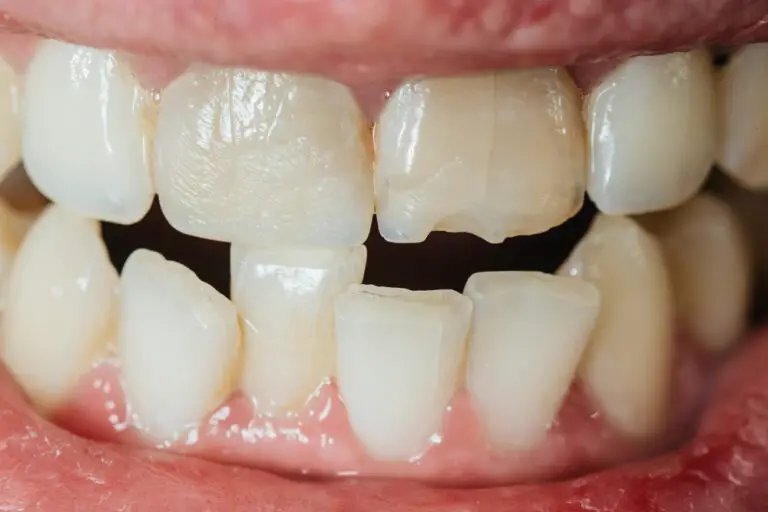
Teeth play a critical role in chewing, speaking, and maintaining the structure of the face. So when teeth become damaged, it can significantly impact a person’s oral health and quality of life.
Unlike bone, skin, and other tissues of the body, teeth do not repair themselves. But why is this? Understanding the reasons why tooth repair is limited provides key insights into developing new ways to regenerate and restore damaged teeth.
Tooth Structure and Composition
Teeth are complex organs composed of multiple specialized tissues that work together:
1. Enamel
Enamel forms the outermost layer of the tooth. It is the hardest substance in the human body. Enamel is composed of 96% mineral, with hydroxyapatite crystals comprising the main mineral. It contains no collagen and has no living cells.
During tooth development, enamel is laid down by epithelial cells called ameloblasts. Once enamel formation is complete, ameloblasts are lost. Enamel cannot regenerate more enamel cells.
2. Dentin
Underneath the enamel is dentin, a bonelike matrix that comprises the bulk of the tooth. Dentin contains 70% mineral crystals with collagen making up the remainder.
Odontoblasts are the cells embedded throughout dentin that form it. Dentin has tiny fluid-filled tubes known as dentinal tubules that radiate outwards from the pulp.
3. Pulp
At the center of the tooth is the pulp, containing soft connective tissue, blood vessels, and nerves. Odontoblasts in the pulp produce the dentin layer. The pulp provides some sensory innervation and nutrition to the tooth.
4. Cementum
Cementum covers the dentin of the tooth root and anchors the periodontal ligaments to the alveolar bone. Cementoblasts produce and maintain the cementum.
5. Periodontal Ligament
The periodontal ligament surrounds the tooth root and connects it to the alveolar bone of the jaw. This fibrous connective tissue helps attach the tooth.
Limitations in Tooth Repair
Given this complex structure, why can’t teeth naturally regenerate and repair damage? There are several key reasons:
1. Lack of Stem Cells
Stem cells are unspecialized cells that can divide and differentiate into specialized cell types. They are critical for tissue and organ regeneration.
Teeth lack a ready source of stem cells to drive reparative processes. The ameloblasts that form enamel are lost after development. Odontoblasts become trapped within dentin and cannot migrate to areas of injury.
2. Low Vascularization
Blood vessels deliver oxygen, nutrients, growth factors, and progenitor cells needed for repair. But teeth are poorly vascularized.
Enamel completely lacks blood vessels, while dentin only has some vasculature from branches of the pulp. This starves teeth of regenerative components.
3. Rigid Mineralized Matrix
The high mineral content of enamel, dentin, and cementum provides strength but makes natural repair difficult. The crystalline matrix is rigid with little flexibility for cell migration or tissue remodeling.
4. No Collagen in Enamel
Collagen provides a scaffold for cells and growth factors during natural tissue repair. But enamel lacks collagen, further limiting any regenerative capacity.
5. Entrapped Odontoblasts
While odontoblasts in the dentin can stimulate limited reparative dentin formation, they cannot regenerate significant lost tooth structure. Odontoblasts get trapped within the dentin during development and cannot migrate to access and remodel damaged areas.
6. Lack of Nerve Regeneration
Sensory nerves in the pulp cannot readily regenerate due to the difficulty of nerve growth crossing the rigid dentin-enamel junction. This can impair tooth vitality and function when innervation is damaged.
Current Tooth Repair Research
While tooth repair is inherently limited, cutting-edge research aims to overcome these regenerative barriers through four key approaches:
1. Stem Cell Therapy
Stem cells from dental or non-dental tissues can be transplanted into teeth to differentiate into odontoblasts or ameloblasts. This can stimulate reparative dentin or enamel formation.
2. Biomaterials Scaffolds
Natural and synthetic biomaterials like collagen are under study to serve as scaffolds that can attract native progenitor cells and facilitate tooth repair.
3. Growth Factors
Signaling molecules called growth factors can stimulate odontoblast proliferation and dentin regeneration when applied to sites of injury.
4. Gene Therapy
Modulating gene expression in existing tooth cells may enhance natural tooth repair processes by upregulating regenerative and dentinogenic genes.
Conclusion
Teeth cannot significantly self-repair due to their specialized composition and structure. But bioengineering approaches offer hope for regenerating damaged enamel and dentin. With further research, we may be able to unlock the full regenerative potential of teeth.
Frequently Asked Questions
Why can bones repair themselves but not teeth?
Bones have living cells, stem cells, blood vessels, and a flexible matrix that enable regeneration. Teeth lack stem cells and blood vessels. Also, the hard mineral matrix of enamel and dentin makes it difficult for cells to migrate to areas of injury for repair.
Can dentin grow back?
Dentin has limited ability to regenerate. When the overlying enamel is damaged, the odontoblasts in the dentin can lay down reparative dentin. However, the amount of dentin regrowth is very small. Dentin cannot significantly reform once lost.
How can we regrow enamel?
Enamel cannot naturally regenerate as it lacks living cells. Current research on enamel regrowth focuses on stem cell transplantation or stimulating ameloblast differentiation. But recreating the intricate structure of enamel remains highly challenging.
Are there any natural ways to repair teeth?
There are no natural ways to significantly rebuild lost tooth structure by self-repair. Good oral hygiene and fluoride treatment can help strengthen enamel and limit damage. But once cavities and tooth fractures occur, the only option is professional dental treatment.
What is the most recent advancement in tooth repair research?
A recent advance is the development of a peptide-based biomaterial scaffold that can stimulate stem cells from the tooth pulp to differentiate into dentin-forming odontoblasts. This shows potential for enabling dentin regeneration when applied to areas of decay.