Toothaches and dental infections are among the most common reasons people seek medical and dental care. Severe tooth decay, cracks, gum disease, and trauma can all allow bacteria to invade the hard outer enamel layer of the tooth and infiltrate the soft inner pulp tissue.
An abscessed tooth is a serious condition requiring urgent dental care. Antibiotics are often prescribed as an adjunctive treatment for tooth infections and abscesses along with definitive dental treatment like root canals or tooth extraction.
But can antibiotics alone cure tooth infections? Are they always necessary? Which antibiotics are commonly used and how are they administered for dental abscesses? Read on as we explore the role of antibiotics for the treatment of tooth infections.
What are tooth infections and what causes them?
Tooth infections, medically known as dental abscesses, occur when bacteria invade the tooth and surrounding gums, multiplying rapidly and producing pus inside the teeth or gums. The most common causes include:
- Untreated tooth decay – Cavities that extend deep into the tooth’s inner layers (dentin and pulp) allow oral bacteria to enter and infect the pulp tissue inside the tooth root.
- Cracked teeth – Fractures and cracks in enamel and dentin create pathways for bacteria to get inside the tooth. Cracks often happen from trauma, grinding, or deteriorating dental work.
- Gum disease – Advanced periodontal disease damages the gums and supporting bone, creating pockets and exposing more tooth surface for bacteria to infect.
- Previous dental work – Fillings, crowns, and root canals that have deteriorated over time can become defective. Bacteria then exploit gaps and cracks to get inside the tooth.
- Pericoronitis – Inflammation and infection of gum tissue around an impacted or partially erupted wisdom tooth.
Once inside the tooth’s inner layers or gum tissues, the bacteria multiply and release toxins that cause swelling, tissue damage, and pus formation. The pus builds up inside the rigid tooth structures or gum pockets, leading to increased pressure, pain, and swelling.
How do dentists diagnose a tooth infection?
Dentists use a combination of visual examination, dental x-rays, and assessment of symptoms to diagnose a tooth infection. Signs can include:
- Visible swelling in the gums near the infected tooth
- Redness and puffiness in nearby gums
- Deep dental decay reaching the pulp upon examination
- Pain in the tooth, especially with pressure or chewing
- Sensitivity to hot and cold foods/drinks
- Halitosis
- Dental abscess visible on x-ray as radiolucent area at tooth apex
- Increased tooth mobility
- Lymph node swelling
- Fever, chills, and malaise if infection becomes severe
The above signs, especially when persistent and not resolving with conservative treatment, point to a bacterial infection needing antibiotic treatment.
Why are antibiotics commonly prescribed for tooth infections?
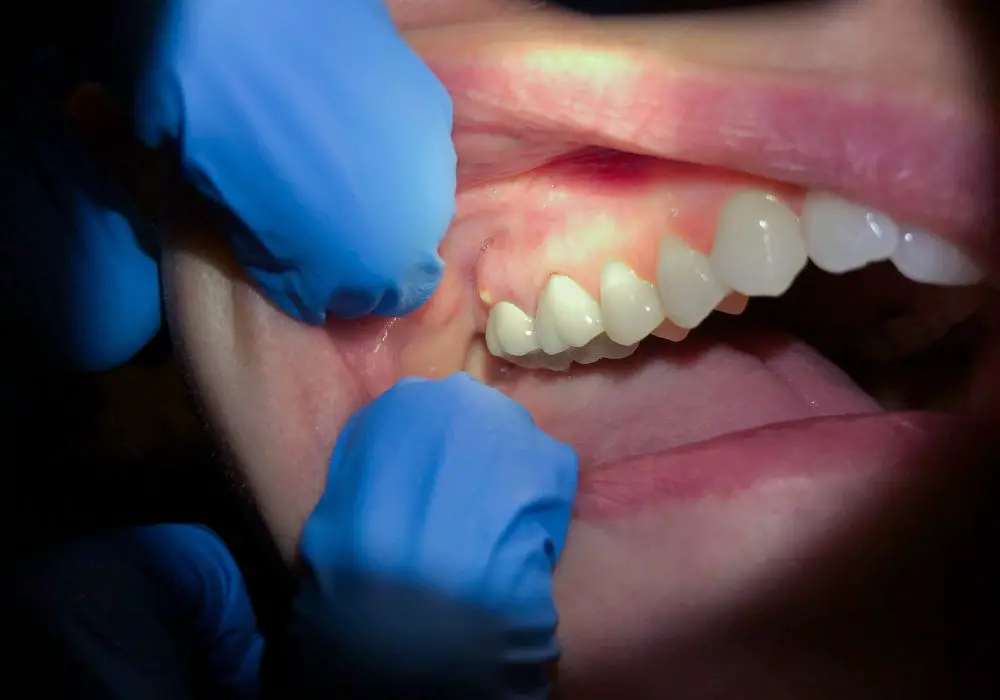
While antibiotics cannot definitively cure tooth infections alone, they play an important role in management by:
- Eliminating active infection – Antibiotics eliminate most of the harmful, pus-forming bacteria allowing the abscess to resolve.
