What is Remineralization and How Does it Work?
Remineralization is the process of restoring minerals that have dissolved from the enamel surface of teeth. Enamel is made up of around 96% minerals, with hydroxyapatite being the main mineral crystal. Hydroxyapatite gives enamel its hardness and strength.
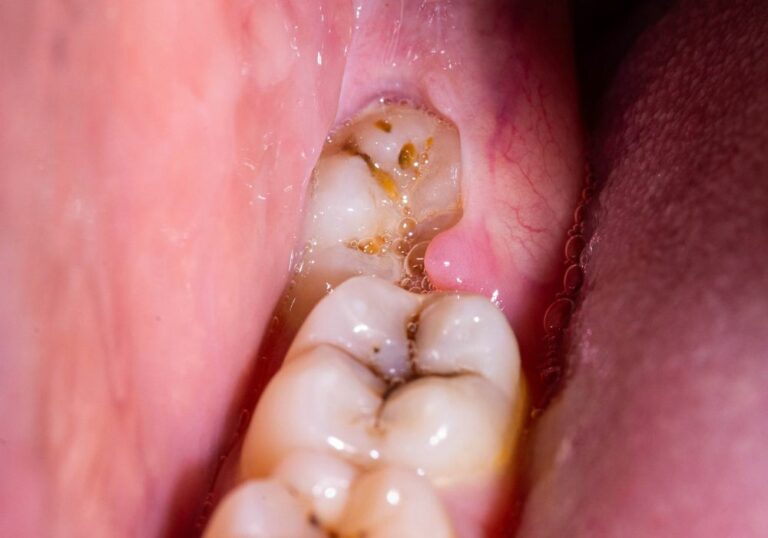
Over time, acids from food debris and bacteria in the mouth create an acidic environment that causes these hydroxyapatite crystals to dissolve, creating tiny pores and defects in the enamel in a process called demineralization. If the demineralization continues over time, it can lead to cavities.
Remineralization is the reversal of this damage, where minerals are redeposited back into the enamel to fill the pores and mend the defects. This helps to restore strength and mineral content to the enamel.
The main minerals involved in remineralization are calcium, phosphate, and hydroxide ions. Our saliva contains calcium and phosphate ions that constantly work to remineralize the teeth. However, when pH drops due to acids, more minerals are lost from teeth than can be replaced.
Fluoride helps tip the balance in favor of remineralization by attracting calcium and phosphate ions and redepositing them into eroded areas of enamel. It can also attract hydroxide ions, helping to neutralize plaque acids and raise pH.
At very early stages of decay, remineralization can repair white spot lesions and areas of enamel where minerals have dissolved but no cavity has yet formed. However, if decay progresses further and cavitates, a restoration is likely needed.
Factors That Promote Remineralization
There are several factors that encourage the natural remineralization process and help prevent tooth decay:
- Fluoride – Fluoride makes enamel more resistant to acid. It also promotes remineralization by incorporating into hydroxyapatite crystals in place of hydroxide ions, making them less soluble. Fluoride is found in toothpaste, rinses, professionally applied treatments, and many public water sources. Using topical fluoride is an important part of preventing cavities.
- Calcium and phosphate – Calcium and phosphate ions are the building blocks of strong enamel. A diet with adequate amounts of calcium-rich foods like milk, cheese, yogurt, eggs, fish with bones, leafy greens, nuts and seeds helps provide raw materials for remineralization.
- Saliva flow – Our saliva provides a constant bathing of calcium and phosphate ions on teeth. Chewing sugar-free gum or mints can help stimulate saliva production and deliver more remineralizing minerals. Staying hydrated is also important.
- Reducing acid attacks – Limiting intake of acidic foods and beverages prevents pH drops in the mouth that lead to demineralization. Saving sugary or acidic snacks for mealtimes only and rinsing with water after consumption can help neutralize acids.
- Oral hygiene – Good oral hygiene habits like brushing, flossing and professional cleanings reduce plaque bacteria on teeth that produce acids as they metabolize sugar and carbs. This minimizes acid attacks on enamel.
- Alkaline environment – Creating a neutral or slightly alkaline oral environment encourages mineral redeposition because minerals are more soluble in acidic environments. Limiting acidic foods and using alkalizing oral care products may aid remineralization.
Types of Remineralizing Toothpastes

There are a variety of specialty toothpastes marketed to enhance remineralization:
- Fluoride toothpastes – All toothpastes contain fluoride, but some contain a higher concentration for enhanced protection against demineralization. Most standard toothpastes contain 1,000-1,500 ppm fluoride, while prescription strength may be 5,000 ppm or greater.
- Calcium phosphate toothpastes – Many brands designed for sensitive teeth or enamel strengthening include calcium phosphate compounds like tricalcium phosphate or hydroxyapatite. These provide free calcium and phosphate ions to redeposit into enamel.
- Nano-hydroxyapatite toothpastes – Nano-hydroxyapatite particles contain the same minerals found in tooth enamel. These tiny particles bind to enamel and attract calcium and phosphate ions to rebuild demineralized crystals.
