Having a bright, white smile can do wonders for your confidence and appearance. But some people are bothered by yellowish or discolored teeth that resist at-home whitening treatments. If you’ve noticed your teeth are not getting as pearly white as you hoped with over-the-counter whitening products, you’re not alone.
Many factors can contribute to yellow teeth that do not sufficiently whiten with strips, toothpaste, rinses and other store-bought methods. The cause, location and severity of stains impact how well they respond to bleaching treatments.
While whitening cannot alter the innate color of teeth, professional procedures may still substantially improve the appearance of yellowed teeth. Discussing your particular staining situation with a dentist can help determine options to safely manage resistant discoloration and boost your smile.
This article explores the common reasons why teeth become resistant to whitening and do not lighten as desired with at-home methods. We’ll discuss causes of difficult stains, whether they can be externally removed or are incorporated internally, and potential professional solutions to significantly brighten your smile.
Causes of Yellow Teeth That Resist Whitening
Yellow teeth that do not respond to whitening treatments are often intrinsically stained deep within the tooth structure. This occurs when the dentin layer underneath the enamel darkens over time.
1. Enamel Thinning
The enamel is the hard, protective outer layer of the tooth. As we age, enamel naturally wears thin and exposes more of the yellow dentin underneath. This dentin contains less mineral content and more organic materials that gradually darken and appear more yellow.
Enamel also thins from chronic acid erosion. Frequent consumption of acidic foods and drinks wears away enamel to reveal yellow dentin. Conditions like bulimia and acid reflux also erode enamel. As thinning enamel no longer adequately covers the dentin, teeth look more discolored.
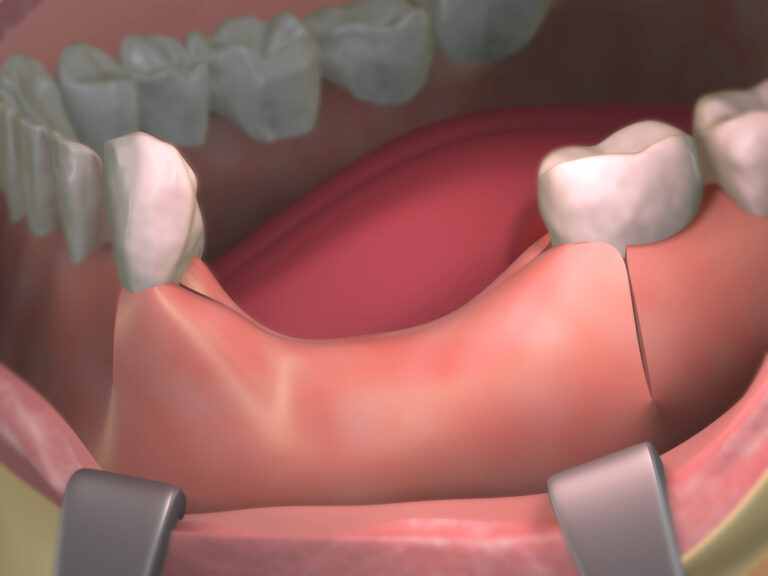
2. Dentin Exposure
Dentin may become visible along the gumline if recession occurs, or near the biting edges of worn teeth. Any exposed dentin will maintain its yellowish color despite surface whitening treatments.
Cracks and chips in teeth can occur from trauma, grinding or cracking hard foods. Any underlying dentin revealed through damage will not change color.
3. Dead Teeth
After a root canal procedure, the pulp tissue inside the tooth is removed. Over time, these non-vital teeth may turn yellow or grey. Since the nerve and blood supply are gone, the inner tooth structure essentially dies.
Whitening gels cannot penetrate deep within a dead tooth’s layers to alter its intrinsic color. The discoloration is permanent unless concealed with a restoration.
4. Tetracycline Staining
Children whose developing teeth absorb tetracycline antibiotics between ages 8 and 12 are prone to intrinsic dark staining. Tetracycline molecules become incorporated into the crystalline structure of enamel and dentin as the teeth form.
