CDHP Dental Health Project
Teeth Health Guides

Recent Dental Health Guides
Can You Go to the Dentist While Pregnant?
Even though pregnancy is the happiest time for most women, this condition may carry unpleasantness and additional…
20 Best Dental Health Books for Kids
One of the crucial things is to explain to kids the importance of oral hygiene. However, visiting…
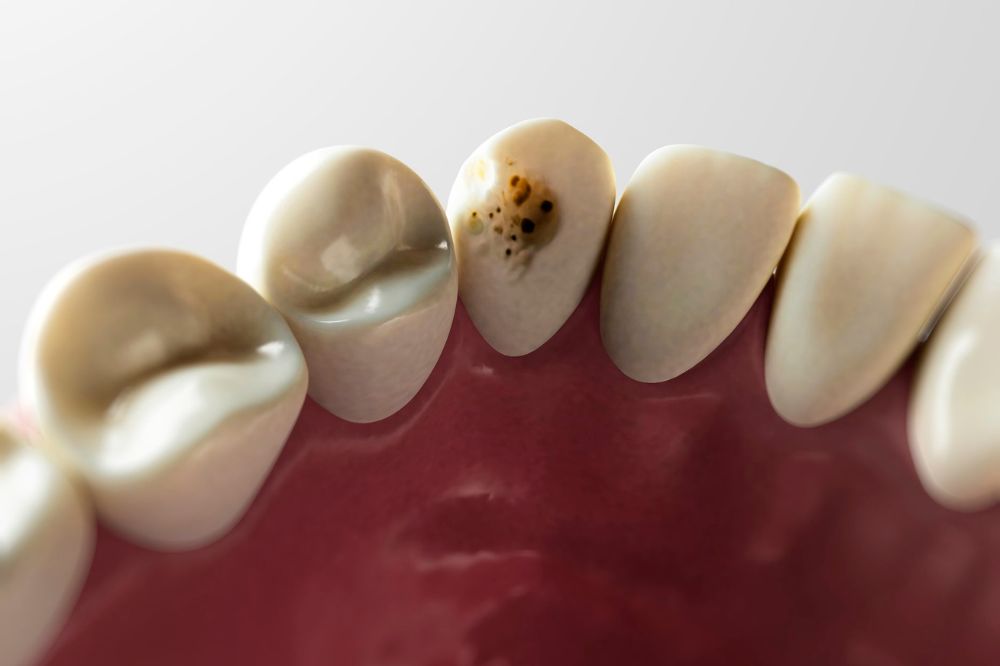
17 Ways to Prevent Tooth Decay
Tooth decay is the first step to a more severe issue, dental cavities. Since such a complex…
Is Dental Insurance Worth It? (Pros & Coins)
Primary dental insurance is far less complicated than health insurance and has the purpose of helping you…
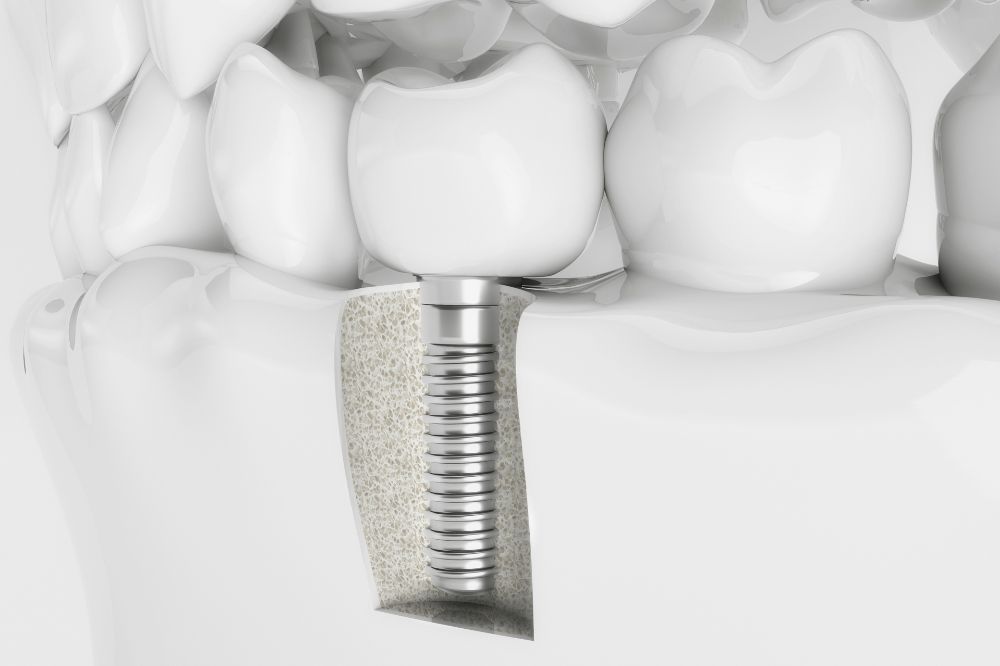
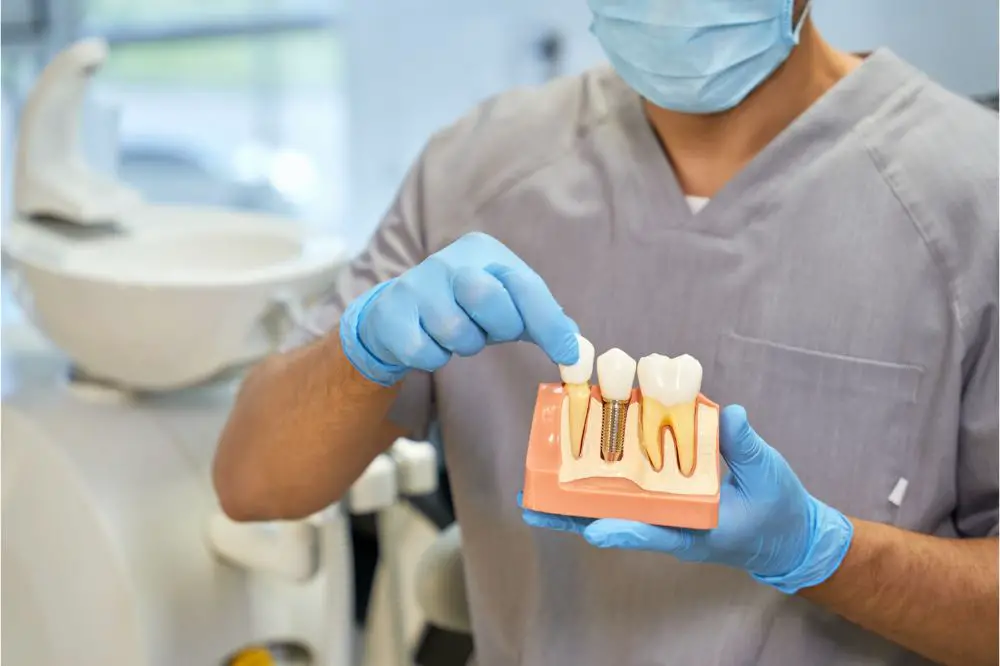
How Much Are Dental Implants? (Price Chart)
