Wisdom teeth are the third and final set of molars that emerge in adulthood. While wisdom teeth were useful for early humans who had coarser, abrasive diets, they’ve become vestigial and problematic for most people today.
There often isn’t enough room for wisdom teeth to fully erupt or function properly. As a result, they frequently become impacted, only partially emerge, or come in crooked. This can lead to a number of problems, including pain, swelling, infection, cysts, and damage to nearby teeth and bone.
So can wisdom teeth ultimately cause permanent harm if they aren’t extracted? Let’s take a more in-depth look at what wisdom teeth are, the types of damage they can trigger, who is at risk, and when extraction should be considered.
What Are Wisdom Teeth?

Wisdom teeth are medically known as third molars. Most people have four wisdom teeth total, one in each corner of the mouth. They are named for the fact that they typically emerge later in life between ages 17 to 25 years old.
Wisdom teeth are the last teeth to develop and erupt. Evolutionarily, they likely enabled early humans to chew and process tough, coarser foods once adult teeth began to wear down. However, as modern diets and food preparation practices evolved to be more refined and processed, wisdom teeth have become largely unnecessary.
The other molar and premolar teeth ahead of them are now sufficient for chewing and grinding most modern foods. Since wisdom teeth are the last to develop, there is often insufficient room for them to fully erupt and function in the modern smaller jaw size. They also become obstructed by the existing aligned teeth ahead of them.
This lack of adequate space leads to a number of potential problems and risks associated with wisdom teeth, as we’ll explore in more detail next.
Common Problems and Risks Associated With Wisdom Teeth
Because of lack of space and obstruction from existing teeth, wisdom teeth frequently become impacted, come in partially, or erupt at odd angles. This can have a number of adverse effects, including:
Impaction
Impaction occurs when wisdom teeth become stuck underneath the gums and trapped by the jawbone or other teeth. They are unable to properly emerge through the gums.
This commonly happens when wisdom teeth develop at odd angles, there is insufficient room in the jaw, or other teeth block their path. Impaction can be partial or complete. It often causes pain, swelling, infection, and damage to neighboring teeth.
According to research, around 73% of young adults have at least one impacted wisdom tooth.
Pericoronitis
Pericoronitis refers to infection and inflammation of the gum tissue surrounding a partially erupted wisdom tooth. It occurs when the flap of gum overlying the tooth crown becomes swollen and infected.
Food debris and bacteria can get trapped under the gum flap and cause infection. Pericoronitis is very common with wisdom teeth because they often only partially emerge. Repeated episodes of pericoronitis are a top reason wisdom teeth require extraction.
Cysts
Fluid-filled sacs called cysts sometimes form around impacted wisdom teeth. These cysts develop in the jawbone tissue surrounding the impacted tooth and can damage neighboring teeth and bone.
Two types of cysts commonly associated with wisdom teeth are dentigerous cysts that involve the crown and radicular cysts that form around the root tips. Cysts may need to be surgically removed along with the wisdom tooth.
Tooth Decay and Cavities
Partially erupted wisdom teeth are challenging to clean and maintain good oral hygiene around. This makes them highly prone to tooth decay and cavity formation, even when wisdom teeth are otherwise normal and healthy.
The uneven chewing surfaces of partially emerged wisdom teeth also accumulate more dental plaque and debris. Studies show the incidence of cavities is much higher in wisdom teeth compared to other teeth. Poor oral hygiene and gum disease also contribute to wisdom tooth decay.
Gum Disease
Similarly, the difficulty cleaning around impacted or partially emerged wisdom teeth makes the area more vulnerable to gum disease.
Gum disease occurs when plaque builds up and causes gingivitis inflammation or periodontitis infection and erosion of bone and gum tissue supporting the teeth. This can ultimately lead to tooth loss. Wisdom tooth impaction is a major predisposing factor.
Crowding and Misalignment
When wisdom teeth try to erupt and emerge into the mouth, it can push and displace neighboring teeth. The pressure on surrounding teeth can cause misalignment of the bite, crowding, or crooked front teeth.
Orthodontists frequently recommend removing wisdom teeth prophylactically after braces treatment to avoid wisdom teeth undoing the corrected bite alignment.