The antibiotic binds to calcium ions needed for normal mineralization of enamel. This affects the light reflection and absorption properties of the developing teeth, causing gray, yellow or brown discoloration. Tetracycline staining may appear in mottled, vertical, horizontal or diffuse patterns. The extent of staining depends on dosage level and duration of the medication.
5. Fluorosis Staining
Consuming excessive fluoride during tooth development can result in intrinsic staining. Fluorosis occurs when fluoride intake consistently exceeds optimal levels between ages 2 and 8. Too much fluoride impacts enzyme function and the process of dentin mineralization.
In mild forms, fluorosis appears as nearly invisible white specks on enamel. Moderate fluorosis stains enamel with white streaks or spots. In the severe form, enamel is discolored dark yellow, brown or black. The stains become incorporated into the teeth as they develop.
6. Chemical Staining
Habitual consumption of certain foods, beverages and medications can deeply stain teeth over time. Chromogens or coloring compounds in these substances penetrate into pores of the enamel to discolor the underlying dentin.
Common causes of chemical staining include:
- Coffee, tea, colas – Contain tannins that impart yellowish stains.
- Wine, berries, sauces – Contain anthocyanins that leave red/purple stains.
- Tobacco – Tar & nicotine create brownish stains.
- Antibiotics like doxycycline – Turn teeth grey.
- Antihistamines – Cause brownish discoloration.
- High blood pressure meds – Lead to black stains.
The longer teeth are exposed to staining substances, the more challenging stains are to lighten. Chemical staining progresses deeper over time.
7. Aging
Aging naturally yellows teeth over time due to gradual chemical and structural changes. Enamel becomes more porous with age, allowing deeper penetration of stains. The enamel layer also thins to reveal darker underlying dentin.
Meanwhile, the dentin layer thickens and more minerals are deposited within it. Aged dentin contains less organic material, allowing light to reflect differently off the yellowish surface. The inner pulp chamber also shrinks, which alters light absorption.
As teeth age, both the enamel and dentin take on a darker and more yellow coloration that resists external bleaching.
Determine If Stains are External or Internal
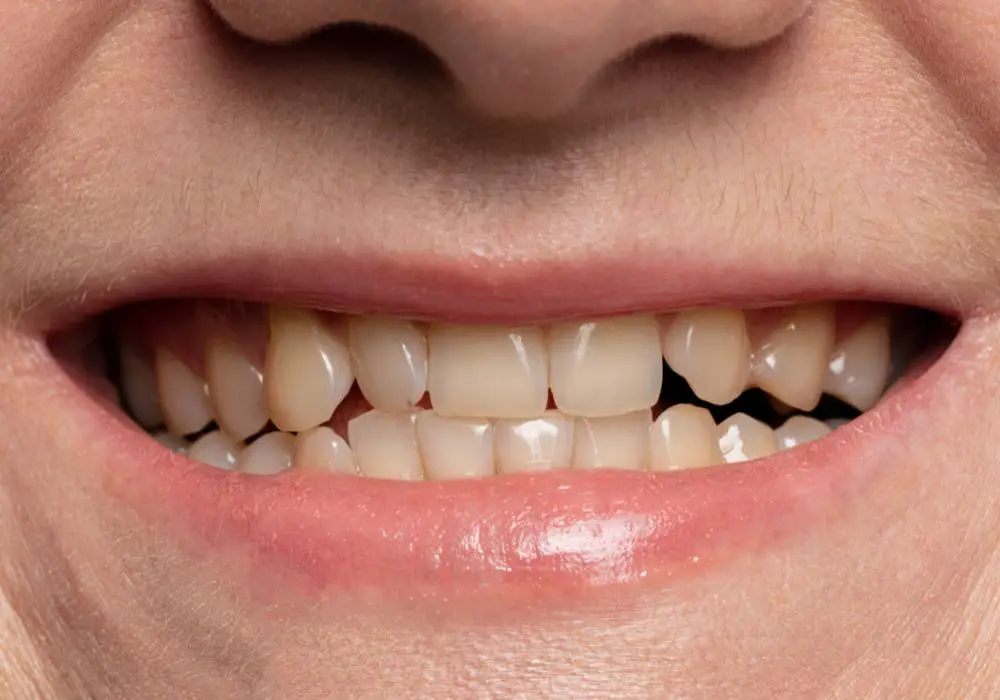
Professional whitening results depend greatly on whether stains are located externally on the enamel, or internally within the dentin layer. A dental examination using visual inspection, tactile probing and x-rays can identify the causes and origins of discoloration.