- Relieving pain/swelling – They quickly reduce inflammation and associated tooth pain and swelling caused by bacterial toxins and pressure buildup.
- Preventing spread – Antibiotics prevent the infection from spreading to deeper facial planes and spaces which can be very serious.
- Stabilizing before definitive treatment – They stabilize the infection so extraction, root canal therapy, or restorative work can be performed safely without complication.
- Supplementing dental treatment – Antibiotics help eliminate residual bacteria remaining after dental procedures on severely infected teeth.
- Protecting at-risk patients – Those with heart conditions, joint implants, or weakened immunity may need antibiotics pre/post-dental treatments to prevent infection spreading.
So while antibiotics don’t cure the problem directly, they play an important supporting role in safely managing tooth infections.
How do dentists select the appropriate antibiotics?
Dentists consider multiple factors when choosing the optimal antibiotics for a tooth infection:
- Type and location of infection – For example, periodontal abscess vs infected root canal. Different bacteria are involved in different sites.
- Severity of infection – Mild, moderate, or severe based on extent of swelling, pain, temperature, and systemic symptoms.
- Patient’s medical history – Underlying conditions, allergies, medications, pregnancy status are considered.
- Culture/sensitivity testing – Identifying the specific bacteria involved and testing antibiotic susceptibility guides selection.
- Susceptibility of likely bacteria – Most dental infections involve aerobic and anaerobic oral streptococci and gram-negative rods which tend to be susceptible to certain antibiotics.
- Pharmacokinetics – How the antibiotic concentrates in oral tissues and penetrates bone is considered.
- Previous antibiotic exposure – Prior antibiotic use can select for resistant bacteria, requiring alternative choices.
After assessing the above factors, the dentist will select the most appropriate antibiotic, dose, duration, and route of administration customized to the patient and their infection.
What are the most commonly prescribed antibiotics for dental infections?

The major antibiotic classes used in dentistry include:
Penicillins
- Amoxicillin – First-line choice preferred by most dentists for dental infections. Provides good coverage against oral streptococci, staphylococci, and gram-negative anaerobes. Bacterial resistance is low.
- Penicillin VK – Narrow spectrum penicillin effective for mild early infections susceptible to penicillin. Resistance limits its use.
- Augmentin (amoxicillin + clavulanate) – Addition of clavulanate extends coverage against beta-lactamase producing bacteria resistant to amoxicillin alone. Used for severe infections.
Tetracyclines
- Doxycycline – Broad spectrum antibiotic alternative for penicillin-allergic patients. Concentrates well in dental tissues. Also used for specific periodontal infections.
Macrolides
- Erythromycin – Alternative to penicillin against oral streptococci and staphylococci. Used for penicillin-allergic patients.
Lincosamides
- Clindamycin – Potent antibiotic effective against many gram-positive aerobes and anaerobes involved in severe odontogenic infections. Used for penicillin-resistant infections.
Metronidazole
- Flagyl – Specifically targets anaerobic bacteria which predominate in dental infections. Often combined with penicillin or clindamycin.
Fluoroquinolones
- Levaquin, Cipro – Broad spectrum antibiotics reserved for severe resistant infections that have not responded to other antibiotics.