Sinus Issues
The maxillary sinuses are located above the upper back teeth and premolars. When upper wisdom teeth try to erupt, they may press into the sinus cavity.
This can block proper sinus drainage and ventilation and lead to recurrent sinus infections. An opening can even erode between the tooth socket and sinus called an oroantral fistula that requires surgery to repair.
TMJ Problems
Wisdom teeth may emerge at odd angles and become impacted against the back molars. The displacement force and pressure on neighboring teeth can cause bite misalignment that leads to TMJ pain and dysfunction.
Problems with wisdom teeth are a common cause of temporomandibular joint disorders and dysfunction that causes jaw pain and impairs proper chewing motion.
Neural Disturbances
The roots of lower wisdom teeth lie close to the inferior alveolar nerve. Attempted extraction may damage this, causing numbness or paresthesia altered sensations in the lower lip, chin, gum, or tongue areas on that side. Lingual nerve disturbances are also possible with lower wisdom teeth.
As you can see, there are many ways impacted or problematic wisdom teeth can contribute to localized issues and oral health decline. But can they ultimately lead to permanent damage if not treated?
Can Wisdom Teeth Cause Permanent Damage?
Yes, in some cases wisdom teeth that develop problems and are not extracted can eventually cause permanent damage. Some examples include:
Bone Loss
Impacted wisdom teeth may progressively damage the bone tissue around them. Attempted eruption can also cause expansion and thinning of the surrounding bone.
Infection, cysts, and tumors around wisdom teeth can also destroy alveolar bone. Extracting problematic wisdom teeth after significant bone loss has already occurred can lead to further loss at the site. The jawbone may have permanent defects or asymmetry after extraction.
Tooth Loss
Untreated decay, gum disease, and infections caused by impacted wisdom teeth can spread to and damage neighboring teeth. This may ultimately necessitate extraction of once-healthy adjacent teeth.
Wisdom teeth extraction may also direclty cause accidental damage or loss of the distal root of the adjacent second molars in a small percentage of cases.
Nerve Injury
Attempting wisdom tooth extraction when the teeth are hooked under or compressing nerves poses a risk of permanent nerve damage. This includes lingual, inferior alveolar, and mental nerve injuries.
Nerve damage can cause numbness, pain, or altered sensations in the lip, chin, gum, or tongue areas which may persist indefinitely after wisdom tooth removal. This occurs in about 0.5% to 5% of extraction surgeries.
TMJ Osteoarthritis
In some cases, long term TMJ problems caused by wisdom tooth impaction and misalignment may result in permanent osteoarthritis of the temporomandibular joint. This causes chronic jaw pain and reduced mobility.
Sinus Perforations
Upper wisdom teeth pushing into the maxillary sinuses can sometimes perforate the bone or create an opening between the extraction site and sinus called an oroantral fistula. Repairing these perforations requires grafting and additional sinus surgery procedures.
Crown or Filling Damage
Adjacent teeth crowns or fillings may suffer irreparable cracks or fractures from the chronic pressure of impacted wisdom teeth trying to erupt. Damaged dental work usually needs replacement after wisdom tooth removal.
As you can see from these examples, allowing problematic wisdom teeth to remain too long before extraction can indeed ultimately cause permanent injury or damage to neighboring teeth, bone, nerves, sinus, TMJ, and oral function.
Who Is at Highest Risk of Wisdom Tooth Damage?
You may be more likely to experience complications and permanent damage from impacted wisdom teeth if:
- Your wisdom teeth are fully or partially impacted beneath the gums
- Infection, cysts, or tumors are present
- Your wisdom teeth are misaligned or mispositioned
- There is inadequate space for your wisdom teeth to erupt
- You already have issues like gum disease, cavities, or crowded/misaligned teeth
- You smoke or use tobacco – much higher pericoronitis risk
- You have uncontrolled diabetes or impaired wound healing
- You have a family history of problems with wisdom teeth
- You have other oral health risk factors
Talk to your dentist about your specific case if you think you may be at high risk for wisdom tooth complications. They can help determine if and when extraction is advisable.