Extrinsic Stains
Extrinsic stains are situated on the outermost enamel surface of teeth. These external stains result when pigments and compounds temporarily adhere to enamel pores.
Common extrinsic stains stem from:
- Foods and Drinks – Coffee, tea, soda, sports drinks, berries, tomato sauce and other food items can impart color on enamel.
- Tobacco Use – Pipe and cigarette smoke introduce tar, nicotine and other pigments that cling to teeth. Smokeless tobacco also stains.
- Poor Oral Hygiene – Inadequate brushing and flossing allows chromogenic dietary compounds to build up on teeth. Plaque and tartar can also yellow enamel.
- Metallic Ions – Iron, manganese, copper and other metals in drinking water or dental alloys may oxidize and deposit on the tooth surface as colored compounds.
- Oral Products – Chlorhexidine, cetylpyridinium chloride (CPC) and stannous fluoride found in some rinses and toothpastes can stain pellicle on teeth.
Most external stains can be lightened with professional whitening treatments like in-office bleaching and take-home trays. Removing surface stains reveals the brighter and whiter underlying enamel.
Intrinsic Stains
Intrinsic stains lie beneath the enamel deep within the tooth’s internal structure. These internalized discolorations cannot be removed by surface techniques alone.
Causes of intrinsic staining include:
- Pulp Necrosis – Death of the pulp after trauma or root canal turns a tooth grey/yellow.
- Aging – The inner dentin gradually darkens and appears more yellow with age.
- Enamel Defects – Developmental enamel imperfections like hypoplasia and hypocalcification.
- Dentin Defects – Imperfect dentin mineralization from disease or tetracycline exposure.
- Congenital Disorders – Conditions like dentinogenesis imperfecta, amelogenesis imperfecta.
- Dental Trauma – Injuries during childhood can cause internal bleeding/discoloration.
- Medications – Tetracyclines, doxycycline, minocycline, and fluorosis from excess fluoride intake.
Whitening treatments only alter the outermost layer of enamel. Intrinsic stains incorporated into deeper tooth structure during development cannot be removed by external methods. More invasive options are required to mask or alter innate tooth color.
Professional Whitening Methods
Dentists have access to highly effective bleaching agents and techniques to manage difficult stains. But individual characteristics of the teeth and patient compliance influence outcomes.
In-Office Bleaching
In-office whitening rapidly lightens teeth during a 60-90 minute office visit. A higher concentration of 15-35% hydrogen peroxide or carbamide peroxide gel is applied directly to the teeth. Advanced light and laser activation speeds up the bleaching process.
Several consecutive in-office sessions may be needed for severe stains, as each session lightens by about 2-3 shades. Results last 1-3 years with touch-up treatments. In-office methods work well for extrinsic stains and mildly intrinsic discoloration.
Take-Home Whitening Trays
Custom-fitted plastic trays are filled with 10-22% carbamide peroxide gel to wear for 2-4 hours daily or overnight. This gradual method often lightens teeth up to 2 shades per week of use. Take-home trays provide a more even bleaching effect that lasts longer than in-office treatments.
But more frequent application for 2-4 weeks is required to lift stubborn intrinsic stains. About half of tetracycline staining may be reduced with diligent use of take-home trays.
