Understanding tooth sensitivity
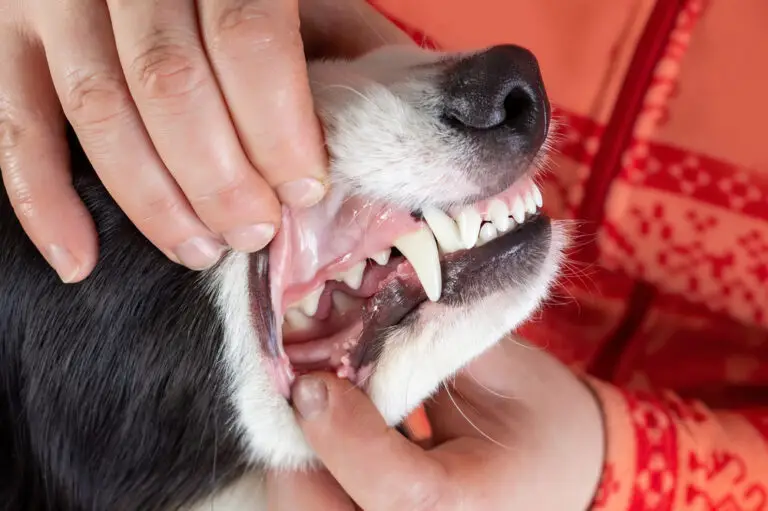
Tooth sensitivity, also known as dentin hypersensitivity, is a common dental condition characterized by pain or discomfort in teeth when exposed to certain triggers. It occurs when the dentin layer underneath the tooth enamel becomes exposed, usually due to receding gums, enamel erosion, cracks or chips in the teeth. The dentin contains thousands of microscopic tubules that lead directly to the nerve of the tooth, making it highly sensitive.
Common triggers for tooth sensitivity include:
- Hot or cold foods and drinks
- Sweet, sour or acidic foods
- Biting or chewing
- Cold air
- Tooth brushing
Tooth sensitivity can range from mild to severe, and may affect one or multiple teeth. Very sensitive teeth are ones that react to even minor stimuli like a small sip of cold water or air flow. The pain is typically sharp and sudden, but goes away once the trigger is removed. Over time, sensitive teeth may become less responsive to common triggers.
What causes very sensitive teeth?
There are several potential causes of severe tooth sensitivity:
- Gum recession – When gums recede due to periodontal disease or overly vigorous brushing, the root surface and dentin are exposed. This loss of protective covering makes teeth prone to sensitivity.
- Tooth erosion – Acidic food and drink can erode enamel over time, making the dentin more vulnerable. Conditions like acid reflux can also cause erosion.
- Cracked or chipped teeth – Fractures or cracks in the enamel expose the sensitive dentin and nerves.
- Teeth grinding – Grinding or clenching teeth, known as bruxism, can wear down enamel and dentin.
- Tooth decay – Cavities that extend to inner layers can become sensitive.
- Tooth bleaching – Whitening treatments may make teeth more porous and prone to sensitivity.
- Root sensitivity – Following root canal treatment, cleaned and filled roots may become sensitive.
- Older fillings – Leaking or ill-fitting fillings allow sensitivity-causing triggers inside the tooth.
Prolonged sensitivity with no obvious cause warrants a dental exam to check for issues like decay, cracked teeth or gum disease. Very sensitive teeth may indicate a significant problem requiring treatment.
