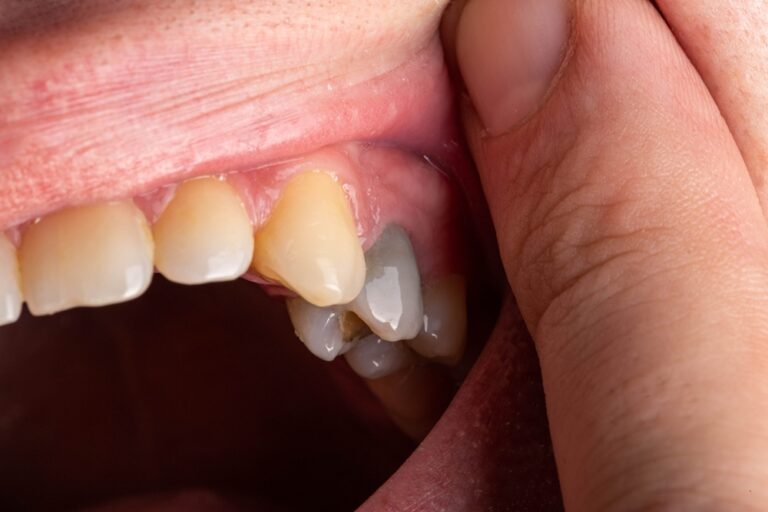
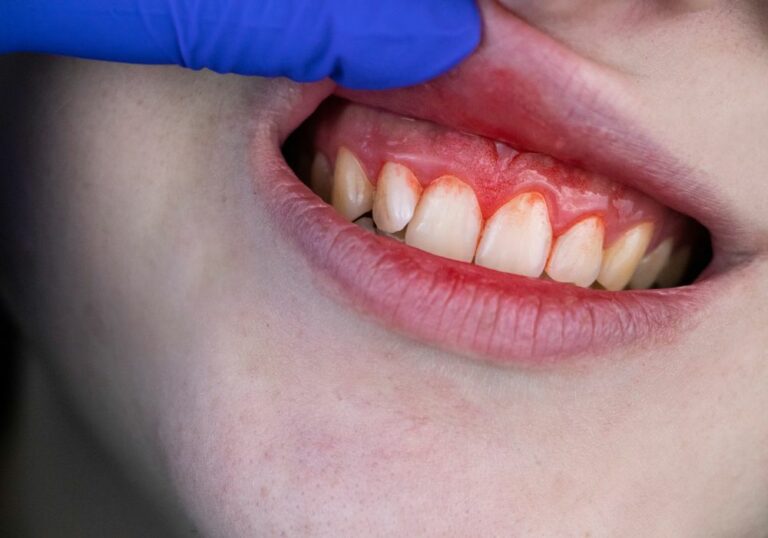
Tooth decay, also known as dental caries or cavities, is one of the most prevalent chronic diseases worldwide, affecting people of all ages. It occurs when acids produced by oral bacteria dissolve the mineralized outer layers of teeth – the enamel, dentin and cementum. This loss of mineralized structure is called demineralization. If cavities are not treated promptly, they can lead to a wide range of problems of increasing severity. Understanding the potential consequences of leaving decay untreated can help motivate people to seek preventive dental care and get cavities filled early.
Stages and progression of untreated tooth decay

Tooth decay begins when bacteria like Streptococcus mutans and Lactobacilli accumulate on the tooth surface in a sticky, colorless biofilm called plaque. The bacteria metabolize carbohydrate foods and produce acids like lactic acid. With frequent exposure to acid, the enamel loses mineral content and develops microscopic pores and flaws. This initial stage of decay is termed white spot lesions or incipient caries.