As you know, dental implants can be costly, so the question is whether they are worth…
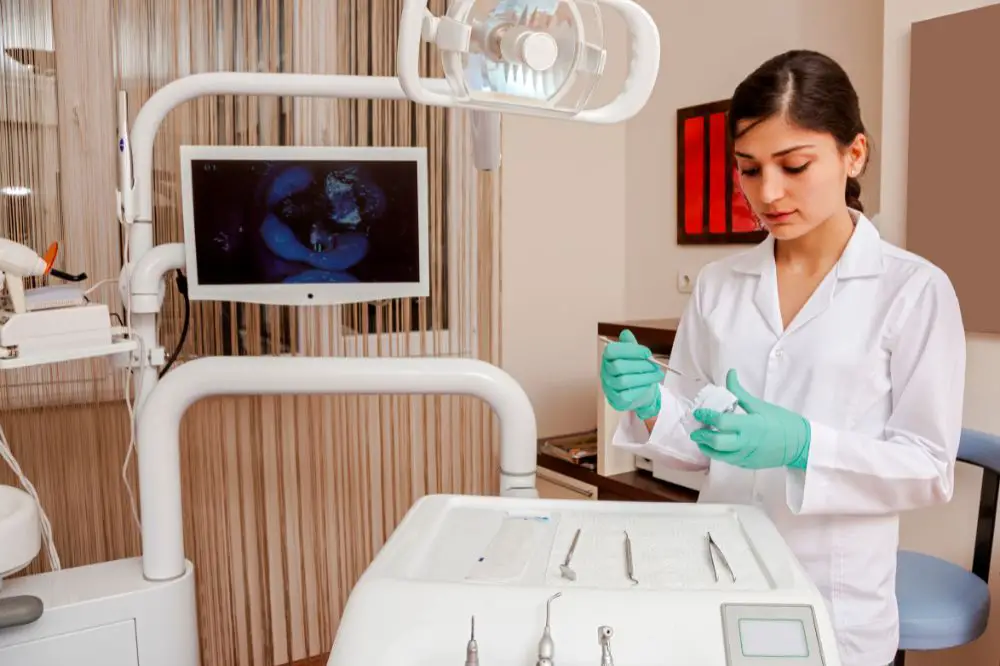
How to Become a Dental Hygienist? Everything You Need to Know
There are medical professionals you should visit at least once a year for an annual checkup. For…
9 Best Dental Insurance With No Waiting Period (Price Chart)
Many dental insurance plans include a waiting period of a few months and sometimes over a year…
How Much Do Dental Implants Cost with Cigna Insurance? (Price Chart)
Dental implants are a popular and effective solution for replacing missing teeth and improving oral health. They…
What Dental Insurance Does Walmart Have? (A Quick Guide)
Walmart is a well-known retail giant that not only offers a vast range of products but also…
5 Steps to Become a Dental Assistant (Requirements & Degree)