When Should Wisdom Teeth Be Removed?
There is debate about the ideal timing for wisdom tooth extraction. Some dentists advise removing asymptomatic wisdom teeth prophylactically to avoid future problems. Others favor a more conservative watch and wait approach.
In general, the following scenarios may warrant wisdom tooth removal:
Impaction or Partial Eruption
Impacted wisdom teeth have a high probability of eventually causing problems. Early removal is recommended by most oral surgeons, especially in young patients, to avoid cysts or decay developing. However, difficulty of surgery and recovery tends to increase with patient age.
Recurrent Pericoronitis
Frequent gum infections around partially erupted wisdom teeth may necessitate extraction to prevent bone loss or spreading infection in this area.
Cysts or Tumors
Cysts, benign tumors like ameloblastomas, or other pathology associated with wisdom teeth require removal along with the abnormal tissue. Your dentist will diagnose conditions via x-rays, CT scans or biopsies.
Existing Tooth Decay or Gum Disease
Untreatable wisdom tooth decay or advanced periodontal disease affecting the wisdom teeth also warrants extraction. However, other mesial teeth should be salvaged if possible.
Progressive Damage
Evidence that impacted wisdom teeth are damaging adjacent teeth or bone indicates extraction should be performed before losses become substantial. This is a case-by-case determination.
Orthodontic Factors
Completing orthodontic treatment often involves wisdom tooth removal to avoid relapses. Wisdom teeth may also be extracted to allow correction of more anterior crowding.
Overall, most surgeons recommend early wisdom tooth extraction based on predicted complications, not waiting for overt symptoms or damage to develop. However, this does need to be balanced against risks of surgery. Talk to your oral surgeon about the advisability of removing problem-free wisdom teeth.
What Does Wisdom Tooth Extraction Involve?
Wisdom tooth removal is performed as an outpatient surgery under local anesthesia or IV sedation. The steps generally include:
Anesthesia
Anesthetic is administered to block pain and discomfort during the procedure. Options include:
- Local anesthetic – numbing shots to the surgery site
- IV sedation – intravenous drugs produce a deeper relaxed state
- General anesthesia – unconscious under general anesthetics
Opening the Soft Tissue
After anesthesia, your oral surgeon will make an incision in the gum tissue flap overlying the tooth and detach it so the tooth is exposed. They may need to remove a small amount of bone with a drill or osteotomy to reveal the crown.
Removing Obstructing Bone
More bone removal with a surgical drill may be necessary to fully visualize and access the wisdom tooth, especially if it is impacted or blocked by other roots. Your surgeon will be very careful to avoid damaging nerves or other structures.
Tooth Sectioning
The wisdom tooth may be sectioned into smaller pieces when necessary to facilitate easier removal without putting extreme pressure on the surrounding tissues and bones.
Tooth Removal
Dental elevators, forceps, and other instruments will be used to carefully loosen and extract the wisdom tooth from its socket once fully exposed. This requires controlled force while avoiding damage. The site is irrigated with sterile saline after removal.
Site Closure
Your gum tissue will be stitched closed using sutures that later dissolve on their own. A sterile dressing is then applied to protect the site while it initially heals.
You’ll receive postoperative care instructions before being discharged home to recover. Healing takes around 2 weeks, during which you should avoid certain foods and activities that could disrupt the site. Stitches dissolve within a week or so.