How teeth whitening works
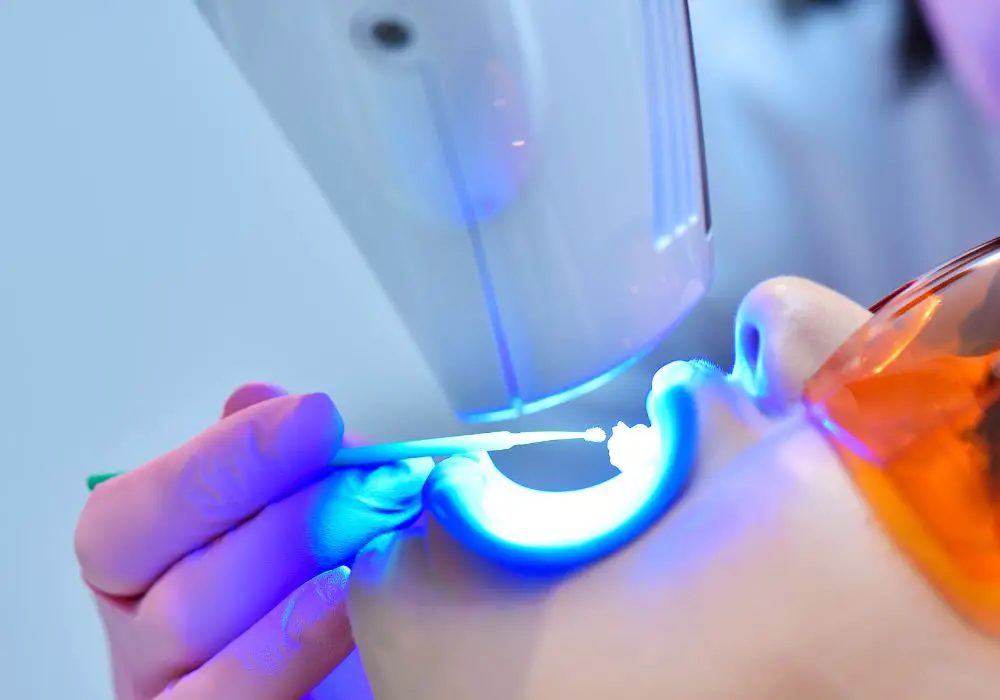
Teeth whitening, also known as dental bleaching, is a common cosmetic procedure that lightens and brightens teeth color. It is an effective way to remove stains from coffee, tea, smoking, food and beverages. Teeth naturally dull over time from aging and wear. Whitening restores teeth to a more youthful, natural shade.
There are two main methods of professional whitening offered by dentists:
- In-office bleaching – The dentist applies a high concentration hydrogen peroxide gel to the teeth and uses a special curing light or laser to accelerate the bleaching. Results are seen after one 30-60 min visit.
- At-home whitening – Custom-fitted plastic trays are filled with a lower concentration carbamide or hydrogen peroxide gel. Trays are worn for 1-2 hours a day or overnight for up to 2 weeks.
Over-the-counter whitening kits typically contain weaker whitening gels with 3-10% carbamide peroxide used with a generic tray or brush application.
Whitening works by the active ingredient, usually hydrogen peroxide or carbamide peroxide, penetrating the tooth enamel and oxidizing or reducing organic stains. This lightens the intrinsic discoloration in the dentin beneath the enamel.
Higher peroxide concentrations give faster results, but also increase risk of tooth sensitivity. Dentists can monitor and adapt treatment to minimize sensitivity.
Potential side effects of whitening
While generally safe, teeth whitening may have temporary side effects:
- Tooth sensitivity – The most common problem, occurring in up to 78% of patients. Usually mild, but can be more severe in susceptible individuals.
- Gum irritation – Whitening gel leaking onto the gums can cause burning or soreness.
- Soft tissue inflammation – Lips, cheeks or tongue may become irritated.
- Canker sores – Some people may develop mouth ulcers.
- Tooth surface changes – Enamel may become more porous or translucent.
- Relapse – Teeth gradually revert back to their original color over time without maintenance whitening.
Proper application and monitoring by a dentist reduces the likelihood of complications. Mild sensitivity can be managed with desensitizing toothpaste before and after treatment.
Can very sensitive teeth be whitened?

Teeth that are already extremely sensitive present a challenge for whitening treatment. However, there are ways to whiten sensitive teeth safely and effectively:
Use lower concentration peroxide gels
Higher concentrations of hydrogen peroxide or carbamide peroxide increase the risk of sensitivity. Using gels with no more than 10-15% hydrogen peroxide or 20-35% carbamide peroxide helps minimize this.
Apply for shorter time periods
Applying whitening gels for less time – 30 mins instead of 1 hour – gives a gentler treatment that is less likely to irritate sensitive teeth.
Undergo in-office whitening procedure
In-office whitening performed under dental supervision allows for close monitoring and adjustment of treatment based on any sensitivity experienced.
Use desensitizing agent before and after
Applying a desensitizing fluoride gel or using a desensitizing toothpaste helps block pain transmission in the dentin before and after whitening sessions.
Get customized whitening trays
Well-fitted trays limit gel contact with gums, preventing irritation and sensitivity in the gingiva.