If you are looking for a challenging and rewarding career in the medical field, becoming a dental…
3 Steps to Get Dental Implants Covered by Insurance
If you’ve lost a tooth or need to have one extracted, you’ll probably be thinking about your…
How Long Does Dental Numbing Last? (Recovering Faster Tips)
If you ever need to undergo a dental procedure other than a mere check-up or an X-ray,…
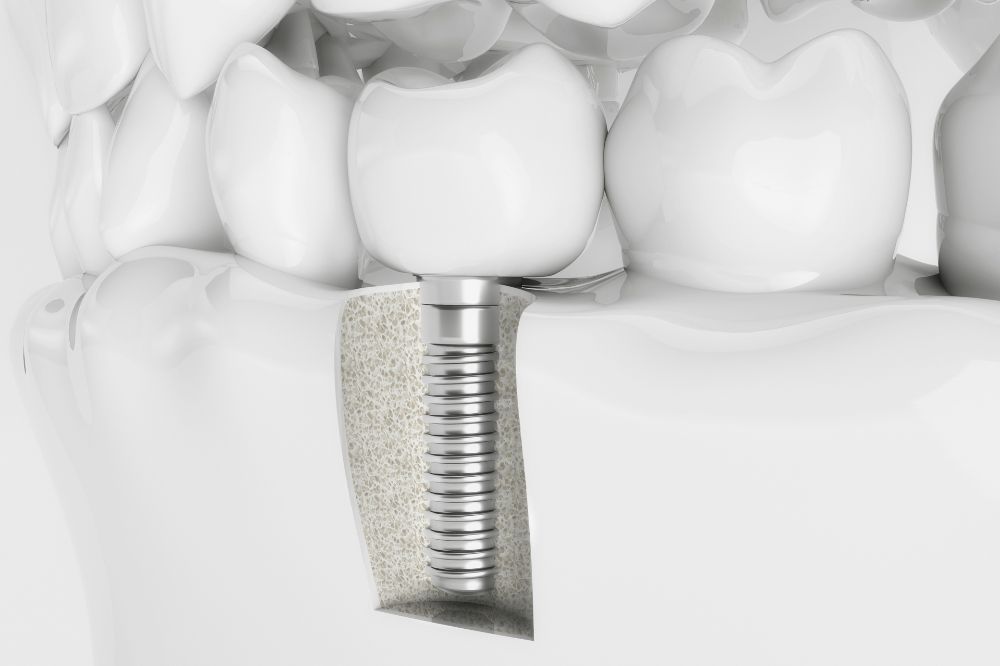
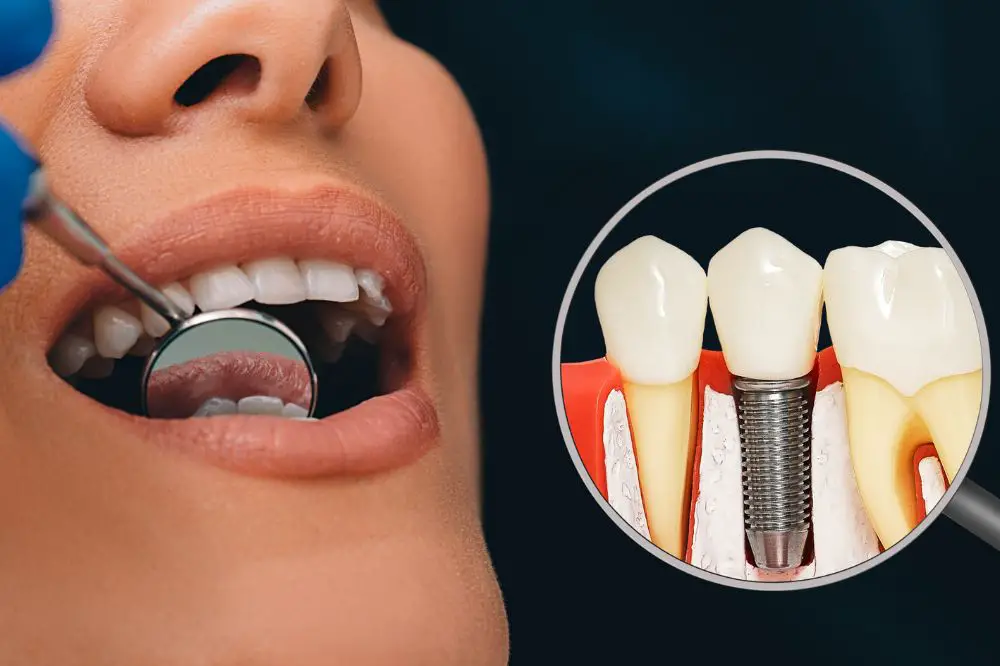
How Long Do Dental Implants Last? (Tips to Last Longer)
Dental implants are a long-term solution to tooth loss, and nowadays, the procedure can give you natural-looking…
How Long Does It Take to Become a Dental Hygienist?
If you are interested in the medical profession and are looking for a rewarding and fulfilling career…
What Does a Dental Hygienist Do? (8 Things)
If you are considering a career in the medical profession but don’t want to become a doctor…
What Does a Dental Assistant Do? (10 Things)
If you’re looking for an exciting job that will see you working as part of a team…
Why No Dairy After a Dental Implant?
Having dental implants fitted is a major procedure, and ensuring your mouth and gums heal properly after…
How Long Do Dental Cleanings Take? (Details)
Dental cleaning is an essential part of looking after your teeth and maintaining your overall oral health,…
How Long Does It Take to Become a Dental Assistant?
If you’re looking for a steady job with a regular, competitive salary and you like working with…
8 Places to Get a Free Dental Makeover
Even for those with plenty of money, the prices of dental procedures can be extremely high, and…