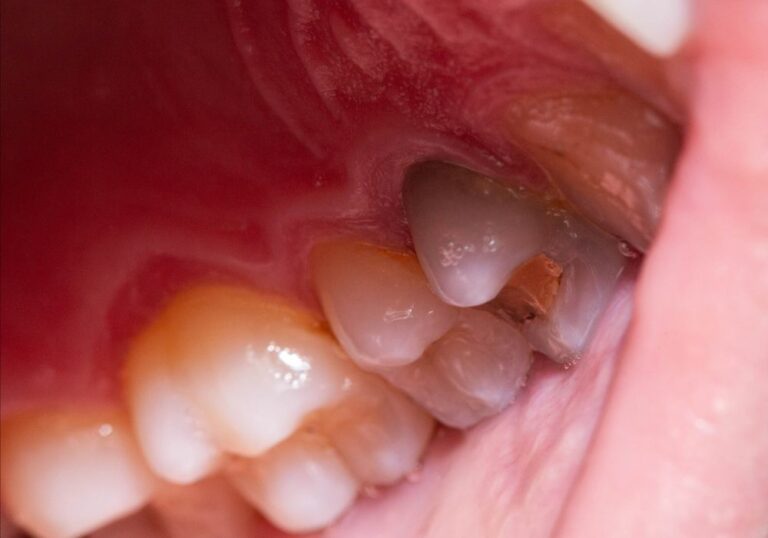
You bite into your morning bowl of ice cream, and suddenly a sharp pain shoots through your upper back tooth. Or maybe you notice pain in a molar when you brush or floss only on one side. This type of localized tooth sensitivity or discomfort can stem from various causes.
One-sided tooth pain is often a signal that something is irritating the inner layers or nerve of that specific tooth. It’s the tooth’s way of letting you know it needs your attention. While the discomfort may come and go at first, it’s essential to identify and address the underlying problem before it progresses.
Left untreated, minor sensitivity can turn into severe tooth decay, infection, or fracture. But when you understand possible causes and see your dentist promptly for diagnosis and care, you can reverse damage and maintain your smile.
What causes a tooth to be sensitive or painful when touched on one side?

There are several potential causes for a tooth to hurt when touched or brushed on one side:
- Dental decay: A cavity affecting the outer enamel layer as well as the deeper dentin and pulp can lead to sharp pain when touched due to inflammation of the tooth’s nerve. Decay usually starts as a small soft spot that gradually enlarges into a hole or cavity. As the decay reaches the inner pulp layer, the pain often becomes more intense and biting may trigger throbbing as well.
- Cracked or fractured tooth: Cracks or fractures in a tooth can make it extremely sensitive and painful when any pressure is applied. These cracks can range from small craze lines in the enamel to major cracks extending down vertically into the root. Damage may be due to trauma, grinding, or flexing forces on the tooth. The pain occurs because the crack allows penetration of temperature, sweet, and pressure stimuli deep into the inner tooth layers.
- Exposed tooth root: Gum recession from periodontal disease, overly vigorous brushing, or other causes can lead to loss of gum tissue, exposing part of the root surface. The cementum layer covering roots is softer than enamel and has microscopic tubules that transmit pain easily when exposed. Hot, cold, sweet, brushing, flossing or even air can trigger sharp pain.
- Abscess: A tooth abscess is a pocket of pus caused by a bacterial infection in the root’s pulp. Abscesses cause throbbing pain and extreme sensitivity to any touch or pressure because of inflammation pressing on the tooth’s nerve. The pus buildup results from untreated decay, cracks, or gum disease that allows bacteria to infect the pulp.
- Damaged filling or dental crown: Old fillings or crowns that become cracked, loose or leak around the edges allow irritation of the inner tooth layers from temperature changes. This can make the tooth extremely sensitive, especially when chewing or brushing near the defective filling or crown margin.
- Gum disease: Gingivitis and periodontitis cause inflammation, gum bleeding, deepened pockets around the tooth, and potential bone loss. These issues make teeth less stable in their sockets and more sensitive to touch. Aggressive brushing of inflamed gums can be quite painful as well.
- Sinusitis: A sinus infection or inflammation of the maxillary sinuses located above the upper teeth can sometimes radiate pain down to the upper back teeth. The pain is often worse when pressure is applied to the tooth. Sinus tooth pain is usually confined to just one side – the side with the sinus problem.
Why does tooth sensitivity occur on just one side?
There are several reasons why tooth sensitivity or pain often occurs on only one side:
- The problem starts on one side first. For example, a new cavity, cracked filling, or gum recession typically begins as a localized issue affecting just a single site on one surface of the tooth. With time, it may spread to encompass the entire tooth if not treated.
- The tooth has multiple root canals that diverge and surround sinus structures. Upper premolars and molars often have two or three roots. If one root canal becomes abscessed or inflamed, it may only cause pain on that side where the infected root lies adjacent to bone or sinus.