As demineralization continues, it leads to cavitation – the formation of tooth cavities. Cavities start as small, shallow pits in enamel that have a frosted white appearance and catch debris readily. Untreated pits can slowly penetrate deeper over 1-2 years into the softer dentin layer underneath enamel. Once decay reaches the inner pulp chamber of the tooth, more rapid damage occurs. The pulp contains nerves, connective tissue and blood vessels to supply the living cells of the tooth. Exposure leads to infection of the pulp tissue, intense pain, and abscess formation.
Bacteria and decay can then continue into the roots at the apex of teeth. This causes destruction of the periodontal ligament anchoring the tooth, eventual loosening, and premature tooth loss. Thus, there is a clear progression of cavities from mild, reversible stages to severe, irreversible ones causing lasting harm. Early intervention is key to prevent complications.
Consequences of untreated tooth decay
Sensitivity
As enamel thins due to demineralization, teeth become hypersensitive. Exposure of microscopic tubules in dentin makes the nerves more susceptible to stimuli. Early decay leads to sharp pains from hot, cold, sweet, or acidic foods and drinks. Sensitivity indicates inner layers of the tooth are unprotected.
Toothache and pain
Advancing decay reaches the pulp inside the tooth containing nerves and blood vessels. The inflamed pulp tissue triggers severe, throbbing tooth pain that can range from mild to excruciating. Pain may be provoked by hot or cold temperatures or pressure from chewing. It can disrupt sleep and routine activities.
Risk of infection
Cavities allow oral bacteria and toxins to invade deeper structures of the tooth, infecting the pulp. This leads to pulpitis – inflammation and infection of the pulp. The infected tooth becomes extremely painful, tender to touch, and sensitive to temperature changes. Pressure builds up in the rigid pulp chamber, causing throbbing pain.
As infection spreads through the root canal system, it leads to formation of an abscess at the root apex. A tooth abscess causes swelling of tissues around the tooth and jaw, gum redness and tenderness, pus drainage, foul tastes, and bites that feel “high.” The infection can spread to surrounding bones.
Impact on development in children
In children, cavities are more likely to occur in molars but can affect any primary or permanent teeth. Rampant caries cause early loss of primary teeth, which can reduce space for permanent teeth coming in, leading to crowding and misalignment. Missing primary molars also impair chewing function.
Difficulty eating and chewing
Untreated decay causes teeth to chip, fracture, or loosen and fall out prematurely. This impairs oral functions like biting, chewing, and speaking. Food choices become restricted to softer foods. Nutrition can suffer due to inability to chew fruits, vegetables, and meats. Dentures and bridges may be needed to replace missing teeth.
Esthetic and self-esteem concerns
Progressive destruction from cavities leads to unsightly holes between teeth, misshapen and discolored teeth, gaps from missing teeth, and collapsed bite structure. This can detract from appearance and self-confidence – especially for anterior teeth in smile zones. Poor dental esthetics may contribute to social withdrawal.
Impacts on overall health
Oral bacteria and inflammation can spread from dental infections to the bloodstream and other body regions. This is linked to heightened risk for heart disease, stroke, poor glycemic control in diabetics, preterm birth, rheumatoid arthritis, and aspiration pneumonia. Tooth loss can also impair nutritional intake, chewing, and digestion – impacting systemic health.
High risk groups for complications of untreated tooth decay

Some individuals and populations face amplified risks if tooth decay is left unaddressed, including:
- Children – primary teeth decay rapidly; cavities affect tooth spacing and alignment
- Older adults – gingival recession exposes more root surfaces to decay; common comorbidities affect oral health
- Individuals with chronic dry mouth – due to Sjogren’s syndrome, radiation therapy, medications, etc.