What are typical antibiotic treatment regimens prescribed by dentists?
Usual dosage and duration protocols:
- Amoxicillin – 500mg 3 times per day for 5-7 days. Can increase to 875mg/125mg Augmentin for severe infections.
- Doxycycline – 100mg 2 times per day for 7-10 days.
- Clindamycin – 300mg 3 times per day for 7 days.
- Metronidazole – 250mg 3 times per day for 7 days.
Higher doses within safe limits may be prescribed for severe infections. It is critically important to complete the full course as directed rather than stopping early when symptoms resolve. This helps eliminate residual bacteria and prevent recurrence.
What precautions should be taken when using antibiotics for dental infections?
- Inform dentist of any medication allergies or prior adverse reactions to guide selection.
- Disclose all medical conditions, immunocompromise, as well as current medications, supplements, pregnancy, and breastfeeding status to avoid potentially dangerous interactions.
- Take the antibiotic exactly as prescribed – dosage, duration, administration with/without food. Never skip doses or stop early.
- Avoid alcohol consumption with metronidazole which can cause severe nausea and vomiting.
- Do not share or self-prescribe leftover antibiotics. Only take antibiotics prescribed directly for your current infection.
- Monitor for side effects like rash, nausea, diarrhea that may indicate intolerance. Promptly report significant side effects.
- Practice good oral hygiene during the antibiotic course to help resolve the infection source.
- Seek immediate care if infection worsens or shows signs of spreading despite antibiotics.
What are some potential risks or downsides to using antibiotics for dental infections?

Some possible risks include:
- Allergic reactions – Rash, hives, swelling, anaphylaxis in those with antibiotic allergies. Need to use alternate antibiotic.
- Antibiotic resistance – Overprescribing and improper use promotes growth of resistant bacteria. Should only be used for diagnosed bacterial infections.
- Gastrointestinal symptoms – Nausea, vomiting, diarrhea are common side effects, especially from broad spectrum antibiotics altering gut flora. Taking with food can help.
- Interactions with other medications – Antibiotics may interact with anticoagulants, birth control pills, anti-seizure medications, and others. Dose adjustments may be required.
- Opportunistic oral infections – Killing normal oral bacteria allows fungal overgrowth like oral thrush or proliferation of Clostridium difficile.
- Recurring infection – Stopping antibiotic course prematurely leads to infection persistence or recurrence in most cases.
- Superinfection – Excessive antibiotic use can suppress normal flora and allow secondary infections by pathogens like Candida or C. diff.
However, with proper usage as directed by a dentist, the benefits outweigh the risks for most cases where antibiotics are truly warranted to treat moderate to advanced tooth infections.
Frequently Asked Questions
Q: Should I take antibiotics for a mild tooth infection?
A: Antibiotics are usually not necessary for mild tooth infections without significant swelling, fever, or facial spread. These may resolve on their own with conservative dental treatment. Antibiotics should be reserved for diagnosed bacterial infections to limit resistance.
Q: How quickly will antibiotics relieve an abscessed tooth?
A: Antibiotics begin working within the first few hours but it typically takes 24-48 hours to substantially reduce pain, swelling, fever, and other symptoms of a severe tooth abscess. Extracting pus via drainage or extraction brings faster relief. But antibiotics require several days to fully eliminate infection.
Q: Can antibiotics substitute definitive dental treatment like a root canal?
A: No. While antibiotics help temporarily manage the infection, decayed and infected tooth structure remains. Root canal therapy or tooth extraction is still required to fully cure and resolve the tooth infection.
Q: Are broader spectrum antibiotics always better?
A: Not necessarily. When appropriate, targeted narrow spectrum antibiotics focused on the specific oral bacteria involved are preferred to avoid unnecessary antibiotic exposure and killing of beneficial bacteria. However, resistant or severe infections may require broad spectrum antibiotics.
Q: Can I stop taking antibiotics when I feel better?
A: No, you should never stop antibiotics prematurely before completing the prescribed course. Although symptoms may start improving, stopping early frequently leads to recurrent infection as residual bacteria persist. It is important to continue taking the antibiotics as directed to fully eradicate the bacteria.