- Xylitol toothpastes – Xylitol is a natural sugar alcohol that prevents the growth of cavity-causing bacteria like S. mutans. By inhibiting acid-producing bacteria, xylitol creates an environment favorable to remineralization.
- pH neutral toothpastes – Most toothpastes are acidic, with pH around 4-5.5. Neutral or slightly alkaline toothpastes counteract plaque acidity and support enamel rehardening.
Professional Remineralization Treatments
In addition to fluoride toothpastes, your dentist may recommend professional remineralizing treatments for high-risk patients:
- Fluoride varnish – This concentrated topical fluoride adheres tightly to enamel when painted on teeth and absorbs deeply to enhance mineral content. It stays on longer than other types of fluoride and is well-retained even with drinking and eating.
- High concentration fluoride gels – Custom trays filled with a fluoride gel containing 12,000-22,500 ppm fluoride are worn 5-60 minutes to allow fluoride to penetrate lesions. This is often repeated frequently in the initial phase, such as daily or weekly for several weeks.
- Calcium phosphate rinses – Rinsing with a highly concentrated calcium phosphate solution can help redeposit minerals into white spot lesions. This may be prescribed for use after routine dental cleanings.
- MI Paste – Casein phosphopeptide-amorphous calcium phosphate (CPP-ACP or Recaldent) attracts and stabilizes calcium and phosphate ions. By enhancing substantivity, MI Paste prolongs contact time with enamel for sustained remineralization.
Is Remineralization Effective for Different Stages of Decay?
White spot lesions – Remineralization has the greatest chance of full success at the earliest white spot stage before any physical cavity forms. High concentration fluoride plus dietary changes has been shown to facilitate rehardening of many shallow white spot lesions.
Small enamel cavities – Small areas of enamel decay may be arrested or remineralized if they are prepped into a saucer-shape that exposes enamel rods optimally to topical minerals. Remineralizing pastes or gels are then placed in the shallow cavity and sealed with adhesive.
Dentin cavities – If decay has progressed deeper into dentin, remineralization is more difficult due to dentin’s lower mineral content and high organic matrix. While some rehardening of the remaining enamel shell is possible, most dentin cavities ultimately need restorative intervention.
Extensive cavities – Large, deep cavities indicate advanced decay that is unlikely to be reversed with remineralization alone. The amount of tooth structure loss is too great. Traditional fillings or dental crowns are needed to restore form and function in these cases.
In summary, remineralization works best at early to moderate stages of tooth decay confined to enamel. While topical fluoride and minerals can harden enamel and prevent cavity progression, restorations are still needed once significant tooth structure is lost. Ask your dentist whether remineralization could be beneficial for your situation.
Tips for Successful Remineralization Therapy

Here are some evidence-based tips for successfully rehardening early tooth decay:
- Use a remineralizing fluoride toothpaste twice per day
- Apply prescription strength fluoride gel via custom trays on a regular basis (e.g. weekly, biweekly)
- Get fluoride varnish or MI Paste professional applications every 3-6 months
- Take calcium & vitamin D supplements if diet is lacking these nutrients
- Chew xylitol gum several times per day
- Limit snacking times to 3/day to reduce acid attacks
- Rinse mouth with water after acidic drinks or foods
- Avoid constant sipping or nursing of sugary/acidic drinks
- Use alkalizing rinses to neutralize plaque acids
- Get routine dental cleanings & exams to find lesions early
Diligent oral hygiene plus professional remineralizing therapies can help rebuild early enamel damage, but results take time and consistency. Ask your dentist for guidance creating a customized remineralization plan for your situation.
Frequently Asked Questions
Q: How long does it take to remineralize teeth?
A: It depends on the severity of demineralization, but you may start to notice improvements in weeks or months with consistent care. Mild white spots could reharden in 3-6 months with fluoride and calcium/phosphate therapies. Deeper lesions may take up to a year to show significant remineralization.
Q: Can dentists put minerals back in teeth?
A: Dentists don’t directly insert minerals back into teeth, but can prescribe treatments like fluoride varnish that facilitate redeposition of calcium and phosphate from your saliva back into enamel. They also polish away superficial enamel to expose fresh mineral-hungry layers.
Q: Do remineralizing pastes really work?
A: Yes, fluoride pastes and pastes containing amorphous calcium phosphate have been clinically proven to reharden early decay and white spot lesions. But consistency and patient compliance with daily use is key to their success.
Q: What remineralizes teeth the fastest?
A: Because fluoride adheres firmly and enhances mineral uptake, high concentration fluoride from gels, varnishes or prescription toothpastes tend to produce the fastest remineralization results.
Q: Can I remineralize teeth without fluoride?
A: You can have some success from calcium phosphate or nano-hydroxyapatite pastes, but remineralization is very difficult without fluoride. Fluoride stabilizes redeposited minerals and makes enamel more acid-resistant. Using fluoride is highly recommended.