Possible Postoperative Complications
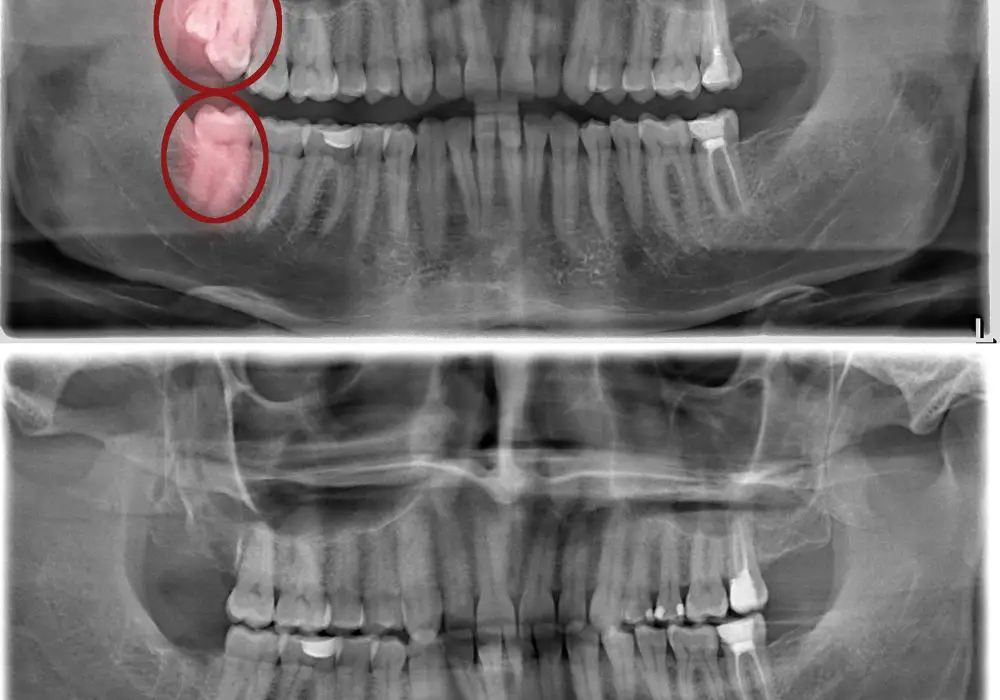
While generally safe when performed by an experienced oral surgeon, wisdom tooth removal carries a small risk of complications, including:
- Dry socket – delayed healing and pain from lost clot
- Nerve injury – causing numbness or parethesia
- Damage to other roots or teeth
- Excessive bleeding that is hard to control
- Postoperative infection – requiring antibiotics
- Sinus perforation with upper teeth
- Trismus – stiffness and difficulty opening jaw
Serious complications are uncommon but can occur in a small percentage of cases depending on difficulty. Follow all postoperative instructions carefully to support proper healing and minimize risks.
Frequently Asked Questions
Below are answers to some common questions about the risks and considerations around wisdom teeth:
How long does wisdom tooth extraction recovery take?
Expect wisdom tooth extraction recovery to take around 2 weeks, with the first 3-4 days being most uncomfortable. Swelling, pain, and bruising should gradually improve over this period. Avoiding hard foods and disruptive activities can expedite healing.
Can wisdom teeth move or damage other teeth?
Yes, wisdom teeth can sometimes apply pressure to and displace neighboring teeth as they try to erupt. This can cause misalignment, crowding, bite changes, and damage over time. Removing them prevents distortion.
Should I get wisdom teeth removed if not causing problems now?
That’s a case-by-case decision to make with your oral surgeon. If they are fully erupted and functional with space, they may be left in place. But given high future complication rates, at-risk or problematic wisdom teeth are often pre-emptively extracted.
How painful is wisdom tooth extraction?
Having wisdom teeth out certainly involves some degree of pain and discomfort afterward. But local anesthetic prevents any pain during the actual procedure. Post-op pain is usually manageable with over-the-counter medication but may require prescription painkillers in more difficult impactions.
Can wisdom tooth extraction cause permanent nerve damage?
In a minority of cases, wisdom tooth removal may cause lasting paresthesia or numbness from damage to nerves like the lingual or inferior alveolar nerves. This risk is low with an experienced surgeon, but you should discuss the potential for long-term neuropathy.
Is there an age limit for removing wisdom teeth?
There is no strict age cutoff, but extraction tends to become more complex and challenging in older patients. Recovery also takes longer. Most dentists recommend early removal as soon as signs of impaction or problems emerge, often late teens to early 20s. The success rate decreases after age 25.
In summary, wisdom teeth that are impacted or developing problems can indeed ultimately cause permanent damage to other teeth, nerves, bone, and surrounding structures if not extracted in a timely manner. Discuss your particular case with your dentist and oral surgeon to determine appropriate timing for removal if indicated. While extracting problem-free wisdom teeth remains controversial, addressing high-risk cases early on can help prevent serious complications.