- There are occlusion issues on just one side. For instance, uneven biting forces could result in excessive pressure on one side, leading to pain from trauma or flexing forces concentrated on that side.
- Sinusitis almost always causes unilateral pain. Maxillary sinus infections lead to tooth pain localized on the affected sinus side once the infection spreads to the bone and tooth roots. The roots and nerves are irritated when the sinus swells and presses on them.
- Nerve hypersensitivity is sometimes an issue. Neuropathic pain or chronically irritated nerves on one side may have hypersensitive hot spots that get triggered by stimuli like brushing or temperature changes, resulting in tooth pain confined to that side. Nerve injuries, chronic inflammation, and some systemic diseases are risk factors.
For pain involving a single tooth only, the cause is usually clear based on an exam and x-rays. However, multiple neighboring teeth hurting on the same side often require considering several possible diagnoses.
What causes tooth pain when biting down on one side?

In addition to pain when brushing or touching the tooth, discomfort or sensitivity when biting down or chewing can indicate an issue on one side:
- Dental decay reaching the pulp chamber causes severe pain from pressure on the inflamed nerve during biting.
- Cracked, broken, or loose fillings move slightly when biting, irritating the inner tooth layers.
- Periodontal disease with damage to supporting ligaments causes pain when the loose tooth moves in its socket during chewing.
- Abscesses cause throbbing, pulsating pain that radiates when any pressure is applied from biting.
- Bruxism or teeth grinding puts extreme forces on teeth, leading to fractures or trauma to the pulp and nerves.
- High dental fillings or uneven bite alignment causes pain on the side of excessive force concentration when biting.
- Maxillary sinusitis can impose pressure on upper teeth roots during chewing, causing ache.
In most cases, the act of biting down compresses an already irritated, inflamed, or damaged nerve. Temperature extremes from food or drink can exacerbate the sensitivity when biting. Prompt dental diagnosis and treatment are critical to resolve bite pain before it becomes severe or leads to tooth loss.
How dentists diagnose the cause of one-sided tooth pain
Dentists have an array of diagnostic tools at their disposal to identify the exact source of pain or sensitivity isolated to one side of a tooth:
- Medical history – Asking about the patient’s description of their pain, location, duration, triggers, and intensity provides your dentist with key clues. Details about any recent dental work or trauma are also helpful.
- Clinical examination – Your dentist will visually examine the tooth crown and surrounding gums, looking for signs of decay, cracks, wear, gum recession, swelling, or irregularities. Gently palpating the gums to check for pain and conducting temperature sensitivity testing or bite tests will aid diagnosis.
- Percussion testing – Tapping lightly on the tooth with a dental instrument applies pressure to the tooth while checking for pain. This helps determine if the tooth is loosened or if biting causes discomfort.
- Pulp vitality testing – Cold and heat applied to the tooth surface, or electric pulp tests stimulate the nerve. Checking its response assesses the nerve health and vitality.
- Probing depths – A periodontal probe is used to measure and record pocket depths around each tooth. This reveals the presence and extent of any gum recession or periodontal damage.
- Dental x-rays – Intraoral, bitewing, panoramic and periapical x-rays allow clear visualization of the tooth roots, bone, and sinuses to identify decay, fractures, abscesses, and bone loss that may explain pain on one side.
Once the dentist pinpoints the cause of discomfort through the diagnostic process, they can then recommend appropriate treatment to resolve your pain and save the tooth. An accurate diagnosis is key to effective, long-lasting relief.
Common treatments for one-sided tooth sensitivity and pain
The recommended treatments will vary depending on the cause of your tooth pain:
Treating dental decay
- Fillings – Removing decayed material and placing composite resin or amalgam fillings helps resolve pain from cavities. For larger decayed areas, a dental crown may be needed.
- Root canal therapy – For decay reaching the pulp, root canal treatment cleans out the canals and seals the interior to save the damaged tooth.
- Extraction – Severely decayed teeth that cannot be restored may need extraction if non-salvageable. Implants can replace extracted teeth.
Treating cracked and fractured teeth
- Dental bonding – Flowing composite resin into superficial cracks may stabilize the tooth’s surface and prevent sensitivity.
- Crown – A full coverage crown protects a cracked tooth from further damage. Ceramic, gold, and zirconia crowns distribute biting forces evenly.
- Extraction – Fractured teeth with cracks extending below the gum line or fractures involving large portions of the tooth may require extraction if crowns cannot stabilize the damage.
Treating gum recession and exposed roots
- Desensitizing toothpaste – Brushing regularly with toothpaste containing potassium nitrate or stannous fluoride can block sensitivity signals.
- Fluoride treatments – Professionally applied high concentration fluoride varnish or gel helps strengthen enamel and dentin.