Microabrasion
An acidic/abrasive compound is used to gently abrade the enamel surface. This polishes away some external discoloration and shallow intrinsic stains up to 0.2mm deep. Several treatments slowly lift stains for a cumulative lightening effect.
Deeper tetracycline and fluorosis stains cannot be removed by microabrasion alone. It offers mild improvement but must be combined with other techniques.
Internal Bleaching
For a discolored root canal treated tooth, the dentist accesses the empty pulp chamber through the back of the tooth. Peroxide gel is sealed inside for several days to internally bleach the tooth.
This method only masks innate grey/yellow color of pulpless teeth from the inside. It cannot alter deeper intrinsic stains affecting the entire tooth structure.
Dental Veneers
Veneers consist of thin porcelain overlays that cover the visible front surface of teeth. While invasive, veneers create an even, bright smile by masking underlying stains that do not bleach well. Veneers are highly resistant to new staining.
Dental Bonding
Bonding places tooth-colored resin material directly onto the tooth surface to conceal stains. Like veneers, bonding hides intrinsic discoloration by applying an overlay coating to the front of the tooth. The composite resin bonds to the natural tooth for seamless blending.
Tooth Jewelry
Those with severe tetracycline staining may choose to conceal it with dental grillz or tooth jewels. Gold, silver or jewel-encrusted accessories adhere to teeth with bonding material to distract from underlying stains. However, grillz pose oral health risks.
When to Visit the Dentist?

Consult a dentist if:
- Over-the-counter whitening yields unsatisfactory improvement of yellow teeth. Identifying causes of resistant stains can guide treatment.
- Suspect intrinsic tooth discoloration due to fluorosis, tetracycline exposure or pulp death. Surface methods cannot alter these innate stains.
- Discoloration localizes in spots, streaks or patches. This may indicate underlying decay or trauma needing treatment.
- Whitening causes pain or high sensitivity. Dentist can identify causes and recommend desensitizing options.
- Gums become irritated from whitening agents. Manage gum inflammation to avoid permanent damage.
- Wanting to expedite the process with professional treatments. Dentist can tailor options to your particular staining and budget.
- Whitening results regress quickly. Dentist can help determine causes of rapid re-staining and preventive strategies.
- Have old discolored dental work needing replacement or concealment.
Visiting a dentist offers the most effective solutions for managing yellow teeth resistant to over-the-counter methods. Be sure to discuss all whitening options – including risks, benefits and costs – before proceeding. But significant improvement of stubborn stains is often achievable with professional help.
Frequently Asked Questions about Whitening Yellow Teeth
Here are answers to common questions patients have about yellow teeth that resist whitening:
Q: Why don’t drugstore whitening strips lighten my yellow teeth?
A: Whitening strips only remove extrinsic surface stains from enamel. Yellow teeth may have intrinsic stains within the deeper tooth structure that strips cannot alter.
Q: I used a store-bought whitening kit for 6 weeks but my teeth are still yellow. Why?
A: Over-the-counter whitening uses low peroxide concentrations that take weeks to lighten teeth a couple shades. Yellow teeth with deep intrinsic stains need stronger in-office bleaching or custom trays from a dentist.
Q: Can yellow tetracycline stains be removed completely by laser whitening?
A: No, tetracycline binds deep within the tooth structure during development. While laser whitening can slightly improve the appearance, it cannot eliminate this type of intrinsic stain.
Q: How long do professional whitening results last on yellow teeth?
A: In-office and custom tray whitening lasts 1-3 years but results vary based on your habits. Avoiding smoking, coffee, tea and red wine helps sustain a whiter smile longer. Doing occasional touch-up whitening also maintains brightness.
Q: Does fluoride cause permanent yellow stains on children’s teeth?
A: If over-consumed during enamel development, fluoride can cause moderate to severe intrinsic discoloration. Mild fluorosis exhibits as nearly invisible white specks. More advanced fluorosis stains enamel dark yellow, brown or black.