- Those with eating disorders – frequent vomiting erodes enamel
- People with substance abuse disorders – especially methamphetamine addiction (“meth mouth”)
- Those taking medications causing dry mouth as a side effect
- Individuals with disabilities – physical, neurological, cognitive, or mental impairments that limit oral hygiene and dental care access
- Persons of low socioeconomic status – financial barriers to professional dental care
Prevention and early intervention for tooth decay
Tooth decay is highly preventable with proper home oral hygiene, use of topical fluorides, dental sealants, and routine professional care. Key preventive measures include:
- Brushing with fluoride toothpaste twice daily
- Flossing between teeth daily
- Rinsing daily with antimicrobial mouthwash
- Replacing toothbrushes regularly before bristles are frayed and worn
- Using fluoride treatments, varnish or gel applications
Dietary habits should also limit frequency of exposure to sugars, acidic foods and beverages. Getting dental checkups and cleanings every 6 to 12 months allows early detection and treatment of cavities before they enlarge. Other beneficial therapies include:
- Pit and fissure sealants – plastic coatings bonded onto vulnerable chewing surfaces
- Fluoride or casein phosphopeptide-amorphous calcium phosphate applications – help remineralize enamel
- Antimicrobial peptides – attack cariogenic bacteria and biofilm acids
- Probiotics – replenish healthy oral microbiome
- Salivary stimulants – for those with chronically low saliva flow
Treating cavities in initial stages with fluoride, sealants, or infiltration minimally invasive techniques can reharden enamel and even reverse small lesions. This reduces need for more complex restorative treatments later on.
Treatments for established tooth decay

Several treatment options exist depending on the extent of decay. Common interventions include:
Dental fillings
Fillings involve removing decayed tooth structure using drill excavation. The cleaned out cavity is then filled and sealed with materials like composite resin, glass ionomer, amalgam, or gold.
Dental crowns
When decay is too extensive for fillings to restore form and function, crowns are used. The visible portion of the tooth is capped with a prosthetic cover made of porcelain-fused-to-metal, ceramic, or zirconia.
Root canal therapy
For infections in the pulp tissues inside teeth, root canals are needed. The pulp, nerves and blood vessels are removed, the space disinfected and sealed with gutta percha filler material. This saves severely decayed teeth from extraction.
Tooth extraction
Extraction involves complete removal of the decayed tooth. Partially erupted wisdom teeth with decay are also often extracted. Extractions are unavoidable in cases of untreatable abscesses, advanced gum disease, or gross tooth destruction.
Dental implants
Missing teeth must be replaced to avoid movement of surrounding teeth leading to misalignment and dental dysfunction. Dental implants – artificial roots screwed into bone – are the premier option vs bridges or dentures for replacing lost teeth.
Antibiotics
For acute dental abscess, antibiotics are prescribed short term to control spread of infection before definitive treatment. But they don’t fix the underlying problem.
Key steps in restoring damaged teeth
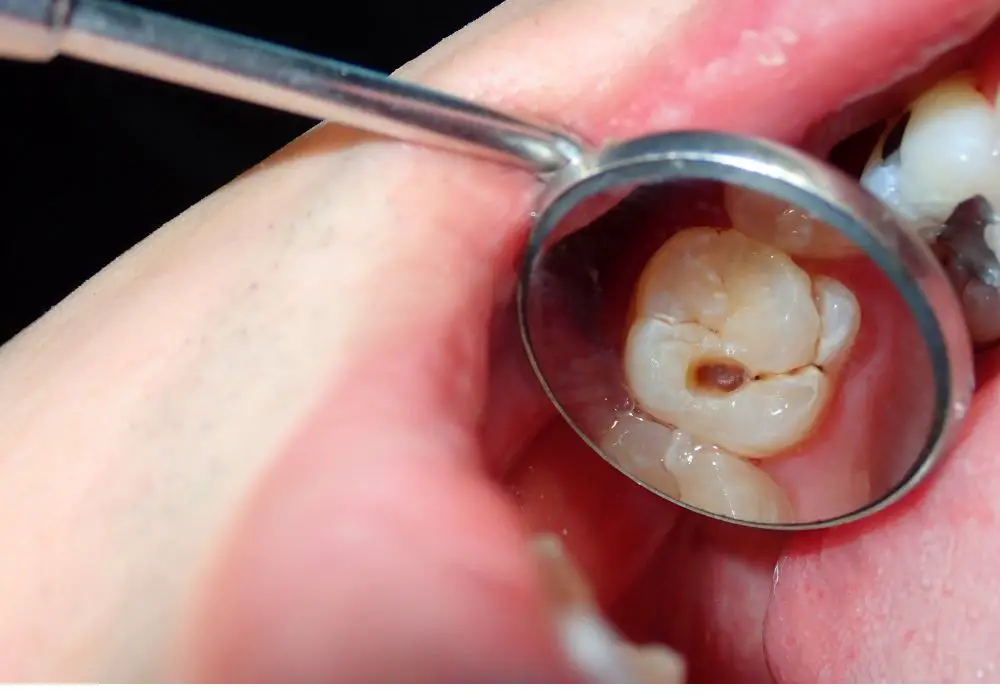