- Gum grafting surgery – A periodontist can surgically place donor gum tissue over exposed roots to protect them.
- Resin coating – Applying a layer of dental adhesive resin can provide a barrier over sensitive root surfaces.
Treating dental abscesses
- Root canal therapy – Draining abscess contents and disinfecting the tooth’s root canal system can often save the tooth.
- Tooth extraction – Non-salvageable teeth with advanced abscesses may need extraction to drain the infection and relieve pain.
- Antibiotics – Prescription antibiotics taken short-term can control abscess infection while definitive treatment is in progress.
Treating other causes
Replacing defective dental work, adjusting the bite with orthodontics, treating gum disease, and resolving sinus problems will alleviate referred pain once the underlying issue is resolved. Night guards protect teeth from damage related to grinding and clenching.
No matter the cause of sensitivity isolated to one side of a tooth, prompt dental treatment is essential for long-lasting pain relief and oral health. Let your dentist accurately diagnose the cause and help you choose the ideal treatment option.
When should someone see a dentist?

You should schedule an appointment promptly if you have a tooth hurting when brushed or touched on one side that persists more than 2-3 days. Seeing your dentist right away provides the best chance of reversing damage before it worsens or spreads. Ignoring the problem risks more complex issues like infection, tooth fractures, or loss of the tooth.
See your dentist immediately if the tooth pain is severe or interferes with eating, wakes you at night, radiates through your jaw, or is accompanied by bumps, swelling, bad taste, or fever. These symptoms may indicate a dental emergency like an abscess needing urgent care to prevent complications.
Other situations that warrant prompt dental evaluation of unilateral tooth pain:
- Discoloration, chipping, or visible cracks in the tooth enamel
- Pain when chewing or biting down
- Prolonged sensitivity to hot or cold temperatures
- Sudden sensitivity in a previously restored tooth with fillings or crowns
- Gum tenderness, swelling, or bleeding associated with the tooth pain
- Unexplained tooth pain that is not relieved by over-the-counter painkillers
The sooner you see your dentist for treatment when you have a painful tooth on just one side, the better your chances of reversing the problem and maintaining your smile. Ignoring symptoms only allows the issue to get worse.
Frequently Asked Questions about One-Sided Tooth Pain:
Q: Why do my teeth hurt temporarily when I eat or drink hot or cold foods?
A: Sharp, brief pain when exposed to temperature extremes is often due to common tooth sensitivity triggered by irritation of the inner dentin layer. Causes include enamel erosion, gum recession, microscopic cracks, a loose filling, or recent whitening treatment making teeth more vulnerable to hot and cold stimuli. Using desensitizing toothpaste and limiting acidic foods can help reduce temporary temperature sensitivity if it’s not severe or persistent long-term.
Q: Can a sinus infection cause pain in my upper back teeth?
A: Yes, it’s very common for sinusitis to radiate pain to the upper posterior teeth, especially when the roots are in close proximity to inflamed sinus linings. The maxillary teeth share nerves with the sinuses, so infection and swelling in those sinuses can irritate those nerves and lead to dental pain perceived as coming from the upper molars or premolars. Treating the sinus infection will usually resolve the toothache.
Q: What home remedies might help soothe a sensitive tooth?
A: These self-care tips may provide relief for mild tooth sensitivity:
- Rinsing with warm salt water helps reduce inflammation and swelling.
- Taking over-the-counter pain relievers like ibuprofen, aspirin, or acetaminophen for pain management.
- Using toothpaste for sensitive teeth containing potassium nitrate or stannous fluoride.
- Avoiding very hot or cold foods that trigger pain.
- Applying dental wax, clove oil, or Sensodyne directly to the sensitive area.
- Switching to a soft-bristle toothbrush and brushing extremely gently near the painful spot.
Q: How can you tell when tooth sensitivity may be a dental emergency?
A: Seek emergency dental treatment promptly if you have severe throbbing tooth pain that:
- Comes on suddenly and feels excruciating or intolerable
- Radiates into your jaw, ear, temple, or side of face
- Is accompanied by obvious swelling around the tooth
- Is causing numbness or making it hard to open your mouth
- Keeps you awake at night even taking painkillers
- Follows any trauma like a hard hit to the mouth area
These symptoms often indicate a significant problem requiring urgent care, like an abscessed tooth, fractured tooth, or injury to the pulp needing immediate treatment.
Q: Can a tooth be sensitive to cold but not hot temperatures?
A: Yes, it’s not uncommon for a tooth to be more sensitive to cold stimuli than hot. Early decay, cracks, or irritated nerves may make the tooth painfully sensitive to cold only. The cold penetrates deep into the microscopic tubules, triggering aggravated nerve responses. Hot foods may only impact the surface, not affecting the irritated inner pulp. If a tooth cringes with cold but not hot, discuss this symptom specificity with your dentist.