Focus on anterior teeth
Since front teeth have the thickest enamel, whitening them minimizes sensitivity risks compared to thinner enamel posterior teeth.
Wait until any oral health issues are treated
Teeth that are sensitive due to decay, fractures, gum recession or other issues should be stabilized first before undergoing whitening.
Avoid overuse of whitening products
Using whitening gels too frequently or for prolonged periods can increase inflammation. Take intermittent breaks in treatment.
With careful treatment planning and proper precautions, even teeth that are prone to sensitivity can benefit from whitening to restore a beautiful smile. Work closely with your dentist to control discomfort and get the maximum whitening result you desire.
How to relieve sensitivity from whitening
If you experience pain or discomfort from teeth whitening, there are ways to get relief:
- Stop treatment – Discontinue use of the whitening gel until sensitivity subsides. Avoid very cold foods and drinks as well.
- Desensitizing toothpaste – Brush with toothpaste for sensitive teeth containing ingredients like potassium nitrate or stannous fluoride.
- Fluoride rinse – An over-the-counter fluoride mouth rinse helps strengthen enamel.
- Desensitizing gel – Applying a desensitizing gel containing compounds like potassium nitrate or sodium citrate helps block pain.
- Over-the-counter pain medication – Anti-inflammatories like ibuprofen may relieve sensitivity discomfort.
- Dental work – For severe sensitivity, dental treatment like fillings or sealants may be required to cover exposed dentin.
- Toothpaste for remineralization – Special toothpastes help rebuild enamel to reduce sensitivity.
Talk to your dentist if sensitivity persists for several days or impedes eating, drinking or brushing. Teeth typically recover in 1-2 weeks.
Maintaining a white smile

While teeth whitening produces dramatic results, the effects are not permanent. Without occasional touch-ups, teeth will gradually darken over time. Here are some tips for keeping your smile bright long-term:
- Use whitening toothpaste daily
- Drink water after consuming staining foods and drinks
- Limit intake of dark-colored foods and beverages
- Stop smoking and other tobacco use
- Have professional whitening treatments annually or biannually
- Use custom-fitted whitening trays at home 2-4 times per year
- Brush and floss carefully to prevent stains from plaque accumulation
- Get regular dental cleanings and exams
- Protect teeth from trauma that can cause internal discoloration
Following a strict oral hygiene routine and getting periodic professional whitening will help you maintain a radiant, youthful smile for years to come. Be sure to schedule follow-up appointments with your dentist.
Frequently Asked Questions
1. How long does teeth sensitivity from whitening last?
Tooth sensitivity from bleaching is usually temporary, lasting 1-2 weeks at most. Sensitivity tends to peak in the early stages of treatment and gradually declines over time. Proper oral hygiene and desensitizing products help shorten the duration.
2. Can sensitive teeth be whitened without pain?
It may be difficult to whiten highly sensitive teeth without any sensitivity or discomfort. However, choosing lower strength peroxide gels, taking breaks between treatments and using desensitizing toothpastes can minimize pain. In-office procedures allow dentists to closely monitor and respond to sensitivity.
3. What is the best whitening method for sensitive teeth?
In-office whitening is generally the best option for sensitive teeth. With higher strength gels and curing light, results are faster with less total exposure time. The dentist can also modify treatment based on your response. Custom trays with low concentration gels are gentler than strips.
4. Can whitening permanently damage sensitive teeth?
There is little evidence properly performed whitening by a dentist will permanently damage healthy teeth, even sensitive ones. However, existing conditions like gum recession may worsen from overuse of peroxide gels. Whitening should not be performed until oral health problems are treated.
5. How can I prevent sensitivity when whitening teeth?
Using lower peroxide concentrations, desensitizing toothpaste before and after treatment, getting well-fitted trays, and avoiding excess product on the gums can help prevent sensitivity from whitening sensitive teeth. Completing any needed dental work beforehand also reduces sensitivity risks.
Conclusion
Whitening is an excellent way to restore discolored sensitive teeth, but requires careful precautions. Consulting a dentist for evaluation and using customized trays with low concentration whitening gels makes the process safer and more comfortable. Preventive measures like desensitizing pastes and gels can further minimize sensitivity. With caution and patience, you can gradually achieve your desired shade and enjoy a brighter, more confident smile.