Effective restoration of decayed, weakened teeth requires these steps:
- Remove all softened, demineralized tissues – continued decay under restorations shorten their longevity
- Seal cavities from oral bacteria and moisture – prevents microleakage, secondary decay
- Bond restorations for fracture resistance – especially for root filled teeth more prone to splitting
- Restore adequate tooth structure for strength and function – improper bite forces lead to damage of teeth, restorations, or opposing teeth
- Ensure proper contacts and occlusion – avoiding excessive biting forces; balancing contacts distributes stresses
Restored teeth must be maintained with ongoing oral hygiene, fluoride use, and regular professional cleanings and monitoring. With conscientious home care and early intervention for new problems, the longevity of restorations is extended.
Conclusion
Tooth decay remains highly prevalent but is more preventable and treatable than ever before in populations with access to fluoride and dental care. Still, without treatment, cavities progress through irreversible destructive stages involving pulp infection, abscess, tooth fractures, and eventual tooth loss. Timely treatment allows decay to be stopped and teeth to be retained and restored with minimal invasive methods. This avoids the cascading problems and discomfort arising from advanced decay. Maintaining vigilant daily oral health habits remains essential to detect and treat caries early. With modern preventive care and restorative techniques, tooth decay and loss are avoidable consequences.
Frequently Asked Questions
What are the earliest signs of untreated tooth decay?
The earliest signs of tooth decay include:
- Tooth sensitivity to hot, cold, sweet foods
- Dull, frosty white spots or lines on tooth enamel
- Small pits or holes in enamel that catch debris
- Mild pain from sugary or acidic foods
These indicate demineralization of enamel is underway but decay has not yet cavitated. Timely treatment can reverse the process.
How long does it take for an untreated cavity to become serious?
This varies based on factors like tooth type and location. Shallow pits may take 6-12 months to turn into larger holes needing fillings. Without treatment, mild decay can reach the inner pulp within 1-2 years, causing severe pain and infection. Timely treatment is critical.
What problems can tooth abscesses cause?
Abscesses cause tissue swelling, gum inflammation, pus discharge, and intense throbbing pain. Infection can destroy periodontal fibers anchoring teeth, causing loosening. It can spread to facial planes, compress nerves, or enter the bloodstream, potentially becoming life-threatening. Urgent dental care is required.
Can tooth extractions lead to bone loss in the jaw?
Yes, missing teeth can trigger gradual bone loss. Teeth stimulate bone with their presence and chewing forces. When a tooth is lost, the socket area atrophies. This can cause facial sagging over time. Dental implants help prevent bone loss by transmitting forces through the jaw like natural teeth roots.
Is tooth decay preventable even as we age?
Yes, tooth decay can be prevented into old age through regular oral hygiene, fluoride exposure, healthy diet, and professional cleanings. Higher risk in seniors due to gingival recession and medications can be managed. Monitoring for early signs of decay and prompt treatment helps avoid problems. Oral health should be lifelong.